International Journal of Oral and Dental Health
Immediate Implant Placement in the Infected Site with Presence of a Pre-Existing Cyst: Report of Two Cases
Binbin Yu, Chun Fan, Ximei Xiao, Jiajia Song, Chenglong Ji and Chunyang Zhang*
Affiliated Hospital of Qingdao University, Shandong, China
*Corresponding author: Chunyang Zhang, Affiliated Hospital of Qingdao of University, Shandong, China, E-mail: chunyangzhang89@hotmail.com
Int J Oral Dent Health, IJODH-1-010, (Volume 1, Issue 2), Case Report; ISSN: 2469-5734
Received: June 15, 2015 | Accepted: July 20, 2015 | Published: July 24, 2015
Citation: Yu B, Fan C, Xiao X, Song J, Ji C, et al. (2015) Immediate Implant Placement in the Infected Site with Presence of a Pre-Existing Cyst: Report of Two Cases. Int J Oral Dent Health 1:010. 10.23937/2469-5734/1510010
Copyright: © 2015 Yu B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Aim: The purpose of this report is to illustrate the possibility of inserting immediate implants into the fresh extraction sockets in the infected site with presence of a pre-existing cyst.
Presentation of case: The 1 of two cases: A 31-year-old man, presented to severe periodontitis with presence of a pre-existing infected cysts developed, which was 5mm × 7mm on the labial side of mandible. The radiography showed that a large translucent image around the periapical portion of 31 with mobility of II° in mandible. The extraction and implantation including bone grafting to substitute 31 tooth had been performed in one appointment. One implant (14mm length × 3.7mm in diameter SIN implants Dentis, made in Korea) was inserted apically through a cyst cavity. Three months later, the second surgery phase (healing screw insertion) had been followed, and no sign of alternation of radiography and clinical indication after 18 months.
The other, a 53-year-old man came to our attention, with presence of a pre-existing infected cyst on labial side of 42 tooth. We placed one implant in the infected position of the mandible with a small amount of heterologous bone after the elimination of the infected 42 tooth, the meticulous cleaning, and alveolar debridement. A second surgery phase had been done after three months.
Discussion and conclusion: This report showed that the placement of immediate implants in presence of a pre-existing infected cyst may not be necessarily contraindicated if appropriate clinical procedures like antibiotic administration, meticulous cleaning, and alveolar debridement are performed before implant surgical procedure. Immediate placement of implants for replacement of teeth with the pre-existing infected cysts is a predictable treatment and can be indicated for replacing teeth lost. This report regards the immediate placement of an implant into a residual cyst; some anatomical, surgery techniques, clinical and pathological considerations arise from this case. Both implants were successfully osseointegrated, and the cysts were healed.
Keywords
Periapical cyst, Immediate dental implant, Infection
Introduction
The use of immediate implants in patients with teeth lost due to the infected site is now an established practice [1]. In the two cases, two implants were placed into the pre-existing cysts where the sites were in a history of a pre-existing infection in mandible. Sometimes the infection is active, so that the possibility exists for the long-term infections that can negatively impact the prognosis of the implants. In the previous literature, the fresh-socket implants are contraindicated with a pre-existing inflammation due to the risk of microbial interference in the healing process. McCracken also reported that immediate implant placement IIP) into an infected socket, like periodontitis due to the previous pathogen may release some inflammatory factors and result in a secondary infection. However, treatment of patients with the periapical pathology may encounter some problems during the process. But the data from animal research, human case reports and case series, and prospective studies showed similar success rates for implants placed into sites associated with chronic periapical pathology compared with implants placed in non-pathologic sites. The aim of this work is to illustrate the importance of periodontal infection control together with prudent management of implant placement in the infected sites in order to best solve the problem of the patient.
Alveolar ridge resorption after tooth extraction may considerably reduce the residual bone volume and compromise the favorable positioning of implants required for optimal restoration. This is even more pronounced in the anterior teeth, where ridge resorption often creates an unfavorable lingual/labial discrepancy between the implant and the prosthesis. To preserve the alveolar bone level from the collapse caused by treatment and to reduce treatment time in situations in which tooth extraction precedes implant placement, IIP has both social and economic advantages. The overall treatment time is reduced, a second surgical intervention is avoided, and there is a decrease in rehabilitation treatment time [2] because it minimizes the number of surgical procedures by combining extraction, implant placement, and bone grafting (if needed) into one appointment [3]. In two cases, the immediate placement of the implants into the fresh extraction sockets with the peri-apical pathology avoids this undesirable resorption [4,5]. Also, this report is to evaluate and to discuss possible predisposing factors for the development of infection after placement of the immediate implants on the site of the patient with presence of a pre-existing infected cyst.
Presentation of Case
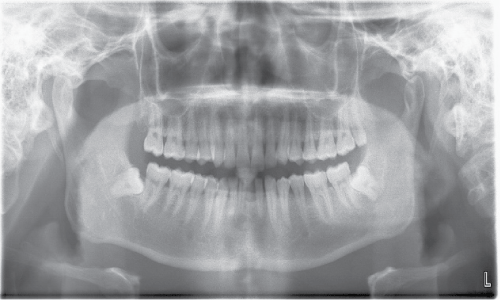
Two patients, systemically healthy, were extensively evaluated with regard to clinical signs, implant treatment, and postoperative complications. The 1 of two cases: A 31-year-old man, smoker without chronic disease presented to the Hangdao Dental Implant Center with history of conservative periodontal treatment, the chief complaint of dull pain in the lower left incisor. Clinical examinations revealed: bleeding index I°, the redness of gum, a gingival recession, the mobility of II° of 31 with deep pocket 6mm. Radiographic examinations confirmed the presence of the horizontal bone loss and size 5mm × 7mm circumscribed translucent image developed on the periapical portion on the 41,31 of mandible (Figure 1). A dark color of the crowns on the 41 and 31 has been showed, and the routine root canal had been done on the 41 (Figure 2). We presented the cases of immediate loading of implants using a scannographic template (Figure 3), and implant placement using a drill guide is created by stereolithography. The notice was informed to the patients before the process of treatment. Prior to surgery, a medical consultation and thorough explanation of possible risks to patients had been done. One hour before the surgical procedure, the patient received a prophylactic dose of 1g amoxicillin and performed for 2 minutes rinse with chlorhexidine 0.20%.
.
Figure 1: Panoramic radiography at the time of preextraction illustrating the radio-transparent image associated with the apex of 31, 41.
View Figure 1
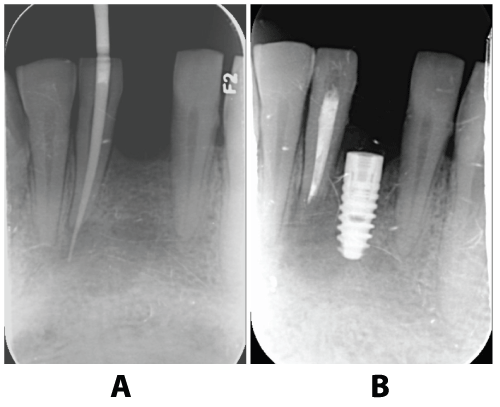
.
Figure 2: (a) The root canal had been done on the 41 before extraction of 31, and note the intentional placement of an endodontic file beyond the apex into the cystic cavity. (b) The image demonstrates the clinical healing at 10 weeks after the 2-stage surgical protocol and submerged healing of the implant.
View Figure 2
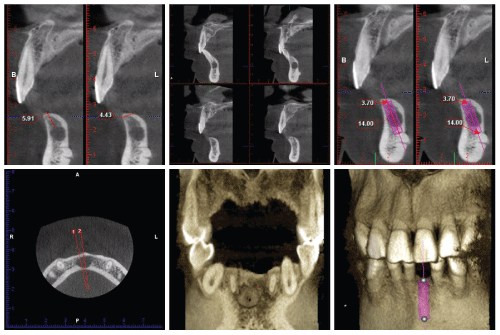
.
Figures 3: CBCT scans showed the presence of a radiolucent image of approximately 1cm in diameter periapically to the 31 tooth, and assessed the available apical bone and the anatomy of the alveolar crestal bone of mandible in the area of the extraction as a potential implant site after tooth extraction.
View Figures 3
The other, a 53-year-old man, nonsmoker in good health conditions with presence of periodontitis and the site of a pre-existing infected cyst, which developed 5mm × 6mm translucent image of radiography, and an alveolar crest resorption on 42 tooth of mandible.
Surgical procedure
The main objective of this protocol is to ensure the lack of pathology when placing the implant, and at the same time, to optimize the availability of soft and hard tissues for primary healing and probable lateral bone augmentation. Under all aseptic precautions in the operation theater, local anesthesia with adrenalin was given for tissue separation using the proper curette on the labial side of the mandible. Surgical access was obtained on the anterior peri-apical cyst of the infected site by means of an incision. The incision was extended from 32 distal crest to the mesial sulcus of the 43. A full thickness flap was carefully elevated (Figure 4) and a dark-blue circumscribed lesion was exposed. The small perforation was made for aspiration of cystic contents. An aspiration biopsy was carried out before the surgery. Then, the 31 tooth with the cystic linings was carefully removed by means of a routine technique and done with socket degranulation. The curettage was done with solution. A second access was gained at the apical level, allowing the meticulous debridement of the surgical chamber for elimination of the periapical lesion and of the infected tissues in combination with peripheral ostectomy of the alveolus. It was decided to proceed with the placement of implants in the site of numbers 31. We advocated a 2-stage surgical protocol for load-free and submerged healing to ensure predictable osseointegration (Figure 2). One implant was inserted on 31 tooth of mandible: (size 3.7 with diameter × 14mm length, SIN implants Dentis, made in Korea) for implantation with two-stage. Following the visual orientation of CBCT (Cone Beam Computed Tomography) for apical setting of the implant (Figure 3), the fixtures of immediate implant are anchored apically to alveolar socket in native bone and achieved the primary stability of the implant. The residual apical bone of 3 to 5mm in a vertical dimension is required. The implant was inserted by placing implant shoulder 1mm under the crestal bone providing the physiological ridge alterations after extraction, and was anchored to the lingual/labial cortical plate of the post-extraction site [6-9]. So, in the presence of large sockets that preclude the involvement of apical native bone, it may be preferable to defer implant placement. The implant was showing thru the area of fenestration, it was filled the surgical chamber with xenogenous bovine bone graft and a collagen membrane. GBR was accomplished to support bone healing of peri-implant alveolar defects with the flap repositioned and sutured. The site was covered with the gauze pack and ice on the rest of the day. The specimen was sent for a histopathologic examination and a diagnosis of was revealed: periapical cyst (Figure 5). Postsurgical antibiotics for 7 days, and postsurgical chlorhexidine were followed for 2 weeks. The patient was shown how to perform a roll-stroke brushing technique and was motivated to control oral hygiene. The patient did not report specific symptoms and showed no adverse clinical signs. Sutures were removed on 7th days of IIP (Figure 6), and surgery healing was satisfactory. The second surgery phase (healing screw insertion) had been done after three months of IIP (Figure 7).
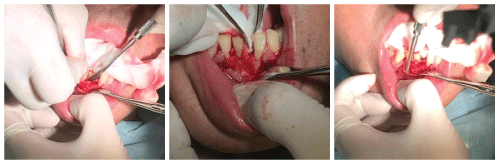
.
Figures 4: Surgical access was obtained on the peri-apical cyst by means of an incision. The incision was extended from the 32 distal crest to the mesial sulcus of the 43. A full thickness flap was carefully elevated.
View Figures 4
.
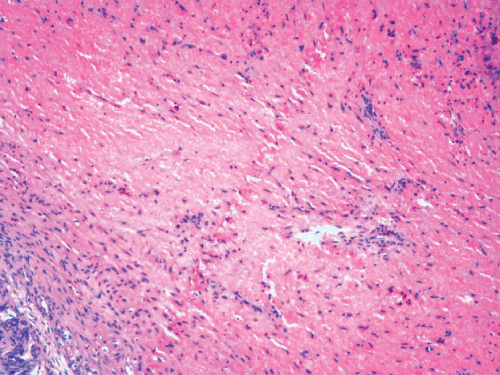
Figure 5: The histopathologic analysis revealed: a stratified squamous epithelium, with granulation tissue forming the cyst wall. Graft particles were visible, surrounded by collagen fibres in the cystic wall. A fibrous capsule with inflammatory infiltrate by chronic inflammatory cells, resulting in a final diagnosis of a paradental cyst.
View Figure 5
.
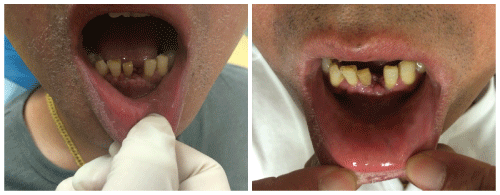
Figure 6: The gingival and crest bone condition of case 1 after the suture was removed on seven days of the implant surgery
View Figure 6
Result
In our two cases, postoperative checkup included the clinical check-up and radiographic examination, which was followed the period ranged from 1 to 2 years after surgical procedures. The implant showed that the adequate initial stability had been gotten in the correct position. Radiographic examination revealed that the complete bone had been filled into the resented area (Figure 8). The stable bone level is 2mm lower than the previously placed implant on the normal range (A mean marginal bone loss of 0.7-2mm was registered). Both cases were healed with no further symptoms and no lasting complications. The implants were fully osseointegrated, presenting without radiographic signs of alterations or clinical pathologies (Figure 7,8).
.
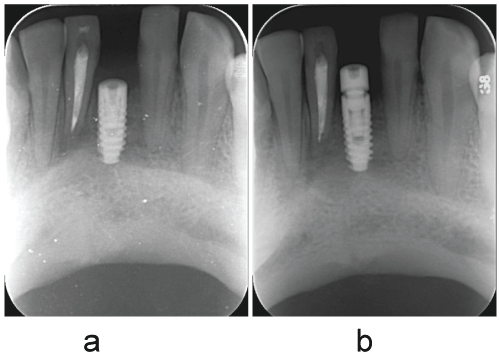
Figure 7: Case 1, (A)There was no radiographic signs of alteration on the implant of 31.
(B) Showing the second surgery phase (healing screw insertion) on the 31 had been followed after 3 months of IIP.
View Figure 7
.
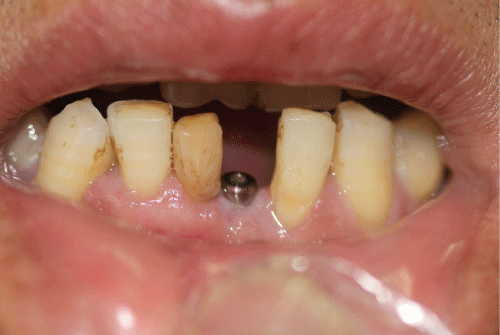
Figure 8: The implant of case 1 was fully osseointegrated, presenting satisfactory esthetic conditions.
View Figure 8
Cyst contains contents (aspirate): a dirty white, low protein, cholesterol crystal content, and viscoid suspension of keratin which has an appearance of pus, but without an offensive smell.
Discussion
This report showed that the placement of immediate implants in presence of a pre-existing infected cysts may not be necessarily contraindicated if appropriate clinical procedures like antibiotic administration, meticulous cleaning, and alveolar debridement are performed before implant surgical procedure. A few cases with present of the teeth in a pre-existing infected cyst have been reported in a success rate of the immediate implant placement (IIP). The further study is still needed to make sure the future evaluation. Short-term implant survival and success rates appear similar for the infected sites and normal tissue sites for IIP [10]. Some factors such as the dimension of the lesion; inadequate morphology of the area or the non-effective debridement need to be concerned during an implant surgery. It is very important that the elimination of all contaminated tissues and the controlled regeneration bone of the alveolar defect. Frequently, the compromised teeth that are indicated for extraction are enveloped in infection, which conventionally contraindicate their immediate replacement with endosseous dental implant [2] because of the risk of microbial interference with the healing process. The protocol that completely removes the contaminated soft and hard tissues by meticulous debridement was maintained, allowing successful GBR of the previously infected alveolus implant. The reason is that there might be a potential contamination of the implant during the initial phase of wound and bone healing due to the remnant of infection, which affects the process of osseointegration. This procedure should be limited to experienced surgeons who are highly skilled in differentiating and debriding granulation tissue. The surgeon must also be proficient in GBR procedures to skillfully correct the significant alveolar defects that are commonly associated with these cases.
The IIP in extraction site is a treatment with a defined protocol, and well accepted, thanks to the preservation of aesthetics, the maintenance of the alveolar walls, a better positioning of the implant, and a reduction in surgery time and the overall treatment [11]. However, the concept of IIP after extraction of a tooth with periapical disease is a very controversial topic, with few scientific studies of quality published. Controversy exists in treatment planning relative to the implant therapy must fulfill both functional and esthetic requirements to be considered as a primary modality. Aiming to reduce the process of alveolar bone resorption and treatment time, the immediate placement of endosseous implants into extraction sockets with the infected sites has been propagated by some authors. However, a few clinical data are available on IIP in the pre-existing infected cysts. In the presence of cyst, one problem in IIP in the site may be an incongruity between the implant diameter and the morphology of the alveolus that is worsened by the presence of a bone defect because of the bone cyst. Many stated that a minimum of residual apical bone of 3 to 5mm in a vertical dimension is required [12,13]. So that some alveolar sites do not qualify for IIP. Another critical aspect is the diameter of the lesion. If it exceeds the diameter of the planned implant, then there may be a need to obtain implant stabilization more apically. Conversely, if the implant diameter is larger than the diameter of the lesion, initial stability may be sufficient without extending 3 to 5mm apically to the extraction socket [14]. One CBCT scan is based on the assessment of the available apical bone and the anatomy of the mandible in the area of the anticipated extraction site. Pre-extraction CT scans may present a useful diagnostic aid to assess the risk of inferior alveolar plate perforation for IIP in the anterior and posterior mandible. Measurements were obtained on the axial sections of the selected teeth to evaluate the amount of bone available apical to the root apices to determine the frequency of sites where an IIP protocol presented a high risk for inferior alveolar plate perforation (Figure 2). In the study of Lindeboom and colleagues [15], in the immediate placement group, larger diameter implants were used more frequently than in the delay-placed group (2-3 months after extraction). Another study has shown that wide-diameter implants are associated with increased removal torque, and that the load on cortical bone decreases with increasing implant diameter. Moreover, according to Truninger and colleagues [16], the axis of an implant placed in the anterior area to match esthetic expectations differs from the axis of the tooth that is extracted. It can therefore be assumed that even though the diameter of the implant might be bigger than that of the lesion, the buccal part of the former pathology would remain intact despite the drilling sequence. Thus, the main criteria for immediate placement of an implant into a socket should be the achievement of primary implant stability after debridement and not the size of the lesion itself.
Our report supports that the immediate post-extraction implant placement has success rates similar to those obtained when the implant is placed on a deferred basis [13] following a protocol that includes antibiotic therapy, debridement, antisepsis of the compromised tissue, and high primary implant stability. The high survival rate and the normal marginal bone changes obtained in several studies support the hypothesis that implants may be successfully osseointegrated when placed immediately after extraction of teeth presenting endodontic and periodontal lesions, provided that appropriate clinical procedures are performed before the implant surgical procedure. Also, we support that the success of fresh-socket implants placed in chronic and acute lesions may be explained by the behavior of endodontic infections because they are mixed infections dominated by anaerobic bacteria (Fusobacterium, Prevotella, Porphyromonas, Actinomyces, Streptococcus) commonly restricted in the infected local area. Extraction of the involved tooth generally leads to eradication of the cultured microorganisms [3]. This inflammatory reactive tissue protects bone from direct bacterial aggression.
In addition, the success factors may influence the outcome of this approach (e.g., host-, implant-, and occlusion-related factors). Implant success and survival depend on various factors including pre-surgical diagnosis and evaluation of general dental conditions, such as:
Primary implant stability
Of all factors involved, primary stability seems to be the most important determining factor on immediate implant loading. Functional loading placed on an immobile implant is an essential ingredient to achieve osseointegration [17]. If an implant is placed in the soft spongy bone with poor initial stability, it often results in the formation of connective tissue encapsulation.
Surgical technique
Gentle surgical placement is also a key element for implant success regardless of the applied treatment protocol. Excessive surgical trauma and thermal injury may lead to osteonecrosis and result in fibrous encapsulation of the implant [18]. In addition, it is critical for the success of endosseous root form implants that adequate load be placed on the drill during the preparation of osteotomies. It has been demonstrated that independently increasing either the speed or the load caused an increase in temperature in bone.
Host-related factors
Bone quality & quantity and occlusion-related factors are included:
Clinically, host bone density plays an important role in determining the predictability of the immediate implant loading success. An implant placed in compact dense bone is more likely to ensure initial stability and, hence, better able to sustain such immediate forces. Within the limited available information, it appears that primary stability, more than the arch (anatomic) location, may be the fundamental requirement for immediate implant loading techniques. Controlling functional forces is one of the ingredients for obtaining success of immediate implant loading [19], found more crestal bone loss in the loaded 1-stage implant group when compared to the 2-stage unloaded control group [19]. Regarding of the two-stage surgical procedure, separated by a period of osteointegration of six months as minimum, prior to the prosthetic loading of the implant at the mandible. It was suggested that the early occlusal loading during healing may account for this observation, since early loading may interfere with the ability of new bone being formed to replace the necrotic bone at the implant/bone interface resulting from surgical trauma. This, added to the period of wound healing and postextraction bone formation, was invariably associated with aesthetics periodontal alterations due to the localized bone resorption observed at the extraction area, caused by the absence of the stimulus associated to the periodontal ligament, as well as the remodeling of the soft tissues [20] despite the clinical success demonstrated in many cases. Hence the submerged implants were preferable for the initial rigid fixation. When a proper surgical/prosthodontic technique is followed, the crestal bone loss around immediately loaded implants seems to be in the normal range when compared to a submerged protocol. However, certain problems/concerns remain when this 2-stage surgical protocol was used. These include: avoiding any prosthesis for a temporary time to promote uneventful healing; loose denture, pain, difficulty with chewing during transitional removable prosthesis wearing. In 1 of our cases, the prosthesis had been done on the 9th months due to the patient was not recalled on time.
Oral hygiene
Regular maintenance may be another factor to ensure the long-term success of immediately loaded implant. What needs to be considered is the well knowledge of patient oral and periodontal conditions. Periodontal disease should be treated completely before implant treatment. In addition, the patient should be monitored over time in order to reduce inflammatory indexes that may increase the failure risk and biological complications of our implant-supported restorations. After surgical curettage of site, implants may develop an inflammatory pathology as a result of a long-term residual infection. It is very important to reduce the inflammatory response on the periodontal tissues. Moreover, it may be beneficial in maintaining the integrity of the extraction sockets and contribute to the maintenance of the interdental papillae around implant restorations.
Various studies have demonstrated the feasibility and predictability of this technique. However, most of these articles are based on retrospective data or uncontrolled cases. Randomized, prospective, parallel-armed longitudinal human trials are primarily based on short-term results and long-term follow-ups are still scarce in this field. Nonetheless, from available literature, it may be concluded that anatomic locations, implant designs, and restricted prosthetic guidelines are key to ensure successful outcomes.
Our report here [2,21-23] demonstrated that IIP in infected extraction sockets can be successful, provided that thorough preoperative care is given. However, more randomized controlled clinical trials with a longer follow-up are required to confirm this procedure as a safe treatment. Moreover, the outcome measures of the cases were not related to the type of infection; the classification of infection was often vague and varied among the studies. Until now, no study compared the immediate placement of implants in infected sites conducting a careful debridement with and without the use of systemic antibiotics. Thus, more research is needed concerning the issues. With the trend of shortening treatment time and reducing patient discomfort/inconvenience, immediate loading implant has reemerged as an alternate approach. This treatment approach has been studied and has shown promising and predictable results. But, it is important to note that a meticulous case selection is still needed to integrate this treatment into daily practice. Certain criteria and guidelines have to be followed to avoid any unnecessary failure. However, within the limit of a case repot, timing of implant placement does not represent a parameter that can affect the short-term treatment outcomes if you meet certain principles.
Conclusion
We concluded that the two cases presented successful results by placing immediate implants into the infected cysts. Immediate placement of teeth implants for replacement of teeth with pre-existing infected cysts is a predictable treatment and can be indicated for replacing teeth lost due to the pre-existing infected cysts. The protocol of meticulous debridement of the infected lesion tissues in combination with peripheral ostectomy of the bone cysts should be followed. Future studies, preferably randomized, prospective longitudinal studies, are certainly needed before this approach can be widely used.
Ethical Statement
Two patients signed the informed consent form approved by the Research Ethics Committee of the Huangdao Hospital, University of Qingdao, authorizing treatment and publication of the case.
Acknowledgements
We are grateful for the Affiliated Hospital of Qingdao University that offers a place to us for the study of clinical cases.
References
-
Temmerman A, Meeus M, Dhondt R, Wierinck E, Teughels W, et al. (2015) Oral implant placement and restoration by undergraduate students: clinical outcomes and student perceptions. Eur J Dent Educ.
-
Chen ST, Wilson TG Jr, Hämmerle CH (2004) Immediate or early placement of implants following tooth extraction: review of biologic basis, clinical procedures, and outcomes. Int J Oral Maxillofac Implants 19: 12-25.
-
Quirynen M, Van Assche N, Botticelli D, Berglundh T (2007) How does the timing of implant placement to extraction affect outcome? Int J Oral Maxillofac Implants 22: 203-223.
-
Siegenthaler DW, Jung RE, Holderegger C, Roos M, Hämmerle CH (2007) Replacement of teeth exhibiting periapical pathology by immediate implants: a prospective, controlled clinical trial. Clin Oral Implants Res 18: 727-737.
-
Araújo MVF, Sommerville D, Dhingra A, Schincaglia GP (2015) Immediate Placement and Restoration of an Implant in an Infected Socket in the Esthetic Zone. Clin Adv Periodontics 5: 83-89.
-
Botticelli D, Berglundh T, Lindhe J (2004) Hard-tissue alterations following immediate implant placement in extraction sites. J Clin Periodontol 31: 820-828.
-
Araújo MG, Sukekava F, Wennström JL, Lindhe J (2005) Ridge alterations following implant placement in fresh extraction sockets: an experimental study in the dog. J Clin Periodontol 32: 645-652.
-
Schropp L, Isidor F (2008) Timing of implant placement relative to tooth extraction. J Oral Rehabil 35 Suppl 1: 33-43.
-
Caneva M, Salata LA, de Souza SS, Bressan E, Botticelli D, et al. (2010) Hard tissue formation adjacent to implants of various size and configuration immediately placed into extraction sockets: an experimental study in dogs. Clin Oral Implants Res 21: 885-895.
-
Álvarez-Camino JC, Valmaseda-Castellón E, Gay-Escoda C (2013) Immediate implants placed in fresh sockets associated to periapical infectious processes. A systematic review. Med Oral Patol Oral Cir Bucal 18: e780-785.
-
Hardt CR, Gröndahl K, Lekholm U, Wennström JL (2002) Outcome of implant therapy in relation to experienced loss of periodontal bone support: a retrospective 5- year study. Clin Oral Implants Res 13: 488-494.
-
Hämmerle CH, Araújo MG, Simion M; Osteology Consensus Group 2011 (2012) Evidence-based knowledge on the biology and treatment of extraction sockets. Clin Oral Implants Res 23 5: 80-82.
-
Schropp L, Wenzel A, Kostopoulos L, Karring T (2003) Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restorative Dent 23: 313-323.
-
Da Silva JD, Kazimiroff J, Papas A, Curro FA, Thompson VP, et al. (2014) Outcomes of implants and restorations placed in general dental practices: a retrospective study by the Practitioners Engaged in Applied Research and Learning (PEARL) Network. J Am Dent Assoc 145: 704-713.
-
Lindeboom L, Nabuurs CI, Hesselink MK, Wildberger JE, Schrauwen P, et al. (2015) Proton magnetic resonance spectroscopy reveals increased hepatic lipid content after a single high-fat meal with no additional modulation by added protein. Am J Clin Nutr 101: 65-71.
-
Truninger TC, Philipp AO, Siegenthaler DW, Roos M, Hämmerle CH, et al. (2011) A prospective, controlled clinical trial evaluating the clinical and radiological outcome after 3 years of immediately placed implants in sockets exhibiting periapical pathology. Clin Oral Implants Res 22: 20-27.
-
Roberts WE, Smith RK, Zilberman Y, Mozsary PG, Smith RS (1984) Osseous adaptation to continuous loading of rigid endosseous implants. Am J Orthod 86: 95-111.
-
Satomi K, Akagawa Y, Nikai H, Tsuru H (1988) Tissue response to implanted ceramic-coated titanium alloys in rats. J Oral Rehabill 15: 339-345.
-
Sagara M, Akagawa Y, Nikai H, Tsuru H (1993) The effects of early occlusal loading on one-stage titanium alloy implants in beagle dogs: a pilot study. J Prosthet Dent 69: 281-288.
-
Klinge B, Meyle J; Working Group 2 (2012) Peri-implant tissue destruction. The Third EAO Consensus Conference 2012. Clin Oral Implants Res 23 6: 108-110.
-
Hämmerle CH, Chen ST, Wilson TG Jr (2004) Consensus statements and recommended clinical procedures regarding the placement of implants in extraction sockets. Int J Oral Maxillofac Implants 19: 26-28.
-
Siegenthaler DW, Jung RE, Holderegger C, Roos M, Hämmerle CH (2007) Replacement of teeth exhibiting periapical pathology by immediate implants: a prospective, controlled clinical trial. Clin Oral Implants Res 18: 727-737.
-
Chrcanovic BR, Martins MD, Wennerberg A (2015) Immediate Placement of Implants into Infected Sites: A Systematic Review. Clin Implant Dent Relat Res.





