International Journal of Neurology and Neurotherapy
Congenital Skull Depression in a Newborn Delivered by Cesarean Section due to Continued Occipitotransverse Position: Case Report and Short Communication
Yuejun Huang, Jingwen Zhuang, Yezhen Chen and Weizhong Li*
Department of Pediatrics and Obstetrics, Second Affiliated Hospital of Shantou University Medical College, China
*Corresponding author:
Weizhong Li, Department of Pediatrics and Obstetrics, Second Affiliated Hospital of Shantou University Medical College, Shantou city, China, E-mail: 344202589@qq.com
Int J Neurol Neurother, IJNN-3-054, (Volume 3, Issue 4), Case Report; ISSN: 2378-3001
Received: May 12, 2016 | Accepted: August 22, 2016 | Published: August 24, 2016
Citation: Huang Y, Zhuang J, Chen Y, Li W (2016) Congenital Skull Depression in a Newborn Delivered by Cesarean Section due to Continued Occipitotransverse Position: Case Report and Short Communication. Int J Neurol Neurother 3:054. 10.23937/2378-3001/3/4/1054
Copyright: © 2016 Huang Y, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Skull depression in a newborn who delivered by cesarean section is a distinctly rare condition. The cause for skull depression in a newborn is puzzling, especially when there is no evidence of abdominal trauma to the mother, or when the newborn is delivered via cesarean section.
Case presentation: We reported one case of congenital skull depression in a male newborn who delivered by cesarean section due to continued occipitotransverse position. His mother had no history of abdominal trauma during the pregnancy, and there were no complications and difficulties in the process of cesarean delivery. The neurological examination of the baby was normal after birth. The depression had completely resolved when the child was 4 months. The child was meeting all appropriate developmental milestones until 3 years old.
Conclusions: We argued that the skull depression in this case resulted from a chronic pressure on the fetal skull in utero, which was due to the L5 vertebra. The existence of this clinical condition and its spontaneous resolution is important knowledge which could assist in the prepartum and postpartum management of children with this pathology.
Keywords
Congenital skull depression, Occipitotransverse position, Cause, Treatment
Background
Neonatal skull depression is uncommon, with an incidence of 1/10000 in Western countries and 3/10000 in Eastern countries [1]. The fontanel and low calcium content in the fetal skull facilitate a great deal of plasticity to the skull of fetus in utero and during the process of delivery. Most neonatal depressed skull fractures could be traced to a traumatic event, such as abdominal blunt trauma in the pregnant women and using obstetric forceps during delivery. It is rare to see congenital skull depression that occurs without instrumentation during labor. These 'congenital molding depressions' or 'spontaneous' intrauterine skull fractures, are thought to be a consequence of continued intrauterine mechanical stresses on the fetal skull by structures such as a prominent sacral promontory, uterine fibroids, exostosis of the lumbar vertebrae, and pelvic abnormalities [2,3]. Treatment options depend on the severity of the skull depression and underlying brain injury identified by clinical examination or with imaging.
.
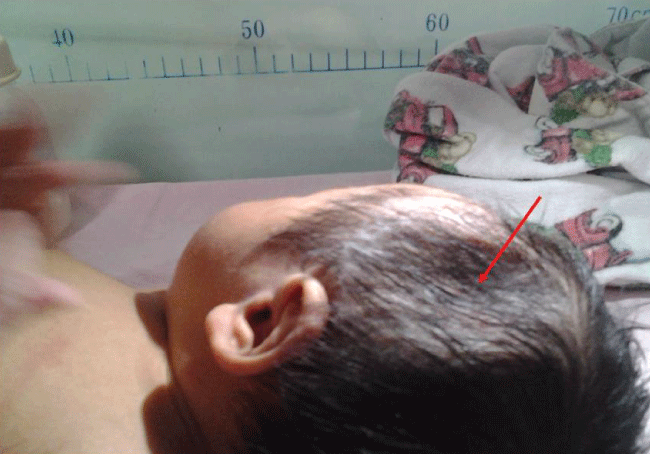
Figure 1: A large left parietal skull depression was seen in the newborn. The skull depression is indicated by arrows. There was no evidence of bruising or soft tissue swelling to support an acute injury.
View Figure 1
.
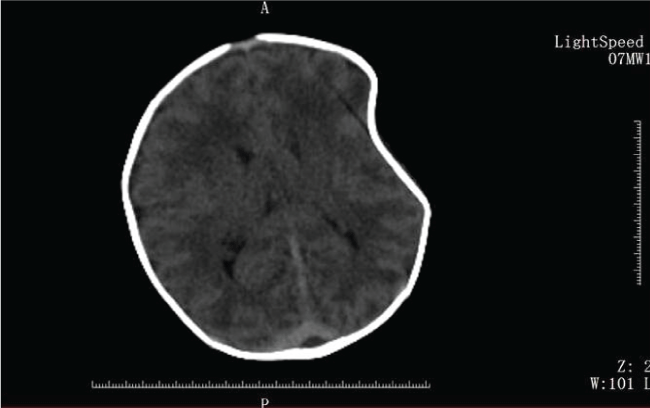
Figure 2: A head CT of the newborn with a large skull depression in the left parietal bone. There was no fracture and no underlying intracerebral hemorrhage or mass effect in the newborn.
View Figure 2
Case Presentation
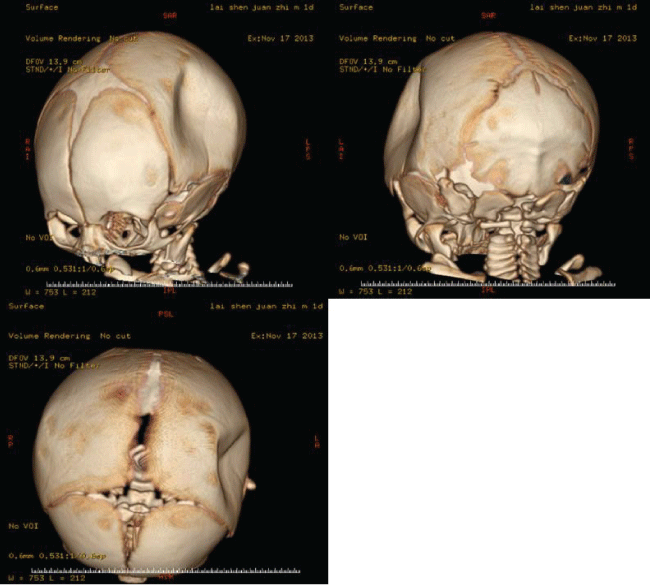
We reported a male term infant (gestational age = 38 w), who was delivered by cesarean section because of continued occipitotransverse position. There was no history of trauma in the mother during gestation period. Maternal obstetrical history was remarkable for 1 previous normal spontaneous vaginal delivery. Fetal ultrasound revealed that the fetus was in occipitotransverse position starting from 28 weeks of gestation until term. The amniotic fluid, the placenta, umbilical cord, and the fetal membrane were normal. The birth weight of the baby was 2.9 kg. Apgar scores were 9 and 10 at 1 and 5 minutes, respectively. The head circumference was 33 cm. A large left parietal skull depression in the baby was noted after birth (Figure 1). The skull depression was 4 cm × 5 cm × 2 cm in the left parietal area. There was no evidence of bruising or soft tissue swelling to support an acute injury (Figure 1). A head CT was performed, which revealed no fractures or underlying intracerebral hemorrhage (Figure 2). Three-dimensional reconstruction of the head CT (Figure 3) showed a depressed fracture in the left parietal bone. The term infant was asymptomatic and showed no sign of intracranial hypertension after birth. He was observed for 1 week in the department of Neonatology. After neurosurgical evaluation, the child was discharge from the hospital and followed expectantly. Follow-up evaluations were scheduled monthly to observe the reshaping of the skull depression. By the baby 4 months old, the depression had completely resolved. After 6 months, the child was follow-up evaluations for each two months. The interval time of follow-up evaluation was extended to 6 months after 1 year. The child was three years old until now, and he was meeting all appropriate developmental milestones.
.
Figure 3: Three-dimensional (3D) reconstruction of a large left parietal skull depression. Computed tomography reconstruction showing the concavity of the skull plate to the left of the sagittal suture and anterior to the lambdoid suture.
View Figure 3
Conclusions
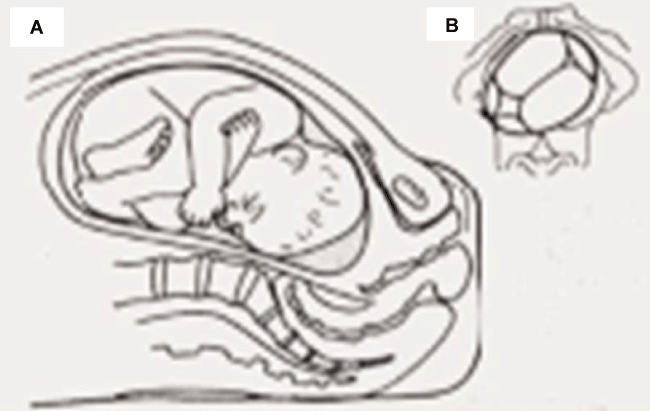
Skull depressions in newborns are often referred to as 'ping pong fracture' because the skull is being transformed from convex to concave, due to its malleability. 'Ping pong fractures' in the neonatal skull do not result in any discontinuity of the bony contour in the skull. Chronic pressure on the fetal skull in utero may be associated with such fractures [3]. Some researcher reported congenital skull depression not due to trauma [4-6], but they did not analyse the relation between congenital skull depression and the position which the fetus in the uterus. In the case reported here, the fetus was in an occipitotransverse position and delivered by cesarean section with no instrumentation used during labor. The term infant did not have any evidence of acute injury, symptoms of intracranial hypertension or radiographic evidence of intracranial lesion. We presumed that the skull depression in this case resulted from a chronic pressure on the fetal skull in utero, which was due to the L5 vertebra (Figure 4A and Figure 4B). Because radiological imaging could not provide enough information to differentiate between the spontaneous fracture and 'instrument associated' fracture, we argued that detailed birth history and postnatal examination for evidence of acute injury were crucial to formulate an exact diagnosis.
.
Figure 4: (A) Continued occipitotransverse position of the fetus; (B) L5 vertebra pressure on the fetal skull.
View Figure 4
Whether to treat a skull depression with no evidence of trauma and instrumentation during delivery perplex pediatrician and neurosurgeon. It was interesting to find that there were strong disagreements between conservative management and surgical intervention. Neurosurgical intervention has been the traditional treatment modality. There are different opinions on whether surgical intervention is the most appropriate method to treat congenital skull depression [7]. Those who supported compulsory surgical elevation, expressed concern that pressure from the depression might cause cerebral injury, a decrease in cerebral blood flow, and secondary epilepsy. In addition, it could cause physiognomic and psychological damage in a growing child. Moreover, the controversies still exist on the timing and method of interventions. Treatment method used in the past few decades included watchful waiting, manual reduction, and vacuum assisted reduction. Some studies recommended a waiting period after the diagnosis of skull depressions because a part of cases would spontaneously reduce [3,8]. Another researcher suggested to use pneumatic traction for the elevation of depressed skull fracture [8,9], which the operator's digits were placed on the opposite margins of the depression, and gentle tangential pressure was applied toward the center of the depression. The main reason for intervention was to prevent cortical damage. It was believed in the past that patients with congenital molding fractures had an increased risk for seizures [10]. However, other study [11] found that no increased incidence of seizures in patients with congenital skull depressions who were not elevated surgically. Several studies [12-14] had also shown that there was no difference between surgically treated and non-surgically treated for skull depression of pediatric patients who without symptoms of intracranial hypertension and radiographic evidence of intracranial lesion in terms of future neurological damage and the occurrence of seizures.
Although most untreated neonatal skull depressions seem to spontaneously resolve within 6 months [3], the skull depression results in considerable distress in the family of the newborn. Taking into account the parents be afraid of neonatal skull depression affect the brain development for the child, pediatrician need to provide sufficient evidence to support the treatment of their choice, such as follow-up observation or surgery.
Consent
Written informed consent was obtained from the parents of the patient for publication of this Case report and any accompanying images. A copy of the written consent is available for review by the Editor of this journal.
Competing Interests
The authors declare that they have no competing interests in our study.
References
-
Mastrapa TL, Fernandez LA, Alvarez MD, Storrs BB, Flores-Urueta A (2007) Depressed skull fracture in Ping Pong: elevation with Medeva extractor. Childs Nerv Syst 23: 787-790.
-
Hung KL, Liao HT, Huang JS (2005) Rational management of simple depressed skull fractures in infants. J Neurosurg 103: 69-72.
-
Aliabadi H, Miller J, Radnakrishnan S, Mehta AI, Thomas K, et al. (2009) Spontaneous intrauterine "ping-pong" fracture: review and case illustration. Neuropediatrics 40: 73-75.
-
Shamsian N, Robertson AT, Anslow P (2012) Congenital skull indentation: a case report and review of the literature. BMJ case reports.
-
Agrawal SK, Kumar P, Sundaram V (2010) Congenital depression of the skull in neonate: a case of successful conservative management. J Child Neurol 25: 387-389.
-
Amin AA, Al-Zeky AM, El-Azm M (2007) Vacuum extraction as a treatment modality of neonatal skull depression in a twin infant. Saudi Med J 28: 1122-1124.
-
Rugolotto S, Grippaldi E, Sidoti G, Padovani EM (2007) Intrauterine depressed skull fracture with spontaneous resolution. Pediatr Med Chir 29: 47-49.
-
Loeser JD, Kilburn HL, Jolley T (1976) Management of depressed skull fracture in the newborn. Journal of neurosurgery 44: 62-64.
-
Kim YJ, Lee SK, Cho MK, Kim YJ (2007) Elevation of depressed skull fracture with a cup of breast pump and a suction generator : a case report in technical aspects. J Korean Neurosurg Soc 42: 346-348.
-
Raynor R, Parsa M (1968) Nonsurgical elevation of depressed skull facture in an infant. The Journal of pediatrics 72: 262-264.
-
Jennett B, Miller JD, Braakman R (1974) Epilepsy after monmissile depressed skull fracture. J Neurosurg 41: 208-216.
-
Pearl PL, McCarter R, McGavin CL, Yu Y, Sandoval F, et al (2013) Results of phase II levetiracetam trial following acute head injury in children at risk for posttraumatic epilepsy. Epilepsia 54: 135-137.
-
Englander J, Bushnik T, Duong TT, Cifu DX, Zafonte R, et al. (2003) Analyzing risk factors for late posttraumatic seizures: a prospective, multicenter investigation. Arch Phys Med Rehabil 84: 365-373.
-
Basaldella L, Marton E, Bekelis K, Longatti P (2011) Spontaneous resolution of atraumatic intrauterine ping-pong fractures in newborns delivered by cesarean section. J Child Neurol 26: 1449-1451.





