International Journal of Neurology and Neurotherapy
Trigeminal Neuropathy as a Relapse in Behçet Disease
Gonçalo Cação*, Isabel Moreira, José Eduardo Alves, Fátima Farinha and Ernestina Santos
Neurology Department, Centro Hospitalar do Porto, Porto, Portugal
*Corresponding author:
Gonçalo Cação, Neurology Department, Centro Hospitalar do Porto, Largo do Professor Abel Salazar, 4099-001 Porto, Portugal, Tel: +351 912860834, Fax: +351 222 053 218, E-mail: goncalo.cacao@gmail.com
Int J Neurol Neurother, IJNN-3-044, (Volume 3, Issue 2), Case Report; ISSN: 2378-3001
Received: February 25, 2016 | Accepted: March 26, 2016 | Published: March 29, 2016
Citation: Cação G, Moreira I, Alves JE, Farinha F, Santos E (2016) Trigeminal Neuropathy as a Relapse in Behçet Disease. Int J Neurol Neurother 3:044. 10.23937/2378-3001/3/2/1044
Copyright: © 2016 Cação G, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
A 49 years old woman, diagnosed with Neuro-Behçet, was admitted with complains of numbness, aching and periods of electric shock-like pain in right side of the face. Associated with painful oral ulcers, anorexia, nausea and gait instability. Neurological examination revealed dysesthesia on right trigeminal nerve territory, horizontal-rotatory nistagmus on horizontal gaze bilateral with fast phase to the right and tandem instability. Brain MRI revealed new lesions. It was assumed a rhombencephalitis in the context of Neuro-Behçet relapse. Started on cyclophosphamide and methylprednisolone with symptoms resolution. Although brainstem involvement in Behçet disease is common, relapses with trigeminal neuropathy are very rare.
Keywords
Behçet disease, Neuro-Behçet syndrome, Trigeminal neuropathy, MRI
Introduction
Behçet disease (BD) is a chronic multisystem relapsing inflammatory disorder of unknown cause [1]. Neuro-Behçet syndrome (NBS) is defined as the occurrence of neurologic symptoms in a patient with BD that is not better explained by any other well-known systemic or neurologic disease [2,3]. The prevalence of NBS in BS is between 3% and 9% in non-selected large series [4]. The most common neurological presentation is a subacute meningoencephalitis, accounting for 75% of cases in NBS with parenchymal involvement [4]. Typical MRI acute lesions are hyperintense in T2,show enhancement in T1 and are often associated with oedema [5].
Case
A 49 years old woman with Behçet disease HLA-B51 positive with previous neurological involvement without sequelae and under treatment with azathioprine, was admitted with complains of numbness, aching and periods of electric shock-like pain in the right side of the face. Associated with painful oral ulcers, anorexia, nausea and gait instability. Neurological examination revealed dysesthesia on right trigeminal nerve territory, horizontal-rotatory nistagmus on horizontal gaze bilateral with fast phase to the right and tandem instability. Brain MRI revealed new brainstem lesions (Figure 1). It was assumed a rhombencephalitis in the context of NBS relapse. Treated with intravenous methylprednisolone pulses for 3 days and intravenous cyclophosphamide, with symptoms resolution. Discharged under treatment with oral prednisolone, presenting no further attacks.
.
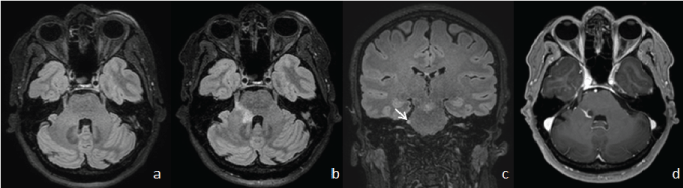
Figure 1: Axial 3D T2-weighted fluid-attenuated inversion recovery (FLAIR) images from April (a) and November; (b) show a "de novo" hyperintense lesion in the right posterior pons and right trigeminal root entry zone. 3D T2-weighted FLAIR image; (c) reveals thickening and hyperintensity in the cisternal segment of the right trigeminal nerve (white arrow). Post-gadolinium 3D T1-weighted turbo field echo (TFE) image; (d) shows partial peripheral enhancement of the right pontine lesion.
View Figure 1
Discussion
According to the International Classification of Headache Disorder [6], our case meets the criteria of painful trigeminal neuropathy attributed to other disorders. In NBS, brainstem relapses are relatively common and although reported in a few cases [7,8], relapses as a trigeminal neuropathy are very rare. Recommended treatment options for acute/sub-acute parenchymal attack is a course of corticosteroids, preferably intravenous methylprednisolone for 3-10 days followed by a maintenance oral corticosteroid for a few months (up to 6 months) [3]. Regarding disease modifying therapy, azathioprine is recommended as first line, with mycophenolate mofetil, methotrexate and cyclophosphamide being considered as alternatives [3,9]. As far as we know, no reported case of NBS with trigeminal neuropathy presented this perfect clinical and image findings correlation.
Authors' Conflicts of Interest
The authors declare no conflict of interest.
References
-
Krause I, Weinberger A (2008) Behçet's disease. Curr Opin Rheumatol 20: 82-87.
-
Peño IC, De las Heras Revilla V, Carbonell BP, Di Capua Sacoto D, Ferrer ME, et al. (2012) Neurobehçet disease: clinical and demographic characteristics. Eur J Neurol 19: 1224-1227.
-
Kalra S, Silman A, Akman-Demir G, Bohlega S, Borhani-Haghighi A, et al. (2014) Diagnosis and management of Neuro-Behçet's disease: international consensus recommendations. J Neurol 261: 1662-1676.
-
Saip S, Akman-Demir G, Siva A (2014) Neuro-Behçet syndrome. Handb Clin Neurol 121: 1703-1723.
-
Al-Araji A, Kidd DP (2009) Neuro-Behçet's disease: epidemiology, clinical characteristics, and management. Lancet Neurol 8: 192-204.
-
Headache Classification Committee of the International Headache Society (IHS) (2013) The International Classification of Headache Disorders, 3rd edition (beta version). Cephalalgia 33: 629-808.
-
Farah S, Al-Shubaili A, Montaser A, Hussein JM, Malaviya AN, et al. (1998) Behçet's syndrome: a report of 41 patients with emphasis on neurological manifestations. J Neurol Neurosurg Psychiatry 64: 382-384.
-
Studer U, Ruehe B, Waldegg G, Vajtai I, Escher R, et al. (2012) Atypical presentation of Behcet's disease with central nervous system involvement successfully treated with infliximab. Rheumatol Int 32: 1431-1435.
-
Diri E, Espinoza LR (2006) Neuro-Behçet's syndrome: differential diagnosis and management. Curr Rheumatol Rep 8: 317-322.





