International Journal of Neurology and Neurotherapy
Long-Term Deep Brain Stimulation for Parkinson's Disease is Associated with Progressive Reduction in Medication Utilization and Cost
Chandler E. Gill1, Elyne N. Kahn2, Aaron Bowman3,4, Thomas L. Davis3,5, Lily Wang6, Yanna Song6, Justin R. Smith7 and David Charles3*
1Department of Neurology, Loyola University Medical Center, USA
2Department of Neurosurgery, University of Michigan Health System, USA
3Department of Neurology, Vanderbilt University Medical Center, USA
4Vanderbilt Kennedy Center for Research on Human Development, USA
5Tennessee Valley VA Health System, USA
6Department of Biostatistics, Vanderbilt University Medical Center, USA
7Vanderbilt University Medical School, USA
*Corresponding author:
David Charles, Department of Neurology, Vanderbilt University Medical Center, 1161 21st Avenue South, Suite A-1106 Medical Center North, Nashville, TN 37232-2551, USA, Tel: 615-936-2596, Fax: 615-936-1229, Email: David.Charles@Vanderbilt.edu
Int J Neurol Neurother, IJNN-2-021, (Volume 2, Issue 1), Research Article; ISSN: 2378-3001
Received: February 12, 2015 | Accepted: February 20, 2015 | Published: February 23, 2015
Citation: Gill CE, Kahn EN, Bowman A, Davis TL, Wang L, et al,. (2015) Long-Term Deep Brain Stimulation for Parkinson's Disease is Associated with Progressive Reduction in Medication Utilization and Cost. Int J Neurol Neurother 2:021. 10.23937/2378-3001/2/1/1021
Copyright: © 2015 Gill CE, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Patients with Parkinson's Disease (PD) treated with Deep Brain Stimulation (DBS) typically reduce anti-PD medication use by 25-50% within 6 months of device placement, but whether the reduction is maintained long-term is less clear. We performed a medical record review of 18 patients with PD treated with DBS and 18 matched control patients treated with medications alone and compared their patterns of medication use. Dose and frequency were extracted from each progress note and converted to levodopa equivalent daily dose and cost. Participants were 20 men and 16 women, with an average age of 63.5 years and 12.9 years since the initial diagnosis of PD. Before initiation of DBS therapy, average daily medication dose increased by 61 levodopa equivalents per year; after implantation, daily dose decreased by 170 levodopa equivalents per year (p=0.0172). Annual cost associated with medical management of PD averaged $6661 ± 3894, which decreased by $2.93/day after implantation (p=0.0199). Our results demonstrate that reductions in anti-PD medication use continue for at least three years after DBS initiation, and generate significant cost savings.
Keywords
Clinical neurology, Movement disorders, Surgery/stimulation, Cost effectiveness research, Parkinson's disease/Parkinsonism
Abbreviations
DBS: Deep Brain Stimulation, IRB: Institutional Review Board, LEDD: Levodopa Equivalent Daily Dose, MED: Control Group (standard medical therapy), PD: Parkinson's Disease , STN: Subthalamic Nucleus, TDD: Total Daily Dose of PD Medication, USD: United States Dollar, UPDRS: Unified Parkinson's Disease Rating Scale
Introduction
Several classes of medication effectively treat the symptoms of Parkinson's disease (PD), including levodopa, dopamine agonists, catechol-O-methyl transferase inhibitors, and monoamine oxidase type B inhibitors, [1] but long-term use can cause motor fluctuations, dyskinesias and impulse control disorders. Despite optimal management, levodopa-associated motor complications develop in 50-75% of patients within seven years of diagnosis [2]. Clinical use of deep brain stimulation (DBS) has dramatically expanded since its approval in 1995. The therapy dramatically reduces motor symptoms [3] and patients can expect to reduce their daily dose of anti-PD medications by 25-50% within six months [1,4]. The longer-term patterns of medication use associated with adjunctive DBS are less clear. Reduction in total daily dose, if maintained, could potentially enhance quality of life and lessen the economic burden of the disease. We sought to determine whether reduction in medication dosages is sustained long-term, and to compare the rates of change in medication dose (and associated cost) before and after starting DBS.
Materials and Methods
Participants
With approval from the Vanderbilt IRB, a retrospective analysis of 36 patients was conducted. Billing and coding records from the Movement Disorders Clinic were queried for patients with idiopathic PD who had undergone bilateral DBS lead placement within the sub thalamic nucleus (STN; DBS+MED group, 18 patients), and age- and gender-matched PD patients who had not undergone DBS implantation (MED group, 18 patients). Exclusion criteria for both groups were clinical trial participation, previous surgical intervention for PD, or less than two clinic visits after implantation. A waiver of written informed consent was granted by the institutional IRB.
Data extraction
Our center uses an electronic medical record which includes all hospital and clinic records since 1991. Pre-1991 medical records are stored on campus in paper form, but we did not request these records because the first DBS surgery at Vanderbilt was not until 1995, and four years of pre-DBS medication data was felt to be satisfactory.
For each patient, trained research assistants reviewed physician and nurse notes associated with every visit to the Movement Disorders clinic and hospitalization, and extracted dose and frequency of each anti-PD medication. For DBS patients, device settings (amplitude, pulse width, and frequency) were also recorded. In the event that the dose of medication actually being used (as documented in clinic progress notes) differed from the dose prescribed by the physician, actual medication dose was used.
Statistical analysis
The levodopa Equivalent Daily Dose (LEDD) was calculated from Total Daily Doses (TDD) of the available PD medications using the following accepted formula:
LEDD=TDD(levodopa)+25×TDD(rotigitine)+100×TDD(pramipexole)+20×TDD(ropinirole)+0.5×TDD(amantadine) [4-6].
This value was multiplied by 1.15 if the patient took entacapone or selegiline because these agents act by sustaining or increasing plasma levels of levodopa [7]. For both study arms, patient age at first prescription of any anti-PD medication was used as a marker for disease onset because both patient report of symptoms onset and diagnosis itself proved unreliable and frequently unavailable. This allowed selection of control (MED) patients who were matched by disease duration. The duration of time between diagnosis and DBS surgery in the DBS+MED group was used to estimate a theoretical date on which control group patients would have received DBS if they had chosen to do so or been eligible ("date of DBS").
A random coefficient model, which falls into the more general class of mixed effects models, was used to estimate and compare rates of medication increase. This model included a systematic component modeling the mean trajectory for each group, and a random component (the random coefficients) modeling how each patient's trajectory varied about the group mean trajectory. To ensure reliable statistical estimation of the trajectory before "date of DBS", when the two groups did not differ in their trajectories, we pooled visits from both groups to estimate a single trajectory. Each model included LEDD as the outcome variable, fixed effects group (DBS+MED, MED), and three linear variables indicating linear trajectories before and after "date of DBS" (both groups before, DBS group after, MED group after). In addition, to account for correlations of repeated measurements from the same patient, we included random time and intercept effects for each patient. To separate out acute symptomatic effects of surgery, data was analyzed starting six months after implantation. LEDD values of 0 were assumed to represent temporarily holding of PD medications for detailed evaluation or preoperative assessment, and were excluded. To improve accuracy of the results, we used the Kenward-Rogers adjusted degrees of freedom solution for statistical inference, an approach specifically proposed for small sample settings [8].
To characterize change in DBS parameters over time, a linear regression model including pulse width, amplitude and frequency was fitted for each patient. The slope of the model estimates parameter annual rates of change, which were compared with the Wilcoxon signed rank test.
Wholesale medication costs were taken from the 2008 edition of the Red Book of Pharmaceutical Costs. This was necessary because several patients had received transdermal rotigitine, which was briefly available in 2008. For medications that were available in both branded and generic formulations, the cost of the generic was used. When multiple generic formulations were available, the least expensive option was used. Per-pill cost was multiplied by the daily frequency of that medication for each clinic visit, and the random coefficient model was used with average cost as the outcome variable.
Results
The records of 186 patients were reviewed to enroll 36 participants (18 in each arm). The participants were 20 men and 16 women with an average age of 63.5 years and disease duration of 12.9 years (Table 1). The average duration of clinic follow-up across all participants was 12.08 ± 6.24 years and there were no differences in baseline characteristics between groups. Patients in the DBS+MED arm were followed an average of 2.83 ± 1.2 years since device implantation.
![]()
Table 1: Patient demographic information and clinical characteristics
View Table 1
Figure 1 demonstrates the change in medication use for the two study groups. Before surgery, the rate of change was similar between groups (p=0.2419), averaging an increase of 61 levodopa equivalents per year (Table 2). The average daily dose at the time of DBS implantation was 1041.4 units. Overall medication dosages were reduced immediately following device programming and continued to decline, by an average of 170 units per year (p=0.0172). In contrast, patients in the MED-only arm required progressively higher doses of medications (average annual increase of 93 units after theoretical "date of DBS", p=0.6642) for symptom control.
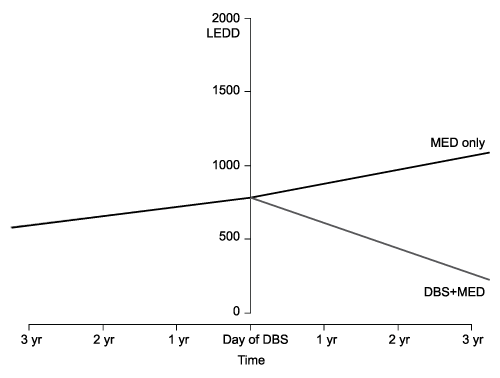
Figure 1: Change in Levodopa Equivalent Daily Dose (LEDD) compared between patients treated with anti-PD medications alone (MED) versus
medications with adjunctive DBS (DBS + MED)
View Figure 1
![]()
Table 2: Estimated rate of change per year for MED and DBS + MED groups.
View Table 2
The annual cost of anti-PD medication in patients at the time of DBS implantation was $6661 ± 3894 (Table 2). Before initiation of DBS, the daily cost was similar between groups and increased by an average of $1.34 per year (Figure 2). In patients who did not receive DBS, daily cost continued to increase by a similar rate ($1.39, p=0.9662). In patients who chose to receive DBS, the daily cost after implantation decreased by an average of $2.93 per year (p=0.0199).
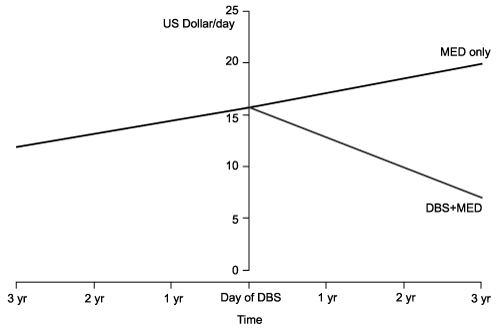
Figure 2: Change in daily cost of medication use compared between patients treated with anti-PD medications alone (MED) or medications with
adjunctive DBS (DBS + MED)
View Figure 2
Device stimulation parameters are presented in Table 3. Briefly, the mean amplitude was 1.41V which increased by an average of 0.76 per year. The mean frequency was 135.74 Hz and increased by 7.42 Hz annually. The mean pulse width was 66.89µs and increased by 6.34µs annually.
![]()
Table 3: Estimated annual change in STN stimulation parameters.
View Table 3
Discussion
We analyzed patterns of long-term medication use in PD patients treated with deep brain stimulation in addition to standard medical therapy, and compared them to patients on medication alone. STN DBS resulted in a significant decrease in medication use, and not only was that benefit sustained long-term, but in fact, the gap between the groups continued to widen while the therapy was continued. Patients who received DBS also paid significantly less for medications at six months and these cost benefits were similarly compounded over time.
Although a rapid reduction in medication dose has been documented [1,4], the continued divergence between the groups was unforeseen. We suggest several possible explanations. First and foremost, the complications associated with high doses of PD medications are common and disabling. When treatment adjustments are needed, many clinicians prefer to up titrate stimulation parameters rather than medication dose to avoid these complications. In addition, the clinical effect of stimulation itself is immediately evident and the side effects are mild and resolve after adjustment of device settings, so physicians have the ability to assess the patient's response to several "doses" within a single clinic visit, whereas a similar approach to medication titration would take several months. This is occasionally reinforced by patients, who may specifically request device adjustment rather than a change in medication out of concern for high medication costs, side effects, or the impracticality of taking a medication dosed multiple times per day. Finally, the continued widening of the gap between DBS and standard therapy groups could be explained by a potential disease-modifying effect, such as stabilization of motor symptoms or delay of motor fluctuations [9]. To date, no prospective clinical trials have attempted to test this theory, but studies in animal models [10,11] and humans [12] have yielded intriguing results.
There are several important limitations to this study. First, we were not able to obtain data on medication brands used by individualized patients, and we did not consider the effects of inflation in our analysis, instead using least expensive 2008 generic prices for all calculations. While this simplification changes our numbers, it presumably affects all data equally and would not change the significance of our findings. Second, we could not exclude patients with presentations that would have made DBS relatively contraindicated (e.g., predominantly axial symptoms, prominent neuropsychiatric features, or suboptimal response to levodopa), because these findings were inconsistently documented and our center did not routinely perform standardized rating scales (such as UPDRS) during the period of interest. If the control arm did include a disproportionate number of these patients, marked differences in baseline characteristics would be present (including baseline pattern of medication utilization). Encouragingly, we compared baseline characteristics and medication use between the two study groups before DBS implantation and found no differences in rate of dose increase or cost. The final limitation is the small sample size, and we acknowledge the need for replication of these results. That our data achieved statistical significance despite the small sample underscores the dramatic treatment effect.
Our results demonstrate an immediate reduction in total medication dose and cost associated with initiation of STN DBS, and also that this benefit continues for several years. The degree and duration of medication reduction is important, because large and frequent doses of levodopa are associated with earlier onset of severe motor fluctuations and greater disability. These findings may also be relevant to target selection, as sub thalamic and pallidal stimulation have similar efficacy and risk profiles, but STN stimulation results in greater medication reduction [13]. It is important to note that surgery itself is expensive, and likely not entirely offset by reduced medication costs. However, even partially offset costs may be welcome for some patients who need DBS but are already facing other economic hardships from their PD, such as loss of employment and reliance on paid caregivers. Perhaps more important than cost, the ability to meaningfully reduce total medication dose for years may delay or reduce complications of therapy, in turn providing a higher quality of life, less economic burden, and improved treatment compliance. This study is small and exploratory, and should be confirmed in a larger retrospective analysis making use of electronic medical record technology, or prospectively, as a secondary endpoint in a large randomized controlled trial.
Acknowledgments and Support
This study was supported in part by the Vanderbilt CTSA grant UL1 RR024975/UL1 TR000445 from the National Center for Research Resources, National Institutes of Health. No funding agency, medical device manufacturer, or pharmaceutical company had any role in data collection, management, analysis, or interpretation of the data or in preparation, review, or approval of the manuscript.
Conflict of Interest
Vanderbilt University has received income from grants or contracts with Medtronic, Allergan, Ipsen, Merz, UCB, and Teva for educational or research programs and research led Dr. Charles. Dr. Charles receives income from Medtronic, Allergan, Ipsen, and the Alliance for Patient Access for education and consulting services. Ms. Gill, Dr. Kahn, Dr. Bowman, Dr. Davis, Mr. Smith, Dr. Wang and Ms. Song have no conflicts to disclose.
References
-
Charles PD, Padaliya BB, Newman WJ, Gill CE, Covington CD, et al. (2004) Deep brain stimulation of the subthalamic nucleus reduces antiparkinsonian medication costs. Parkinsonism Relat Disord 10: 475-479.
-
Rajput AH, Fenton ME, Di Paolo T, Sitte H, Pifl C, et al. (2004) Human brain dopamine metabolism in levodopa-induced dyskinesia and wearing-off. Parkinsonism Relat Disord 10: 221-226.
-
Krack P, Batir A, Van Blercom N, Chabardes S, Fraix V, et al. (2003) Five-year follow-up of bilateral stimulation of the subthalamic nucleus in advanced Parkinson's disease. N Engl J Med 349: 1925-1934.
-
Vingerhoets FJ, Villemure JG, Temperli P, Pollo C, Pralong E, et al. (2002) Subthalamic DBS replaces levodopa in Parkinson's disease: two-year follow-up. Neurology 58: 396-401.
-
Herzog J, Volkmann J, Krack P, Kopper F, Pötter M, et al. (2003) Two-year follow-up of subthalamic deep brain stimulation in Parkinson's disease. Mov Disord 18: 1332-1337.
-
LeWitt PA, Boroojerdi B, MacMahon D, Patton J, Jankovic J (2007) Overnight switch from oral dopaminergic agonists to transdermal rotigotine patch in subjects with Parkinson disease. Clin Neuropharmacol 30: 256-265.
-
Khor SP, Hsu A (2007) The pharmacokinetics and pharmacodynamics of levodopa in the treatment of Parkinson's disease. Curr Clin Pharmacol 2: 234-243.
-
Kenward MG, Roger JH (1997) Small sample inference for fixed effects from restricted maximum likelihood. Biometrics 53: 983-997.
-
Charles PD, Gill CE, Davis TL, Konrad PE, Benabid AL (2008) Is deep brain stimulation neuroprotective if applied early in the course of PD? Nat Clin Pract Neurol 4: 424-426.
-
Temel Y, Visser-Vandewalle V, Kaplan S, Kozan R, Daemen MA, et al. (2006) Protection of nigral cell death by bilateral subthalamic nucleus stimulation.Brain Res 1120: 100-105.
-
Wallace BA, Ashkan K, Heise CE, Foote KD, Torres N, et al. (2007) Survival of midbrain dopaminergic cells after lesion or deep brain stimulation of the subthalamic nucleus in MPTP-treated monkeys. Brain 130: 2129-2145.
-
Simonin C, Tir M, Devos D, Kreisler A, Dujardin K, et al. (2009) Reduced levodopa-induced complications after 5 years of subthalamic stimulation in Parkinson's disease: a second honeymoon. J Neurol 256: 1736-1741.
-
Follett KA, Weaver FM, Stern M, Hur K, Harris CL, et al. (2010) Pallidal versus subthalamic deep-brain stimulation for Parkinson's disease. N Engl J Med 362: 2077-2091.





