International Journal of Neurology and Neurotherapy
Recurrent Ischemic Strokes and Headaches Originating from Lambl's Excrescences: A Case-Report
Oana Dumitrascu* and Evgeny Tsimerinov
Department of Neurology, Cedars-Sinai Medical Center, Los Angeles, CA, USA
*Corresponding author:
Oana Dumitrascu, Department of Neurology, Cedars-Sinai Medical Center, 127 S. San Vicente Blvd, 6th floor, Los Angeles, CA 90048, USA, Tel: 310-423-6472, Fax: 310-423-0148, E-mail: Oana.dumitrascu@cshs.org
Int J Neurol Neurother, IJNN-2-019, (Volume 2, Issue 1), Original Case-Report; ISSN: 2378-3001
Received: January 11, 2015 | Accepted: January 29, 2015 | Published: January 31, 2015
Citation: Dumitrascu O, Tsimerinov E (2015) Recurrent Ischemic Strokes and Headaches Originating from Lambl's Excrescences: A Case-Report. Int J Neurol Neurother 2:019. 10.23937/2378-3001/2/1/1019
Copyright: © 2015 Dumitrascu O, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Determining recurrent stroke etiology and subsequent therapeutic approaches is an important, but not always straightforward task. Lambl's Excrescences (LE) are cardiac valve strands that can be a source of recurrent cerebral ischemic events. We report the case of a 60 year old female that was seen in neurologic consultation for recurrent ischemic strokes. The patient developed migraine headache with complex auras at the age of 59. She reported three admissions for ischemic strokes in the past year. Stroke work-ups were unrevealing. The patient remained on daily Aspirin. Upon current admission, a brain MRI showed a combination of sub acute and chronic infarcts in diverse brain areas bilaterally. Further diagnostic evaluation revealed a relatively unremarkable CT head and neck angiogram. Transcranial Doppler (TCD) showed increased pulsatility index throughout the insonated vessels. Transesophageal echocardiogram (TEE) showed a trileaflet aortic valve with a 10 mm long thin fibrin strand prolapsing into the left ventricle outflow tract in diastole, meeting echocardiographic criteria for an LE. The patient refused anticoagulation and surgical intervention. She opted instead for a combination of two antiplatelet agents. Recurrent cerebral infarcts presenting concurrently with late-age onset migraine with aura should raise a clinical suspicion of cardiogenic valvular etiology. The use of TEE in evaluating patients with unexplained recurrent stroke is imperative so that LE is not missed. Anti-platelet agents, anti-coagulants, and cardiothoracic surgical intervention are proposed in the literature for the management of long-term complications associated with LE. Asymptomatic patients should be monitored, counseled, and made aware of LE complications, neurological symptoms, and alarm signals. Migraine headaches associated with LE should raise a red flag and prompt treatment with anti-platelet agents.
Keywords
Ischemic stroke, Migraine headache with aura, Cardiac valvular disease
Introduction
Recurrent ischemic stroke is still a challenge for the modern neurologist. Rare cardiac culprits include Lambl's Excrescences (LE), which are native cardiac valve strand variants. LE is associated with cerebral thromboembolism, recurrent cerebral infarcts, and transitory ischemic attacks which are more common in younger patients [1]. Microemboli coming from LE have been reported in association with recurrent migraine headaches [2]. Current data on LE cerebral complications and their management is limited. The treatment selection criteria and indications are variable and not evidence-based [3].
Case Reports
We report the case of a 60 year old right-handed female seen in neurologic consultation for recurrent stroke management. The patient presented with acute onset of binocular blurry vision, and an abnormal left peri-ocular sensation that started during casual conversation with a family member, and lasted about 2 hours. The event was associated with slurred speech and a persistent frontal headache. Upon arrival to our emergency department, visual and speech disturbances were resolved but a moderate headache remained. An initial neurological examination was unremarkable. A brain MRI reveals a subacute infarct in the left parietal lobe with petechial hemorrhages, old infarcts in the bilateral centrum semiovale, and chronic right occipital infarct (Figure1). The patient reported three prior admissions for acute stroke management. The first admission was for ataxia and visual changes, five months prior to the current presentation. Two months later, the patient was admitted for sudden-onset of non-fluent aphasia and right upper extremity weakness. Finally, she was admitted for right upper and lower extremity weakness, one month prior to the current presentation. Stroke work-ups performed during all three admissions did not reveal any specific causes for the stroke recurrences. She was left with multiple residual neurological symptoms after each event, including mild subjective gait abnormality which did not require assistive devices, intermittent episodes of stuttering speech, transitory visual symptoms (difficulties focusing on objects and reading because of "jumping" letters, and intermittent left-sided hemianopsia), and abnormal skin sensations around the left eye. In addition, the patient reported recurrent unilateral throbbing headaches of a mild intensity lasting hours, sometimes in association with visual and sensory symptoms. Despite recurrent strokes, the patient was prescribed Aspirin 162 mg daily.
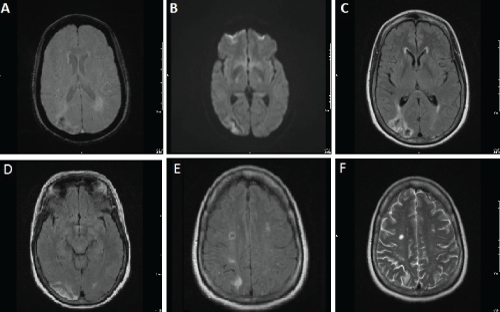
Figure 1: Brain MRI without contrast at presentation
Subacute right parietal infarct with petechial hemorrhage is illustrated on
DWI (A), SWI (B) and FLAIR (C) images. Chronic right occipital (D-FLAIR
sequence), old bilateral corona radiata (E- FLAIR sequence) and right frontal
lobe (F- T2W sequence) infarcts are identified.
View Figure 1
Upon arrival to our emergency department, a medical history was remarkable for treated controlled hypertension, untreated obstructive sleep apnea, dyslipidemia, left upper extremity DVT in 2005 of unknown etiology (was on warfarin for 2 years), and bilateral knee osteoarthritis. Family history was positive for cardiac ischemic disease and negative for migraine headaches. Besides Aspirin 162 mg daily, the patient was also taking Lipitor 10 mg daily and two anti-hypertensive agents to maintain good blood pressure control.
Outside hospital medical records showed a normal Transthoracic Echocardiogram (TTE) and negative work-up for some hypercoagulable disorders. Although the majority of her co-morbidities were taken into consideration as independent stroke risk factors, we decided to conduct further investigation into her recurrent and frequent cerebrovascular events. Serologic work-up revealed normal cell blood count, normal complete metabolic profile, normal TSH, HbA1c, and hypercoagulable profile (consisting of unremarkable anti cardiolipin antibodies, prothrombin time, INR, lupus anticoagulant, protein C and S activities, activated protein C resistance, factor V Leiden, homocysteine, beta 2 glycoprotein, fibrinogen), and an LDL of 112 mg/dl.
A CT angiogram of the head and neck revealed minimal atherosclerotic changes in the right greater than in the left internal carotid artery at the high cervical level; a moderate irregularity in the right A1 segment and mild to moderate narrowing bilaterally in the M1-M2 junctions. No aneurysm or dissection was identified in the anterior circulation. Evaluation of the posterior circulation demonstrated a dominant right vertebral artery and a fetal origin of the right posterior cerebral artery. No flow-limiting stenosis, aneurysm, or dissection was identified in the posterior circulation. A large mixed soft tissue and fat-containing mass was incidentally noticed on the CT angiogram in the left neck. The mass biopsy revealed a fibrolipoma.
As no clear causes for the recurrent strokes were currently identified, and initial cardiac work-up was negative at the other institutions, we elected to conduct a TEE. The TEE revealed a trileaflet aortic valve with mildly calcified aortic cusps and a 10 mm long thin fibrin strand on the aortic valve prolapsing into the left ventricle outflow tract in diastole, strongly suggestive of Lambl's excrescences, based on echocardiographic criteria (Figure 2). No other valvular, atrial or ventricular abnormalities were identified. There were no thrombi and absent intracardiac shunts. A moderate (2-4 mm) atheroma was seen in the ascending aorta.
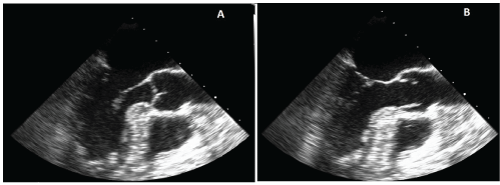
Figure 2: Transesophageal echocardiogram view of giant Lambl's
excrescences deriving from the aortic valve (A- valve is closed; B- valve is
opened)
View Figure 2
A cardiothoracicteam was consulted to address management of the giant LE. The patient refused anticoagulation treatment and surgical intervention. She opted instead for management with two antiplatelet medications, Aspirin 81 mg and Clopidogrel 75mg, daily. The patient was discharged home in stable condition. A nine-month follow-up confirmed that the patient remained free from headaches and stroke recurrence.
Discussion
Recurrent cerebral infarct scan arise from endovascular plugs, vascular stenosis and vascular malformations, coagulation pathway dysfunctions due to genetic defects, or autoimmune disorders. One of the most common sources is cardiogenic, arising from hemodynamic instability due to structural and/or diverse cardiac valve disorders [4,5]. Valvular strands contribute to systemic thromboembolisms and cerebrovascular pathology [2,3,5-9]. In daily clinical practice the terms LE, cardiac papillary fibroelastoma, and valvular strands are sometimes interchangeable based on echocardiographic characterization alone; however, their management and prognosis should be individualized [3].
LE are usually thin (1 mm) and long (4-10 mm), mobile, filiform projections from native cardiac valves, more commonly seen on mitral than on aortic valve leaflets. They consist of a collagenous structure (elastic fibers surrounded by loose connective tissue), which gathers subsequent fibrin deposition [1,8]. Little is known about the exact prevalence and incidence of cerebral embolism from LE because of their rare occurrence and possible under-recognition. Standardized diagnostic criteria are not established due to paucity of retrospective and prospective clinical trials. The mechanism of recurrent cerebral infarcts in patients with LE, in absence of other risk factors, has been explained by the formation of thrombi along the endothelial surface [3]. The influence of LE size, morphology and location on these thromboembolic events has not been elucidated [1].
While TTE can be used as a screening tool for cardiac sources of cerebral embolism, TEE is necessary and remains the gold standard in determining the etiology of multiple recurrent strokes. Echocardiographic criteria of LE are described in the literature [3,5,9]. Multi-slide computed tomography can be used as an alternative diagnostic tool if a TEE cannot be performed [10].
Current scientific literature does not provide strong recommendations for stroke prevention in patients with LE [1], emphasize that asymptomatic patients do not require treatment. Other authors suggest that antiplatelet agents are indicated after the first stroke, while anticoagulation or cardiothoracic intervention should be reserved for recurrent events [3]. Controversially, Azis and Baciewitz strongly support anticoagulation as an initial intervention, followed by LE surgical excision if stroke prevention is not achieved [6].
Migraine headaches are known to be associated with intracardiac shunts and structural heart anomalies [11]. Migraine headaches with aura and amaurosis fugax have been reported as a first presentation of cerebral ischemia, preceding the stroke manifestations in patients with LE [2]. No clinical or scientific studies are available to guide headache management in these cases. Some clinicians support the prevention of migraine headaches with antithrombotic medications based on a presumed mechanism of micro-emboli originating from LE [2].
Our case report suggests that the presentation of multiple recurrent strokes in concurrence with late-age onset migraine with aura should raise a clinical suspicion of cardiogenic valvular etiology. Early TEE use is strongly indicated to diagnose cardiac valvular strands such as LE in these patients. Even though our experience and data are very limited, we feel safe managing our patient on the combination of two antiplatelet agents for stroke and migraine prevention. Further prospective clinical trials should be conducted to establish benefits of different therapeutic options and better management guidance once diagnosis of LE is made in patients with recurrent strokes.
References
-
Roberts JK, Omarali I, Di Tullio MR, Sciacca RR, Sacco RL, et al. (1997) Valvular strands and cerebral ischemia. Effect of demographics and strand characteristics. Stroke 28: 2185-2188.
-
Liu RZ, Yu SY, Li Y (2012) Migraine-like headache and ischemic strokes in two patients with Lambl's excrescences. Chin Med J (Engl) 125: 3346-3348.
-
Wolf RC, Spiess J, Vasic N, Huber R (2007) Valvular strands and ischemic stroke. Eur Neurol 57: 227-231.
-
Wu TY, Gerber IL, Roxburgh RH (2013) Thrombo-embolic cerebral infarction secondary to giant Lambl's excrescence. J Clin Neurosci 20: 1632-1634.
-
Sun JP, Asher CR, Yang XS, Cheng GG, Scalia GM, et al. (2001) Clinical and echocardiographic characteristics of papillary fibroelastomas: a retrospective and prospective study in 162 patients. Circulation 103: 2687-2693.
-
Aziz F, Baciewicz FA Jr (2007) Lambl's excrescences: review and recommendations. Tex Heart Inst J 34: 366-368.
-
Kalavakunta JK, Peddi P, Bantu V, Tokala H, Kodenchery M (2010) Lambl's excrescences: a rare cause of stroke. J Heart Valve Dis 19: 669-670.
-
Nakahira J, Sawai T1, Minami T1 (2014) Pathologic examination of Lambl's excrescence. J Cardiothorac Vasc Anesth 28: e3-4.
-
Leitman M, Tyomkin V2, Peleg E2, Shmueli R2, Krakover R2, et al. (2014) Clinical significance and prevalence of valvular strands during routine echo examinations. Eur Heart J Cardiovasc Imaging 15: 1226-1230.
-
Rbaibi A, Bonnevie L, Guiraudet O, Godreuil C, Martin D, et al. (2002) [Importance of transesophageal echocardiography and computed tomography in the differential diagnosis of a case of papillary fibroelastoma revealed by a neurologic accident]. Arch Mal Coeur Vaiss 95: 601-605.
-
Schwedt TJ (2009) The migraine association with cardiac anomalies, cardiovascular disease, and stroke. Neurol Clin 27: 513-523.





