International Journal of Neurology and Neurotherapy
Cortical Diffusion Restriction as the Single Abnormality on MRI in Creutzfeldt-Jakob disease
Johnny Samijn*, Alisha Godschalk, Rezan Demir and Esther Brusse
Department of Neurology, Maasstad Hospital, Netherlands
*Corresponding author:
Johnny Samijn, Department of Neurology, Maasstad hospital, Maasstadweg 21, 3079 DZ, Rotterdam, Netherlands, Tel: 0031102911457, Fax: 0031102911014, E-mail: Samijnj@maasstadziekenhuis.nl
Int J Neurol Neurother, IJNN-2-016, (Volume 2, Issue 1), Case Report; ISSN: 2378-3001
Received: October 28, 2014 | Accepted: January 09, 2015 | Published: January 12, 2015
Citation: Samijn J, Godschalk A, Demir R, Brusse E (2015) Cortical Diffusion Restriction as the Single Abnormality on MRI in Creutzfeldt-Jakob disease. Int J Neurol Neurother 1:016. 10.23937/2378-3001/2/1/1016
Copyright: © 2015 Samijn J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Introduction
Creutzfeldt-Jakob disease (CJD) is a rare neurodegenerative disease characterized by rapidly progressive dementia, ataxia and myoclonus. MRI is an important tool in discriminating CJD from other dementias. Among mimics of CJD are rapidly evolving Alzheimer's disease, vascular dementia, frontotemporal dementia and paraneoplastic or immune-mediated limbic encephalitis. A CJD diagnosis can be missed and strong clinical suspicion is not always confirmed on autopsy [1]. Typical imaging findings are white matter abnormalities in the thalamus, the striatum and progressive atrophy [2,3]. We present two cases of CJD, both with atypical onset, in which the single abnormality on MRI consisted of a diffusion restriction (diffusion-weighted imaging) of part of the neocortex.
Keywords
Creutzfeldt-Jakob disease, Sporadic CJD, Magnetic resonance imaging, Diffusion MRI.
Case 1
A 62-year-old man presented with unsteadiness of gait, tingling in the feet and progressive cognitive impairment. On neurological examination the patient was dysarthric, smooth eye pursuit was impaired, there were sensory disturbances in the feet, extensor plantar responses and gait ataxia. A limbic encephalitis with polyneuropathy was suspected. Standard MRI sequences - performed by a 1,5 T Siemens scanner (axial T2 TSE, T2 BLADE, TIRM DF, axial T1 MPRAGE) - showed no abnormalities. Serological testing for paraneoplastic antibodies, including anti-Hu, proved negative. Repeated imaging one month later showed DWI hyperintensity of the cortex in the temporal, parietal and occipital region without pathology of the white matter (Figure 1). Background pattern on EEG was slow but without triphasic complexes. Cerebrospinal fluid showed an elevated tau level of 2400 ng/l and slight 14-3-3 protein positivity. The patient developed myoclonus and a diagnosis of CJD was made shortly before death. At autopsy sporadic CJD was confirmed.
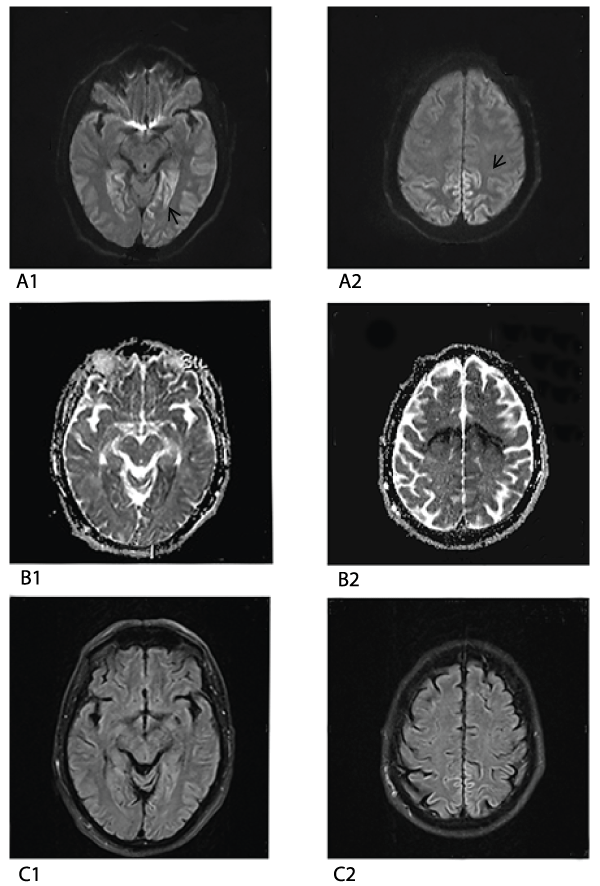
Figure 1: MRI in axialplane; DWI (A1,2): hyperintensity of temporal and
occipital cortex (arrows). ADC map (B1,2): hypointensity of cortex. TIRM DF
(C1,2): mild hyperintensity of cortex.
View Figure 1
Case 2
A 72-year-old man presented with apathy, aphasia and unilateral weakness. There was a history of hypertension and an initial diagnosis of stroke was made. Standard MRI T2 sequencing showed a small, subcortical white matter lesion. The patient developed progressive ataxia and cognitive symptoms which were incompatible with the initial diagnosis. The EEG demonstrated a slow wave pattern with generalized triphasic complexes. Cerebrospinal fluid showed an elevated tau level of 9400 ng/l and 14-3-3 protein positivity. DWI cortical hyperintensity of the right temporal and occipital lobe was seen on a second MRI (Figure 2). The patient was diagnosed with probable CJD and died soon afterwards. Autopsy was not allowed.
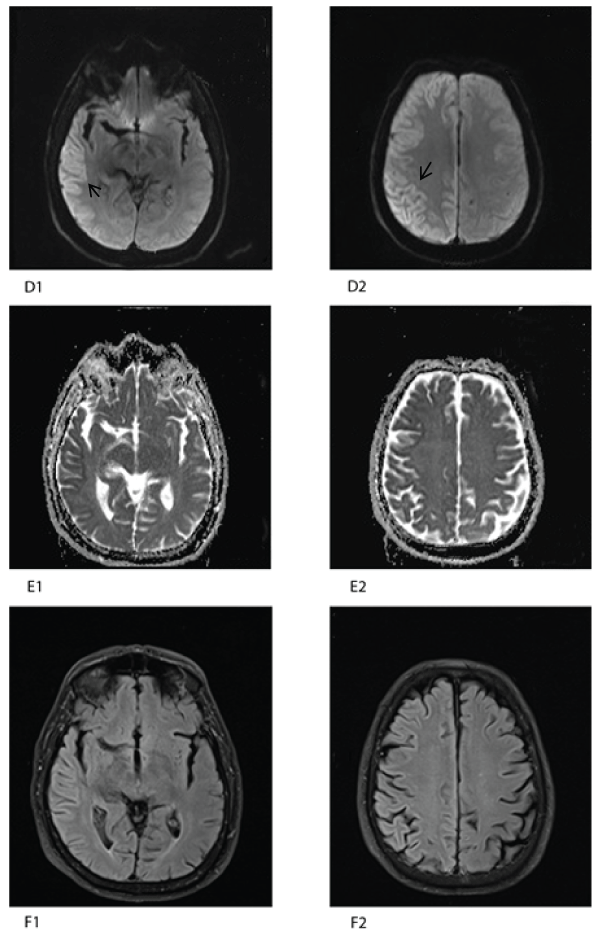
Figure 2: MRI in axialplane; DWI (D1,2): hyperintensity of cortex right
hemisphere (arrows). ADC map (E1,2): hypointensity of cortex. TIRM DF
(F1,2): mild hyperintensity of cortex.
View Figure 2
Discussion
An early diagnosis of probable CJD can be difficult if signs are mild or atypical. Early differentiation from other causes of dementia is vital for determining prognosis and preventing unnecessary investigations. In case number one an anti-Hu paraneoplastic syndrome was considered more likely than CJD because of a new sensory neuropathy and cerebellar symptoms in a heavy smoker. The second patient was diagnosed with cerebrovascular disease at first. MRI led to a diagnosis of probable CJD. Diffusion restriction of the cortex was the single abnormality in 24% of cases in a study focussing on interrater characteristics [4]. DWI is found to have better sensitivity and specificity compaired to other T2 weighted sequences in most studies [5]. New MRI criteria for CJD reflect the higher sensitivity of DWI compaired to FLAIR/TIRM DF [6]. Since many standard MRI scanning protocols do not include DWI, cortical diffusion pathology can easily be missed so given the right index of suspicion the sequence should be included.
References
-
Chitravas N, Jung RS, Kofskey DM, Blevins JE, Gambetti P, et al. (2011) Treatable neurological disorders misdiagnosed as Creutzfeldt-Jakob disease. Ann Neurol 70: 437-444.
-
Lee H, Cohen OS, Rosenmann H, Hoffmann C, Kingsley PB, et al. (2012) Cerebral white matter disruption in Creutzfeldt-Jakob disease. AJNR Am J Neuroradiol 33: 1945-1950.
-
Meissner B, Kallenberg K, Sanchez-Juan P, Krasnianski A, Heinemann U, et al. (2008) Isolated cortical signal increase on MR imaging as a frequent lesion pattern in sporadic Creutzfeldt-Jakob disease. AJNR Am J Neuroradiol. 2008 29: 1519-1524.
-
Young GS, Geschwind MD, Fischbein NJ, Martindale JL, Henry RG, et al. (2005) Diffusion-weighted and fluid-attenuated inversion recovery imaging in Creutzfeldt-Jakob disease: high sensitivity and specificity for diagnosis. AJNR Am J Neuroradiol 26: 1551-1562.
-
Fujita K, Harada M, Sasaki M, Yuasa T, Sakai K, et al. (2012) Multicentre multiobserver study of diffusion-weighted and fluid-attenuated inversion recovery MRI for the diagnosis of sporadic Creutzfeldt-Jakob disease: a reliability and agreement study. BMJ Open 30: 2: e000649.
-
Vitali P, Maccagnano E, Caverzasi E, Henry RG, Haman A, et al. (2011) Diffusion-weighted MRI hyperintensity patterns differentiate CJD from other rapid dementias. Neurology 76: 1711-1719.





