Journal of Dermatology Research and Therapy
Two-Year Evaluation of Either Bilobed Flap or Full Thickness Skin Graft as a Closure Technique of the Nasal Tip
Marius A Kemler*
Department of Plastic Surgery, Martini Hospital Groningen, The Netherlands
*Corresponding author:
Marius A Kemler, Department of Plastic Surgery, Martini Hospital Groningen, PO Box 3000, 9700 RM Groningen, The Netherlands, Tel: +31505245980, E-mail: M.Kemler@mzh.nl
J Dermatol Res Ther, JDRT-2-038, (Volume 2, Issue 6), Original Article; ISSN: 2469-5750
Received: July 04, 2016 | Accepted: November 21, 2016 | Published: November 23, 2016
Citation: Kemler MA (2016) Two-Year Evaluation of Either Bilobed Flap or Full Thickness Skin Graft as a Closure Technique of the Nasal Tip. J Dermatol Res Ther 2:038. 10.23937/2469-5750/1510038
Copyright: © 2016 Kemler MA. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: There is no clarity if a bilobed flap is the best treatment of choice for reconstruction of nasal tip defects.
Method: The nose of twenty patients was photographed 2 years after surgical excision of skin cancer and closure either with a bilobed flap (n = 7) or a full thickness skin graft (n = 13). Photographs were assessed by 2 dermatologists, 2 plastic surgeons and 2 non medically trained individuals, applying the POSAS scale.
Results: There were no significant differences between opinions of the two techniques. Overall, on a scale from 0 to 10 where 0 means 'no visual abnormalities' the bilobed flap scored 2.22 versus 2.33 for the skin graft. Where medical consultants preferred the bilobed flap, non medical individuals favored the skin graft closure.
Conclusion: We found no evidence to support the textbook statement that the bilobed flap "excels" for reconstruction of defects less than 1.5 cm around the nasal tip.
Keywords
Skin cancer, Local flap, Skin graft
Introduction
Skin cancer frequently occurs at or around the tip of the nose. Repair of small surface defects after resection of skin cancer therefore form an everyday problem to the plastic surgeon. The nose has a number of characteristics that make it unique when planning for reconstruction of surgical defects. The skin over the lower third of the nose has limited mobility and, therefore, cannot be easily recruited for closure of anything but small defects. In addition, the texture and color of this skin are so unique that neither distant nor nearby skin can always provide a good match. The only local skin that will restore the specialized color, texture and skin thickness of the nasal tip and ala is the skin of the nose itself.
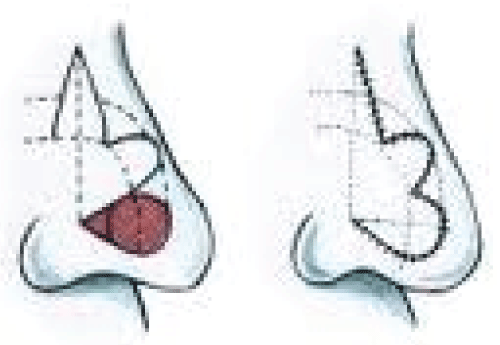
The rotation flap most frequently used and promoted to reconstruct small tissue defects on the nose is the bilobed flap. As described by Esser, et al. [1,2] each flap was the same size, and the lobes were oriented 90 degrees to each other. Zimany, et al. [3] modified this in 1953 by designing the second flap smaller than the first flap. Zitelli, et al. [4] kept the second flap smaller and reduced the angle between the two flaps to approximately 50 degrees, preventing buckling and large dog ears. This flap is used when sufficient tissue laxity is available to close the donor site primarily. When used in distal nasal reconstruction, the defect should be less 1.5 cm in diameter. The primary flap is the same size as the adjacent defect, and a second flap adjacent to the primary flap is about half the width of the primary flap. The primary flap then rotates into the defect, the secondary flap rotates into the primary flap donor site, and the secondary flap donor site is closed primarily (Figure 1).
Skin grafts are another alternative but, like local flaps, must be chosen with consideration to their limitations. Equally important to successful reconstruction is the effect of wound healing on grafts and flaps. Although a skin graft donor site may be chosen preoperatively because it matches in color and texture, the transient ischemia associated with skin graft take causes unpredictable color and texture changes after transfer. Postoperatively, skin grafts are tipically shiny, atrophic, and hypopigmented or hyperpigmented. Also, a skin graft may shrink but rarely pincushions. Thus a shiny skin graft will stand out as a mismatched patch if used within the pitted, sebaceous tip where a flap would be a better choice. Skin flaps, in contrast, maintain their donor characteristics but have a tendency to pincushion and elevate above the surface of the defect, appearing as a bulge above adjacent normal skin. Taken all in all, there is no clarity if a bilobed flap is the best treatment of choice for reconstruction of nasal tip defects. The aim of the present study was to assess two years postoperatively, which technique to reconstruct the tip of the nose is leads to the best appearance according to the opinion of dermatologists, plastic surgeons and nonmedically trained individuals.
Patients and Methods
Twenty consecutive patients were included, who had undergone reconstruction of a nasal tip defect of no more than 1.5 cm at its greatest diameter, after surgical excision of skin cancer two years earlier. Patients were randomly sent to one of two types of surgeons, one type always using the bilobed flap and the other type always applying a preauricular skin graft. In this way, patients were randomly appointed to one of the two treatnments, while the personal preference of the surgeon could not introduce bias. In this way, after surgical excision of skin cancer, the defect was closed with a bilobed flap in 7 cases and by a full thickness skin graft in 13 cases. All skin grafts were taken from preauricular skin with primary wound closure: all these scars healed perfectly.
Two years postoperatively, the nose of these twenty patients was photographed in a standardized fashion in 3 directions. These photographs were assessed by 2 dermatologists, 2 plastic surgeons and 2 non medically trained individuals, applying the POSAS observer scale. The reviewers of the post operative photos were blinded as to which treatments patients had received. Means of the POSAS scores were compared using the student's t-test.
Results
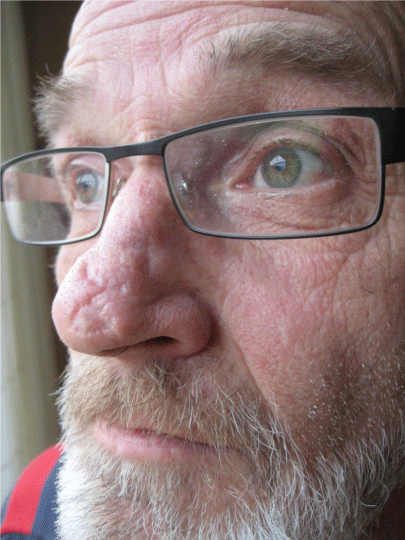
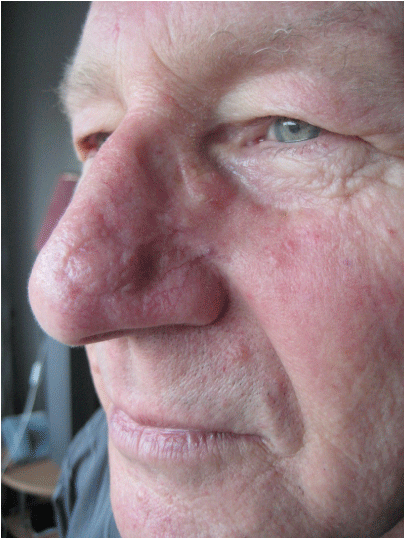
In both groups, wound healing complications did not occur.There were no significant differences between opinions of the two techniques. Overall, on a scale from 0 to 10 where 0 means 'no visual abnormalities' the bilobed flap scored 2.22 versus 2.33 for the skin graft. Where medical consultants preferred the bilobed flap, non medical individuals favored the skin graft closure. Figure 2, figure 3, figure 4 and figure 5 present acceptable and unacceptable results of both blobed flaps and skin grafts.
Discussion
The present study found no evidence to support the textbook statement that the bilobed flap "excels" for reconstruction of defects less than 1.5 cm around the nasal tip.
McGregor and Soutar studied 44 patients by whom an average size of nasal defect of 1.5 cm had been closed with a bilobed flap at least six months in advance [5]. They noted excellent cosmetic results with minimal tissue distortion, hardly visible residual scars and the colour match, contour and tissue symmetry described as remarkably good. Occasionally bilobed flaps on the nose developed teleangiectasia on one or both of the transposed flaps. Contrary to popular belief, pincushioning, did not appear to be a problem and was found in only one case. In approximately 30% of the cases reviewed, the results were considered less than satisfactory and in all cases the faults could be attributed either to poor judgement or design.
The ideal situation for using a bilobed flap, they stated, is where there is tissue available in close proximity to the defect and where it is crucial to avoid producing tissue distortion in important anatomical sites. In contrast to Esser (1918), who stated [2] that the angle of tissue transfer had to be 90 degrees and [3] that both flaps should be equal in size, in McGregor and Soutar's experience the technique offers a great variation in the angle of tissue transfer without appearing to affect the cosmetic result, and most commonly, the first flap is larger than the second flap.
Full-thickness skin grafts are used to resurface even large superficial defects of skin and fat in the thin skin zone of the upper two thirds of the nose, but preferably not on the tip or ala [6]. The hairless preauricular area is the best donor site. A strip of hairless skin can be harvested, even in men. Postauricular skin and supraclavicular skin are also potential donor sites, but often appear more red or brown, respectively.
The use of any local flap following excision of any malignant skin lesion requires careful consideration. Incomplete excision will require further surgery and recurrence may occur even though the original pathology reports complete excision. For this reason, in our clinic, we generally do not perform closure with a bilobed flap until radical excision has been ascertained by pathological examination. Having to leave the defect open during one week when applying a bilobed flap, by some surgeons is considered too great a disadvantage and enough reason always to use a skin graft. Should histologic examination reveal incomplete excision, the skin graft can easily be reexcised and repeated.
In conclusion, for future cases with nose tip defects, the selection of closure technique can be made on an individual basis.
References
-
Esser JFS, Burget GC, Menick FJ (1994) Aesthetic reconstruction of the nose. St. Louis, Mosby.
-
Esser JSF (1918) Gestielte lokale Nasenplastik mit Zweizipfligen Lappen, Deckung des sekunderen Defektes vom ersten Zipfel durch den Zweiten. Deutsche Zeitschrift für Chir 143: 385.
-
Zimany A (1953) The bilobed flap. Plast Reconstr Surg 11: 424-434.
-
Zitelli JA (1989) The bilobed flap for nasal reconstruction. Arch Dermatol 125: 957-959.
-
McGregor JC, Soutar DS (1981) A critical assessment of the bilobed flap. Br J Plast Surg 34: 197-205.
-
Spear SL, Kroll SS, Romm S (1987) A new twist to the nasolabial flap for reconstruction of lateral alar defects. Plast Reconstr Surg 79: 915-920.