Journal of Dermatology Research and Therapy
Refractory Perianal Ulcers in a Neonate. Beyond the Diaper Rash
Khodayar-Pardo Parisa1,2*, Sanchez Mari Maria1 and Lopez Garcia M Jose1,2
1Department of Pediatrics, Hospital Clínico Universitario de Valencia, Spain
2School of Medicine, University of Valencia, Spain
*Corresponding author:
Parisa Khodayar-Pardo, MD, PhD, Department of Pediatrics, Hospital Clínico Universitario de Valencia, Avda. Blasco Ibanez, 17-10. 46018, Valencia, Spain, E-mail: parisa.khodayar.pardo@gmail.com
J Dermatol Res Ther, JDRT-2-025, (Volume 2, Issue 3), Short Note; ISSN: 2469-5750
Received: March 28, 2016 | Accepted: April 30, 2016 | Published: May 02, 2016
Citation: Khodayar-Pardo P, Sánchez-Marí M, López-García MJ (2016) Refractory Perianal Ulcers in a Neonate. Beyond the Diaper Rash. J Dermatol Res Ther 2:025. 10.23937/2469-5750/1510025
Copyright: © 2016 Khodayar-Pardo P, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The diaper rash is a common medical query in pediatric offices. Most of the time it is due to a contact dermatitis or mild infection that only requires local care for its resolution. The appearance of more severe lesions, such as ulcers, and the resistance to conventional therapy should make us suspect the existence of an underlying disease.
Keywords
Diaper rash, Infantile hemangioma, Vascular tumor
Introduction
The Infantile hemangioma with minimal or arrested growth (IH-MAG) is a recently defined type of hemangioma in which the proliferative phase could not be appreciated as it is limited to less than 25% of the surface. Its recognition is important as it often becomes ulcerated and this can lead to misdiagnosis and thus to an inappropriate and inefficacious therapy. Furthermore, IH-MAG could be associated to inner malformations that should be evaluated thoroughly.
Case Report
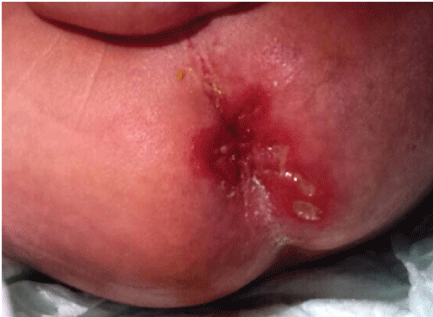
A three week-old boy was evaluated at the emergency department because of the presence of two deep ulcers of 25 × 10 and 5 × 10 mm on a reddish skin in the perianal area (Figure 1). Neonate was born with normal delivery at 38 weeks of gestation and 3 kg from Italian and no consanguineous parents. The pregnancy was uneventful, including normal serum screen and no herpetic lesions in the birth canal. The baby was exclusively breastfed and his bowel transit was normal.
.
Figure 1: At the time of consultation the neonate showed a reddish skin in the perianal area and two deep ulcers of 25 × 10 and 5 × 10 mm.
View Figure 1
Two weeks prior to presentation, his mother noticed the gradual appearance of a severe reddish discoloration in the perianal area that extended along the intergluteal cleft. Two papules appeared over it one week after. They were friable with the diaper friction and became the two ulcers described above. The different antibacterial (mupirocin and fusidic acid) and moisturizer ointments tested were unsuccessful. The neonate was otherwise asymptomatic. A physical examination showed a well-appearing afebrile male neonate with a severe perianal reddish discoloration, which had extended along the intergluteal cleft and sideways with two deep ulcers.
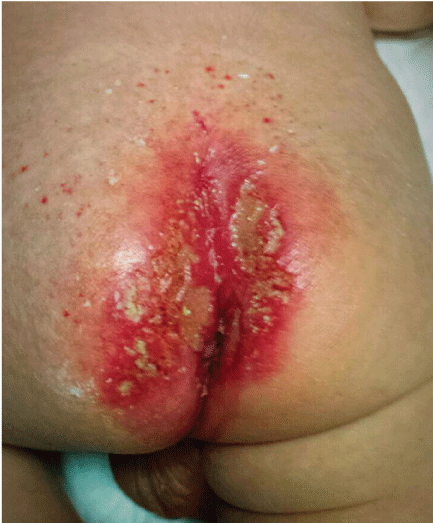
Despite the complete healing of the ulcers after the application of antifungal (fluconazole) and cicatrizing ointments and intravenous antibacterial (amoxycilin/clavulanic acid and clindamycin) treatment during one week, new lesions appeared and spread rapidly. Note that the new ulcers were coalescing and their edge showed hyperemia rather than proliferation (Figure 2). Bacterial and fungal cultures were normal. Serum screen for Herpes simplex virus was negative.
.
Figure 2: Despite of the application of antifungal and cicatrizing ointments and intravenous antibacterial medication, the reddish skin affected the intergluteal cleft and spread sideways and new ulcers appeared. Note that the new ulcers were coalescing and their edge showed hyperemia rather than proliferation. Additionally a telangiectatic rash existed in the lumbar and sacral area and a subtle bluish or violet reticulated pattern was underneath.
View Figure 2
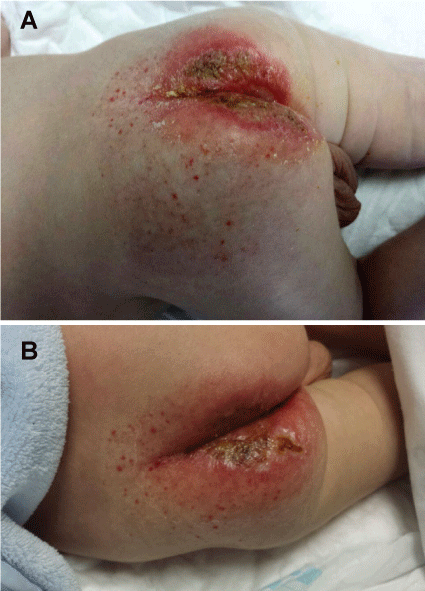
We noticed the presence of a bruise-like lesion with a reticulated pattern on the lumbar and sacral region (Figure 3). It was first attributed to a birthmark but a telangiectatic rash showed up over it suggesting an underlying disease, and this led to the final diagnosis: an infantile hemangioma with minimal or arrested growth.
.
Figure 3: (a) The neonate showed a differentiated area of the normal skin on the lumbar and sacral region from the time of birth. This area displayed a vascular reticulated pattern lateralized to the left over which a telangiectatic rash extended. Fine vessels formed a reticulated pattern and reddish petechiae appeared above suggesting an underlying vascular condition; (b) After the initiation of propranolol the lesions start to change. The petechiae became lighter, the reticulated pattern whiter and the ulcers started to heal.
View Figure 3
Discussion
The lack of response to the ointments usually employed in the diaper rash raised the suspicion of an uncommon etiology of infection leading to the use of topic antifungal and intravenous antibacterial medication. The diaper rash is the most frequent dermatological problem during infancy and constitutes a regular enquiry for medical assessment. It manifests in association with irritation in the areas in contact with the diaper and respects skin folds, except for severe cases and those infected with Candida spp. The Erosive dermatitis of Jacquet is a rare variant of diaper rash that affects patients with chronic diarrhea or fecal incontinence, such as children with neurological impairment or Hirschsprung disease. It produces a very intense reddish discoloration and maceration of the skin folds and even ulcers. The normal bowel transit of our patient made this implausible. Additionally, cow's milk allergy or lactose intolerance could produce perianal lesions. However, this was not an issue in this patient given that he was exclusively breastfed and no digestive or allergic symptoms were identified.
Finally, the gradual appearance of a telangiectatic rash over the bruise-like area was crucial to suspect an underlying vascular disease, such as an Infantile hemangioma (IH). The IH is the most common benign vascular tumor of infancy. The typical IH appears postnatally, grows rapidly from a few days or weeks until several months and regresses slowly within up to 8 years. The Infantile hemangioma with minimal or arrested growth is a recently described and thus under-recognized variant of IH in which an interruption of the proliferative phase occurs [1]. The main features that make it different from typical IH are that IH-MAG remains unaltered for a long period of time and its growth is limited to less than 25% of the surface. IH-MAG shows fine or coarse telangiectasias over normal or reddish skin, reticular distribution and congenital bruise-like lesions, with preferential onset on the lower part of the body.
Diagnosis of IH-MAG is often challenging, even for experienced clinicians, as it is often mistaken with birthmarks or port-wine stains. Moreover, IH-MAG located in the perianal area becomes ulcerated in 50% of the cases and the appearance of these ulcers prevents from the detection of the underlying vascular lesion, therefore, the implementation of futile treatments and procedures. IH-MAG’s vascular lesions stain positively for glucose transporter protein 1 (GLUT-1) [2]. Although biopsy is currently unnecessary, it could be useful in selected cases where the diagnosis is not clear to distinguish these lesions from vascular malformations. When an IH-MAG is suspected it is mandatory to rule out associated bone, medullar, vascular, anorectal and urogenital deformities, as they could take part of a PELVIS syndrome [3,4]. Thus, a Doppler ultrasound and a contrast enhanced MRI were performed showing normal results.
The neonate was treated with propranolol 2 mg/kg/day [5-7]. The result was a complete ulcer epithelization after 2 days and total recovery at the 15th day (Figure 4). The prompt and complete resolution of the lesion confirmed our suspicion.

.
Figure 4: At the 15th day after the initiation of propranolol the recovery was complete. Note that a whitish shadow appeared at the site of the hemangioma.
View Figure 4
Recognition of Infantile hemangiomas with minimal or arrested growth would help in more accurate characterization of vascular birthmarks of infancy. The frequent ulceration of perianal IH-MAG occurring in up to half of the cases, could hinder the diagnosis leading to the aggravation of the lesions and the application of inadequate treatments. Timely diagnosis and treatment would facilitate an early resolution of them.
References-
Suh KY, Frieden IJ (2010) Infantile hemangiomas with minimal or arrested growth: a retrospective case series. Arch Dermatol 146: 971-976.
-
Corella F, Garcia-Navarro X, Ribe A, Alomar A, Baselga E (2008) Abortive or minimal-growth hemangiomas: Immunohistochemical evidence that they represent true infantile hemangiomas. J Am Acad Dermatol 58: 685-690.
-
Martínez-Criado Y, Fernández-Pineda I, Merchante E, Bernabeu-Wittel J (2014) Lumbosacral abortive hemangioma with intradural extension. Pediatr Dermatol 31: e80-81.
-
Shimizu M, Sakai S, Tatekawa Y, Ishikawa S, Miyamoto M, et al. (2014) AAn Infant with PELVIS (Perineal Hemangioma, External genital malformations, Lipomyelomeningocele, Vesicorenal abnormalities, Imperforate anus, and Skin tag) Syndrome misdiagnosed as Diaper rash. J Pediatr 165: 634.
-
Léauté-Labrèze C, Dumas de la Roque E, Hubiche T, Boralevi F, Thambo JB, et al. (2008) Propranolol for severe hemangiomas of infancy. N Engl J Med 358: 2649-2651.
-
Tan ST, Itinteang T, Leadbitter P (2011) Low-dose propranolol for infantile haemangioma. J Plast Reconstr Aesthet Surg 64: 292-299.
-
Léauté-Labrèze C, Hoeger P, Mazereeuw-Hautier J, Guibaud L, Baselga E, et al. (2015) A randomized, controlled trial of oral propranolol in infantile hemangioma. N Engl J Med 372: 735-746.





