Journal of Dermatology Research and Therapy
Dry Eye Syndrome: What the Dermatologist Needs to Know
David M. Kleinman*
Associate Professor of Ophthalmology, University of Rochester Medical Center, New York, USA
*Corresponding author:
David M. Kleinman, MD, MBA, FACS, Associate Professor of Ophthalmology, Flaum Eye Institute, University of Rochester Medical Center, 601 Elmwood Avenue, Box 659 Rochester, New York 14642, USA, Tel: 585-275-0626, Fax: 585-276-0292, E-mail: David_Kleinman@URMC.rochester.edu
J Dermatol Res Ther, JDRT-2-024, (Volume 2, Issue 2), Short Review; ISSN: 2469-5750
Received: March 28, 2016 | Accepted: April 18, 2016 | Published: April 21, 2016
Citation: Kleinman DM (2016) Dry Eye Syndrome: What the Dermatologist Needs to Know. J Dermatol Res Ther 2:024. 10.23937/2469-5750/1510024
Copyright: © 2016 Kleinman DM. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
It is very likely that dermatologists will see patients who have both skin concerns and concomitant dry eye syndrome [1,2]. Over 25 million Americans have some form of dry eye, and symptoms related to dry eye are one of the leading causes of visits to ophthalmologists. Dry eye syndrome can often be easy to diagnose, and the first line of interventions are simple, low risk, and low cost. Specialists and subspecialists are generally averse to making medical recommendations outside their field of expertise, but, a few helpful recommendations from a dermatologist whose patient describes mild dry eye symptoms might benefit the patient, strengthen the dermatologist-patient relationship, and save an unnecessary trip to an eye care provider.
Dry eye syndrome is a disease of the ocular surface whereby the natural tears stop providing necessary protection to the cornea both in terms of preventing desiccation and generally supporting epithelial health [3]. A formal definition of dry eye syndrome was developed by an expert working group in 2007. This definition has been broadly accepted by the ophthalmic community; it is worthwhile to share it with dermatologists:
Dry eye is a multifactorial disease of the tears and ocular surface that results in symptoms of discomfort, visual disturbance, and tear film instability with potential damage to the ocular surface. It is accompanied by increased osmolarity of the tear film and inflammation of the ocular surface [4].
Dry eye syndrome is currently divided into two distinct but overlapping subtypes: aqueous deficient and evaporative [3-5]. Patients may present with features of both subtypes. The hallmark of the condition generally is tear film instability, and corneal findings are then found secondarily. Patients with dry eye syndrome may describe transient blurred vision often made better with blinking, a burning sensation of the eyes, irritated or a gritty sensation in the eyes, excessive tearing (patients with dry eye have excessive tearing because when the eye gets dry enough reflexive tearing is triggered and the lacrimal gland secretes more tears than the eye can hold), and discomfort with blinking (due to the movement of the palpebral conjunctiva over the irritated cornea). One or multiple symptoms may be present. On examination, there can be no findings especially on general inspection of the eye without the use of a slit lamp or biomicroscopy. Occasionally the conjunctiva is injected. Sometimes there is a reduced tear lake inferiorly, but this finding can be hard to appreciate even for experienced observers. The hallmark of more moderate to severe dry eye is epithelial staining with commercially available fluorescein dye for topical ophthalmic use. Once a small amount of this dye is placed in the lower fornix, the eye is illuminated with cobalt blue light which is found on a slit lamp and a direct ophthalmoscope (use the +40 lens for a magnified image) or a Woods lamp to view this finding (Figure 1). More advanced methods for assessing dry eye include assessing tear film break-up time by slit lamp, measuring tear production with Schirmer's strips, or testing the osmolarity of tears [5]. These steps are not necessary to initiate a basic treatment plan for dry eye when the symptoms are obvious and there are no concerns for alternative or potentially serious diagnoses. Thus, when a dermatologist encounters a patient that likely has dry eye syndrome, a basic and low risk therapeutic regimen as described below can and probably should be initiated. Based on the patient's concomitant skin and medical problems, communication with the primary care physician or additional direct referrals can be initiated.
.
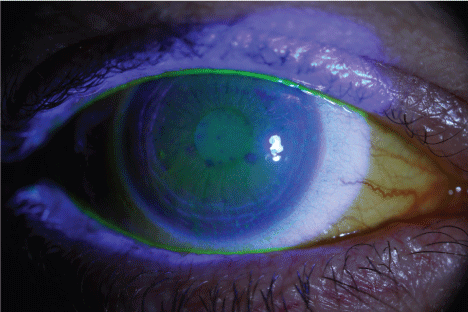
Figure 1: Fluorescein findings under cobalt blue light illumination in a patient with dry eye syndrome. Note the fluorescein dye staining damaged epithelium. [Courtesy Flaum Eye Institute, Rochester, NY].
View Figure 1
There are, of course, situations when referral to an eye care provider is indicated. Examples include:
• If a patient is symptomatic in only one eye, and there is no obvious explainable reason such as presumed mild viral conjunctivitis or unilateral ectropion, consideration should be given to a referral to an ophthalmologist.
• If the patient is a contact lens wearer and reports redness, pain or decreased vision, a contact lens related complication should be considered. Occasionally contact lens wearers can get a corneal infection. A prompt ophthalmologic assessment is needed as specialized antibiotic treatment may be sight saving.
• For recent ocular or periocular trauma, a formal ophthalmic assessment is suggested. In particular, a corneal abrasion from vegetative matter could lead to an infection that would require immediate therapy. Trauma with sharp objects creates significant risks to the eye, and occasionally even mild blunt trauma can lead to intraocular hemorrhage, inflammation or retinal tears-all of which should be considered by an examining ophthalmologist.
• Urgent referral is mandated when the possibility exists for an intraocular foreign body. For example, a patient that was grinding metal or hammering metal on metal may have minimal symptoms including ophthalmic discomfort at first. However, a small piece of metal could have penetrated the globe and emergent surgery may be indicated. This scenario is one for which emergency medicine physicians must be acutely aware as a missed intraocular foreign body is a source of both poor visual outcomes and litigation.
• Patients that present with photophobia or significant decreases in vision should also be referred as there may be an underlying uveitis or retinal abnormality that needs attention.
• Patients that have been placed on eye drops can sometimes secondarily develop tear film abnormalities. This relationship needs to be kept in mind, but these patients often have an eye care provider who can directly manage these concerns.
In general, however, in a patient that presents with classic dry eye symptoms and has no associated pain, redness, lid or conjunctival edema, or vision loss, a presumptive diagnosis of dry eye can be made, and treatment (as described below) can be initiated while a routine eye examination can be temporarily deferred or set up at the patient's convenience.
The eyelids are a region of the body where dermatology and ophthalmology intersect. Blepharitis is an extremely common condition and may lead to or exacerbate dry eye syndrome (meibomian dysfunction can result in evaporative dry eye) [5]. Fortunately lid hygiene and warm compresses are a reasonable first-line intervention for both conditions. Although a combination topical antibiotic/steroid ointment can be an effective next step, for patient safety related to the small but real likelihood of an undiagnosed glaucoma and the associated risks of a steroid-induced elevation of intraocular pressure, it is recommended that care be taken with prescription topical therapy. Thus, when blepharitis fails to respond to supportive measures referral to an eye care provider is indicated. Trichiasis (inward growth of the eyelashes) may also be found in dermatology patients, and eyelashes rubbing on the cornea may lead to ocular irritation. Thus, the eyelashes should be carefully inspected when symptoms point toward trichiasis. An easy temporizing approach here is forceps epilation of the offending lashes. Dermatologists also may identify lid laxity, ectropion, or entropion. Sometimes these underlying conditions must be assessed for possible repair, and an oculoplastic surgeon should be consulted. An abnormal growth on the eyelid can also cause ophthalmic symptoms. Cooperation between ophthalmologists, dermatologists and sometimes oculoplastic surgeons is appropriate in many such situations. Another possible cause of excessive tearing is when tears cannot traverse the lacrimal drainage system. Tears will then run down the cheek. Punctal occlusion is possible due to external scarring, and ectropion can cause a loss of contact between the puncta and the eye. Again, close inspection should allow even a non-expert examiner to conclude if either of these findings is present. Internal nasolacrimal duct blockage can also develop. An irrigation test is used to evaluate the status of the internal tear drainage system and is typically performed by an ophthalmologist. It is clear that dermatologists and ophthalmologists may need to work together to help patients with eyelid pathology.
Since dry eye can be seen in many dermatology patients and often the symptoms are mild (especially at first) it is helpful to review common systemic and skin conditions associated with dry eye syndrome (Table 1). When associated with skin disorders, dry eye syndrome is primarily of the evaporative subtype. Importantly, there may be more than one factor causing dry eye syndrome. For instance, a patient with rosacea and dry eye symptoms may have a behavioral contribution as well. Working for long hours on computers or extended contact lens wear may exacerbate environmental stress on the ocular surface in the setting of an underlying dermatological condition. The classic triad of dry eyes, mouth and skin is known to most dermatologists as indicative of Sjogren's Syndrome (SS) or non-Sjogren's sicca. Other cutaneous manifestations of SS mainly include pruritus, annular erythema, vasculitis, or panniculitis. Furthermore, cutaneous B-cell lymphoma can be associated with sicca symptoms. The early diagnosis of SS is important in order to expedite the investigation of possible extra glandular manifestations, B-cell lymphoma or monoclonal gammopathy [7]. If an underlying inflammatory disease is a potential concern, the dermatologist should ensure the patient's primary care physician is aware of this issue, or alternatively a consultation with a rheumatologist may be indicated.
![]()
Table 1: Conditions seen by dermatologists where dry eye syndrome is likely (in alphabetical order).
View Table 1
Many times, though, a little basic ophthalmic advice from a dermatologist can be valuable. In the setting of dry eye symptoms with no suggestion of anything more severe regarding the eyes, it is appropriate to recommend several effective interventions for dry eye. Fortunately, for mild to moderate dry eye syndrome, and at times even for severe dry eye, the treatment regimen is simple, low cost, and low risk (Table 2). These interventions are not complex and can often be conveyed easily and quickly to the patient. Although supportive, and not always effective (for example artificial tears over the course of one year were effective in improving the status of dry eye in 68% of patients one recent study), these recommended interventions can be very helpful, are safe and will likely remain as part of a more rigorous therapeutic regimen if one is required [8].
![]()
Table 2: Effective and low risk interventions for dry eye syndrome.
View Table 2
The past decade has witnessed increased attention to the role of fatty acids in inflammatory diseases including dry eye syndrome. Epidemiologic data has demonstrated a decreased risk for dry eye syndrome with increasing rates of dietary consumption of omega-3 fatty acids. Regarding omega-3 supplementation, there is growing consensus that this intervention has value in certain conditions. Beneficial effects from omega-3 supplementation have been seen in rheumatoid arthritis as well as dry eye syndrome. Omega-3 supplementation has been shown to increase tear volume and tear production in one study and symptoms of dry eye and tear stability in another. Omega-3 supplementation may benefit dry eye patients and possibly especially those with underlying rheumatoid arthritis, rosacea, or psoriasis [4,9-11].
Despite the systematic approach to dry eye recommended here, not infrequently more advanced treatments such as prescription products (topical cyclosporine eye drops), moisture goggles, specialized contact lenses, gold weights in the eye lid for cranial nerve VII paresis, or tarsorrhaphy for a neurotrophic cornea may be required. Obviously expert ophthalmic opinion should be sought in patients either not responding to the first-line therapy, or when the dermatologist has a concern for a more significant underlying ophthalmic process.
In summary, dry eye syndrome is very common and certainly will be encountered in dermatology clinical practice. The condition can be easy to diagnose, and many management approaches are both effective and low risk. There are certainly times when an eye examination or ophthalmic consultation should be requested and when communication with the patient's primary care provider or a rheumatologist is indicated, but the dermatologist should feel comfortable providing some basic assistance to a patient when dry eye syndrome is identified.
References
-
Gayton JL (2009) Etiology, prevalence, and treatment of dry eye disease. Clin Ophthalmol 3: 405-412.
-
Moss SE, Klein R, Klein BE (2000) Prevalence of and risk factors for dry eye syndrome. Arch Ophthalmol 118: 1264-1268.
-
Pflugfelder SC, Solomon A, Stern ME (2000) The diagnosis and management of dry eye: a twenty-five-year review. Cornea 19: 644-649.
-
(2007) The definition and classification of dry eye disease: report of the Definition and Classification Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf 5: 75-92.
-
Bron AJ (2001) Diagnosis of dry eye. Surv Ophthalmol 45 Suppl 2: S221-226.
-
http://www.reviewofophthalmology.com/content/d/therapeutic_topics/i/1308/c/25170/
-
Masaki Y, Sugai S (2004) Lymphoproliferative disorders in Sjögren's syndrome. Autoimmun Rev 3: 175-182.
-
Rao SN (2010) Topical cyclosporine 0.05% for the prevention of dry eye disease progression. J Ocul Pharmacol Ther 26: 157-164.
-
Miljanovic B, Trivedi KA, Dana MR, Gilbard JP, Buring JE, et al. (2005) Relation between dietary n-3 and n-6 fatty acids and clinically diagnosed dry eye syndrome in women. Am J Clin Nutr 82: 887-893.
-
Wojtowicz JC, Butovich I, Uchiyama E, Aronowicz J, Agee S, et al. (2011) Pilot, prospective, randomized, double-masked, placebo-controlled clinical trial of an omega-3 supplement for dry eye. Cornea 30: 308-314.
-
Macsai MS (2008) The role of omega-3 dietary supplementation in blepharitis and meibomian gland dysfunction (an AOS thesis). Trans Am Ophthalmol Soc 106: 336-356.





