International Journal of Diabetes and Clinical Research
Conventional Versus Intensive Insulin Therapy in Young Children with Diabetes: Impact of a Long Term Targeted Multidisciplinary Education Program
Piero Balice1,2, Gerald Theintz1 and Mario G Bianchetti2*
1Department of Pediatrics, University Hospital Center, Lausanne, Switzerland
2Department of Pediatrics, Ente Ospedaliero Cantonale, Bellinzona, Switzerland
*Corresponding author:
Mario G Bianchetti, Department of Pediatrics, Ente Ospedaliero Cantonale, Ospedale San Giovanni, 6500 Bellinzona, Switzerland, E-mail: Mario.bianchetti@eoc.ch
Int J Diabetes Clin Res, IJDCR-4-068, (Volume 4, Issue 1), Research Article; ISSN: 2377-3634
Received: October 28, 2016 | Accepted: March 07, 2017 | Published: March 09, 2017
Citation: Balice P, Theintz G, Bianchetti MG (2017) Conventional Versus Intensive Insulin Therapy in Young Children with Diabetes: Impact of a Long Term Targeted Multidisciplinary
Education Program. Int J Diabetes Clin Res 4:068. 10.23937/2377-3634/1410068
Copyright: © 2017 Balice P, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Intensive insulin therapy is progressively replacing conventional therapy in young children to improve diabetes control. However, the specific skills required to manage insulin pumps may hamper social integration as much as the fear of severe hypoglycemia using conventional therapy.
Methods: The impact of a continuous education program targeting parents and their substitutes on their living places, was assessed in 23 subjects aged 2.3 ± 0.2 years treated by insulin pump (CSII) for 3.2 ± 0.6 years and compared to 23 subjects aged 3.2 ± 0.2 years treated by conventional therapy (CV) for 3.5 ± 0.3 y.
Results: HbA1c levels were undistinguishable in both groups throughout the study period, remaining within recommended ADA target. Whereas a greater increase in insulin dose was observed in the CV group (0.57 ± 0.06 to 0.79 ± 0.03 U/kg/day, p < 0.001) versus 0.64 ± 0.04 to 0.70 ± 0.04 U/kg/day (ns) in the CSII group over time, inter-group differences failed to reach significance. BMI SDS increased significantly in CSII group (p = 0.004). No significant difference was observed in the number of days of admission/subject and in the number of admissions for severe hypoglycemia. The number of admissions for ketoacidosis was higher in the CSII group (p = 0.027).
Conclusions: Externalizing targeted education programs on the child living place allows to minimize the hypoglycemia risk of CV. This result may be particularly relevant for less developed countries and contribute to reduce the cost of diabetes management without increasing the risks of side effects.
Keywords
Insulin dependent diabetes mellitus, Patient education, Preschool child, Cost effectiveness
Abbreviations
BMI: Body Mass Index; CSII: Continuous Subcutaneous Insulin Infusion; CV: Conventional Therapy; HbA1c: Glycosylated Haemoglobin
Background
Type 1 diabetes incidence is rising particularly among preschool children [1-6]. Whereas conventional therapy is still widely used, subcutaneous continuous insulin infusion (CSII) has recently been proposed to improve meal schedule flexibility, overcome glycemia instability, decrease the risk of severe hypoglycemia and therefore improve HbA1c levels [7-10]. Pump therapy also appears to be helpful to parents by decreasing their anxiety towards daily care [11]. Despite pumps technical challenge, improved quality of life is described by a majority of parents [9,12,13]. On the other hand, this therapeutic approach appears to be more expensive than conventional therapy and consequently limited to industrialized countries [14].
Whichever therapeutic strategy is used, education is the cornerstone of diabetes therapy with a good relationship between parental know how and diabetes balance [15,16]. Know how is usually gained through formal teaching sessions dispensed by specialized nurses at hospital. It can also be gained through less formal teaching by trained public health nurses working at home or at school [17-19]. However, the impact of educating families and parental substitutes on their places of life has not been well documented for young children, particularly the results on parameters such as the occurrence of severe hypoglycemia, the number of ketotic episodes leading to hospital admission and their correlation to HbA1c values as a marker of diabetes balance [20,21]. At a time of change towards a more general use of insulin pumps in patients who depend almost entirely on the supervision of adults, a program of therapeutic education and advice was designed to target parents and parental substitutes (grand-parents, kindergarten teachers, au pair girls, neighbors) on their places of life. The objective was a) to test whether such a targeted program followed up on the patients' places of life could compensate for the relative simplicity of conventional therapy compared to children using insulin pumps and b) whether a strategy involving externalized education and care programs might be relevant to disadvantaged countries as particularly cost effective.
Methods
The study approved by the Ethics Committee of our Institution involves 46 children with diabetes regularly followed in our unit and split up into two groups according to the therapeutic strategy chosen by parents at the onset of diabetes, namely continuous subcutaneous insulin infusion (CSII) and conventional therapy (CV) with 2 or 3 daily insulin injections. Parental choice was made after a few days reflection following detailed explanation of both strategies involving trained diabetologists (PB, GT), specialized nurses and dieticians. Mean and SEM are represented for tables and figures. Table 1 summarizes relevant information for both groups. The exclusion criteria were: a) chronological age < 1.0 year or > 5.5 years at the onset of diabetes; b) therapy duration < 6 months.
![]()
Table 1: Pertinent characteristics of 46 subjects participating to the study. Mean ± SEM is shown for each variable. Anova significance (p) < 0.05 level.
View Table 1
The CSII group used a Disetronic V100 insulin pump loaded with soluble human insulin Actrapid® U-100 (Novo Nordisk) or U 10 (diluted 1/10 with NaCl 0.9%) or Insuman Infusat® U-100 (Aventis Pharma). In young children, the use of diluted human insulin Actrapid® allows to administer insulin of very low doses (< 0.1 U/h). As a consequence, there is no risk of nocturnal hypoglycemia. The CV group used NovoRapid® (Novo Nordisk) or Humalog® (Eli Lilly) and Insulatard® (Novo Nordisk) or Huminsulin Basal® (Eli Lilly) either in 2 injections (mixture of rapid and NPH) or in 3 injections (mixture of rapid and NPH morning and evening and one NPH injection after lunch). Diabetes control was assessed by 3-4 (CV group) or 4-6 (CSII group) daily glycemias. Formal medical controls were performed on a 3-4 months basis with HbA1c measurement using a DCA® 2000 (Bayer) device regularly calibrated and checked through an external laboratory quality control program. In addition, each subject underwent a full yearly check up including microalbuminuria determination, lipid profile determination and screening for auto-immune diseases.
As part of a larger program aiming at controlling the cost/effectiveness ratio of paediatric diabetes care for local public health authorities, the Unit has designed a prospective structured education and follow-up program integrating the socio-cultural scope. The ultimate goal is to ensure familial autonomy in diabetes care at home as well as in the children's various places of life regardless of therapeutic strategy. The program is split into two parts: a) at the onset of diabetes, during hospitalization: 15 teaching hours given by the multidisciplinary team and discussing each aspect of diabetes therapy and balance including the management of daily hazards; b) educational follow up and advice on the various places of life (neighbors, kindergarten, school) by two specialized public health nurses. This follow up comprises 10 interventions lasting 1-2 hours on a monthly basis during the first 3 months then one intervention per trimester including family evaluation, information at kindergarten or school with active participation of caretakers and teachers: teaching is mainly practical using games developed for young children. The program is backed up by an emergency line open 24 h/24.
Data computerization included cause of admission, duration of hospital stays, number and cause of severe hypoglycemia, number and origin of ketoacidosis episodes, pump failures, follow up of auxological and laboratory parameters as well as insulin doses. For each subject, data were collected at the onset of diabetes (T0), at the time of best HbA1c values during the first semester of therapy (T1), corresponding to the remission phase and at the end of the study period (T2) as shown in table 1. Data were analyzed using SYSTAT 7.0 statistical package (Evanston, Ill).
Results
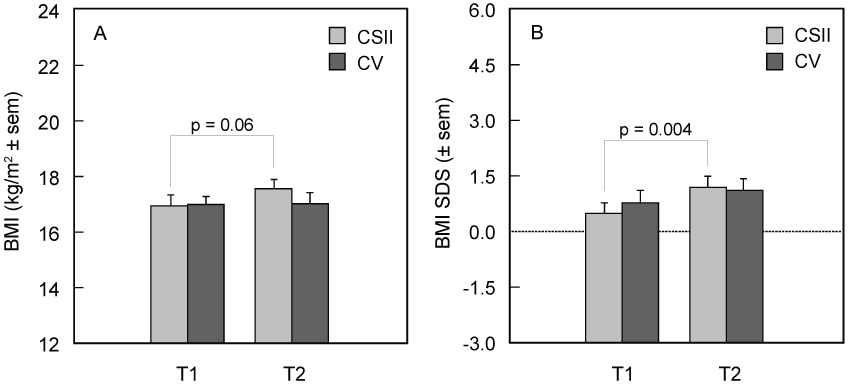
The evolution of average insulin doses expressed as U/kg BW is shown in table 2. The insulin dose given with CSII group does not increase significantly with time (T1 vs. T2) in contrast with that given in the CV group. At T1, the comparison between groups is not significant. At the end of the study period (T2), the insulin dose is lower in the CSII group but the difference fails to reach significance. Paradoxically, the increase in BMI is significantly higher in this group (Figure 1, left panel). This difference remains significant when BMI is expressed as SDS (Figure 1, right panel). The evolution of HbA1c levels over time is shown in figure 2: no difference in HbA1c values could be demonstrated either as a function of time for each group (T1 versus T2) or between groups at both T1 and T2. Mean HbA1c values are within ADA recommended target [22]. The impact of educational program is also evaluated (Figure 3) by the number of ketotic episodes requiring hospital admission (left panel), the number of severe hypoglycemias (middle panel) and the duration of hospital stays directly caused or precipitated by diabetes during intercurrent paediatric illnesses (right panel). The number of hazards is expressed as episodes respectively days of admissions per subject during the whole study period. Each variable shows low figures; in particular, prevention of severe hypoglycemia was as efficient in the CV group as in the CSII group. In contrast, the number of ketoacidosis was significantly higher in the CSII group. In keeping with these data, the number of days of admission per subject is low, reaching an average of 1.5 day/subject/year in the CSII group and 1.1 day/subject/year in the CV group, the difference being not statistically significant.
.
Figure 1: Evolution of body mass index (BMI) from the onset (T1) to the end (T2) of the study in two groups of subjects treated with continuous subcutaneous insulin infusion (CSII) or with conventional therapy (CV). The trend towards significant increase in BMI gain in the CSII group (A) becomes significant when data are expressed as SDS (B).
View Figure 1
.
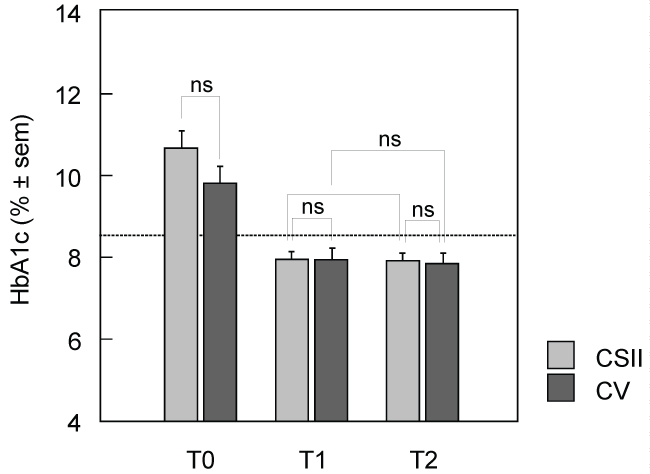
Figure 2: Comparative evolution of HbA1c levels from the onset (T1) to the end (T2) of the study in two groups of subjects treated either with continuous subcutaneous insulin infusion (CSII) or with conventional therapy (CV). The values are compared to HbA1c levels at the onset of diabetes (T0).
View Figure 2
Discussion
It is well documented that intensive therapy improves glycemic control and HbA1c levels in children and adolescents and that it contributes to delay microvascular complications [13,23-30]. Moreover and particularly in young children, insulin pump therapy appears to reduce the risk of repeated severe hypoglycemias susceptible to cause brain damage [31]. It is therefore not surprising that this technique be applied to ever younger children [29,30,32]. Several studies evaluating parental satisfaction have also shown that the flexibility of insulin pump therapy improves family confidence: the system can be adapted to any child rhythm; insulin delivery can be modulated instantly thus decreasing the risk of hypoglycemia [9,12,13]. However, this technique which appears to be more costly may not be applicable to any family [14]. It is so far reserved to industrialized countries. Concerning strategies involving multiple daily injections, it has also been shown that the number of injections may not be correlated to diabetes control [33]. Whichever therapy is chosen, therapeutic education appears not only as one of the major determinants of diabetes balance but also as a tool contributing to control the rising cost of diabetes care and improve the financial balance of less privileged families [22,34-36]. For young children, therapeutic education is provided almost exclusively to the parents by specialized pediatric teams working in defined hospital settings [37]. For practical reasons, this teaching cannot be systematically extended to parental substitutes by the hospital team. Parents may also experience difficulties transferring their own knowledge outside home, which inevitably generates failures in the daily management of diabetes. As a result, diabetes care may become a burden increasing family anxiety and represent an obstacle to the developing autonomy of the child.
.
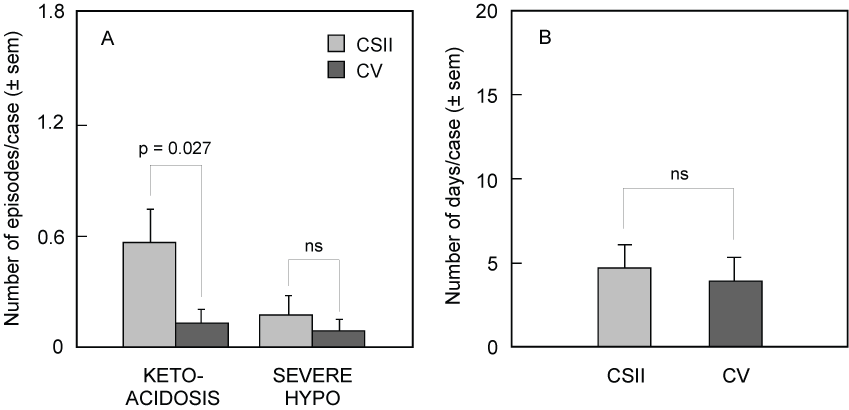
Figure 3: Left Panel A) Number of episodes of ketoacidosis and severe hypoglycemia per case in the CSII treated group compared to the CV treated group during the whole observation period. Significantly less ketoacidosis episodes were observed in the CV treated group Right panel; B) Number of admission days per case in the same groups during the whole observation period.
View Figure 3
![]()
Table 2: Mean insulin dose (U/kg/day ± sem) of 23 subjects treated with continuous subcutaneous insulin infusion (CSII) compared to 23 subjects treated by conventional therapy (CV) at the onset (T1) and at the end (T2) of the study period.
View Table 2
The goal of our study was to determine to which extent different therapeutic strategies applied to children depending almost entirely on adults can be influenced by a long lasting targeted education and advice program performed on the children's places of life. In this strict setting, analyzing children of comparable age treated for several years, the first salient result is that pump therapy fails to maintain its expected advantages over conventional therapy. Mean HbA1c values are similar in both groups and within ADA recommended target [22]. It should be noted that the study protocol is designed to avoid the misinterpretation of the HbA1c decrease found in the first months of therapy as well as the "novelty effect" sometimes observed when introducing new techniques. In addition, other parameters such as the number of severe hypoglycemias and the number of days of hospitalization are low, without significant difference between groups. The number of ketoacidosis episodes was even significantly greater in the CSII group. The increased frequency DKA in the CSII group is likely related to the absence of slow-acting insulin. As the baseline flow of the pump is ensured by small doses of of regular insulin administered every hour, flowdiscotinuation is sometimes followed by an abrupt increase blood sugar and, 8-10 hours later, by a relevant risk of DKA. Several studies have discussed the insulin pump therapy issue in children: [7-9,13,28,29]. however, the groups of patients are heterogeneous comprising even adults [13,28,29]. Follow up study is relatively short with difficulty to disentangle the "novelty effect" [7,9]. Last but not least, the advantages attributed to pump therapy included parameters expressed in units difficult to compare [7,9,13,28,29]. Our findings are similar those of Tubiana, et al. analyzing two groups of children of comparable age but with a shorter follow up [8]. Our study also shows inappropriate weight gain for age as expressed by the progression of BMI SDS in the CSII group whereas the average insulin dose is similar to that of CV group. Our results contrast with studies cited above reporting that insulin pump therapy has no effect on BMI and on the number of ketoacidosis episodes, as for adolescents [38-40]. Finally, targeted continuous education programs represent a source of substantial savings in the cost of diabetes management [34]. Specialized pediatric centers should develop teaching processes outside hospital for example through public health nurses belonging to centers and working in a multidisciplinary approach. This "externalized" diabetes management bears other advantages including hospital costs reduction mainly through shorter hospitalization time, decreased cost for insurances through longer time intervals between medical controls and fewer side effects [41-44]. Last but not least, indirect positive effects include improved parental confidence and better child socialization. It improves the general knowledge of diabetes among kindergarten and school teachers.
In conclusion, the less costly conventional therapy is by no means a second choice therapy when supported by quality teaching programs which can be run on the children's places of life [14]. Such programs might be particularly applicable to underprivileged families or countries without altering diabetes control or increasing the risk of severe hypoglycemia. In our experience, insulin pump therapy remains a remarkable therapeutic tool particularly in the neonatal period and in the first year of life during which it appears to be the tool of choice.
Acknowledgement
We gratefully acknowledge the work of our nursing team (Virginie Boegli, Anabel Domingues, Marie Fachinger, Cristina Gaspar, Sophie Gauthier, Christine Lambelet, Maxine Schlaeppi), our dieticians (Sylvie Borloz, Véronique Pidoux, Yolande Cherica) and psychologist (Carine Moreillon) who, in turn, have devoted time and energy in the last 8 years to ceaselessly improve teaching programmes for young children and their parents. We also warmly thank the medical board of the Department of Health of the Canton of Vaud as well as the medical board of the Health School Services of the City of Lausanne for having greatly facilitated the access to school and kindergarten supervisors, teachers, nurses and doctors.
References
-
SG Gardner, PJ Bingley, PA Sawtell, S Weeks, EA Gale (1997) Rising incidence of insulin dependent diabetes in children aged under 5 years in the Oxford region: time trend analysis. BMJ 315: 713-717.
-
Karvonen M, Pitkäniemi J, Tuomilehto J (1999) The onset age of type 1 diabetes in Finnish children has become younger. Diabetes Care 22: 1066-1070.
-
Dahlquist G, Mustonen L (2000) Analysis of 20 years of prospective registration of childhood onset diabetes-time trends and birth cohort effects. Acta Paediatr 89: 1231-1237.
-
Bruno G, Merletti F, Biggeri A, Cerutti F, Grosso N, et al. (2001) Increasing trend of type 1 diabetes in children and young adults in the province of Turin (Italy). Analysis of age, period and birth cohort effects from 1984 to 1996. Diabetologia 44: 22-25.
-
Schoenle EJ, Lang-Muritano M, Gschwend S, Laimbacher J, Mullis PE, et al. (2001) Epidemiology of type 1 diabetes mellitus in Switzerland: steep rise in incidence in under 5 year old children in the past decade. Diabetologia 44: 286-289.
-
(2000) Variation and trends in incidence of childhood diabetes in Europe. EURODIAB ACE Study Group. Lancet 355: 873-876.
-
Weinzimer SA, Ahern JH, Doyle EA, Vincent MR, Dziura J, et al. (2004) Persistence of benefits of continuous subcutaneous insulin infusion in very young children with type 1 diabetes: a follow-up report. Pediatrics 114: 1601-1605.
-
Tubiana-Rufi N, de Lonlay P, Bloch J, Czernichow P (1996) Disparition des accidents hypoglycémiques sévères chez le très jeune enfant diabétique traité par pompe sous-cutanée. Arch Pédiatr 3: 969-976.
-
Litton J, Rice A, Friedman N, Oden J, Lee MM, et al. (2002) Insulin pump therapy in toddlers and preschool children with type 1 diabetes mellitus. J Pediatr 141: 490-495.
-
Rodrigues IA, Reid HA, Ismail K, Amiel SA (2005) Indications and efficacy of continuous subcutaneous insulin infusion (CSII) therapy in type 1 diabetes mellitus: a clinical audit in a specialist service. Diabetic Med 22: 842-849.
-
Sullivan-Bolyai S, Deatrick J, Gruppuso P, Tamborlane W, Grey M (2003) Constant vigilance: mother's work parenting young children with type 1 diabetes. J Pediatr Nurs 18: 21-29.
-
Sullivan-Bolyai S, Knafl K, Tamborlane W, Grey M (2004) Parents' reflections on managing their children's diabetes with insulin pumps. J Nurs Scholarsh 36: 316-323.
-
McMahon SK, Airey FL, Marangou DA, McElwee KJ, Carne CL, et al. (2005) Insulin pump therapy in children and adolescents: improvements in key parameters of diabetes management including quality of life. Diabet Med 22: 92-96.
-
Palmer AJ, Weiss C, Sendi PP, Neeser K, Brandt A, et al. (2000) The cost-effectiveness of different management strategies for type 1 diabetes: a Swiss perspective. Diabetologia 43: 13-26.
-
Zgibor JC, Songer TJ, Kelsey SF, Weissfeld J, Drash AL, et al. (2000) The association of diabetes specialist care with health care practices and glycemic control in patients with type 1 diabetes: a cross-sectional analysis from the Pittsburgh epidemiology of diabetes complications study. Diabetes Care 23: 472-476.
-
Renders CM, Valk GD, Griffin SJ, Wagner EH, Eijk Van JT, et al. (2001) Interventions to improve the management of diabetes in primary care, outpatient, and community settings: a systematic review. Diabetes Care 24: 1821-1833.
-
Moyer A (1989) Caring for a child with diabetes: the effect of specialist nurse care on parents' needs and concerns. J Adv Nurs 14: 536-545.
-
Schnackel K (1979) Pediatric clinical specialist and diabetes nurse specialist: a twofold position. Nurs Adm Q 4: 91-95.
-
Robbins G (1981) School visits: an extension of the diabetes education program for children. Diabetes Educ 7: 30-33.
-
Assal JP, Jacquemet S, Morel Y (1997) The added value of therapy in diabetes: the education of patients for self-management of their disease. Metabolism 46: 61-64.
-
Cahané M, Reach G, Vias M (1991) The aide to juvenile diabetes association: its role in the management and education of patients with insulin-dependent diabetes. Ann Pediatr 38: 261-267.
-
Silverstein J, Klingensmith G, Copeland K, Plotnick L, Kaufman F, et al. (2005) Care of children and adolescents with type 1 diabetes: a statement of the American Diabetes Association. Diabetes Care 28: 186-212.
-
Pickup J, Mattock M, Kerry S (2002) Glycaemic control with continuous subcutaneous insulin infusion compared with intensive insulin injections in patients with type 1 diabetes: meta-analysis of randomised controlled trials. BMJ 324: 705.
-
(1994) Effect of intensive diabetes treatment on the development and progression of long-term complications in adolescents with insulin-dependent diabetes mellitus: Diabetes Control and Complication Trial Research Group. J Pediatr 125: 177-188.
-
Chase HP, Dixon B, Pearson J, Fiallo-Scharer R, Walravens P, et al. (2003) Reduced hypoglycemic episodes and improved glycemic control in children with type 1 diabetes using insulin glargine and neutral protamine Hagedorn insulin. J Pediatr 143: 737-740.
-
Boland EA, Grey M, Oesterle A, Fredrickson L, Tamborlane WV (1999) Continuous subcutaneous insulin infusion. Diabetes Care 22: 1779-1784.
-
Weissberg-Benchell J, Antisdel-Lomaglio J, Seshadri R (2003) Insulin pump therapy. Diabetes Care 26: 1079-1087.
-
Willi SM, Planton J, Egede L, Schwarz S (2003) Benefits of continuous subcutaneous insulin infusion in children with type 1 diabetes. J Pediatr 143: 796-801.
-
Plotnick LP, Clark LM, Brancati FL, Erlinger T (2003) Safety and effectiveness of insulin pump therapy in children and adolescents with type 1 diabetes. Diabetes Care 26: 1142-1146.
-
Ahern JA, Boland EA, Doane R, Ahern JJ, Rose P, et al. (2002) Insulin pump therapy in paediatrics: a therapeutic alternative to safely lower HbA1c levels across all age groups. Pediatr Diabetes 3: 10-15.
-
Warren RE, Frier BM (2005) Hypoglycaemia and cognitive function. Diabetes Obes Metab 7: 493-503.
-
Maniatis AK, Klingensmith GJ, Slover RH, Mowry CJ, Chase HP (2001) Continuous subcutaneous insulin infusion therapy for children and adolescents: an option for routine diabetes care. Pediatrics 107: 351-356.
-
Mortensen HB, Robertson KJ, Aanstoot HJ, Danne T, Holl RW, et al. (1998) Insulin management and metabolic control of type 1 diabetes mellitus in childhood and adolescence in 18 countries. Hvidovre Study Group on Childhood Diabetes. Diabet Med 15: 752-759.
-
Beck JK, Logan KJ, Hamm RM, Sproat SM, Musser KM, et al. (2004) Reimbursement for pediatric diabetes intensive case management: a model for chronic diseases? Pediatrics 113: e47-e50.
-
Svoren BM, Butler D, Levine BS, Anderson BJ, Laffel LM (2003) Reducing acute adverse outcomes in youths with type 1 diabetes: a randomized, controlled trial. Pediatrics 112: 914-922.
-
Songer TJ, LaPorte R, Lave JR, Dorman JS, Becker DJ (1997) Health insurance and the financial impact of IDDM in families with a child with IDDM. Diabetes Care 20: 577-584.
-
Betts PR, Swift PG (2003) Doctor, who will be looking after my child's diabetes? Arch Dis Child 88: 6-7.
-
Raile K, Noelle V, Landgraf R, Schwarz HP (2002) Weight in adolescents with type 1 diabetes mellitus during continuous subcutaneous insulin infusion (CSII) therapy. J Pediatr Endocrinol Metab 15: 607-612.
-
Kaufman FR, Halvorson M, Miller D, Mackenzie M, Fisher LK, et al. (1994) Continuous subcutaneous insulin infusion: a review of the past and its implementation for the future. Diabetes Spectr 7: 80-84.
-
Kaufman FR, Halvorson M, Miller D, Mackenzie M, Fisher LK, et al. (1999) Insulin pump therapy in type 1 pediatric patients: now and into the year 2000. Diabetes Metab Res Rev 15: 338-352.
-
Laffel LM, Vangsness L, Connell A, Goebel-Fabbri A, Butler D, et al. (2003) Impact of ambulatory, family-focused teamwork intervention on glycemic control in youth with type 1 diabetes. J Pediatr 142: 409-416.
-
Laffel LM, Brackett J, Ho J, Anderson BJ (1998) Changing the process of diabetes care improves metabolic outcomes and reduces hospitalisations. Qual Manag Health Care 6: 53-62.
-
Lipman TH (1988) Length of hospitalisation of children with diabetes: effect of a clinical nurse specialist. Diabetes Educ 14: 41-43.
-
Dougherty G, Schiffrin A, White D, Soderstrom L, Sufrategui M (1999) Home-based management can achieve intensification cost-effectively in type I diabetes. Pediatrics 103: 122-128.





