International Journal of Diabetes and Clinical Research
Continuous Insulin Releasing and Blood Sugar Monitoring via Dental Implant Supported Semi-Implanted Device
Yu-Jung Li1,2*
1Graduate Institute of Mechanical and Electrical Engineering, National Taipei University of Technology, Taipei 106, Taiwan
2Department of Nursing, St. Mary's Junior College of Medicine, Nursing, and Management, Yilan 266, Taiwan
*Corresponding author:
Yu-Jung Li, Department of Nursing, St. Mary's Junior College of Medicine, Nursing and Management, Yilan 266, Taiwan, Tel: +886 2 2795-6030, +886-980-023203, E-mail: richard513.tw@yahoo.com.tw
Int J Diabetes Clin Res, IJDCR-3-057, (Volume 3, Issue 2), Research Article; ISSN: 2377-3634
Received: January 11, 2016 | Accepted: May 14, 2016 | Published: May 17, 2016
Citation: Yu-Jung L (2016) Continuous Insulin Releasing and Blood Sugar Monitoring via Dental Implant Supported Semi-Implanted Device. Int J Diabetes Clin Res 3:057. 10.23937/2377-3634/1410057
Copyright: © 2016 Yu-Jung L. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
As life expectancy prolonged currently, geriatrics become important and therefore it is urgent to improve the life quality throughout the chronic and critical diseases among the elderly above sixty-fifth years old. On the other hand, diabetes mellitus (DM) is the most famous chronic and metabolic disease which may lead to many cardiac, renal and infectious complications. Therefore regular blood sugar control is extremely important in diabetic management to avoid further complications. However, these procedures performed in the later stages of diabetes including blood sugar monitoring and insulin injections are all invasive and may result in irritations and unbearable stress inevitably. Diabetes also shows high correlations to periodontitis and has great influences in dental implant decisions. Currently diabetes under regular blood sugar control is not regarded as a contraindication of dental implant and the overall implant survival rate within five years is around 90%, which shows no significant differences compared to the patients without diabetic conditions. Furthermore, proper implant design will contribute in oral hygiene maintenance and bring benefits in blood sugar control indirectly by reduce the inflammatory status among the gingiva. By the above facts, we proposed a newly intra-oral device via dental implant to achieve long-term painless and continuous insulin releasing and blood sugar monitoring. We introduce the mechanism to avoid painful sensations during insulin releasing and blood sugar monitoring. We also introduce the relative considerations for the device applied in diabetes. With proper improvements and standard procedure establishments under safety considerations, the newly device may have potential to achieve painless insulin releasing and blood sugar monitoring.
Keywords
Diabetes mellitus (DM), Dental implant, Insulin, Blood sugar monitoring
Current Situations about Diabetes Mellitus
As medical and technological improvements, life expectancy has been prolonged and Geriatric care is therefore become an important issue in the twenty-first century. For example, one third of the Europeans may more than 65 years old in 2035 [1-3], and the elderly in the United States may reach 70 million before 2030 [2]. The main purpose of Geriatric care is to improve life qualities throughout those critical and chronic diseases. On the other hand, Diabetes Mellitus (DM) has been regarded as the major chronic health problems since this metabolic disorder affects 15.7 individuals, which is approximately 5.9% of the population in the United States [4]. Furthermore, estimated 18.4% of the population above 65 years old suffered from this metabolic disease. DM is commonly divided into two pathogenic types including insulin-dependent (type 1; IDDM), and non-insulin dependent (type 2; NIDDM). Most patients belong to type 2 DM (> 90%), while 5% of them are type 1 diabetics. According to the current standard procedure, patients suffering from diabetes would receive multiple dosages of insulin injections (MDII) regularly in the later stages, and intra-venous insulin injections (IVII) in the emergent condition in hospital [5]. Here MDII therapy requires four times of blood sugar detections and subcutaneous insulin injections per day regularly, and IVII therapy performs twelve times of the above invasive procedures per day. These procedures may bring major sufferings and should be regarded as unbearable. Therefore we will provide another possibility for regular diabetes management in this article to improve the life quality among the elderly and promote geriatrics. First we will discuss the current correlations between diabetes and dentistry, including the importance of oral hygiene maintenance in diabetes, surgical concern in dental implantology within diabetes conditions, and the improvement of implant prosthesis among diabetes patients.
The Relationships between Diabetes and Dental Implant
Infection control in diabetes patients is extremely important to avoid further relative complications including cellulitis, diabetic ketoacidosis (DKA), and hyperglycemic hyperosmolar nonketotic syndrome (HHNK), which may end up with amputations or even mortality [6-9]. Unfortunately, the diabetes status may increase the risks of infection due to hypoxia, higher blood osmolality, and other relative factors that lead to delay wound healing [10].
Due to the higher risks of infection status, the surgical concern in dental implant has been broadly discussed. In general, diabetes under regular blood sugar control is not regarded as a contraindication in dental implant [11]. Raj reported that diabetes may have negative influences on bone formations and remodeling, but the overall implant failure rate is low and diabetes should not be a contraindication for implant placement [12]. Klokkevold and Han reported that the dental implant survival rate among diabetes is 91.7% compare to 93.2% in healthy patients [13]. Mellado-Valero also reported a range of one year survival rate between 88.8% and 97.3% in diabetes [14]. To sum up, the overall dental implant successful rate in diabetic patients under regular blood sugar control is approximately around 90% and shows no significant differences from other patients without the disease [15].
On the other hand, there exist high correlations between diabetes and periodontitis inside the oral cavity. That means uncontrolled periodontitis with poor oral hygiene may worsen the diabetes status, and affect the blood sugar control by bacterial infiltrations throughout the inflammatory gingiva with bleeding tendency [16]. As a result, proper implant restorations may increase mucosal health and maintain oral hygiene, which may have benefits in further blood sugar control [17]. Finally, gangrenous necrosis seldom occurs in the oral cavity due to rich of blood supply and the moist environments provide by saliva. All of the above background conditions may allow us to design a long-term drug releasing and bio-sensing device based on the dental implant. Then we will introduce the device and the relative benefits along with the limitations for diabetic applications in detail.
Basic Design of the Dental Implant Supported Semi-Implanted Device
Frequently direct blood sugar monitoring and insulin releasing into blood is essential in the later stage diabetes to control infectious status and avoid further complications. However, the procedure is invasive and inevitably leads to unbearable irritations and stress eventually. Basically the painful sensation is carried out by nociceptors, the free, branching, and unmyelinated nerve endings that stimulated by the potential to arise tissue damage. Pain from face and neck is mainly passing through the Trigeminal Pain Pathway by the second-order sensory neurons in the spinal trigeminal nucleus. Then these cells may cross the midline of the spinal cord and send the pain message ascending to the thalamus in the trigeminal lemniscuses [18]. Aδ and C neural fibers that carry noxious sensory information are both belong to the primary afferent fibers, which are responsible for the sharp, localized and the dull with diffused pain. In our oral cavity, the main origins to arise painful sensations from tooth structure are mainly from (a) the pulp structure, and (b) the periodontal ligament (PDL), where the pulp will induce sharp and unbearable pain, and PDL may bring the dull pain with swelling sensations similar to skins. Finally with the replacement from natural tooth to the pure titanium implant fixture (c), both of the two major pain origins are removed and lead to the relative painless conditions as shown in figure 1.
.
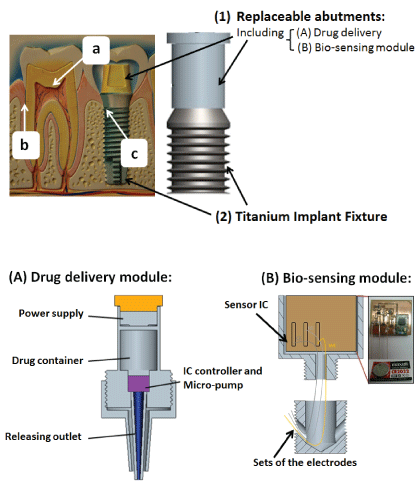
Figure 1: The basic concept of the dental implant supported drug delivery (A) and bio-sensing module (B) [19]. Both of the two modules belong to the replaceable abutment (1) above the titanium implant fixture (2), which is placed into the jaw bone after natural tooth extraction with removal of the pulp structure (a) and PDL (b).
View Figure 1
Basically the standard dental implant system contains the two major components including (1) the replaceable prosthetic abutment exposed to the outside oral cavity, and (2) the pure titanium implant fixture submerged into the jaw bone marrow structure. Figure 1 shows the basic design of the dental implant supported device and the mechanism to avoid painful sensations [19]. The (A) drug delivery and (B) bio-sensing modules are designed replaceable above the implant fixture. Then there are a set of channels inside the titanium implant fixture with outlets responsible for outside bone marrow connections. The drug delivery module contains a power supply, a drug container, a piezoelectric micro-pump and the drug releasing outlets below the module. The loading drug may be both in liquid type or slightly polymerized to prevent from micro leakage and further safety problems. While the bio-sensing module contains the power supply, the integrated circuit (IC), the wireless module, and a set of electrodes including working, counter, and reference ones that extended into the outside bone marrow.
Discussions about the Intra-Oral Device for Diabetic Applications
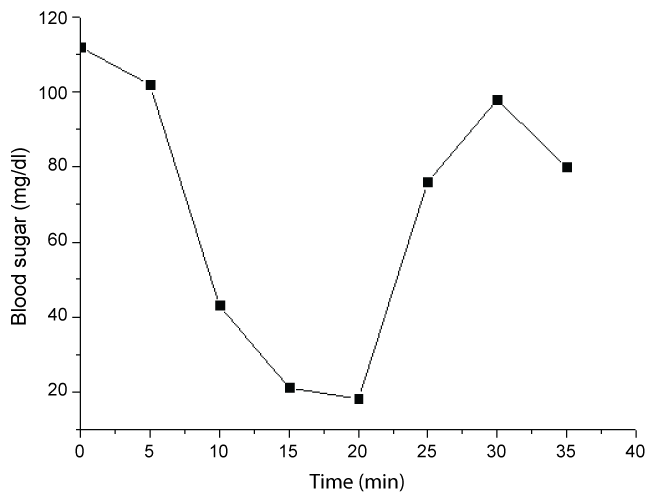
The preliminary study and experiments to prove the newly intra-oral and semi-implanted design have been published [19]. We also performed the preliminary canine model for the efficiency evaluation. The one-year-old canine's bilateral maxillary first premolar was extracted, and then two of the 6 × 5 mm Bicon© titanium fixtures with the created cannels in the apical sides were implanted over bilateral maxilla on premolar area under barbiturate anesthesia. After 1 month of primary osseointegration, the drug delivery module is placed above its right hand side, while the bio-sensing module is on the opposite. Then we loaded 5 units of the Neutral Protamine Hagedorn (NPH) as the rapid onset insulin via the drug delivery module at the right hand side, and monitored the blood sugar value at the opposite every 5 minutes for 35 minutes. The results are shown in figure 2. After 5 units of insulin administration, the blood sugar decreased rapidly within 5 minutes and last for about 20 minutes. Then it rebounded at the 20th minute due to the reactive glucogen releasing. Finally the blood sugar value present in 80 mg/dl at the 35th minute. The preliminary canine study may present the efficiency of the drug delivery module in insulin releasing.
.
Figure 2: The blood sugar changes in the canine model after loading 5 units of insulin [19]. The blood sugar value decreased rapidly, and then rebound due to the reactive glucogen releasing.
View Figure 2
We should notice that this design is not limited in diabetes applications, but here we will discuss in detail about clinical concern for diabetic applications as following:
(1) The other continuous blood sugar monitoring device has been reported lasting for about 1 month (28 days) and realized in animal study [20]. Of course it is not sufficient for clinical applications as the normal human body implanted device because additional surgical procedures may be needed for further component exchanges monthly. But that has been already suitable in our intra-oral device, because the intra-oral implant supported device has the properties of semi-implanted. That means the device is not totally implanted into human body, while the above prosthetic abutment is exposed into the oral cavity. The fact allows the abutment become replaceable without additional surgical procedures, and thus minimizes the irritations and lower down the discomfort with such device applications.
(2) Since diabetes under regular blood sugar control is not regarded as a contraindication for dental implant, and the survival rate among the diabetic patient is approximately around 90%, to realize such device into practical applications seems possible with current technology supported. Furthermore, combination drug delivery may achieve throughout this module by mixture of insulin with other anti-bacterial agent to lower down the infection risks. For example, calcium hydroxide has been recognized by its antimicrobial effects and further stimulated mineralization toward the alveolar hard tissue since first announced by Herman in 1920 [21-24]. Topical applications of calcium hydroxide may reduce initial inflammation and promote new bone formation within 1 to 2 months. In addition, Iodoform (CHI3) and its mixture with calcium hydroxide also present the antimicrobial activity and capacity to promote periapical healing [25-27]. Mixtures of the above agents may enhance the antimicrobial efficiency during the intra-bony drug delivery process.
On the other hand, the continuous bio-sensor may also contribute in blood sugar monitoring, which will result in healthier periodontal condition indirectly.
(3) The total loading volume is around 1 ml, which depends both on the abutment size and the width of the edentulous ridge. While some may think that not sufficient for normal diabetic dosage. But the concentration of insulin may be adjusted according to the module demand individually. For traditional intravenous injections, lower insulin concentration will increase the accuracy for drug loading and ensure the safety. However, drug releasing toward such intra-oral device may be much similar to dissolve into the surrounding bone marrow structures rather than directly push into it to lower down the bearing stress and avoid unnecessary injury including surrounding bony resorptions. Actually such drug delivery pathway has been mature in endodontic applications during root canal treatments [25]. In addition, other continuous insulin releasing devices, also known as the insulin pumps, have been the commercial products for more than 35 years [28]. Within proper concentration, the insulin pump may provide the average capacity around 300 units per loading. Currently there is no evidence that insulin induces surrounding bony resorptions. However, long-term animal study arrangement is needed for further histological improvements.
(4) The intra-oral modules should be regarded as the assistance for diabetic management. That means it may provide daily blood sugar monitoring and a baseline insulin supplement. Once when the blood sugar increasing reaches a certain degree, additional subcutaneous insulin injection is still needed. However, such device has been sufficient to lower down most of the sufferings when receiving standard diabetic procedures.
(5) Further dental support including device maintenance, standard disinfection procedure, implantitis condition monitoring under regular clinical appointment is strongly recommended to ensure its normal functions.
Actually the development of such newly device is undergoing, and it is still not mature currently. Fortunately, most of the challenges remain in the technological aspects and seems achievable. Basically it is possible whether in dental, medical aspects theoretically or even in the preliminary canine studies. However, more experiments, improvements and further clinical studies along with the histological proves are still needed.
Acknowledgments
Special thanks to Associate Prof. Chih-Cheng Lu of National Taipei University of Technology and his advanced microsystem and device laboratory for the technological support. Valuable assistance from Prof. Jung-Tang Huang of National Taipei University of Technology is also acknowledged. This research received financial support under grants MOST 103-2221-E-027-017 and MOST 103-2218-E-027-012, Taiwan.
References
-
http://www.aal-europe.eu
-
Iliev TI, Tabakov DS, Dotswinsky AI (2011) Automatic fall detection of elderly living alone at home environment. Global Journal of Medical Research 11: 49-53.
-
COOP-005935-HEBE, Cooperative research project- CRAFT, (2006) Automatic fall detection and activity monitoring for elderly. April 5-7.
-
Bethesda MD (1995) Diabetes in America. National Diabetes Data Group, National Institutes of Health., 2nd Ed. Publication 95-1468.
-
Weng J, Li Y, Xu W, Shi L, Zhang Q, et al. (2008) Effect of intensive insulin therapy on β-cell function and glycaemic control in patients with newly diagnosed type 2 diabetes: A multicentre randomised parallel-group trial. Lancet 371: 1753-1760.
-
Lipsky BA, Berendt AR, Cornia PB, Pile JC, Edgar JG, et al. (2012) 2012 infectious diseases society of America clinical practice guideline for the diagnosis and treatment of diabetes foot infections. Clinical Infectious Diseases 54: 132-173.
-
Pischke MA (2001) Diabetic ketoacidosis. Physician Assistant 25: 42-48.
-
Venkatraman R, Singhi SC (2006) Hyperglycemic hyperosmolar nonketotic syndrome. Indian J Pediatr 73: 55-60.
-
Lipsky BA, Berendt AR, Deery HG, Embil JM, Joseph WS, et al. (2004) Diagnosis and treatment of diabetic foot infections. Clin Infect Dis 39: 885-910.
-
Chin-Hong PV (2006) Infections in patients with diabetes mellitus: Importance of early recognition, treatment, and prevention. Adv Stud Med 6: 71-81.
-
Judith A, Anthony von Fraunhofer J (2005) Success or failure of dental implants? A literature review with treatment considerations. General Dentistry 20050.
-
Raj KC, Swapna M, Amit K, Namrata SN (2014) Osseointegration of dental implants in diabetic patients-A review. American Journal of Advances in Medical Science 2: 1-8.
-
Klokkevold PR, Han TJ (2007) How do smoking, diabetes, and periodontitis affect outcomes of implant treatment? Int J Oral Maxillofac Implants 22: 173-202.
-
Mellado-Valero A, Ferrer-Garcia JC, Herrera-Ballester A, Labaig-Rueda C (2007) Effects of diabetes on the osseointegration of dental implants. Med Oral Patol Oral Cir Bucal 12: 38-43.
-
Farzad P, Andersson L, Nyberg J (2002) Dental implant treatment in diabetic patients. Implant Dent 11: 262-267.
-
Carpenter JF (2010) Management of a patient who develop uncontrolled diabetes after implant placement: A case report. Journal of Implant & Advanced Clinical Dentistry 2: 81-87.
-
Peled M, Ardekian L, Tagger-Green N, Gutmacher Z, Machtei EE, et al. (2003) Dental implants in patients with type 2 diabetes mellitus: A clinical study. Implant Dent 12: 116-122.
-
Bear MF, Connors BW, Paradiso MA (2007) Neuroscience; Exploring the brain. Third edition. Lippincott Williams & Wilkins, ISBN: 0-7817-6003-8.
-
Li YJ, Lu CC (2015) A novel scheme and evaluations on a long-term and continuous biosensor platform integrated with a dental implant fixture and its prosthetic abutment. Sensors 15: 24961-24976.
-
Brockway R, Coskun T, O'Farrell LS, Haefner P, White K, Jackson CV, Peterson RG (2013) Continuous glucose monitoring via telemetry in rats. Poster 1099, European Association for the Study of Diabetes Annual Meeting, Barcelona, Spain.
-
Estrela C, Holland R (2003) Calcium hydroxide: Study based on scientific evidences. J Appl Oral Sci 11: 269-282.
-
Siqueira JF, Lopes HP (1999) Mechanisms of antimicrobial activity of calcium hydroxide: a critical review. Int Endod J 32: 361-369.
-
Mohammadi Z, Dummer PMH (2011) Properties and applications of calcium hydroxide in endodontics and dental traumatology. Int Endod J 44: 697-730.
-
Mustafa M, Saujanya KP, Jain D, Sajjanshetty S, Arun A, Uppin L, Kadri M (2012) GJMEDPH 1: 66-70.
-
Nurko C, Ranly DM, Garcia-Godoy F, Lakshmyya KN (2000) Resorption of a calcium hydroxide/iodoform paste (Vitapex®) in root canal therapy for primary teeth: A case report. Pediatr Dent 22: 517-520.
-
Kuga MC, Faria G, So MV, Keine KC, Santos AD, et al. (2014) The impact of the addition of iodoform on the physicochemical properties of an epoxy-based endodontic sealer. J Appl Oral Sci 22: 125-130.
-
Gautam S, Rajkumar B, Landge SP, Dubey S, Nehete P, et al. (2011) Antimicrobial efficacy of Metapex (calcium hydroxide with iodoform formulation) at different concentrations against selected microorganisms-An in vitro study. Nepal Med Coll J 13: 297-300.
-
Grunberger G, Jill M, Bailey TS, Bode BW, Handelsman Y, et al. (2014) Task force for insulin pump management. AACE/ACE Consensus Statement, Endocr Pract 20: 463-489.





