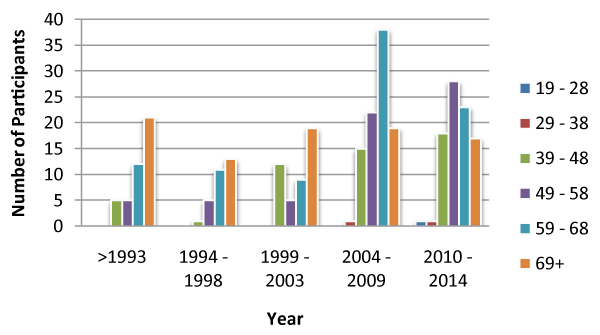International Journal of Diabetes and Clinical Research
Trends in the Occurrence of Type 2 Diabetes in Community-Dwelling Trinidadian Subjects, 1993-2014
Koreen Peter, Lilly Paul, Renee Richardson, Brandon Ramdass, Aisha Ali and Kameel Mungrue*
Faculty of Medical Sciences, Department of Paraclinical Sciences, The University of the West Indies, Trinidad
*Corresponding author:
Kameel Mungrue, Faculty of Medical Sciences, Department of Paraclinical Sciences, The University of the West Indies, EWMSC, Mt Hope, St Augustine, Trinidad, Tel: 868-645-2018, Fax: 868-645-2018 , E-mail: Kameel.Mungrue@sta.uwi.edu
Int J Diabetes Clin Res, IJDCR-2-026, (Volume 2, Issue 2), Research Article; ISSN: 2377-3634
Received: February 07, 2015 | Accepted: March 22, 2015 | Published: March 24, 2015
Citation: Peter K, Paul L, Richardson R, Ramdass B, Ali A, et al. (2015) Trends in the Occurrence of Type 2 Diabetes in Community-Dwelling Trinidadian Subjects, 1993-2014. Int J Diabetes Clin Res 2:026. 10.23937/2377-3634/1410026
Copyright: © 2015 Peter K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective: The purpose of this study is to examine secular trends in the occurrence of type 2 diabetes in community-dwelling Trinidadian subjects.
Methods and design: We selected two regions in Trinidad and identified communities where people both live and seek health care services. We used several definitions of type 2 diabetes to recruit participants. Data on age, gender, onset of illness and educational level as a marker of socioeconomic status was collected.
Findings: 301 participants were entered into the study. There was ethnic disparity but a reversal from South East to Africans. A strong inverse linear relationship (Pearson�s coefficient r=-0.82, p ≤ 0.05) was found between BMI and age at diabetes onset. Between the 1990�s and 2004-2014 in two regions of Trinidad the number of patients with T2DM doubled, occurring more commonly among females, the obese and overweight, a tendency towards younger age groups and those of lower socioeconomic status (SES).
Conclusion: We provide evidence that at the community level that the occurrence of T2DM is increasing, and shifting towards younger age groups.
Introduction
Type 2 diabetes (T2DM) is a global public health crisis that threatens the economies of all nations, particularly developing countries. Fueled by rapid urbanization, population growth, increasing life expectancy, nutrition transition, and increasingly sedentary lifestyles, the epidemic has grown in parallel with the worldwide rise in obesity in both adults and adolescents. [1,2]. The burden of type 2 diabetes and its complications, including macro- and microvascular complications, are increasingly recognized as a global health priority. The estimated prevalence of diabetes in Trinidad reported by the International Diabetes Federation is 13.9% [3], one of the highest in the region of the Americas, with the total number of cases (20-79) years at 2013, being 132 340. The mean health care expenditure per person with diabetes is estimated at $1212 (USD). [3]
Reliable estimates of secular trends in the prevalence of T2DM and quantifying the number of people affected, now and in the future, is important to allow for rational planning, allocation of resources and effective strategies for prevention and management [4]. In addition comprehensive and up-to-date survey data at the community level helps to identify potential gaps in care, and to monitor and evaluate the provision of treatment to patients in the most efficient manner.
The purpose of this study is to examine secular trends in the occurrence of type 2 diabetes in community-dwelling Trinidadian subjects.
Methods
We used a cross sectional study design. The population consisted of all adult patients (>18 years) with T2DM, residing in the community and receiving care at the main primary health care facility (PHCF) serving that community. In Trinidad there are four Regional Health Authorities (RHA) that deliver care to well demarcated communities. The communities chosen for this study came from two of these RHA, the North-Central RHA and the Eastern RHA. The two main PHCF serving these communities were selected for the conduct of the study. The starting point was the identification of all patients who met the criteria for T2DM. We defined T2DM as a physician diagnosis as well as satisfying the WHO criteria i.e. � a fasting plasma glucose ≥ 7.0mmol/l (126mg/dl) or 2�h plasma glucose ≥ 11.1mmol/l (200mg/dl), or an HbA1c of >7%. [4]. Patients who met these criteria were invited to participate in the study. All patients with gestational diabetes or type 1 diabetes were excluded from the study. All data were collected using a specifically designed data collection instrument, which include demographic data, i.e. age, gender, ethnicity, body mass index (BMI), education level and treatment. Body mass index (BMI) was based on measured height and weight on physical examination. BMI is computed as weight in kilograms divided by height in meters squared (kg/m2). BMI was defined according to standard methods, normal (less than 25), overweight (25�29.99) and obese (30 or greater) [5]. Educational level was classified into five categories based on access to education in Trinidad. All data was stored, retrieved and analyzed using SPSS version 22. A p ≤ 0.05 was considered significant. Ethical approval for this study was obtained from the Ethics Committee of the University West Indies St Augustine.
Results
There were 301 participants who satisfied the entry criteria and were available for analysis. The study participants consisted of 194(64.5%) from one PHCF (1) and 107(35.5%) from the PHCF (2). The mean age was 60.78 years (SD ± 11.5) with an interquartile range of 51-70 years, table 1. There are two major diaspora in Trinidad, Africans and South East Asians (SA) both representing approximately 35% of the population respectively. While other studies have shown that T2DM is more common in SA than Africans [6], we had significantly (p< .05) more Africans (42%) than SA (33.2%) receiving treatment at the PHCF we studied. There were more females (179, 59.5%) than males 122 (40.5%), f:m 1.5:1. The proportion of participants classified as overweight or obese was 66% (191), while 73(24.3%) were obese. An inverse linear relation was found between BMI and age at diabetes onset. Adults with early diagnosed diabetes were more obese and more likely to be female than were adults with a later onset of type 2 diabetes. The overwhelming majority (82.4%) of participants attained only a secondary level of education which is now universal in Trinidad.
![]()
Table 1: Demographic and other characteristics of the sample
View Table 1
We enquired from each participant the year in which they were first diagnosed with T2DM and found that in this setting there were twice as many people diagnosed with T2DM between in 2004-9 and 2010-14 compared to 1994-1998 and 1999-2003, figure 1. Therefore between the 1990�s and 204-14 in two areas in Trinidad the number of cases with T2DM increased by 100%. Further studies are required to determine the causes of this increase.
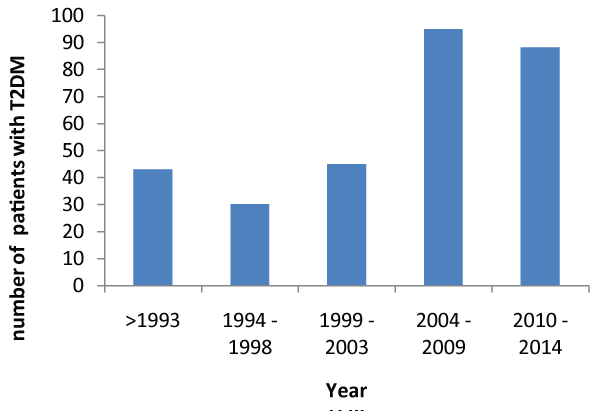
Figure 1: Bivariate relationship between the number of patients admitted and treated in a primary care setting for T2DM and time (calendar years).
View Figure 1
In addition to the year of diagnosis we also enquired about the age at first diagnosis, figure 2, and showed that while the age group >69 years remained fairly constant over time, from 2004-09 for the first time there were participants in the age group 29-38 years and similarly in 2010-14 for the first time there were participants in the age group 19-28 suggesting that T2DM is occurring in younger age groups (Table 1).
Discussion
The results of this study indicate a rapid raise in the number of adults who meet the criteria for T2DMduring the first decade of the 21st century. These patients are currently receiving treatment at the primary care level. This rapid rise in such a short period of time is particularly disturbing because it suggests that large changes at the population level can occur in a relatively short period of time. If there is no coordinated response to arrest this increase in T2DM, the consequences are formidable. Increases in health expenditure, diabetic complications and cardiovascular morbidity and mortality are all likely to occur. These findings are particularly problematic given the strong association of T2DMand an array of both micro and macrovascular complication. Therefore, these findings have important implications for the debate on introducing stratergies such as health checks and other public health interventions to arrest the progression to overt diabetes.An effective and determined program of policies and actions is mandatory. These findings are also relevant to other countries considering challenged by increasing levels of T2DM.
At the two PHCF studied for the first time in 2010-2014 there were patients with T2DM in the age group 19-28, a disease once thought to be a metabolic disorder exclusively of adulthood [7]. This trend in the occurrence of T2DM is not unique to our setting. For example, in Japan 80% of all new cases of diabetes in children and adolescents were diagnosed as T2DM [7]. Similar patterns have been reported in Taiwan [8], and to a less extent in Europe, U.K. and the U.S.A. [9,10]. T2DM is progressive, resulting in a gradual decline in β-cell function [11]. Overt T2DM does not occur until β-cells fail to respond appropriately to peripheral insulin resistance. The ability of the β-cell to secrete sufficient insulin to adequately respond to the peripheral insulin resistance state depends on multiple factors. These include β-cell mass [12] and secretory capacity [13], which is influenced by genetic [12] and environmental factors [12]. While little can be done in regard to genetic factors, much can be achieved by tackling environmental factors. Improving the physical environment such as increasing availability of healthy food choices and opportunities for physical activity together with a structured lifestyle-change program is vital to reducing T2DM among people at high risk. Both randomized clinical trials and real-world implementation studies have proven that structured lifestyle-change programs can help prevent or delay T2DM by 60% in people with pre-diabetes [13,14].
Our data show that overweight (39%) and obesity (24%) are common in a population of type 2 diabetic patients attending diabetes clinics, in keeping with known epidemiological associations [15-23]. Obesity is the major potentially modifiable risk factor for type 2 diabetes [24]. Early obesity and almost any weight gain after adolescence are risk factors for type 2 diabetes [20,23]. Further Schienkiewitz and colleagues concluded that weight gain in early adulthood is related to a higher risk and earlier onset of type 2 diabetes than is weight gain between 40 and 55 years of age [25]. Using educational level, as a socioeconomic indicator there is a considerable burden of T2DM associated with lower levels of educational attainment in Trinidad. This finding is consistent with the literature [26].
The strengths of our study were the uniform ascertainment of diabetes and related variables over the time interval. Nevertheless, several limitations deserve mention. First, the secular patterns we observed were based entirely on cross-sectional data; therefore, these results may have been influenced by survival and/or selection bias. Secondly information on diabetes risk factors, such as dietary intake and family history of diabetes, were not available. Hence, we could not rule out the possibility of residual confounding.
In conclusion, we provide evidence that at the community level that the occurrence of T2DM is increasing, and shifting towards younger age groups. Obesity may be the driving factor in the pathogenesis of T2DM, although we were not able to quantify the contribution to current BMI of potentially avoidable weight gain. Nevertheless this evidence is critical for the future planning, allocation of resources and effective strategies for the prevention and management of T2DM.
References-
King H, Aubert RE, Herman WH (1998) Global burden of diabetes, 1995�2025: prevalence, numerical estimates, and projections. Diabetes Care 21: 1414-1431.
-
Pinhas-Hamiel O, Zeitler P (2005) The global spread of type 2 diabetes mellitus in children and adolescents. J Pediatr 146: 693-700.
-
International Diabetes Federation (2013) Diabetes in Trinidad and Tobago - 2013.
-
Wild S, Roglic G, Green A, Sicree R, King H (2004) Global prevalence of diabetes: estimates for the year 2000 and projections for 2030. Diabetes Care 27: 1047-1053.
-
(1998) Executive summary of the clinical guidelines on the identification, evaluation, and treatment of overweight and obesity in adults. Arch Intern Med 158: 1855-1867.
-
World Health Organization (1999) Definition, diagnosis and classification of diabetes mellitus and its complications: report of WHO consultation. (WHO/NCD/NCS/99.2). Part 1: Diagnosis and Classification of Diabetes Mellitus. Geneva: World health Organization.
-
Fagot-Campagna A, Pettitt DJ, Engelgau MM, Burrows NR, Geiss LS, et al. (2000) Type 2 diabetes among North American children and adolescents: an epidemiologic review and a public health perspective. J Pediatr 136: 664-672.
-
Kahn SE, Hull RL, Utzschneider KM (2006) Mechanisms linking obesity to insulin resistance and type 2 diabetes. Nature 444: 840-846.
-
Lyssenko V, Jonsson A, Almgren P, Pulizzi N, Isomaa B, et al. (2008) Clinical risk factors, DNA variants, and the development of type 2 diabetes. N Engl J Med 359: 2220-2232.
-
Ali MK, Echouffo-Tcheugui J, Williamson DF (2012) How effective were lifestyle interventions in real-world settings that were modeled on the Diabetes Prevention Program? Health Aff (Millwood) 31: 67-75.
-
Katula JA, Vitolins MZ, Morgan TM, Lawlor MS, Blackwell CS, et al. (2013) The Healthy Living Partnerships to Prevent Diabetes study: 2-year outcomes of a randomized controlled trial. Am J Prev Med 44: S324-332.
-
Knowler WC, Barrett-Connor E, Fowler SE, Hamman RF, Lachin JM, et al. (2002) Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med 346: 393-403.
-
Guide to Community Preventive Services (2014) Combined diet and physical activity promotion programs to prevent type 2 diabetes among people at increased risk. [www.thecommunityguide.org] Accessed September 17, 2014.
-
Wilson PW, Anderson KM, Kannel WB (1986) Epidemiology of diabetes mellitus in the elderly. The Framingham Study. Am J Med 80: 3-9.
-
Holbrook TL, Barrett-Connor E, Wingard DL (1989) The association of lifetime weight and weight control patterns with diabetes among men and women in an adult community. Int J Obes 13: 723-729.
-
Lundgren H, Bengtsson C, Blohme G, Lapidus L, Sj�str�m L (1989) Adiposity and adipose tissue distribution in relation to incidence of diabetes in women: results from a prospective population study in Gothenburg, Sweden. Int J Obes 13: 413-423.
-
Kaye SA, Folsom AR, Sprafka JM, Prineas RJ, Wallace RB (1991) Increased incidence of diabetes mellitus in relation to abdominal adiposity in older women. J Clin Epidemiol 44: 329-334.
-
Haffner SM, Mitchell BD, Hazuda HP, Stern MP (1991) Greater influence of central distribution of adipose tissue on incidence of non-insulin-dependent diabetes in women than men. Am J Clin Nutr 53: 1312-1317.
-
Everhart JE, Pettitt DJ, Bennett PH, Knowler WC (1992) Duration of obesity increases the incidence of NIDDM. Diabetes 41: 235-240.
-
Chan JM, Rimm EB, Colditz GA, Stampfer MJ, Willett WC (1994) Obesity, fat distribution, and weight gain as risk factors for clinical diabetes in men. Diabetes Care 17: 961-969.
-
Perry IJ, Wannamethee SG, Walker MK, Thomson AG, Whincup PH, et al. (1995) Prospective study of risk factors for development of non-insulin dependent diabetes in middle aged British men. BMJ 310: 560-564.
-
Hanson RL, Narayan KM, McCance DR, Pettitt DJ, Jacobsson LT, et al. (1995) Rate of weight gain, weight fluctuation, and incidence of NIDDM. Diabetes 44: 261-266.
-
Colditz GA1, Willett WC, Rotnitzky A, Manson JE (1995) Weight gain as a risk factor for clinical diabetes mellitus in women. Ann Intern Med 122: 481-486.
-
Pinkney J (2002) Prevention and cure of type 2 diabetes. BMJ 325: 232-233.
-
Schienkiewitz A, Schulze MB, Hoffmann, Anja Kroke K, Boeing H (2006) Body mass index history and risk of type 2 diabetes: results from the European Prospective Investigation into Cancer and Nutrition (EPIC)�Potsdam Study. Am J Clin Nutr 84: 427-433.
-
Wannamethee SG, Shaper AG, Walker M (2005) Overweight and obesity and weight change in middle aged men: impact on cardiovascular disease and diabetes. J Epidemiol Community Health 59: 134-139.
-
Agardh E, Allebeck P, Hallqvist J, Moradi T, Sidorchuk A (2011) Type 2 diabetes incidence and socio-economic position: a systematic review and meta-analysis. Int J Epidemiol 40: 804-818.