International Journal of Cancer and Clinical Research
Pigmented Paget Disease of the Nipple: A Rare Breast Cancer Presentation
Santiago Sherwell-Cabello1*, Antonio Maffuz-Aziz1, Silvia Natalia Lopez-Hernández1, Melissa Lizeth Flores-Cortés1, Veronica Bautista-Pina2 and Sergio Rodriguez-Cuevas1
1Department of Breast Surgery, Instituto de Enfermedades de la Mama, México
2Department of Pathology, Instituto de Enfermedades de la Mama, México
*Corresponding author:
Santiago Sherwell-Cabello, Instituto de Enfermedades de la Mama, FUCAM AC, Bordo 100, StaUrsula Coapa, Coyoacan 04980, Mexico City, Mexico, Tel: +52-55-5678-0600, E-mail: sherwell@gmail.com
Int J Cancer Clin Res, IJCCR-3-073, (Volume 3, Issue 6), Short Review; ISSN: 2378-3419
Received: March 03, 2016 | Accepted: November 23, 2016 | Published: November 26, 2016
Citation: Sherwell-Cabello S, Maffuz-Aziz A, Lopez-Hernández SN, Flores-Cortés ML, Bautista-Pina V, et al. (2016) Pigmented Paget Disease of the Nipple: A Rare Breast Cancer Presentation. Int J Cancer Clin Res 3:073. 10.23937/2378-3419/3/6/1073
Copyright: © 2016 Sherwell-Cabello S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objetive: To show the incidence and clinical characteristics of the patients diagnosed with Pigmented Paget Disease in our Institution. In addition, we present the pathological and immunohistochemical criteria for a precise diagnosis.
Materials and methods: Institutional board approval was obtained before commencement of this study. A retrospective study was conducted in all women diagnosed with breast cancer at our institution from January 2005 to December 2013. Standard immunohistochemical breast cancer panel was performed to all patients (ER, PR, Her-2 and Ki-67) and CK-7, P63 and S-100 when the pigmented variety was presented. Patients with pigmented Paget disease were selected and demographic characteristics were established.
Results: Between January 2005 and December 2014, 4148 patients were diagnosed with breast cancer at our institution; Paget disease was found in 69 patients (1.66%), six of them showed the pigmented variety (8.7%). Two of them presented pure Pigmented Paget's disease, while four an invasive component associated. CK-7 was positive in the 6 patients and overexpression of Her-2 in 5 patients, while P63 and PS100 were negative in all patients. The median follow-up was 33.8 months (13-59). No patient developed local or distant recurrence.
Conclusions: Pigmented Paget is a rare entity found in the 8.7% of the patients with Paget disease. Histological with immunohistochemical assessment is essential for diagnosis. Clinical stage should be defined by the invasive component, if it exists. Treatment should be given as in any other mammary Paget disease of the breast, since prognosis is not affected by this kind of presentation.
Keywords
Pigmented paget disease, Breast cancer, Melanoma
Abbreviations
FUCAM: Breast Disease Institute FUCAM; ER: Estrogen Receptors; PR: Progesterone Receptors; HER-2: Human Epidermal Growth Factor 2 Receptor Protein; CK-7: Cytokeratin 7
Introduction
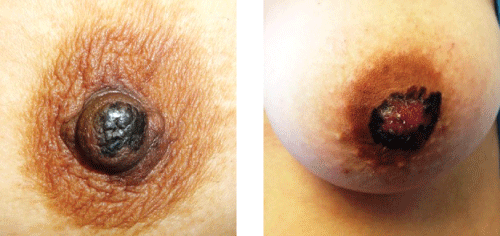
Pigmented Paget Disease is an extremely infrequent form of presentation of mammary Paget disease. It is characterized by a hyperpigmented macula in the nipple or areola with an underlying breast carcinoma [1,2]. Eczema and erythema in the Nipple-areola complex (NAC) could be often associated [3] Trough this study we pretend to show the incidence and clinical characteristics of the patients diagnosed with Pigmented Paget Disease in the Instituto de Enfermedades de la Mama, FUCAM. In addition, we present the pathological and immunohistochemical criteria for a precise diagnosis.
Materials and Methods
Institutional board approval was obtained before initiation of this study. A retrospective study was conducted in all women diagnosed with breast cancer at our institution, from January 2005 to December 2014. Patients with Pigmented Paget disease were selected and demographic characteristics were established.
TNM/AJCC stage (Tumor, Node, Metastases/American Joint Committee on Cancer) were all evaluated during the tumor board sessions [4]. Multimodal treatments were administered according to the NCCN Breast Cancer Clinical Practice Guidelines [5]. Pathological and immunohistochemical diagnostic protocols were applied. Immunohistochemical panel was performed according to the American Society of Clinical Oncology and the College of American Pathologists and molecular phenotypes were determined according to the St. Gallen International Breast Cancer Conference [6-8]. Standard immunohistochemical breast cancer panel was routinely performed to all patients with breast cancer in the invasive component, if present (ER, PR, Her-2 and Ki-67). In order to rule out other diseases, when pigmented Paget disease was found, supplementary especial stains were applied directly in the pigmented area. CK-7, Her-2, P63 and S-100 were used in these cases.
Results
Between January 2005 and December 2014, 4148 patients were diagnosed with breast cancer at FUCAM; 69 patients, with invasive or in situ carcinoma, were diagnosed with Paget disease (1.66%). The pigmented variety was shown in six of these patients (8.7%). The mean age of the patients with the pigmented variety was 64.2 years (49-79), and 62.5 years in the rest of patients with Paget disease (44-78).
Analysing in detail the pigmented category, we found that two patients presented a pure Pigmented Paget disease, without infiltrating component found in the surgical specimen. Both patients were treated with wide excision of the Nipple Areola Complex (NAC). Invasive component was detected in the other four patients. Clinical stages are presented in table 1.
![]()
Table 1: Clinical stages (TNM) in patients with pigmented paget disease.
View Table 1
![]()
Table 2: Immunohistochemical panel in pigmented cells.
View Table 2
Discussion
Described in 1874, Paget's disease accounts for approximately 1 to 3% of all breast cancers [9,10]. This condition is associated with ductal carcinoma in situ and infiltrating ductal carcinoma in 87 to 100% of cases. When it is associated with an invasive component, it is usually more aggressive, with high histological grade, positive axillary nodes and the absence of hormone receptor expression [11].
The usual presentation of Paget's disease is through eczematous changes in the Nipple-Areola Complex (NAC), said itching, scaling and erythema. There is a rare variant of Paget's disease that may mimic melanoma. This form is known as Pigmented Paget disease. It is characterized by the presence of hyperpigmented macules on the NAC (Figure 1).
When the pagetoid component is only present, just 35 to 50% of cases will have some suggestive mammographic manifestations of malignancy [3]. These changes will be characterized by distortion of architecture and periareolar skin thickening of the NAC.
Pigmented Paget's disease is a rare entity, difficult to distinguish from other conditions such as squamous cell carcinoma of the nipple and melanoma in situ of the nipple, which also presents with pagetoid spread.
Paget pigmented cells have a melanin-like pigment which is believed to be transferred by melanocytes. The exact physiopathology remains unknown, but some theories describe a proliferation of melanocytes stimulated by chemotactic factors produced by neoplasic cells; Paget cells phagocyte melanin from melanocytes and finally there is a transference blockage of pigment from melanocytes to keratinocytes (Figure 2a) [12].
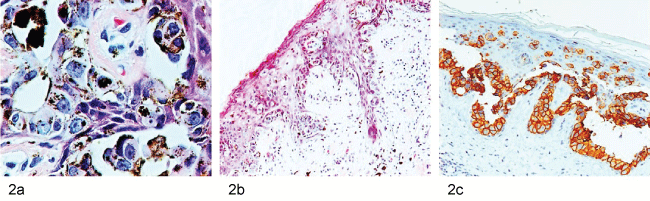
.
Figure 2: (a) Typical paget pigmented cells with melanin-like pigment; (b) Pigmented cells in the suprabasal and the presence of carcinoma in the underlying dermis; (c) Positive staining for Her-2.
View Figure 2
Microscopically, cells with abundant eosinophilic cytoplasm and large nuclei are observed. Such cells will be found grouped in "nests" at the epidermis; infiltration may be attached to the skin. This is a subtle histological difference with pigmented lesions; some authors have described that melanocytes in melanoma spread through all levels of the epidermis while in pigmented Paget disease, isolated cells or nests are seen in the suprabasal layers without the junctional component and an invasive or intraductal mammary carcinoma is often discovered in the underlying dermis (Figure 2b) [13,14].
The diagnosis might be made by immunohistochemistry, as it will be necessary to make the appropriate treatment. An important immunohistochemical marker for confirming the breast origin is the cytokeratin 7 (CK-7). It is expected to be positive in all patients. This cytokeratin is expressed in epithelial cells of ovary, lung and breast [15]. Anothercomplimentary immunohistochemistry test that should be done in the pigmented cells is Her-2 staining; 80 to 100% of the cells will express strongly this marker, since Paget disease is commonly associated with High-grade Ductal Carcinoma In Situ. The positivity of these two indicators will guide to a mammary origin.
Besides these markers, in order to rule out squamous cell carcinoma or melanoma, it is essential to perform P63 and S-100 respectively, which should be negative in pigmented mammary Paget disease [16].
Currently, there is controversy about the relevance of the expression of Her-2 in carcinomas in situ. Provenzano and Han established that its over-expression was related to a higher incidence of ipsilateral DCIS recurrence, Noh and colleagues in May 2013 stated that although there is no increase in recurrence, it does occur earlier [11,17,18].
As it has been established, treatment should be determined by clinical stage given by the invasive component, if exists. Pigmented variety should be treated as any other mammary Paget disease. Prognosis is not affected by this entity.
Conclusions
Paget's disease represents 1 to 3% of all breast cancers. The pigmented variant is a rare entity, which can mimic cutaneous melanoma; both clinically and histologically with immunohistochemical profile an essential tool to differentiate between these diseases. The positivity to CK-7 and Her-2 in the pigmented cells will lead to confirm pigmented Paget disease. At our institution, incidence of this unusual variation accounts for 8.7% of breast Paget; treatment should be the same as in any other mammary Paget disease of the breast, since prognosis is not affected by this kind of presentation.
References
-
Ji Hye Lee, Tae Hyung Kim, Soo-Chan Kim, You Chan Kim, Mi Ryung Roh (2014) Pigmented Mammary Paget Disease Misdiagnosed as Malignant Melanoma. Ann Dermatol 26: 747-750.
-
David J Dabbs (2012) Breast Pathology. Elsevier - Health Sciences Division, Saunders, Philadelphia, United States of America.
-
Bland C (2009) The Breast. Saunders, United States of America.
-
Edge SB, Byrd DR, Compton CC, Fritz AG, Greene FL, et al. (2010) AJCC Cancer Staging Manual. (7th ed) Springer, New York, USA, 347-376.
-
Carlson RW (2003) NCCN breast cancer clinical practice guidelines in oncology: an update. J Natl Compr Canc Netw 1: S61-S63.
-
Hammond ME, Hayes DF, Dowsett M, Alfred DC, Hagerty KL, et al. (2010) American Society of Clinical Oncology/College of American Pathologists guideline recommendations for immunohistochemical testing of estrogen and progesterone receptors in breast cancer. J Clin Oncol 28: 2784-2795.
-
Wolff AC, Hammond ME, Schwartz JN, Hagerty KL, Allred DC, et al. (2007) American Society of Clinical Oncology/College of American Pathologists guideline recommendations for human epidermal growth factor receptor 2 testing in breast cancer. J Clin Oncol 25: 118-145.
-
Goldhirsch A, Winer EP, Coates AS, Gelber RD, Piccart-Gebhart M, et al. (2013) Personalizing the treatment of women with early breast cancer: highlights of the St Gallen International Expert Consensus on the Primary Therapy of Early Breast Cancer. Ann Oncol 24: 2206-2223.
-
Vani B, Thejaswini M, Srinivasamurthy V, Rao MS (2013) Pigmented Paget's disease of nipple: A diagnostic challenge on cytology. J Cytol 30: 68-70.
-
Dixon AR, Galea MH, Ellis IO, Elston CW, Blamey RW (1991) Paget's disease of the nipple 78: 722‑723.
-
Provenzano E, Hopper JL, Giles GG, Marr G, Venter DJ, et al. (2004) Histological markers that predict clinical recurrence in ductal carcinoma in situ of the breast: an Australian population-based study, 36: 221-229.
-
Gabbi TV, Valente NY, Castro LG (2006) Pigmented Paget disease of the nipple mimicking cutaneous melanoma: importance of the immunohistochemical profile to differentiate between these diseases. An Bras Dermatol 81: 457-460.
-
Requena L, Sangueza M, Sangueza OP, Kutzner H (2002) Pigmented mammary Paget disease and pigmented epidermotropic metastases from breast carcinoma. Am J Dermatopathol 24: 189-198.
-
Petersson F, Ivan D, Kazakov DV, Michal M, Prieto VG (2009) Pigmented Paget disease--a diagnostic pitfall mimicking melanoma . Am J Dermatopathol 31: 223-226.
-
S Kummar, M Fogarasi, A Canova, A Mota, T Ciesielski (2002). Cytokeratin 7 and 20 staining for the diagnosis of lung and colorectal adenocarcinoma. Br J Cancer 86: 1884-1887.
-
Fuertes L, Santonja C, Kutzner H, Requena L (2013) Immunohistochemistry in dermatopathology: a review of the most commonly used antibodies (part I). ActasDermosifiliogr 104: 99-127.
-
Han K, Nofech-Mozes S, Narod S, Hanna W, Vesprini D, et al. (2012) Expression of HER2neu in ductal carcinoma in situ is associated with local recurrence . ClinOncol (R CollRadiol) 24: 183-189.
-
Noh JM , Lee J, Choi DH, Cho EY, Huh SJ, et al. (2013) HER-2 overexpression is not associated with increased ipsilateral breast tumor recurrence in DCIS treated with breast-conserving surgery followed by radiotherapy. Breast 22: 894-897.