International Journal of Cancer and Clinical Research
The Many Faces of Lung Cancer
Luciano Cardinale*, Valeria Angelino, Edoardo Piacibello* and Andrea Veltri
Department of Radiology, AOU San Luigi Gonzaga Hospital, Orbassano, Torino, Italy
*Corresponding authors:
Luciano Cardinale, Department of Radiology, AOU San Luigi Gonzaga, Regione Gonzole 10, 10043 Orbassano, Torino, Italy, Tel: +39011902601, Fax: +390119026303, E-mail: luciano.cardinale@gmail.com
Edoardo Piacibello, Department of Radiology, AOU San Luigi Gonzaga, Regione Gonzole 10, 10043 Orbassano, Torino,
Italy, Tel: +393333709855, E-mail: edopiaci@gmail.com, edoardo.piacibello@hotmail.it
Int J Cancer Clin Res, IJCCR-3-050, (Volume 3, Issue 2), Short Review; ISSN: 2378-3419
Received: February 23, 2016 | Accepted: March 25, 2016 | Published: March 27, 2016
Citation: Cardinale L, Angelino V, Piacibello E, Veltri A (2016) The Many Faces of Lung Cancer. Int J Cancer Clin Res 3:050. 10.23937/2378-3419/3/2/1050
Copyright: © 2016 Cardinale L, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The aim of this short review is to illustrate various CT findings of lung cancer (LC) other than the classical aspects. Overall, LC is the second commonest cancer in men and women in the developed world and small cell lung cancer (SCLC) accounts for about 20-25% of cases. In comparison with Non-Small Cell Lung Cancer (NSCLC), SCLC typically exhibits more aggressive behaviour with rapid growth, early metastatic spread and frequent association with paraneoplastic syndromes. LC can have a wide spectrum of morphologies, some of which are not commonly known. The article will describe in a pictorial essay format the variability of presentation.
We will discuss:
-Typical presentation
-Cystic airspace presentation
-Pneumonia like presentation
-Pleural neoplasms like presentation
-Lymphoma like presentation
-Sarcoidosis like presentation
-TBC like presentation
In conclusion, radiologists must be aware of these different forms of presentation prompting for its rapid recognition and differential diagnosis.
Keywords
Computed Tomography, Lung Cancer, Pleural Disease, Lymphoma, Sarcoidosis, Tuberculosis
Introduction
Lung cancer is the most important cancer killer in Europe, accounting for approximately 20% of total cancer deaths. In Europe, the overall 5-year survival is respectively 11.2% for men and 13.9% for women [1]. The differential diagnosis between lung cancer and some other conditions is sometimes a challenge as lung cancer may demonstrate heterogeneous aspects. Differential diagnosis can be particularly challenging when lung cancer exhibit cystic airspace presentation, pneumonia like presentation, pleural neoplasms like presentation, lymphoma like presentation or a tuberculosis like presentation.
Typical Appearance
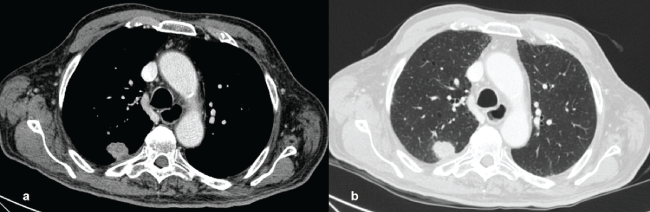
Lung cancer can be peripheral, arising beyond the segmental bronchi or central, arising in a large bronchus close to the hilum. Except Pancoast's tumours or superior sulcus tumours that may resemble an apical pleural thickening, the majority of peripheral lung cancers are approximately spherical or oval in shape (Figure 1).
.
Figure 1: Adenocarcinoma. Axial contrast-enhanced CT (mediastinal window, a, lung window, b). Peripheral tumor of the right upper lobe, with an irregular contour, undissociated from the chest wall pleura.
View Figure 1
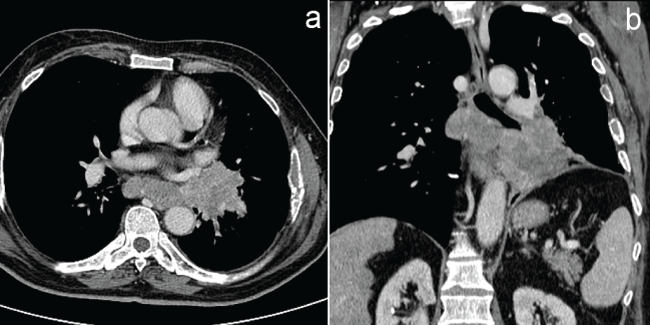
Lobulation is an aspect that indicates uneven growth rates in different parts of the neoplasm and it is common. The "corona radiata" sign is a common finding that may be referred to neoplastic infiltration, oedema of the surrounding tissues and obliteration of the small vessels and bronchioles. Adenocarcinoma often shows hilar and mediastinal adenopathy, though the nodal enlargement is not as massive as it is with SCLC (small cell lung cancer) (Figure 2).
.
Figure 2: SCLC. Contrast-enhanced chest CT scan (a, axial view with mediastinal window; b, reformatted coronal reconstruction). Left hilar mass with sub-carinal confluent lymphadenopathies. Diagnosis was established from trans-bronchial biopsy.
View Figure 2
Squamous cell carcinoma is the most likely cell type to show cavitation. At the end, calcifications, air bronchograms, pleural tags, bubble-like lucencies or pseudocavitation may be seen not rarely within peripheral lung cancers [2].
The fundamental imaging signs of a central tumour are collapse/consolidation of the lung beyond the tumour and the presence of hilar enlargement, all signs that may be seen alone or associated. Collapse/consolidation of the lung is due to obstruction of a major bronchus that often brings to a combination of atelectasis and retention of secretions with a consequent pulmonary opacity.
Cystic like presentation
Lung cancer arising from the wall of a pre-existing pulmonary cystic airspace has been reported, but this presentation has been described as uncommon. It is still unclear whether these cystic spaces were congenital cysts or appeared later in life and whether the cyst antedated the development of the lung cancer [3].
The definition of cystic airspaces was standardized by the Fleischner Society in 1996 and updated in 2009, including size criteria, pathologic findings and the presence of emphysema [4].
Cysts appear as round parenchymal lucency with a well-defined interface with normal lung. Cysts have variable wall thickness but are usually thin-walled (< 2 mm) and occur without associated pulmonary emphysema, while cavities are gas-filled spaces, seen as lucency or low-attenuation areas, within pulmonary consolidation, a mass, or a nodule.
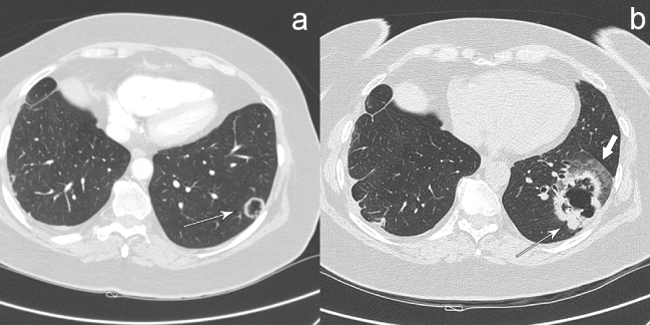
As reported by Farooqi et al. radiologists interpreting chest CT scans of patients at risk of lung cancer should pay careful attention to the walls of cystic airspaces because progressive wall thickening over time may represent a neoplastic evolution [3] (Figure 3).
.
Figure 3: SCLC. Axial contrast-enhanced chest CT scan, lung window, performed in 2009 (a) and non-enhanced CT scan, lung window performed in 2012; (b). Pulmonary cyst (arrow in a) with slightly diffuse thickened walls in the left lower lobe. Enlargement of the lesion and walls thickening (thin arrow in b) with peripheral ground- glass consolidation of adjacent parenchyma (thick arrow in b). Diagnosis was obtained with CT-guided percutaneous biopsy and confirmed after surgery (lower left lobectomy).
View Figure 3
Pneumonia-like presentation
Invasive mucinous adenocarcinoma (ex mucinous BAC or bronchioloalveolar carcinoma), based on new IASLC/ATS/ERS classification [5] is a subtype of adenocarcinoma of the lung that frequently consists of consolidative opacities with air bronchograms.
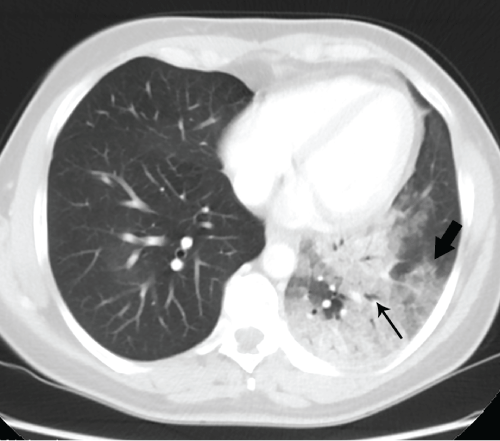
Invasive mucinous adenocarcinoma’s imaging consists of the following three patterns: a solitary nodule or mass, a localized area of parenchymal consolidation, or multicentric or diffuse disease [6]. On CT scan the presence of stretching, sweeping and widening of branching air-filled bronchi within an area of consolidation, pseudocavitation and crazy paving, favour the diagnosis of cancer instead of pneumonia [7]. When the tumor exhibit a localized area of parenchymal consolidation often the correct diagnoses is posticipated (Figure 4).
.
Figure 4: Adenocarcinoma in situ. Axial contrast-enhanced chest CT scan with lung window. Consolidative area of the left lower lobe with air bronchogram (thin arrow) and with peripheral ground-glass opacity (thick arrow), mimicking infectious pneumonia.
View Figure 4
Pleural neoplasms-like presentation
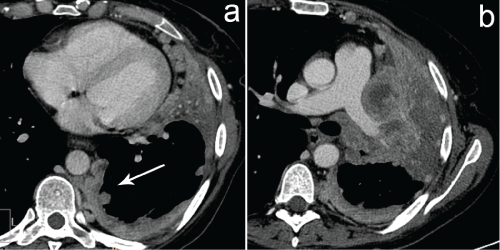
Lung cancer is the most common cause of malignant pleural effusion. Any histologic type of lung cancer can involve the pleura, but adenocarcinoma is the most common type due to its frequent peripheral location [8]. In some cases, lung cancer may predominate as diffuse pleural disease pattern (pleural effusion, diffuse pleural thickened and pleural nodules), hardly differentiating from pleural metastasis or malignant pleural mesothelioma (Figure 5).
.
Figure 5: NSCLC. Axial contrast- enhanced chest CT mediastinal window (a,b). Unilateral pleural effusion in the left hemithorax with irregular pleural thickening; (a) mimicking a malignant pleural mesothelioma. Note the presence of hilar mass originating from left upper lobe inseparable from the pleural thickening; (b). Diagnosis was confirmed by transthoracic CT-Guided biopsy.
View Figure 5
Lymphoma-like presentation
Lung cancer is the most common primary neoplasm involving mediastinal lymph nodes [9]. In some patients with lung cancer, a mediastinal mass or diffuse mediastinal lymphadenopathies may be the only presenting abnormality, occurring in the absence of a visible lung mass. Isolated mediastinal mass are usually associated with small cell carcinoma (SCC) or poorly differentiated carcinoma [10].
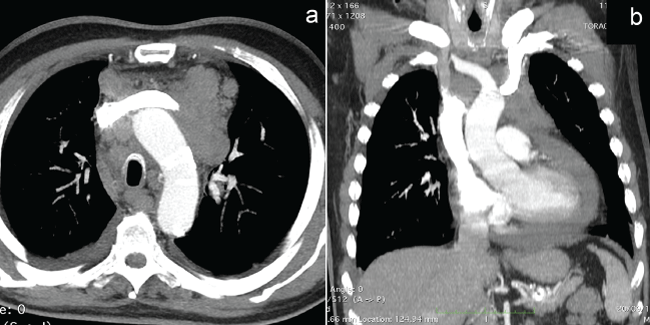
SCC usually grow rapidly and metastasize to mediastinal lymph nodes relatively early in the course of the disease. Differentiating central lung tumours from a real mediastinal tumor can be sometimes problematic (Figure 6). The most useful CT finding in distinguishing between central lung tumours and mediastinal masses is the "mass-lung interface". Marginal spiculation, nodular or irregular edge between the mass and the surrounding lung usually indicate that the mass has arisen from the lung, on the contrary a smooth interface suggests a mediastinal origin [10].
.
Figure 6: SCLC. Contrast-enhanced chest CT scan (a, axial view with mediastinal window; b, reformatted coronal reconstruction). Multiple, confluent lymphadenopathies invading the mediastinum. No parenchymal lesions were present. Diagnosis was obtained with trans-bronchial biopsy.
View Figure 6
A notable exception was Hodgkin's lymphoma which may occasionally cross the pleura, invade the lung and result in a poorly marginated mass, mimicking a lung cancer. In cases in which lung cancer presents with only diffuse mediastinal lymphadenopathies is impossible the differential diagnosis with sarcoidosis and lymphoma.
Sarcoidosis-like presentation
Rarely lung cancer appears with micronodular dissemination without ancillary signs suggesting the diagnosis, (a predominant and typical lung lesion for example). In patients with multinodular lung carcinoma, nodules usually range from 1 to 3 cm and nodular margins are both sharply and poorly defined. The nodules are often distributed in a centrilobular region and spare the pleural surfaces and the fissures with a random distribution [11].
Metastatic nodules from extra-thoracic origin, tend to be smooth, well-defined lesions, with basilar predominance due to preferential blood flow to the lung bases. Individual nodules may have "feeding vessels" according to their hematogenous origin [12].
Tumor growth can at the same time occur also in the lymphatic system of the lungs (lymphangitic carcinomatosis), resulting from hematogenous spread to lung, with subsequent interstitial and lymphatic invasion, but can also occur because of direct lymphatic spread of tumor from mediastinal and hilar lymph nodes. The pulmonary lymphatics involved in patients who have lymphangitic carcinomatosis are located in the peribronchovascular and centrilobular interstitium and in the peripheral interstitial compartment (within the interlobular septa and in the subpleural regions), similar to sarcoidosis, coal- worker's pneumoconiosis or silicosis [13].
The most typical findings of pulmonary sarcoidosis involvement are micronodules with a perilymphatic distribution, small nodules along pleura, fibrotic changes, such as reticular opacities, traction bronchiectasis, bronchiolectasis, volume loss, and bilateral hilar lymph node enlargement [14]. In sarcoidosis, although septal nodules are commonly seen, septal thickening is usually less extensive than that seen in patients who have lymphangitic carcinomatosis [13]. Moreover, pulmonary nodules and masses are seen in 15%-25% of patients with sarcoidosis [14]. At CT, they usually appear as irregular opacities measuring 1-4 cm in diameter that represent interstitial granulomas.
These lesions are typically multiple and bilateral and have to be differentiated from multinodular carcinoma [14]. The clinical context is fundamental, eventually with a biopsy approach, but also is mandatory performing the CT scan using a dedicated thin slice reconstruction algorithm.
Tuberculosis (TB)-like presentation
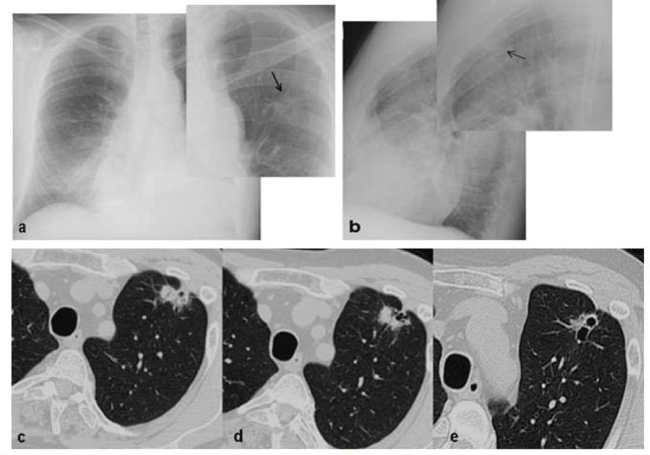
Patients with lung cancer are sometimes misdiagnosed as pulmonary TB leading to delay the correct diagnosis. There are many similarities between these diseases, they both are common with high prevalence, they involve the lung parenchyma and above all, they are characterized by similar symptoms. Due to high TB prevalence and clinico-radiological similarities, a large number of lung cancer patients initially get wrongly treated for tuberculosis based on radiological image alone [15]. Mass with or without collapse is the commonest radiological finding in lung cancer [16]. Furthermore it was postulated that a proportion of lung cancers arise at the edge of pre-existing scars, and that parenchymal scarring can stimulate atypical epithelial cell proliferation and metaplasia involving the terminal air-space [16]. In the genesis of scar carcinoma play an important role infections such as TB that cause chronic inflammation and implies that there is a preexisting scar in which a carcinoma developed [17]. In some cases, CT scan does not clearly distinguish lung cancer from a pulmonary TB. The cavitation, typical of TB, is not a reliable criteria and the same for the speculate margins, frequently seen in both diseases (Figure 7).
.
Figure 7: Adenocarcinoma surrounded by scar tissue. Postero-anterior and lateral chest X-ray (a,b) shows multiform subtle heterogeneous opacity in the left upper zone (arrow). CT scans (c,d,e) obtained two months later, shows irregular solitary nodule in the upper segment of right upper lobe with bronchogram and pseudo-cavitation associated with a fibrotic scar tissue.
View Figure 7
Moreover, numerous inflammatory and infectious processes, such as tuberculosis or fungal infections, may uptake fluorodeoxyglucose (FDG) in PET studies and mimic a malignancy. Patients with post-TB infections presenting pulmonary lesions, require more attention; the comparison with previous radiographies is mandatory and, in case of doubt, a CT scan with dedicated thin slice reconstruction allow to select the patients in which the diagnosis of lung cancer is based on the findings of biopsy [17,18].
Conclusion
In conclusion, radiologists must be aware of these different forms of presentation drawing for their rapid recognition and differential diagnosis. Lung cancer produces radiological findings that can sometimes mimic a wide variety of pulmonary conditions. In these cases, when the clinico-radiological examination and the multidisciplinary study is not sufficient, the correct diagnosis can be made certainly only by biopsy.
References
-
Lung White Book, published by the ERS (chapter 19): 225-226.
-
Lederlin M, Revel M, Khalil A ,G Ferrettid, B Milleron, et al. (2013) Management strategy of pulmonary nodule in 2013. Diagnostic and Interventional imaging 94: 1081–1094.
-
Farooqi AO, Cham M, Zhang L, Beasley MB, Austin JH, et al. (2012) Lung Cancer associated with cystic airspaces. AJR Am J Roentgenol 199: 781-786.
-
David M Hansell, Alexander A Bankier, Heber MacMahon, Theresa C McLoud, Nestor L Müller (2008) Fleischner Society: glossary of terms for thoracic imaging. Radiology 246: 697-722.
-
William D. Travis, Elisabeth Brambilla, Masayuki Noguchi, Andrew G Nicholson, Kim R Geisinger, et al. (2011) State of the Art: Concise Review.International Association for the Study of Lung Cancer/American Thoracic Society/European Respiratory Society International Multidisciplinary Classification of Lung Adenocarcinoma. Journal of Thoracic Oncology 6: 244-285.
-
Kim TH, Kim SJ, Ryu YH, Chung SY, Seo JS, et al. (2006) Differential CT features of infectious pneumonia versus bronchioloalveolar carcinoma (BAC) mimicking pneumonia. Eur Radiol 16: 1763-1768.
-
Piacibello E, Angelino V, Moretti F, Busso M, Cardinale L, et al. (2015) Lung Cancer: one issue, many faces. EPOS: DOI 10.1594/ecr2015/C-2202.
-
Jeong YJ, Kim S, Kwak SW, Lee NK, Lee JW, et al. (2008) Neoplastic and Non-neoplastic Conditions of Serosal Membrane Origin: CT Findings.RadioGraphics 28: 801-818.
-
Woodring JH, Johnson PJ (1991) Computed tomography distinction of central thoracic masses. J Thorac Imaging 6: 32-39.
-
Hollings N, Shaw P (2002) Diagnostic imaging of lung cancer. Eur Respir J 19: 722-742.
-
Akira M, Atagi S, Kawahara M, Iuchi K, Johkoh T (1999) High-Resolution CT finding of diffuse Bronchioalveolar carcinoma in 38 Patients. AJR Am J Roentgenol 173: 1623-1629.
-
Raoof S, Amchentsev A, Vlahos I, Goud A, Naidich DP (2006) Pictorial Essay: Multinodular Disease: A High-Resolution CT Scan Diagnostic Algorithm. Chest 129: 805-815.
-
W Richard Webb, Nestor L Muller, David P Naidich (2009) High-Resolution CT of the Lung, 4th edition,Diffuse Pulmonary Neoplasms and Pulmonary Lymphoproliferative Diseases. P241-272.
-
Criado E, Sánchez M, Ramírez J, Arguis P, de Caralt TM, et al. (2010) Pulmonary Sarcoidosis: Typical and Atypical Manifestation at High- Resolution CT with pathologic Correlation. Radiographics 30: 1567-1586.
-
MLB Bhatt, Surya Kant, Ravi Bhaskar (2012) Pulmonary tuberculosis as differential diagnosis of lung cancer. South Asian J Cancer 1: 36-42.
-
KL Wig, EJ Lazaro, NG Gadekar, JS Guleria (1961) Bronchogenic carcinoma: Clinical features and diagnosis. Indian J Chest Dis 3:209-18.
-
Zhou Y, Cui Z, Zhou X, Chen C, Jiang S, et al. (2013) The presence of old pulmonary tuberculosis is an independent prognostic factor for squamous cell lung cancer survival. J Cardiothorac Surg 8: 123.
-
Kim YI, Goo JM, Kim HY, Song JW, Im JG (2001) Coexisting bronchogenic carcinoma and pulmonary tuberculosis in the same lobe: radiologic findings and clinical significance. Korean J Radiol 2: 138-144.





