International Journal of Critical Care and Emergency Medicine
Cerebral Fat Embolism Syndrome: Diagnostic State of the Art: with and without Intra-medullary Fixation, with and without Long Bone Fractures
Bethany Radin DO1, H Neal Reynolds1*, Uttam K Bodanapally2 and David Dreizin2
1R Adams Cowley Shock Trauma Center, University of Maryland Medical Center, USA
2Department of Diagnostic Radiology, University of Maryland Medical Center, USA
*Corresponding author:
H. Neal Reynolds, R Adams Cowley Shock Trauma Center, University of Maryland Medical Center, UMMC, 22 South Greene Street, Baltimore, Maryland, 21201, USA, Tel: 410-328-1201, E-mail: HNeal.Reynolds@gmail.com
Int J Crit Care Emerg Med, IJCCEM-1-004, (Volume 1, Issue 1), Research Article; ISSN: 2474-3674
Received: July 31, 2015 | Accepted: August 28, 2015 | Published: August 31, 2015
Citation: Bethany RDO, Reynolds HN, Bodanapally UK, Dreizin D (2015) Cerebral Fat Embolism Syndrome: Diagnostic State of the Art: with and without Intra-medullary Fixation, with and without Long Bone Fractures. Int J Crit Care Emerg Med 1:004. 10.23937/2474-3674/1510004
Copyright: © 2015 Bethany RDO. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective: To review the spectrum of scenarios in which cerebral fat embolism syndrome (CFES) may present, the clinical presentation, traditional diagnostic criteria, and current diagnostic technologies.
Methods: Three cases are presented representing Classical presentation (CFES presenting after Intramedullary rods for long bone fractures), Atypical presentation (CFES presenting after long bone fractures without intramedullary rods), and Unexpected presentation (CFES without any long bone fractures). All diagnoses were confirmed with MRI studies. Literature was reviewed on the spectrum of presentations, classical diagnostic criteria, clinical presentations, and use of MRI to confirm diagnosis.
Results: CFES may present after a wide spectrum of insults beyond the typical repaired long bone fracture. Additionally, CFES has been suspected after elective joint replacements. The classical Gurd criteria and Schoenfeld Fat Embolism Index are very non-specific and include some criteria or diagnostic studies not routinely available. Finally, none of the traditional criteria distinguish between CFES and diffuse axonal injury (DAI) which would represent the two primary differential diagnostic considerations for altered mental status after trauma when the head CT is negative.
Conclusions: The occurrence of CFES may be more prevalent than previously thought and can be confirmed by combining clinical criteria and course of the mental status changes with abnormalities on the MRI-all of which are distinguishable from DAI.
Introduction
In the majority of patients who present with altered mental status after major trauma, direct traumatic brain injury is the presumed insult. When the routine head computerized tomogram (CT) is negative with an altered mental status, diffuse axonal injury (DAI) is the presumed lesion. The clinical and historical time-line of patients with severe traumatic brain injury (TBI) and DAI includes immediate altered mental status following the trauma. By contrast, patients with altered mental status due to CFES will develop delayed onset of altered mental status after an initial period of clear sensorium. As an introduction to the topic of CFES, three cases are presented: one with very typical history, one somewhat atypical, and another completely unexpected. When combining clinical presentation and the characteristic changes on MRI, a diagnosis of cerebral fat embolism syndrome (CFES) can be confidently made. Otherwise, such patients may present with many of the same neurologic signs and symptoms as diffuse axonal injury (DAI). The distinction is important, despite lack of therapy for either CFES vs DAI, since the prognosis may be dramatically different.
Classical Cerebral Fat Embolism
Presenting after placement of intra-medullary rods (ORIF) for long bone fractures
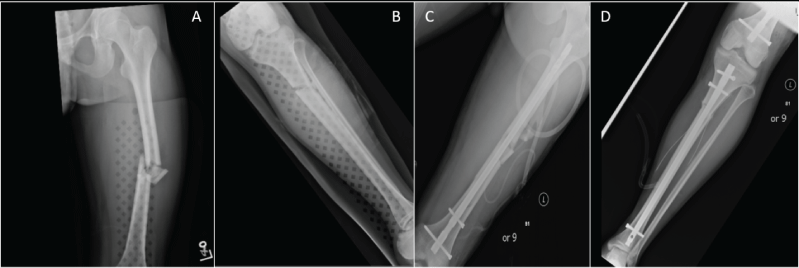
19 year old male was admitted to a tertiary trauma center after a motor vehicle accident. The mechanism involved a head-on impact by the patient's vehicle into a dump truck. After full trauma screen, the injuries discovered were limited to a mid-shaft left femur and upper third left tibial fractures. The head CT was negative (Figure 1).
.
Figure 1: Initial fractures of the left femur and left tibia are shown in (A) and (B). Post- operative films with intra-medullary rods transfixing both fractures are shown in (C) and (D).
View Figure 1
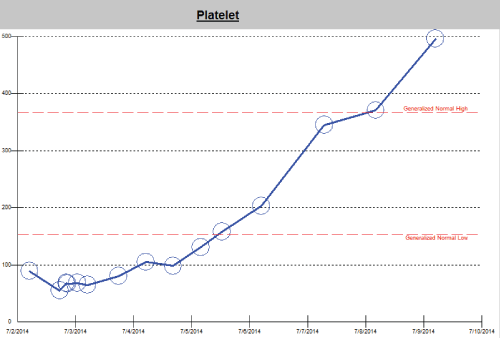
At time of admission the patient was fully oriented, conversant, breathing spontaneously with normal laboratory values except first measured platelet count of 80 K. He was taken quickly to the operating room for placement of intra-medullary rods in the left femur and left tibia. Post operatively he was agitated, disoriented, hemodynamically unstable, tachycardic and ventilator dependent. CT of the chest was negative for bland pulmonary emboli but revealed scattered patchy parenchymal infiltrates. Platelet count reached a nadir of 67 K then rebounded rapidly as shown in figure 2.
.
Figure 2: Platelet count trend from admission to discharge, patient 1 with long bone fractures and ORIF.
View Figure 2
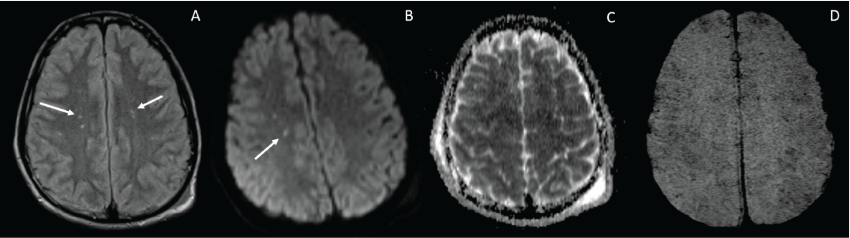
He required ventilator support for three days then was weaned rapidly to extubation. Due to a delayed return to normal sensorium, an MRI was performed which revealed abnormalities on fluid-attenuated inversion recovery (FLAIR), diffusion-weighted imaging (DWI), attenuation diffusion coefficient map (ADC), and susceptibility weighted imaging (SWI), as described in the caption for figure 3.
.
Figure 3: Scattered foci of hyperintensity are seen primarily within the deep white matter at the level of the centrum semiovale on the FLAIR image (Image A, arrows). While similar findings on FLAIR can be seen in older patients secondary to chronic white matter disease, the finding is unusual in this age group. There is corresponding high signal on DWI (Image B arrows), without associated high signal on the ADC map (Image C), consistent with foci of cytotoxicity secondary to microinfarcts rather than T2-shine through from vasogenic edema. The SWI image (image D) shows innumerable extensive fine foci of low signal intensity with a diffuse distribution.
View Figure 3
Sensorium improved although with mild persistent cognitive deficits till time of discharge. He was subsequently discharged to a rehabilitation institution. During the hospital course and retrospectively, this case was felt to be completely consistent with classical CFES. For the non-radiologists, there is an appendix at the end briefly describing physiology and pathological findings associated with each of the different MRI imaging techniques.
Atypical Cerebral Fat Emolism Syndrome
Presenting after long bone fractures without intramedullary rods (ORIF))
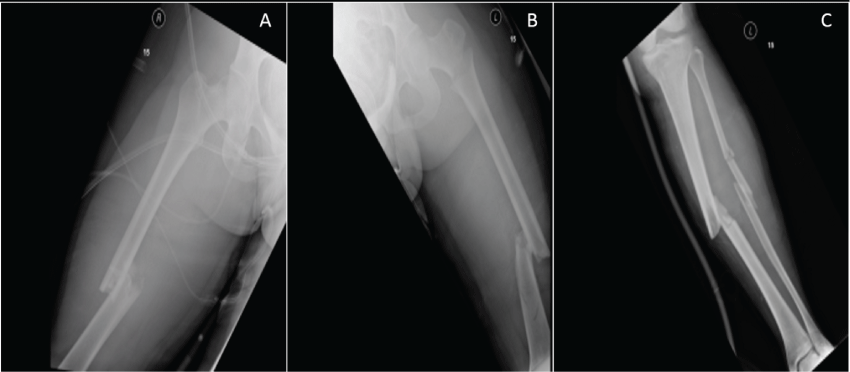
28 year old female driving a motor vehicle, opposite to the normal flow of traffic on a major city circumferential highway and at extremely high rate of speed, collided head on with an 18 wheel tractor-trailer. Sustained injuries included atlanto-occipital dissociation (AOD), severe laceration/maceration of the right lobe of the liver, bilateral femur fractures (right femur mid shaft, left femur mid shaft and subtrochanteric), left tibia and fibula, left ulnar fracture (Figure 4).
.
Figure 4: Initial injuries in patient #2 with right mid-shaft femur (Image A), leftmid-shaft femur and sub-trochanteric fracture (image B), and left tibial mid shaft fracture (image C).
View Figure 4
At time of admission, her Glasgow coma scale was described at 14 of a possible 15 maximum, despite a blood alcohol level of 175 mg/dl. Due to the overall hemodynamic instability, all long bone fractures were initially stabilized only with external fixation or splints. On day two, she was noted to have significant neurological deterioration to GCS of 3T (intubated). Non-Contrast enhanced CT of the brain was normal. An unenhanced MRI of the brain revealed the following figure 5.
.
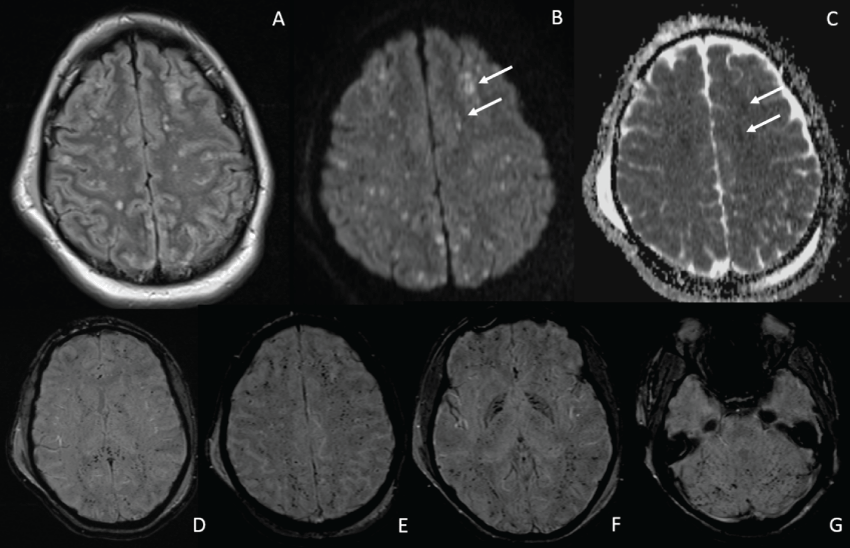
Figure 5: High signal intensity foci of varying sizes are seen on FLAIR scattered throughout the convexities, and involving both superficial and deep white matter as well as cortex (image A). Many of these lesions have restricted diffusion and are cytotoxic rather than vasogenic, resulting in high signal on DWI (image B), and low signal on ADC (image C- arrows point to the same lesions on DWI and ADC map). The bottom four susceptibility weighted images (D-G), show low signal diffusely involving the corpus callosum (D), inter-digitate white matter and gray matter throughout the convexities (E), basal ganglia (F) and cerebellum (G). The relative lack of predilection for specific areas of the brain commonly involved in DAI (e.g. midline splenium of the corpus callosum, parahippocampal white matter, and dorsolateral brainstem or midbrain) and the extensive fine granular appearance of microhemorrhages on the SWI images is consistent with a radiologic diagnosis of CFES.
View Figure 5
Due to the profound reduction of the GCS, an intracranial pressure monitoring device was placed for about 3 days and revealed Intracranial Pressure (ICP) < 5 mm Hg during the time of ICP monitoring. Continuous EEG was performed for 48 hours and revealed no sharp wave or localizing epileptic/epileptiform activity. Over the subsequent 21 days, the patient gradually awoke to follow commands with all 4 extremities. No repeat MRI was performed. All long bone fractures were stabilized in a delayed fashion with no evident worsening of neurologic status. She was seen again about 12 months after discharge, fully and independently ambulatory with clear sensorium and had returned to college.
Unexpected Cerebral Fat Emboli
Presenting without long bone fractures or intramedullary fixation
A 20 year old female presented following a motor vehicle collision with transient loss of consciousness. She was a restrained passenger, sitting in the front passenger seat of a 4 door compact passenger vehicle. The vehicle was struck by a standard school bus moving at an estimated 35 MPH when the passenger vehicle failed to yield to a stop sign. Airbags were deployed as the car was struck from the right ("T-boned") as shown in figure 6.

.
Figure 6: View of passenger vehicle demonstrating at least 12 inches of side impact movement.
View Figure 6
Upon arrival at the trauma center, she was completely neurologically intact but emergently intubated for hypoxia. Triage CT screen showed the following injuries: right pneumothorax, right lung lacerations, multiple right rib fractures, a grade 3 liver laceration, right superior sacral fracture, and bilateral superior and inferior pubic rami fractures (Figure 7).
.
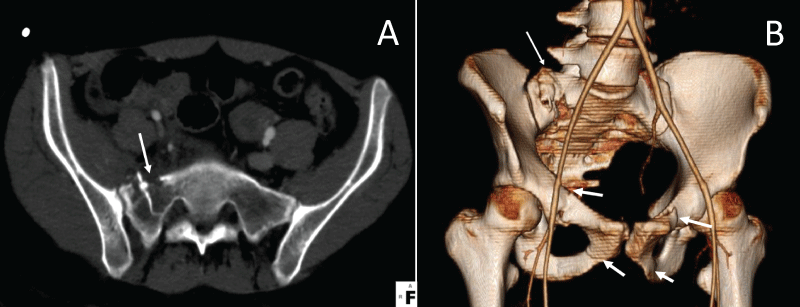
Figure 7: Right, non-displaced sacral fracture was the largest bony fracture discovered in patient 3 (Image A arrows). Mildly displaced anterior pubic ramus fractures are shown (Image B thick arrows) in addition to the sacral fracture (Image B single thin arrow) in the 3D image. The patient had no long bone fractures or ORIF procedures performed.
View Figure 7
Due to the extensive subcutaneous emphysema, bronchoscopy was performed which revealed a right endo-bronchial tear. There were no long bone fractures. Other pertinent negatives include a head CT which was structurally normal on admission.
She was taken to the OR for a right thoracotomy and primary repair of the bronchial tear. Surgery was well tolerated and the patient was quickly weaned from the ventilator and extubated. Subsequent to the surgery, her mental status did not return to baseline. Considering that there may have been a lateral head-strike onto the passenger window, an MRI study was obtained on day 7 to evaluate for suspected DAI. The MRI showed restricted diffusion, vasogenic edema, and diffuse punctate micro- hemorrhages most consistent with CFES (Figure 8).
.
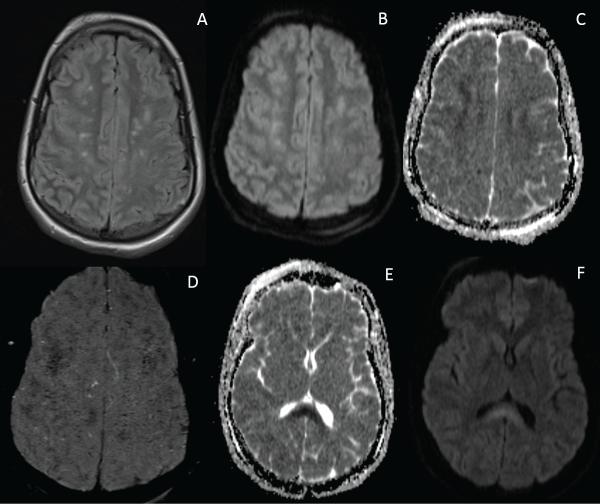
Figure 8: As in the prior two patients, scattered high signal foci are seen on FLAIR (A), with corresponding areas of restricted diffusion producing high signal on DWI (B) and low signal on ADC (C). SWI (D) shows similar findings of extensive diffuse fine granular hypointensities resulting from showering of fat emboli and free fatty acids with resultant vasculitic micro-hemorrhage. ADC map (E) and DWI (F) show cytotoxic edema also diffusely involving the splenium of the corpus callosum.
View Figure 8
Otherwise, during her hospital stay, she developed thrombocytopenia, mildly elevated liver function tests, and a fever. The remainder of the hospital course was consistent with emergence from brain injury. Cognitive evaluation was performed on hospital day # 9 revealing a Rancho-Los Amigos Scale (RLAS) [1] of IV/V consistent with her clinical confusion, inappropriate behavior, and agitation. She was subsequently transferred to a neuro rehabilitation center for 14 days and ultimately discharged home.
Discussion
CFES and DAI often may appear with similar neurologic signs and symptoms. However, those patients with DAI will have immediate and major neurologic deficits and are more likely to be recognized in the Emergency Department. By contrast, those with CFES will more likely be delayed in onset and will not be recognized in the ED and more likely recognized with time in the ICU. Fat Embolism Syndrome (FES) is defined as the presence of clinical symptoms arising from the showering of fat emboli [2]. The vast majority of cases of FES or CFES are related to long bone fractures with the highest incidence related to femur and tibial fractures [3]. A single long bone fracture has up to a 3% chance of FES, bilateral femur fractures is related to FES in up to 33% of patients with a mortality from FES alone reported at 5 - 20% [4]. Kimet et al. [5] reported FES after elective surgical hip arthroplasties and Sulek [6] reported FES after total knee replacement. On the other hand, Stein et al. collected data from 1979 to 2005 reporting the incidence of developing FES from an isolated pelvis fracture as "too small to calculate" [7]. When patients have showering of fat emboli, there is cerebral fat embolization in up to 86% of FES cases [7]. CFES is defined as a diffuse constellation of neurologic symptoms related to adipose embolization in the brain ranging from focal neurological deficits, mild confusional states, generalized encephalopathy or even, coma [8]. The full CFES is generally associated with concurrent respiratory failure [9] but may present only with neurologic deficits [10]. Severity can vary significantly from non-descript headache, altered mental status, focal deficits, visual and pupillary defects, seizures, and coma [4,9]. There is usually a delay in symptomatology of 24 - 72 hours from the original injury [11]. FES most commonly manifests with signs, symptoms and/or findings in the skin, lungs, and brain [11].
There are two proposed mechanisms of injury for FES: a mechanical theory and a biochemical theory [2,4,6,7]. The mechanical theory proposes that actual traumatic bony injury causes fat droplets to enter the venous system from injured bone. The adipose droplets are thought to either enter directly into capillary beds or can travel to the brain by pulmonary arterio-venous (AV) shunts [6]. Some of the fat emboli are small enough to traverse the capillaries obviating the A-V shunt mechanism such as a patent foramen ovale [7]. According to the mechanical theory, when fat droplets ultimately deposit in the cerebral capillary system causing local ischemia, inflammation, or hemorrhage. The biochemical theory suggests that inflammatory mediators cause the mobilization and release of stored fat into the bloodstream with some converted to inflammatory fatty acids [12,4]. Cerebral vasogenic edema induced by the free fatty acids is thought to be histo-toxic causing vasculitis, break-down of the blood brain barrier, loss of vascular integrity and localized petechial hemorrhaging [8]. Alternatively, the neurologic defect may be due to ischemic effect from small vessel occlusion by the fat globules [9]. In addition, there may be a surgical orthopedic mechanical element exacerbating or driving the development of FES. Specifically, with long bone fractures, medullary rods may be inserted into long bone marrow cavities that requiring medullary reaming prior to rod insertion. It is believed that this reaming effect may force marrow fat droplets into the venous circulation [12].
Gurd's Criteria shown in table 1 [13] and the Schoenfeld Fat Embolism Index shown in table 2 [14] can be used to guide the clinician in the diagnosis of FES.
![]()
Table 1: Gurd's Criteria: Gurd's Criteria defines FES as 1 major criteria, 4 minor criteria [15].
View Table 1
![]()
Table 2: Schonfeld's Fat Embolism Index 5 or more points on the Fat Embolism Index indicates FES [16].
View Table 2
Both the above Gurd's Criteria and Schonfelds index focus on the general FES and have relatively limited weight for the neurologic aspects of the FES. To achieve a higher level of confidence when considering the diagnosis of CFES, MR imaging can be highly supportive and perhaps diagnostic. Non-gadolinium enhanced MRI of the brain, ideally performed with SWI and DWI is considered the imaging test of choice to confirm the specific diagnosis of CFES [15-18]. Specific lesions may present as scattered or confluent areas of hyper-intensity on fluid-attenuated inversion recovery (FLAIR) imaging. T2/FLAIR hyperintensities resulting from cytotoxicity may correspond with foci of restricted diffusion (high signal on DWI and low signal on ADC maps (Figure 2, Figure 5 and Figure 8), whereas areas of vasogenic edema, which may have an identical appearance on FLAIR, will be bright on both DWI and ADC- a phenomenon known as T2-shine through. Susceptibility-weighted images (SWI) may reveal foci of low signal intensity corresponding with diffuse petechial hemorrhages due to microvascular rupture again caused by severe vasculitis from FFAs. These petechial hemorrhages tend to be very small and much greater in number than the lesions seen in DAI.
DAI lesions tend to involve areas of the brain that impact against hard surfaces such as the falx and tentorium (especially the medial aspect of the genu of the corpus callosum, the septum pellucidum, and the posterolateral brainstem); that splay out as a result of impulsive forces during whiplash (the peri-frontal horn and parahippocampal white matter); or that demarcate transitions between parts of the brain with different densities and water content that are susceptible to shear stress (subcortical white matter along the convexities). On the other hand, CFES has a more diffuse distribution throughout the white matter, basal ganglia, and cerebellar hemispheres, and like other embolic phenomena, has a predilection for watershed areas. Unlike DAI, which typically spares the digitate white matter (just below the gyri) and the cortex, CFES involves both of these areas.
In CFES, hyper-intense lesions on FLAIR images are thought to be due to breakdown of the blood-brain barrier induced by severe vasculitis from free fatty acids (FFAs), resulting in vasogenic edema. Hyper-intense lesions on DWI that correspond with cytotoxic edema (i.e. those associated with low ADC values) are attributed to microvascular occlusion by fat droplets resulting in ischemic lesions. Diffusion tensor imaging measures fractional anisotropy. Water normally preferentially diffuses along axons, but when nerves become bloated as a result of histo-toxicity there is more radial diffusivity (RD). Greater proportions of radial diffusivity are associated with lower fractional anisotropy (FA), indicating nerve dysfunction is present. CFES is associated with higher radial diffusivity and therefore lower FA values than DAI.
Differences in pattern and distribution of lesions between CFES and DAI are striking. A recent study has shown that qualitative evaluation of FLAIR, DWI, ADC and SWI images leads to the same diagnostic performance as when DTI parameters are used [20]. Table 3 highlights the similarities and differences between CFES and DAI MRI characteristics, and figure 9 shows a case of severe DAI for comparison.
.
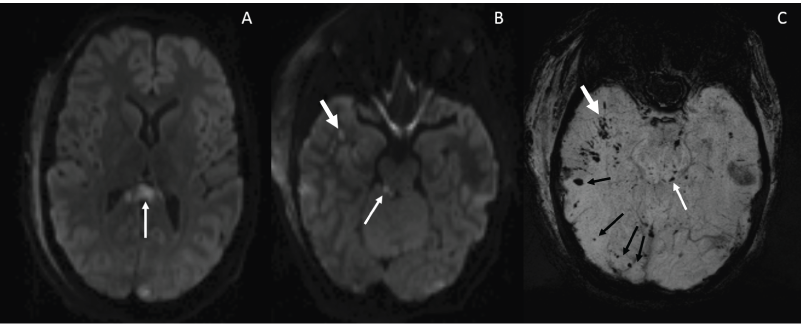
Figure 9: 21 year old woman following MVC with severe traumatic brain injury, and characteristic grade 3 diffuse axonal injury pattern on MRI, including foci of restricted diffusion on DWI in the midline splenium of the corpus callosum (Image A), right parahippocampal region (Image B thick arrow) and dorsolateral midbrain (Image B thin arrow) and coarse microhemorrhages in the right parahippocampal region (Image C thick white arrow), left dorsolateral midbrain (Image C thin white arrow), and predilection for the gray white matter junctions of the convexities (Image C black arrows) not extending into the digitate white matter.
View Figure 9
![]()
Table 3: MRI characteristics to distinguish CFES for DAI.
View Table 3
In the future, FA values may provide a more objective measure for assessing correlation with outcome in larger studies.
In the first case, classical cerebral fat embolism, was associated initially with clear sensorium, which then deteriorated after ORIF of two long bones, leading us to immediately consider the diagnosis of CFES. The MRI was supportive of the diagnosis of CFES, and the clinical and biochemical courses a well as rapid return to near normal neurologic function were all features consistent with CFES. Therefore, this was considered a "CLASSICAL CFES". In the second case labeled "Atypical Cerebral Fat Embolism Syndrome" the MRI was initially ordered to look for torsion/stretch injury to the brain stem related to the Atlanto-Occipital Dissociation. The brain stem was found to be normal; however, the typical MRI characteristics of CFES were unexpectedly discovered. Retrospectively the diagnosis of CFES was highly plausible in light of the major and multiple long bone injuries despite there having been no surgical intervention.
In case 3 (Unexpected Cerebral Fat Emboli), in which there were no long bone fractures, CFES was not considered when it was discovered that the patient had a cognitive deficit. Consequently, studies that may have supported the diagnosis such as bubble echocardiogram, urine or sputum analysis for fat globules, ESR, etc. were not performed. Either way, without the MRI, she still satisfied Schonfelds Fat Embolism Index (4 points bilateral alveolar infiltrates, 3 points hypoxia, and 1 point each for confusion, tachycardia and tachypnea: total 11 points). By comparison, the imaging abnormalities seen on the MRI of the "Classical CFES Patient with long bone fractures" were identical to the case presented here without long bone fractures and the clinical course of initial clear sensorium was also consistent.
The mainstay of treatment is primarily supportive and symptomatic treatment, as there are no proven pharmacologic therapies [5]. Patients that develop FES have a wide range of recoverability. Early fracture immobilization and repair are thought to decrease the risk of developing FES [5]. By contrast, it is presumed that more manipulation of a fractured extremity would enhance the chances of fat embolization. Most extremities will have immobilization placed by Emergency Medical Services but subsequent manipulation in the ED should be minimized where possible.
Making the distinction between DAI and CFES likely has significant prognostic value. Using MRI, the severity of DAI can be graded and time to recovery predicted. Mild DAI (grade I) involves only peripheral gray-white matter junctions; moderate DAI (grade II) involves the corpus callosum (usually the splenium and posterior body); and severe DAI (grade III) involves the dorsolateral midbrain or brainstem. With Grade I DAI, one can expect recovery in one week, with Grade II, recovery in 2 weeks, but with Grade III recovery may not occur or could be delayed 2 months or more [19]. With CFES, while there may be episodes of prolonged recovery [20], generally recovery occurs in days [21]. Of our three cases presented, the Atypical CFES patient devolved to a Glasgow Coma Scale of 3(T) yet demonstrated a full neurologic recovery over a period of approximately 30 days. A cognitive evaluation may be appropriate for patients with CFES.
Finally, regarding the third case, Unexpected Cerebral Fat Emboli Syndrome, the etiology remains unclear. There are a variety of traumatic and non-traumatic etiologies suggested by others [22-24]. Traumatic etiologies, in addition to those presented, include severe burn, and a variety of iatrogenic causes including bone marrow biopsy, bone marrow transplant, cardiopulmonary resuscitation, liposuction, and median sternotomy. Non-traumatic conditions are very uncommon causes of FES but include acute pancreatitis, fatty liver, corticosteroid therapy, lymphography, fat emulsion infusion, and hemoglobinopathies. In our Unexpected presentation case, while it is possible that the sacral fracture was the origin, blunt injury to fat deposits in soft tissue such as the abdominal wall could also be the source of fat embolism.
Conclusion
Altered mental status in trauma patients with clinical evidence of TBI but normal CT exams may not always be caused by DAI. Manifestations of CFES can be subtle, and the diagnosis may not be expected. By considering characteristic lesion patterns at MRI in combination with the early clinical neurologic course, it is possible to distinguish CFES from DAI with high reliability. Note that radiologists may be more likely to consider the diagnosis of CFES when relevant clinical information from bedside clinicians is communicated. This opens the door for further understanding and management of CFES. Previously, the gold standard to diagnosis of CFES was via clinical exam and application of various clinical indices or scores. However MRI now appears to be the new gold standard. More studies and investigations are needed. Additionally, more education will be required both in the clinical and the radiology communities.
Appendix
References
-
http://www.tbims.org/combi/lcfs/lcfs.pdf
-
Talbot M, Schemitsch EH (2006) Fat embolism syndrome: history, definition, epidemiology. Injury 37 Suppl 4: S3-7.
-
Muller C, Rahn BA, Pfister U, Meinig RP (1994) The incidence, pathogenesis, diagnosis, and treatment of fat embolism. Orthop Rev 23: 107-117.
-
Gupta A, Reilly C (2007) Fat Embolism. Contin Educ Anaesth Crit Care Pain 7: 148-151.
-
Kim YH, Oh SW, Kim JS (2002) Prevalence of fat embolism following bilateral simultaneous and unilateral total hip arthroplasty performed with or without cement: a prospective, randomized clinical study. J Bone Joint Surg Am 84: 1372-1379.
-
Sulek CA, Davies LK, Enneking FK, Gearen PA, Lobato EB (1999) Cerebral microembolism diagnosed by transcranial Doppler during total knee arthroplasty: correlation with transesophageal echocardiography. Anesthesiology 91: 672-676.
-
Stein PD, Yaekoub AY, Matta F, Kleerekoper M (2008) Fat embolism syndrome. Am J Med Sci 336: 472-477.
-
Kim HJ, Lee CH, Lee SH, Cho BM, Kim HK, et al. (2001) Early development of vasogenic edema in experimental cerebral fat embolism in cats: correlation with MRI and electron microscopic findings. Invest Radiol 36: 460-469.
-
Kim HJ, Lee CH, Lee SH, Moon TY (2003) Magnetic resonance imaging and histologic findings of experimental cerebral fat embolism. Invest Radiol 38: 625-634.
-
Bardana D, Rudan J, Cervenko F, Smith R (1998) Fat embolism syndrome in a patient demonstrating only neurologic symptoms. Can J Surg 41: 398-402.
-
Georgopoulos D, Bouros D (2003) Fat embolism syndrome: clinical examination is still the preferable diagnostic method. Chest 123: 982-983.
-
Koul PA, Ahmad F, Gurcoo SA, Khan UH, Naqash IA, et al. (2013) Fat embolism syndrome in long bone trauma following vehicular accidents: Experience from a tertiary care hospital in north India. Lung India 30: 97-102.
-
Gurd AR (1970) Fat embolism: an aid to diagnosis. J Bone Joint Surg Br 52: 732-737.
-
Schonfeld SA, Ploysongsang Y, DiLisio R, Crissman JD, Miller E, et al. (1983) Fat embolism prophylaxis with corticosteroids. A prospective study in high-risk patients. Ann Intern Med 99: 438-443.
-
Citerio G, Bianchini E, Beretta L (1995) Magnetic resonance imaging of cerebral fat embolism: a case report. Intensive Care Med 21: 679-681.
-
Takahashi M, Suzuki R, Osakabe Y, Asai JI, Miyo T, et al. (1999) Magnetic resonance imaging findings in cerebral fat embolism: correlation with clinical manifestations. J Trauma 46: 324-327.
-
Stoeger A, Daniaux M, Felber S, Stockhammer G, Aichner F, et al. (1998) MRI findings in cerebral fat embolism. Eur Radiol 8: 1590-1593.
-
Bodanapally UK, Shanmuganathan K, Saksobhavivat N, Sliker CW, Miller LA, et al. (2013) MR imaging and differentiation of cerebral fat embolism syndrome from diffuse axonal injury: application of diffusion tensor imaging. Neuroradiology 55: 771-778.
-
Park SJ, Hur JW, Kwon KY, Rhee JJ, Lee JW, et al. (2009) Time to Recover Consciousness in Patients with Diffuse Axonal Injury : Assessment with Reference to Magnetic Resonance Grading. J Korean Neurosurg Soc 46: 205-209.
-
Gregorakos L, Sakayianni K, Hroni D, Harizopoulou V, Markou N, et al. (2000) Prolonged coma due to cerebral fat embolism: report of two cases. J Accid Emerg Med 17: 144-146.
-
Parizel PM, Demey HE, Veeckmans G, Verstreken F, Cras P, et al. (2001) Early diagnosis of cerebral fat embolism syndrome by diffusion-weighted MRI (starfield pattern). Stroke 32: 2942-2944.
-
Riska EB, Myllynen P (1982) Fat embolism in patients with multiple injuries. J Trauma 22: 891-894.
-
Shapiro MP, Hayes JA (1984) Fat embolism in sickle cell disease. Report of a case with brief review of the literature. Arch Intern Med 144: 181-182.
-
Dillerud E (1990) Abdominoplasty combined with suction lipoplasty: a study of complications, revisions, and risk factors in 487 cases. Ann Plast Surg 25: 333-338.





