International Journal of Blood Research and Disorders
HemoCue versus Complete Blood Count for Hemoglobin Measurement in Adults with Vaso-occlusive Crisis due to Sickle Cell Disease
Michael Bursey1*, Kane Curtis1, Robert Gibson1, Hongyan Xu2 and Matthew Lyon1
1Department of Emergency Medicine, Georgia Regents University, USA
2Department of Biostatistics, Medical College of Georgia, Georgia Regents University, USA
*Corresponding author:
Max Bursey DO, Department of Emergency Medicine, Georgia Regents University, USA, Tel: (706) 721-4951, E-mail: mbursey@gru.edu
Int J Blood Res Disord, IJBRD-2-007, (Volume 2, Issue 1), Research article; ISSN: 2469-5696
Received: January 01, 2015 | Accepted: February 14, 2015 | Published: February 17, 2015
Citation: Bursey M, Curtis K, Gibson R, Xu H, Lyon M (2015) HemoCue versus Complete Blood Count for Hemoglobin Measurement in Adults with Vaso-occlusive Crisis due to Sickle Cell Disease. Int J Blood Res Disord 2:007. 10.23937/2469-5696/1410007
Copyright: © 2015 Bursey M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Hemoglobin (Hgb) measurement is an important risk-stratification tool for patients presenting to the Emergency Department with vaso-occlusive crisis (VOC) from sickle cell disease (SCD). Point-of-care (POC) Hgb testing such as the HemoCue device decreases time to identification of significant anemia. However, there are no studies evaluating the accuracy of HemoCue testing in patients with SCD and VOC. The purpose of this study was to evaluate the correlation of Hgb measurements from HemoCue compared to automated complete blood counts (CBC) in SCD patients with suspected VOC. This was a retrospective database and chart review comparing Hgb values from CBC (Beckman-Coulter LH-750) to values from HemoCue (Hb 201+) analyzers among SCD patients with VOC. All patients (age ≥ 18) with VOC presenting to the ED (annual census 85,000) were included in the study. HemoCue testing was completed via finger stick, and whole blood for CBC was obtained within 30 minutes of establishing IV access. Subjects were grouped based on ED use (low-users ≤ 1 ED visit/year, high-users >1 visit/year) and Hgb level (Hgb>12.0 g/dL, 8.0 to 11.9g/dL, and < 8g/dL). Paired CBC and HemoCue hemoglobin measurements were obtained from 653 ED visits from 107 SCD patients over a period of eight years. The mean hemoglobin values obtained from HemoCue and CBC are 9.1g/dL (SD 2.02), and 9.2g/dL (SD 1.83), respectively. The mean difference of HemoCue and CBC hemoglobin measurements is 0.008, and it is not significant with p=0.939. The 95% confidence interval of the mean difference is (-0.217, 0.201). There were 30 patients in the low-user group and 77 patients in the high-user group. There are no significant differences in results grouped by hemoglobin level, at the 0.05 significance level. Correlation between the two methods of measurement was best in the 8.0-11.9g/dL hemoglobin range (r=0.73). Correlation at hemoglobin values greater than 12.0g/dL and less than 8.0g/dL was poor (r=0.30, r=0.57). These results demonstrate that Hgb measurements from HemoCue testing are comparable to values obtained by CBC in patients with SCD VOC, especially the 8.0-11.9g/dL hemoglobin range.
Keywords
Sickle cell disease; Vaso-occlusive crisis; Anemia; Point-of-care; Hemoglobin
Introduction
Sickle-cell disease is one of the most common genetic disorders in the world and results from mutation of the HHB gene, which leads to production of abnormal beta-globin subunits of hemoglobin, known as hemoglobin S (HbS). This abnormal hemoglobin is prone to polymerization, causing erythrocyte rigidity and vaso-occlusion, which is the central pathophysiology of this disease. Adults with SSD almost universally suffer from chronic anemia and hemolysis, and most are at risk for serious complications such as aplastic crisis, acute chest syndrome, sepsis, central nervous system infarction, pulmonary hypertension, priapism, and many others. Pain associated with vaso-occlusive crisis (VOC) is the most common complication in patients with Sickle Cell Disease (SCD) presenting to the emergency department [1-4]. Emergency physicians are charged with the task of not only treating the pain associated with VOC, but to evaluate for serious precipitating causes and coexisting complications, some of which may be life-threatening [2,5,6]. While a variety of clinical criteria are useful in risk-stratifying patients presenting with suspected VOC, laboratory evaluations often play a significant role in identifying high-risk presentations [2,3,5-7]. Because almost all patients with sickle cell disease have some degree of baseline anemia, measurement of the hemoglobin level is one of the most important lab evaluations, because it identifies worsening from baseline anemic states, prompting changes in management strategies and disposition [1,3,5]. Clinically significant anemia generally only occurs with severe VOC, or in association with other emergency conditions such as aplastic crisis or acute chest syndrome. A patient presenting with VOC symptoms and significant worsening of anemia should prompt more extensive evaluation for such pathologies. Therefore, the rapid determination of hemoglobin level in the emergency department has significant implications on many quality-focused endpoints to include time to definitive diagnosis, length of ED stay, and overall resource utilization.
Point-of-care hemoglobin testing using such systems such as the HemoCue device may aid in decreasing time to identification of significantly worsening or severe anemia. Previous studies have shown variability in hemoglobin results using HemoCue systems [8-11]. However, there is relative agreement that this variability does not negatively impact the utility of the HemoCue in making clinically important decisions, specifically those regarding the need for transfusion [10-14]. Additionally, Jaeger et al. [11] showed adequate correlation between HemoCue and standard hemoglobin measures across a broad range of hemoglobin values in patients without SCD [11]; McNulty et al. [13] showed that HemoCue values continued to show excellent correlation even at hemoglobin values less than 8.0 g/dL [13]. However, there are no studies to date evaluating the accuracy of hemoglobin measurement using HemoCue in SCD patients. The objective of this study was to evaluate the correlation of hemoglobin values obtained from point-of-care (POC) HemoCue testing compared to those obtained from automated blood counts in patients with SCD patients with suspected VOC. Secondary analysis was performed on subgroups to evaluate for consistency of correlation across high, intermediate, and low hemoglobin ranges.
Methods
This study is a retrospective database and chart review comparing hemoglobin values obtained from automated blood counts to those obtained from a HemoCue for SCD patients with pain and suspected VOC. All adult (age ≥ 18) patients with SCD and suspected VOC who presented to the ED were included in the study as part of an observation unit-based VOC protocol; the study was conducted at a tertiary care urban ED with an annual census of approximately 90,000 patients per year. Patients had a screening POC HemoCue completed at ED triage obtained from capillary blood via finger stick. Subjects subsequently underwent venipuncture to obtain blood for an automated blood count, performed after placement in a room in the observation unit or the main ED. POC hemoglobin analysis was performed using a HemoCue Hb 201+ analyzer, while automated measurements were obtained as part of the complete blood count using a Beckman-Coulter LH 750 analyzer.
The number of ED visits per year was highly variable between subjects. In order to minimize bias introduced by a few patients with a high number of visits, subjects were broken down into low-users (those with a maximum of one visit per year) and high-users (those with greater than one visit per year) and analyzed separately. A one-sample paired t-test was performed to compare the HemoCue values with CBC hemoglobin values between high and low utilizers. The data was also analyzed cumulatively.
An analysis was performed to evaluate for correlation of hemoglobin values between the two methods of measurement. The cumulative data was analyzed by calculating an intra-class correlation coefficient (ICC) between POC HemoCue and hemoglobin values derived from CBC. Additionally, a Bland-Altman analysis was performed to examine the agreement between HemoCue and lab hemoglobin values. Further analysis was performed by dividing the hemoglobin values into three groups consisting of hemoglobin values greater than 12.0g/dL, hemoglobin values 8.0 to 11.9g/dL, and hemoglobin values less than 8.0g/dL, in order to determine differences based on degree of anemia. A one-sample paired t-test was then performed on each subgroup. No distinction was made between males and females. For analyses, we chose a significance level (α) of 0.05.
Results
Paired CBC and HemoCue hemoglobin measurements were obtained from 653 ED visits from 107 SCD patients over a period of eight years. The mean hemoglobin values obtained from HemoCue and CBC are 9.1g/dL (SD 2.02), and 9.2g/dL (SD 1.83), respectively. The overall mean difference of HemoCue and CBC hemoglobin measurements is 0.008, and it is not significant with p=0.939. The 95% confidence interval of the mean difference is (-0.217, 0.201). The ICC = 0.86 with 95% CI (0.839, 0.879). An F-test is highly significant (p=1.51E-193), indicating the high consistency between HemoCue and CBC hemoglobin values. The Bland-Altman plot (Figure 1) shows that most of the differences between HemoCue and CBC hemoglobin values are well within the 95% limit, and there is no systematic difference between HemoCue and hemoglobin values.
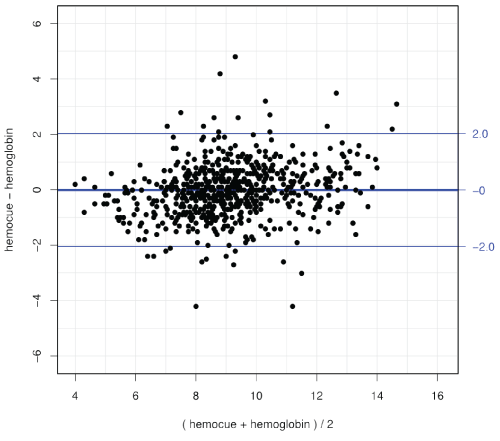
Figure 1: Bland-Altman plot of cumulative data
View Figure 1
There were 30 patients in the low-user group and 77 patients in the high-user group. The HemoCue and automated hemoglobin values are shown in Table 1. There is no significant difference between the two methods of hemoglobin measurement in either group at the 0.05 significance level. Results grouped by hemoglobin level are shown in Table 2. There are no significant differences at the 0.05 significance level. Correlation between the two methods of measurement was best in the 8.0-11.9g/dL hemoglobin range (r=0.73), and is shown in Figure 2. Correlation at hemoglobin values greater than 12.0g/dL and less than 8.0g/dL was poor (r=0.30, r=0.57). Figure 3 shows correlation for hemoglobin less than 8.0g/dL, and Figure 4 shows correlation for hemoglobin greater than 12.0g/dL.
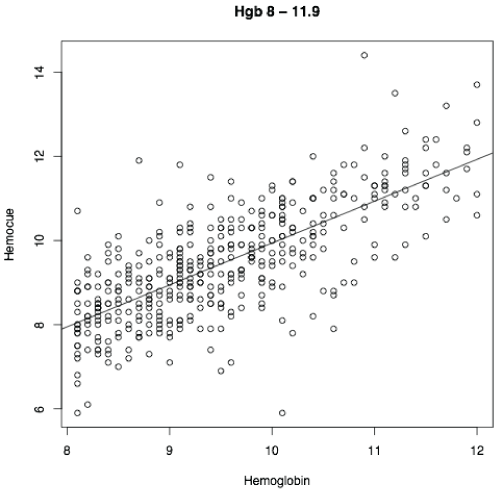
Figure 2: Correlation in the Hgb 8.0 � 11.9g/dL group r=0.73
View Figure 2
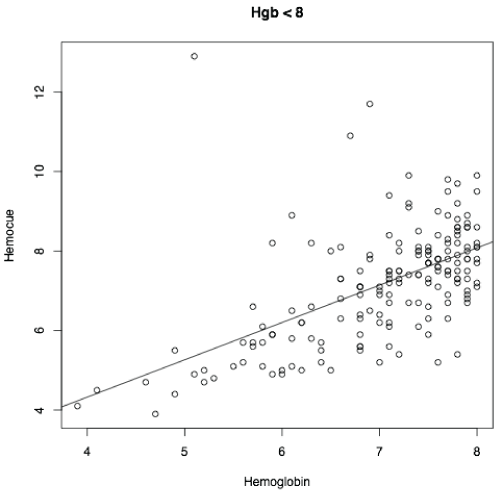
Figure 3: Correlation in the Hgb < 8.0g/dL group r=0.57
View Figure 3
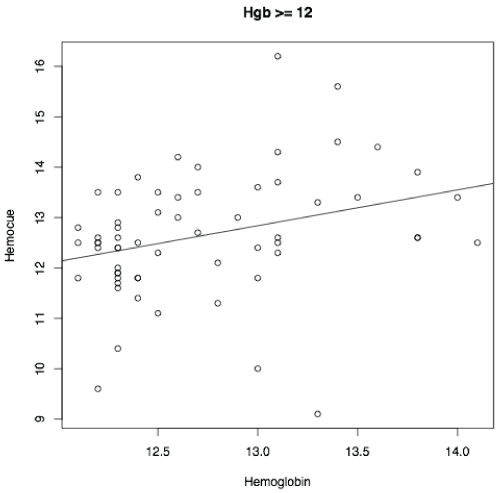
Figure 4: Correlation in the Hgb >12.0 g/dL group r=0.30
View Figure 4
![]()
Table 1: High and low user group analysis of hemoglobin levels derived by POC HemoCue and automated CBC. hemoglobin measurement.
View Table 1
![]()
Table 2: Analysis of hemoglobin levels based on degree of anemia.
View Table 2
Discussion
The results of this study demonstrate that hemoglobin measurements obtained from point-of-care HemoCue testing are comparable to hemoglobin values obtained from automated blood count testing in the setting of sickle cell disease vaso-occlusive crisis, especially in hemoglobin range of 8.0 � 11.9g/dL. At lower values, the correlation is poor. In the clinical setting, a HemoCue measurement of less than 8.0g/dL should prompt a CBC performed by the lab (the gold standard test in evaluating for anemia) in order to determine the true hemoglobin level. Accurate determination of hemoglobin in the severely anemic SSD patient is crucial in order to identify a significant drop from baseline hemoglobin, as this may be a clue to indicate serious underlying pathology requiring more extensive evaluation.
This study also demonstrated that correlation to CBC hemoglobin level is also poor with HemoCue values greater than 12.0g/dL. However, routinely obtaining follow-up CBC to accurately determine hemoglobin level in this group of patients, assuming they are non-toxic appearing without significant hemodynamic derangement, is probably not necessary. Emergent complications related SSD generally present with worsening anemia, not an increase in Hgb from baseline, so the poor correlation at values greater than 12.0g/dL is likely of little clinical significance.
These findings have clear, positive implications in the emergency department setting. They suggest that the triage process of patients with SCD may be streamlined by utilizing POC hemoglobin measurements, thus allowing clinicians to more quickly distinguish between routine VOC and complicated presentations. It may also reduce the volume of blood drawn from the patients that comprise this already anemic population. Furthermore, there is likely a significant cost benefit to obtaining only POC hemoglobin for most SCD patients with suspected VOC, rather than routinely ordering CBCs. In 2014, the Centers for Medicare and Medicaid Services national limit for reimbursement of a POC hemoglobin was $3.23, whereas a CBC with automated differential was $10.61, more than three times as much [15]. Additionally, the HemoCue micro-cuvettes are inexpensive, approximately $1.87 per cartridge [16], although some studies have noted the difficulty in obtaining them internationally [17,18] which may limit its cost-effectiveness outside of the United States. The overall implication is that when combined with other subjective and objective markers of complicated crisis, POC hemoglobin testing may help identify a low risk group of ED patients with SCD who do not require more in-depth laboratory evaluation. These patients could then be routinely treated by a protocoled pain management plan for VOC and avoid additional resource-intensive evaluations.
Limitations
There are several limitations to this study. First, the sample population is a cohort of patients presenting to one urban academic ED. Despite the 8-year length of the study, the sample population was still relatively small, with only 107 patients, and the results may therefore not be generalizable to other patient populations or environments. As a single center study, the results do not account for patient visits to other local emergency departments, nor did we take into account the addition or loss of patients from the sickle cell observation pathway. Furthermore, only the HemoCue analyzer was used for this study and it is unknown whether alternative POC hemoglobin devices would perform similarly. Lastly, this study only addressed adult patients with SCD, and did not include pediatric patients, nor did it differentiate between males and females.
References
-
Koshy M, Leikin J, Dorn L, Lebby T, Talischy N, et al. (1994) Evaluation and Management of Sickle Cell Disease in the Emergency Department (An 18-year Experience): 1974--1992. Am J Ther 1: 309-320.
-
Glassberg J (2011) Evidence-based management of sickle cell disease in the emergency department. Emerg Med Pract 13: 1-20.
-
Redding-Lallinger R1, Knoll C (2006) Sickle cell disease--pathophysiology and treatment. Curr Probl Pediatr Adolesc Health Care 36: 346-376.
-
Shapiro BS, Benjamin LJ, Payne R, Heidrich G (1997) Sickle cell-related pain: perceptions of medical practitioners. J Pain Symptom Manage 14: 168-174.
-
Brandow AM, Liem R (2011) "Sickle Cell Disease in the Emergency Department: Atypical Complications and Management" Clin Pediatr Emerg Med 12: 202-212.
-
Hampton R, Balasa V, Bracey SEA (2005) Emergencies in Patients with Inherited Hemoglobin Disorders-An Emergency Department Perspective. Clin Ped Emerg Med 6: 138-148
-
Bernard AW, Venkat A, Lyons MS (2006) Best evidence topic report. Full blood count and reticulocyte count in painful sickle crisis. Emerg Med J 23: 302-303.
-
Neufeld L, Garc�a-Guerra A, S�nchez-Francia D, Newton-S�nchez O, Ramirez-Villalobos MD, et al. (2002) Hemoglobin measured by Hemocue and a reference method in venous and capillary blood: a validation study. Salud Publica Mex 44: 219-227.
-
Morris SS, Ruel MT, Cohen RJ, Dewey KG, de la Bri�re B, et al. (1999) Precision, accuracy, and reliability of hemoglobin assessment with use of capillary blood. Am J Clin Nutr 69: 1243-1248.
-
Rippmann CE, Nett PC, Popovic D, Seifert B, Pasch T, et al. (1997) Hemocue, an accurate bedside method of hemoglobin measurement? J Clin Monit 13: 373-377.
-
Jaeger M, Ashbury T, Adams M, Duncan P (1996) Perioperative on-site haemoglobin determination: as accurate as laboratory values? Can J Anaesth 43: 795-798.
-
Gehring H, Hornberger C, Dibbelt L, Rothsigkeit A, Gerlach K, et al. (2002) Accuracy of point-of-care-testing (POCT) for determining hemoglobin concentrations. Acta Anaesthesiol Scand 46: 980-986.
-
McNulty SE, Torjman M, Grodecki W, Marr A, Schieren H (1995) A comparison of four bedside methods of hemoglobin assessment during cardiac surgery. Anesth Analg 81: 1197-1202.
-
Lardi AM, Hirst C, Mortimer AJ, McCollum CN (1998) Evaluation of the HemoCue for measuring intra-operative haemoglobin concentrations: a comparison with the Coulter Max-M. Anaesthesia 53: 349-352.
-
(2014) Centers for Medicare and Medicaid Services: Clinical Laboratory Fee Schedule.
-
(2015) Fisher Scientific: HemoCue Hb 201+ Analyzer. Accessed 7 February.
-
Johns WL, Lewis SM (1989) Primary health screening by haemoglobinometry in a tropical community. Bull World Health Organ 67: 627-633.
-
Medina Lara A, Mundy C, Kandulu J, Chisuwo L, Bates I (2005) Evaluation and costs of different haemoglobin methods for use in district hospitals in Malawi. J Clin Pathol 58: 56-60.





