International Journal of Brain Disorders and Treatment
Speech Disorder and Behavioral Involvement in a Thalamic Stroke: A Case Report
Paola Caruso*, Moretti R and Manganotti P
Clinical Neurology, University of Trieste, Trieste, Italy
*Corresponding author:
Paola Caruso, MD, Neurologist, Clinical Neurology, University of Trieste, Azienda Ospedaliero Universitaria di Trieste, Trieste, IT, Italy, E-mail: caruso.paola1983@libero.it
Int J Brain Disord Treat, IJBDT-1-007, (Volume 1, Issue 1), Case Report; ISSN: 2469-5866
Received: November 10, 2015 | Accepted: December 11, 2015 | Published: December 14, 2015
Citation: Caruso P, Moretti R, Manganotti P (2015) Speech Disorder and Behavioral Involvement in a Thalamic Stroke: A Case Report. Int J Brain Disord Treat 1:007. 10.23937/2469-5866/1510007
Copyright: © 2015 Caruso P, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Data from literature on clinical manifestation of thalamic strokes have been published for ages. First in 1906 Dejerine e Roussy has spoken about sensory motor disturbances and have opened the door to new pathologic disorders that may occur after thalamic lesions. From 1925 behavior and speech disorders related with thalamic injury were described. Since then a classification of thalamic syndromes into four groups based on the four main arterial territories was accepted. As we know thalamic stroke account for 11% of vertebra basilar infarct. Inferolateral territory infarctions are the most common injury (45%), followed by the paramedian territory infarctions (35%) and the anterior territory lesions (12%), the posterior territory infarctions are less frequent (8%). Anyway lots of symptoms cannot still be classified easily and strictly into only one of these four groups and several variant topographic patterns of thalamic strokes with distinct manifestation and etiology have been proposed.
Here we described the case of one young Caucasian man that was admitted to the emergency department for a sudden onset of dizziness with left lateropulsion, vertigo, visual impairment and speech disorder involving unpredictable topic shifts but grammatically correct. During recovery patient performed a typical behavior disorder consisting mainly in lack of emotion and memory long or short term loss. Magnetic resonance was performed and showed left thalamic infarction involving paramedian territory.
The complex cognitive and behavioral disorders described can be explained only supporting the already described different topographic patterns of thalamic infarction.
Keywords
Acute thalamic stroke, Speech disorders, Palipsychism, Memory disorders.
Case Report
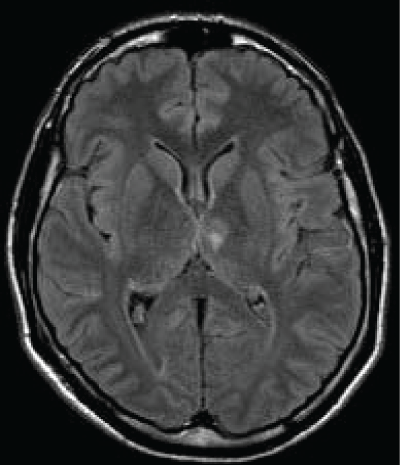
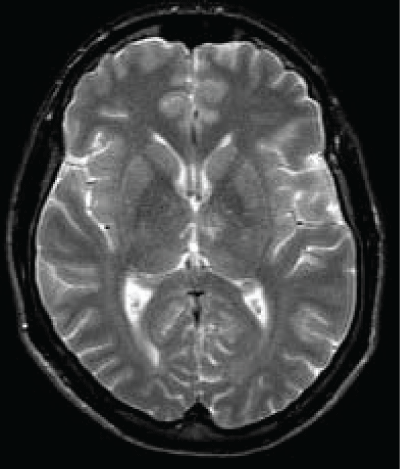
A 45 years old Caucasian male was admitted to our Neurological Clinic for a sudden onset of visual impairment and pure horizontal diplopia, disequilibrium and left lateropulsion. While he was coming to hospital he noted also a speech disorder (mainly referred as word-finding difficulties, reduced fluency, denomination and writing disorders). At admission cerebral CT and angio-CT was performed but no lesions were seen, neither vessels abnormalities. During hospitalization antiplatelet therapy was started. Patient performed screening vascular examination including echocardiography carotid Doppler and thrombophylic screening tests. Soon dizziness and visual disorder ameliorated but then he showed palipsychism (which corresponds to an overlap of sequential cognitive processes in two or more domains); patient also showed severe perseverative behavior with increased sensitivity to interference, anterograde memory retrieval deficit with memory loss and produced a decreased and invalid-output speech, characterized by unpredictable topic shifts, with grammatically correct phrases, sometimes he accused naming difficulties and apathy with affective flatness. Moreover he accused some kind of stiffness on both his upper arms. Neuropsychological tests were performed showing preservation in performing automatic series and executive functions, and a "transcortical sensitive-aphasia-like speech disorder". After a few days cerebral magnetic resonance was performed, it showed a thalamic ischemia in the paramedian left thalamic nuclei territory (Figure 1 and Figure 2); as a result of a possible cardioembolic stroke.
It's well known that Paramedian artery arises from P1 Cerebral Posterior artery, and supplies several thalamic nuclei as medial dorsal nucleus, intralaminar, posteromedial ventrolateral, ventromedial pulvinar, paraventricular and dorsal internal medullary lamina.
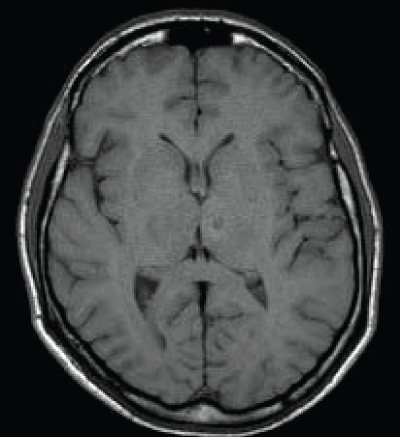
As we said the fluid-attenuated inversion recovery (FLAIR) and T2 MRI revealed a hyperintense lesion (hypointense in T1 sequences) compatible with a left paramedian thalamic infarction in a patient with onset of confusion, confabulation, and memory impairment (Figure 3). Patient was discharged at home but he felt not to be confident to live alone anymore.
From a neuropsychological point of view the patient is right handed (+ 22 at Brigg's and Nibes test). He was bilingual L1 Slovenian, L2 (non mother tongue) Italian speaking frequent.
He commonly employed L2 in every day speech and in ordinary activities. During hospitalization he was tested only in L2. Very little hypophonie has been observed, but no dysprosody. Language was fluent with frequent perseveration and not-finalistic verbosity.
Occasionally he made paraphasic mistakes; he produced morphologically correct but semantically unfitting sentences, without relevant comprehension deficits. Regard to the examiner comments he was emotionally unperturbed, showing loss of initiative and reported absence of spontaneous thoughts, conceptualized as loss of psychic self activation.
No dysgraphia or apraxia and no chronotaraxis (meant as distortion or confusion in the perception of time) have been observed [1].
As Hodges et al. have reported also our patients manifested major memory loss, with a systematic distortion of irrelevant stimuli but relative spearing of knowledge of public events suggesting a thematic retrieval memory disorder [2].
Discussion
Thalamic stroke account for 11% of vertebro-basilar infarcts, during ages according to pathological data four territories for thalamic vascularization were identified and four different thalamic syndromes have been described.
The main vessels that supply thalamic circulation are four, following the current topographic nomenclature they're named tuberothalamic, paramedian, inferolateral and posterior choroidal artery; the tuberothalamic (anterior or polar artertery; the artery is absent in about one third of cases, and the anterior territory is then supplied by the paramedian arteries) for the anterior territory; the paramedian arteries (the left and right paramedian arteries that can originate from a single pedicle, the thalamogeniculate arteries) principally for the dorsomedial nucleus, internal medullary lamina, and intralaminar nuclei; inferolateral artery for the same territory and the posterior choroidal arteries that provide for posterior territory irroration [3].
Cardioembolism is the most frequent stroke mechanism for the anterior territory injury, hypertensive microangiopathy for central strokes and microangiopathy and artery-to-artery embolism for infarctions in the posterolateral area [4].
A borderzone mechanism between adjacent territories can be suspected in all of the variant territories. A transient occlusion of 1 of the 4 main arteries of the thalamus may result in ischemia of the most distal area supplied by the artery, causing borderzone infarct. Borderzone infarcts occur especially in patients with small thalamic infarcts. It's well known that all thalamic arteries can be subject to variation. Carreara et al. showed that for the anteromedian territory, the variant anteromedian arteries, as paramedian arteries do, probably originate from the first part of the posterior cerebral arteries near the "top of the basilar" artery. The arteries supplying the posterolateral territory might be thalamogeniculate arteries; this may explain the predominant microangiopathic etiology of posterolateral infarcts.
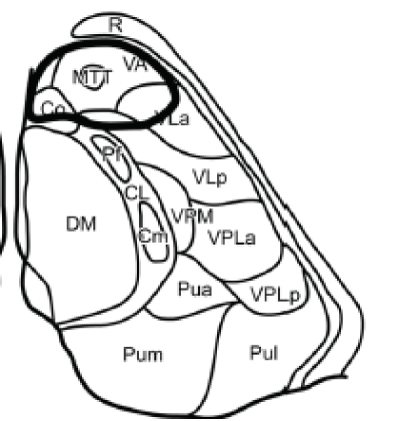
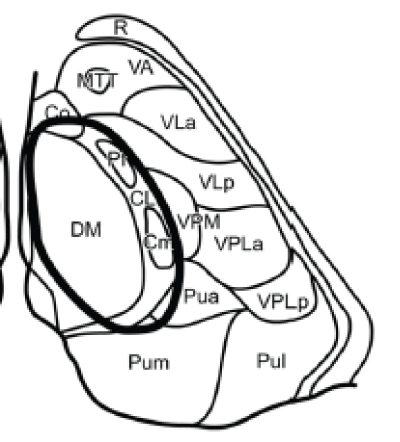
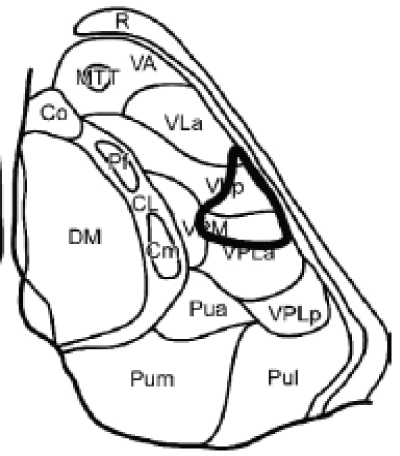
Tuberothalamic artery originates from the posterior communicating artery, irrigates the reticular nucleus, ventral anterior nucleus (VA), rostral part of the ventrolateral nucleus (VL), ventral pole of the medial dorsal nucleus (MD), ventral part of the internal medullary lamina, and anterior thalamic nuclei [anteromedial (AM), anteroventral (AV), and anterodorsal (AD)]. The anterior nuclei receive projections from the mammillothalamic tract (MTT) and are connected to the anterior limbic system (including the cingulated gyrus, hippocampus, parahippocampal formation, and orbitofrontal cortex) and to the medial and prefrontal cortex. Thereof injury in this area may lead to a particular behavioral pattern, including superimposition of unrelated information ("palipsychism" from the Greek "palin" (again) and "psyche" (soul), with parallel expression of mental activities, irrespective of sequential order) and perseverations ("anterior behavioral syndrome"), apathy, and amnesia [5] (Figure 4).
The clinical syndrome resulting from anterior territory injury consists in wide-ranging neuropsychological deficits. Patients might exhibit fluctuating levels of consciousness, personality changes disorientation in time and place, euphoria, lack of insight, apathy, and lack of spontaneity. Very frequently can be observed an impairment of recent memory, as well as verbal and visual memory deficits, impairment of new learning (more evident for left-sided lesions). Patients frequently show perseverative pattern in thinking and speech with inappropriate maintenance of semantic categories. Anomia, impairment of comprehension and fluent paraphasic speech is often seen. Semantic and phonemic paraphasic errors occur, with occasional neologisms and perseveration. Repetition is usually preserved. Left thalamic lesions maybe associated with acalculia. Visual spatial processing deficits occur after right tuberothalamic lesions, visual memory deficits and hemispatial neglect. If the lesion involves mainly the anterior nuclei memory is severely impaired, but language is relatively spared. Ghika-Schmid and Bogousslavsky described several patients in which dysarthria, hypophonia, anomia, and decreased verbal and nonverbal fluency were noted, but comprehension, writing, reading, and repetition were normal. Moreover all patients, showed persistent deficits in new learning and severe perseverative behaviors in thinking, spontaneous speech (patients were giving unrelated information, producing a state of parallel expression of mental activities, with disorganization of autobiographic recollection and newly acquired information), memory, and executive tasks.
The patient first described, as we said, presented at the beginning dizziness and visual disorder (soon ameliorated), then he showed several neuropsychological deficit as palipsychism, lack of emotion, apathy and anxiety. Moreover, like is well described in literature, our patient showed memory impairment with relatively spared language. Memory loss and palipsychism are also described in the thalamopolar syndrome as described later on.
Paramedian arteries (arising from the P1 section of the posterior cerebral artery) supplies dorsomedian nucleus (divided into anteromedial magnocellular and posterolateral parvocellular mediodorsal nucleus) that receives projections from the amygdala and has connections to the prefrontal cortex and ventral pallidum; and the intralaminar nuclei: central lateral (CL), centromedian (CM), and parafascicular (Pf); the intralaminar nuclei are divided into the caudal part and the rostral part they project to the orbitofrontal and mediofrontal cortex, the motor and premotor cortex, and the internal globus pallidus. When the tuberothalamic artery is absent, the paramedian artery may assume that territory as well (Figure 5).
As we said lesions in those areas cause almost the 35% of all thalamic infarction, this may lead to neuropsychological disturbances with "loss of psychic self activation", impairment of arousal with decreased and fluctuating level of consciousness confusion, agitation, aggression, and apathy may be persistent features. Guberman and Stuss described the adynamic aphasia, a speech and language disorder with hypophonia, dysprosody, perseveration, reduced verbal fluency. For bilateral infarction in the paramedian artery territory deep coma, "coma vigil" or akinetic mutism often accompanied by eye movement abnormalities has been described. The amnestic syndrome resulting from paramedian territory injury may be illustrated as thalamic dementia with behavioral and cognitive deficit. Finally neurological signs include complete or partial vertical gaze, paresis, and loss of convergence, pseudo-sixth nerve palsies, bilateral internuclear ophthalmoplegia, miosis, and even intolerance to bright light.
The inferolateral arteries arise from the P2 branch of the posterior cerebral artery, supply the major part of the ventral posterior nuclei (lateral [VPL], medial [VPM], and inferior [VPI]), as well as the ventral and lateral parts of the VL nucleus more rostrally. The ventrolateral nucleus has connections to the cerebellum and the motor and prefrontal cortex, while the ventroposterolateral nucleus receives inputs from the medial lemniscal and spinothalamic pathways, finally the ventroposteromedial nucleus receives inputs from the trigeminothalamic pathway (Figure 6).
Infarction in the inferolateral territory are the most common infarctions and account for the 45% of all thalamic injury. Lesions drive to the thalamic pain syndrome described by Dejerine and Roussy with sensory loss impaired extremity movement, sometimes with postlesion pain. Controlateral Ataxia and hypesthesia is common. The involvement of the different subcomponents of the VL, in particular, which link deep cerebellar nuclei with motor, premotor, prefrontal, and posterior parietal regions of the cerebral hemispheres, may also have markedly different clinical consequences.
The posterior choroidal arteries (from the posterior cerebral artery) supply the subthalamic nucleus and midbrain, the medial half of the medial geniculate nucleus, the posterior parts of the intralaminar nuclei CM and CL and the pulvinar nuclei. Only limited information on the clinical manifestations injury in this area is known. Data from literature showed that quadrantanopsia and controlateral hypesthesia was detected. Neuropsychological signs included neglect and aphasia.
Somewhere else thalamopolar syndrome was described, this can occur when vascular variation exit and in up to one third of humans, the polar artery is missing and its territory taken over by the paramedian arteries. The infarct is clinically dominated, in the acute phase, by "palipsychism" and is in most cases associated with severe perseverative behavior and increased sensitivity to interference, anterograde memory disturbance, intrusions, naming difficulties, dysarthria, hypophonia, and apathy. Thalamopolar stroke involving left side o thalamus is associated with subcortical aphasia, while right-sided with hemineglect and impaired visuospatial processing [6].
Leaving that about 30% of all stroke patients with isolated thalamic infarct may have a lesion outside the classical territories, in 2004 Carrera at al proposed three variant territories: the anteromedian territory which lesions are in charge for cognitive impairment, decreased consciousness, and vertical eye paresis (less frequent are memory impairment, loss of initiative and executive dysfunction, aphasia, visual agnosia, ideomotor apraxia with orofacial apraxia, and vertical eye paresis). The central territory responsible of decreased consciousness, cognitive impairment, including aphasia, executive dysfunction, and memory impairment. All patients had contralateral hypesthesia. Vertical eye paresis was found in the patient with bilateral lesions. Finally the posterolateral territory, neurological deficit for lesions in this area is sensory deficit, moderate to severe contralateral hypesthesia, contralateral ataxia.
Conclusion
The intralaminar nuclei seem to play an important role in arousal and motivation due to a direct involvement of the striatal-ventral pallidal-fronto orbital circuits. This system highly reflects on motivation and limbic strategies, and the eventual brisk interruption of these circuits may lead to a disconnection of the posterior orbital and rostral frontal cortex to the anterior cingulated gyrus and back to the striatum.
The thalamic peduncles at the superior medial and inferior and lateral aspects of thalamus convey information in and out of the thalamus.
Lesions restricted to these parts occur rarely but their relevance is considering the anatomic basis on the behavior is suggestive. In particular the intralaminar nuclei play a role in autonomic drive and they provide the striatum with attention-specific sensory information important for conditional responses
Moreover the functional properties of the different thalamic nuclei are inferred from these clinical-anatomic observations and from the reciprocal connections with behaviorally defined regions of the cerebral cortex. As we saw, behavioral manifestations are multiple, and virtually all "cortical" syndromes may be mimicked by thalamic strokes, which reflect the role of the "little brain" of the thalamus in behavior and cognition. Particular behavioral syndromes associated with anterior and paramedian lesions may often be difficult to distinguish from primary psychiatric disorders [7].
In the same way highly selective centromedian thalamic lesion responsible to the complete clinical picture of thalamic astasia was described, while, as we know, thalamic astasia has been reported more often in patients with posterolateral thalamic lesions [8].
Our patient experienced a syndrome that might be classified into the anterio-median territory injury, infect he developed a speech related disorder with decreased verbal and nonverbal fluency, perseverative behaviors in thinking and spontaneous speech (palipsychism), but also neuropsychological disturbances with "loss of psychic self activation", dysprosody, deficit in the use of the speech and not linguistic deficit, short memories loss. Moreover when admitted he presented partial vertical gaze, pseudo-sixth nerve palsies and intolerance to bright light.
According to the literature we believe that the classification of thalamic infarctions cannot be limited at the four classical syndromes but must consider also the several clinic-anatomic variants already described. Damage to thalamic circuits results in wide-ranging effects, including cognition and behavior. Knowledge of functional anatomy is important in the recognition and understanding of such impairment. More studies are required to explain different thalamic syndrome pathways.
References
-
Spiegel EA, Wycis HT, Orchinik C, Freed H (1956) Thalamic chronotaraxis. Am J Psychiatry 113: 97-105.
-
Evans Jon, Wilson Barbara, Wraight E Philip, Hodges John R (1993) Neuropsychological and SPECT scan findings during and after transient global amnesia: evidence for the differential impairment of remote episodic memory. J Neurol Neurosurg Psychiatry 56: 1227-1230.
-
Schmahmann JD (2003) Vascular syndromes of the thalamus. Stroke 34: 2264-2278.
-
Carrera E, Michel P, Bogousslavsky J (2004) Anteromedian, central, and posterolateral infarcts of the thalamus: three variant types. Stroke 35: 2826-2831.
-
Carrera E, Bogousslavsky J (2006) The thalamus and behavior: effects of anatomically distinct strokes. Neurology 66: 1817-1823.
-
Perren F, Clarke S, Bogousslavsky J (2005) The syndrome of combined polar and paramedian thalamic infarction. Arch Neurol 62: 1212-1216.
-
Janssen PM, Schreuder AH, Koehler PJ (2015) Delayed dysosmia and dysgeusia after thalamic infarction. J Neurol Sci 348: 286-287.
-
Elwischger K, Rommer P, Prayer D, Mueller C, Auff E, et al. (2012) Thalamic astasia from isolated centromedian thalamic infarction. Clinical/Scientific Notes. Neurology 78: 146-147.