International Journal of Brain Disorders and Treatment
Subarachnoid Haemorrhage in Patient with Eosinophilic Granulomatosis with Polyangiitis (Churg and Strauss): A Probable Central Nervous Localisation of Vasculitis
Lescuyer Sylvain*, Rondeau-Lutz Murielle, Martinez Camille, Rakotoarivelo Hanta-Nirina and Weber Jean-Christophe
Service de medecine interne, NHC, Hopitaux Universitaires de Strasbourg, 1 place de l'hôpital 67091 Strasbourg cedex, France
*Corresponding author:
Lescuyer Sylvain, Service de medecine interne, NHC, Hopitaux Universitaires de Strasbourg, 1 place de l'hopital 67091 Strasbourg cedex, France, E-mail: lescuyer.s@gmail.com
Int J Brain Disord Treat, IJBDT-1-006, (Volume 1, Issue 1), Case Report; ISSN: 2469-5866
Received: September 27, 2015 | Accepted: October 20, 2015 | Published: October 22, 2015
Citation: Sylvain L, Rondeau-Lutz M, Camille M, Hanta-Nirina R, Jean-Christophe W (2015) Subarachnoid Haemorrhage in Patient with Eosinophilic Granulomatosis with Polyangiitis (Churg and Strauss): A Probable Central Nervous Localisation of Vasculitis. Int J Brain Disord Treat 1:006. 10.23937/2469-5866/1510006
Copyright: © 2015 Sylvain L, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
We report the case of a 43 year-old patient with Subarachnoid haemorrhage (SAH). He was diagnosed with EGPA because of asthma, naso-sinusal polyposis, asymmetrical peroneal neuritis, general signs, eosinophilic count at 4000/mm3, CRP at 50 mg/l and positive pANCA with anti-MPO specificity at 74 U/ml. Arteriography was normal. He was treated by methylprednisolone and cyclophosphamide. Remission was complete. EGPA is a rare primary vasculitis. Only seventeen cases of central nervous haemorrhages have been reported. EGPA may be revealed by an acute neurologic manifestation as in seven (41%) reported cases.
Keywords
Subarachnoid haemorrhage, Churg and Strauss
Introduction
We report the case of a 43 year-old patient with Subarachnoid haemorrhage (SAH) as part of an Eosinophilic Granulomatosis with Polyangeitidis (EGPA) (ex-Churg and Strauss).
Case History
A 43 year old patient known for allergic asthma since he was 20 years was admitted in emergency for SAH.
The history began on 2012 with a florid and disabling nasal and sinusal polyposis. On February 2013, an asthma attack was treated with prednisolone while he was asymptomatic for years. Eosinophilic count rated 875/mm3 and chest computer tomography scan showed alveolar infiltrates.
On May 2013, he was diagnosed with EGPA. New clinical signs were: arthro-myalgia, asymmetrical peroneal neuritis, weight loss and night-sweats. Eosinophilic count was 4000/mm3, CRP was 50 mg/l, pANCA were positive with anti-MPO specificity at 74 U/ml. Because of Five Factor Score (FFS) at 0, he was treated with prednisolone 60 mg/d. On June 2013, Cyclophosphamide (750 mg/m2 monthly) was added because of continued inflammation (CRP 27 mg/l) and eosinophilia (1500/mm3). Anti-MPO antibodies rated 6.6 U/ml. On August 2013, after two cycles of cyclophosphamide, he presented with general signs, myalgia, eosinophilic count at 1400/mm3 and CRP at 52 mg/l. Prednisolone was increased to 80 mg/d. Blood arterial pressure remained in the normal range.
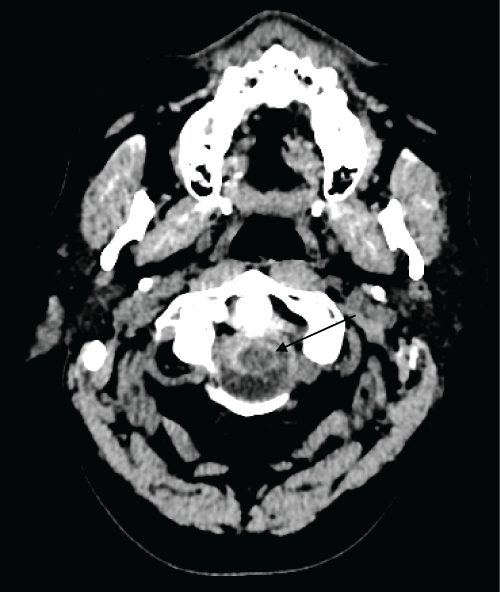
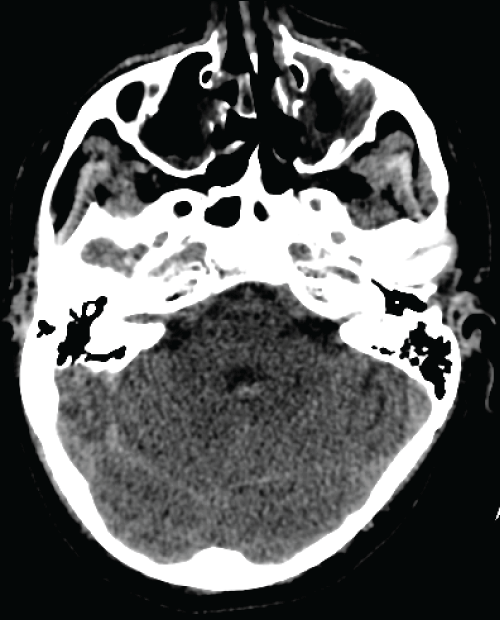
Two days after, he was admitted through Emergency room with sudden cervical rachialgia which appeared during effort (cycling). Clinical examination founded a meningeal syndrome without fever. Blood arterial pressure was 140/110 mmHg. CT-scan revealed a peri-bulbar haemorrhage and intraventricular hemorrhage of the 4th ventricle (Figure 1 and Figure 2). Eosinophilic count was 3330/mm3 and CRP rose at 40 mg/l, but ANCA and anti-MPO antibodies were negative. Other biological parameters were in normal range. A treatment with Nimodipine was started in neurosurgery department.
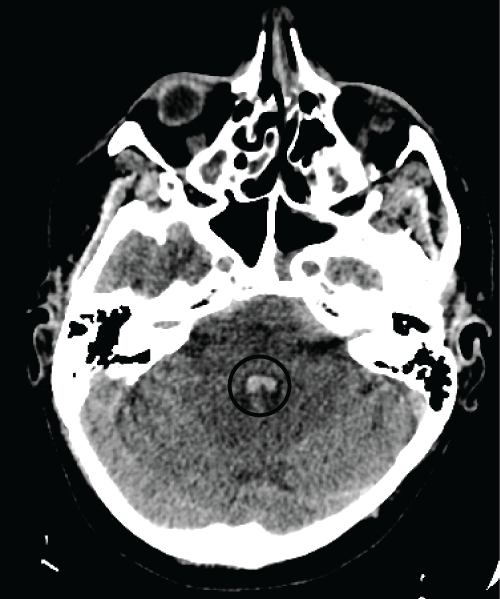
.
Figure 2: Cerebral CT-scan at day 0 : intraventricular (4th ventricle) haemorrhage.
View Figure 2
Arteriography showed no aneurysm or cerebral or spinal arteriovenous malformation. The association of past history, eosinophilic count, and absence of cardiovascular risk factor supported the assumption of a vasculitis flare. Cyclophosphamide 1 g and Methylprednisolone 3 × 500 mg were then infused (days 3-5). At day 5, cerebral CT-scan showed regression of the SAH (Figure 3), CRP was 14 mg/l and eosinophilic count 140/mm3. Clinical recovery was complete. Angio-MRI at month 3 confirmed the absence of any vascular malformation. Further treatment included intraveinous cyclophosphamide every three weeks for a total of 11i, and then maintenance with methotrexate and prednisone in decreasing doses. On April 2015, complete remission is still observed.
Discussion
EGPA is a rare primary vasculitis involving small calibre vessels. The prevalence is 11 cases per million inhabitants. Incidence is maximal from 30 to 50 years. Neurological manifestations are most commonly multinevritis (63 - 78%), especially peroneal nerves, with a good prognosis. Central neurologic involvement is much rarer (8%), appears early in the course of the disease, is associated with positive ANCA, and bares a poor prognosis. Non specific symptoms (i.e., headaches, behaviour troubles) and acute vascular accidents (commonly ischemic) are described.
Only seventeen cases of central nervous haemorrhages have been reported [1-5]: 9 SAH, 10 intracerebral haemorrhages. Both were associated in 2 cases. Two patients died (13%), 5 had sequel (26%) and 10 remitted. The two patients who died had not been treated with cyclophosphamide, but full remission was obtained with steroids alone in 4/8, and with Steroids + Cyclophosphamide in 5/9. Radio-embolization was associated in some cases.
Our observation suggests that SAH occurs when the disease is still active. This is consistent with other case reports. EGPA may be already diagnosed but not controlled or may be revealed by an acute neurologic manifestation as in seven (41%) reported cases. Cerebral arteriography is generally abnormal (six of nine SAH cases reported) and shows artery calibre disparities or dissections. It can be normal without excluding diagnosis like in our patient.
Current treatment recommendations include methylprednisone 15 mg/kg/d for 3 days followed with oral prednisone 1 mg/kg/d for 3 weeks before tapering, and monthly cyclophosphamide 500 -750 mg/m2. It may be noted that the revised FFS does not mention neurological involvement.
Conclusion
In the general population, 80% of SAH are due to aneurysm ruptures and 15% remain idiopathic. In the latter, general signs (i.e., fever, arthromyalgia) or biological abnormalities (i.e., inflammatory syndrome) may be consistent with systemic vasculitis.
References
-
Go MH, Park JU, Kang JG, Lim YC (2012) Subarachnoid and intracerebral hemorrhage in patients with churg-strauss syndrome: two case reports. J Cerebrovasc Endovasc Neurosurg 14: 255-261.
-
Menditto VG, Di Rienzo A, De Nicola M, Balzano L, Polonara S (2013) Subarachnoid hemorrhage from ICA aneurysm rupture in a Churg-Strauss patient: A case report and a review of the litterature. Clin Neurol Neurosurg 115: 197-199.
-
Diamanti L, Berzero G, Bini P, Ravaglia S, Rognone E, et al. (2014) Spinal hemorrhage in eosinophilic granulomatosis with polyangiitis (Churg-Strauss). J Neurol 261: 438-440.
-
Murthy SB, Khalaf N, Shah S, Ma B, Goldsmith CE, et al. (2013) Churg-Strauss syndrome: an uncommon cause of intracerebral hemorrhage. JAMA Neurol 70: 1580-1581.
-
Taormina G, Andolina G, Banco MA, Costanza-Gaglio EJ, Bonura A, et al. (2014) An uncommon presentation of eosinophilic granulomatosis with polyangiitis: a case report. J Med Case Rep 8: 190.