Clinical Medical
Reviews and Case Reports
Intercostal Lung Hernia: A Case for Conservative Treatment
Edupuganti Mohan Mallikarjuna Rao*, Sarah Patterson Mitchell, Janina Fordyce and Vyjayanthi Ganga
College of Health Professions, University of Arkansas for Medical Sciences, USA
*Corresponding author:
Edupuganti Mohan Mallikarjuna Rao, Radiologist Assistant Program, College of Health Professions, University of Arkansas for Medical Sciences, 4301 West Markham St. Little Rock, AR 72205, USA, Tel: 501-686-7438, E-mail: mmedupuganti@gmail.com
Clin Med Rev Case Rep, CMRCR-2-038, (Volume 2, Issue 6), Case Report; ISSN: 2378-3656
Received: April 20, 2015 | Accepted: June 23, 2015 | Published: June 26, 2015
Citation: Rao EMM, Mitchell SP, Fordyce J, Ganga V (2015) Intercostal Lung Hernia: A Case for Conservative Treatment. Clin Med Rev Case Rep 2:038. 10.23937/2378-3656/1410038
Copyright: © 2015 Rao EMM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Lung herniation, defined as the protrusion of the lung beyond the thorax, is rarely encountered in the clinical setting. Most pulmonary hernias are caused by congenital defects and thoracic trauma. Spontaneous hernias are uncommon. We present a 70 year old patient with spontaneous intercostal lung herniation following a bout of bronchitis and several days of vigorous coughing. We highlight the pitfalls in establishing a diagnosing, present the outcome with conservative management, review the literature and outline the types, causes, incidence, and treatment options.
Keywords
Lung hernia, Intercostal hernia, Valsalva maneuver, Reducible hernia, Spontaneous hernia, Chest wall mass, Vigorous cough
Introduction
A portion of the lung herniating through the chest wall can be alarming and is commonly misdiagnosed. The case is important for several reasons, firstly the condition should be considered in the appropriate clinical circumstance as it carries a potential for adverse outcomes, secondly establishing a diagnosis can be difficult as an initial radiographic examination can be misleadingly normal and requires specialized maneuvers to establish a diagnosis. Finally knowledge of the natural history is essential to avoid unnecessary, potentially harmful invasive management option. The case demonstrates the importance of Computed Tomographic Examination (CT) with Valsalva maneuvers in clarifying the diagnosis and highlights the importance of conservative management and periodic surveillance once a diagnosis is established.
We review the literature and summarize the types of lung hernia, the diagnostic approach and the available management options. Given the rarity of the condition there is a lack of consensus on the best management approach and clinicians continue to rely on published reports and expert opinion when faced with this condition.
Case Presentation
A 72- year- old white male presented to his primary physician with pleuritic chest pain after a cough that lasted one week. He was well until a week ago following which he developed a cough productive of mucopurulent sputum. The cough subsided spontaneously followed by the onset of a pleuritic right chest pain. There was no significant past medical or surgical history and no history of smoking.
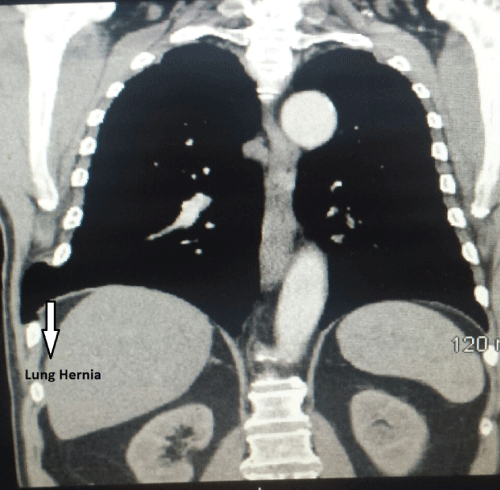
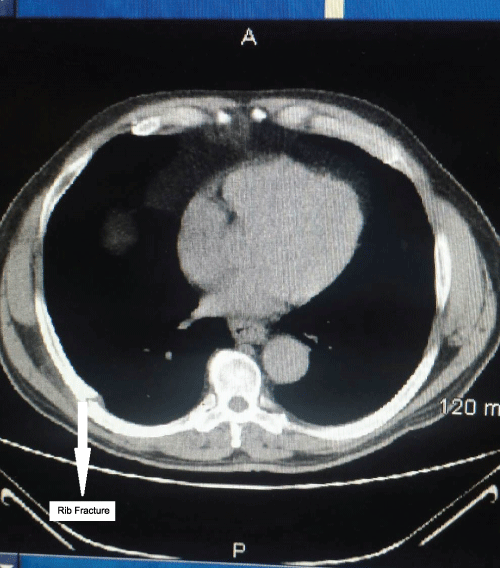
The examination was significant for localized tenderness over the right posterolateral chest wall overlying an ill circumscribed soft mass measuring 4 cm x 4cm. It was non tender, soft in consistency and easily reducible. No abnormalities were detected on a postero anterior chest radiographic examination. Lung herniation was suspected and a computed tomographic examination with Valsalva maneuver was requested. Imaging utilizing Computed Tomographic Scanning (CT), with and without contrast, showed an intercostal lung herniation and an 8th rib fracture (Figure 1,2).
.
Figure 1: Cross sectional computed tomographic scan (Bone window) showing rib fracture.
View Figure 1
Treatment and Outcome
The hernia was small in size and the neck was wide, the risk of strangulation was small and a decision was made to treat conservatively and follow the patient clinically with serial examination. The patient was instructed to follow up if the mass enlarged in size or became painful. The pain was mild to moderate and the patient was instructed to use over the counter pain medications for symptomatic management. At sixth month follow up the patient stated that his chest pain had resolved completely and there were no evidence of chest wall mass. A repeat chest radiograph showed no evidence of recurrence.
Discussion
Types of lung hernia
Lung herniation is defined as the protrusion of the lung beyond the thorax. It is a rare entity with a variety of presentations including dyspnea, chest wall pain and as a visible or palpable chest or neck bulge. In some cases pulmonary hernias can be asymptomatic. Lung hernias are classified by their anatomic locations and the mechanism of origin. These hernias can be described as cervical, intercostal, or diaphragmatic. Each of these types can be either congenital or acquired [1,2]. Acquired hernias can be spontaneous, traumatic, iatrogenic, or pathologic as a result of a neoplasm or inflammatory process. Only a few cases have been described in the current literature [3,4], it is an important condition for primary physicians, radiologists, emergency room physicians, and pulmonologists to consider in the appropriate clinical setting.
Cervical lung hernias account for approximately 35% of all pulmonary hernias [5]. Cervical hernias present when portions of the lung protrude through the anterior region of the thoracic inlet between the scalenus anterior and sternocleidomastoid muscles. They are most often encountered in elderly patient with a history of emphysema and weakened cervical fascia. Intercostal lung hernia's account for around 60-80% of lung hernias [5], resulted from a protrusion of lung tissue through a weakened area in the chest wall between the ribs. This weakening could be due to trauma and can present immediately or even years after the event. Diaphragmatic lung hernias are uncommon.
The rare abdominal intercostal hernia is related to the intercostal thoracic lung hernia. There are very few case reports of this condition in the literature [6]. This occurs when contents of the abdomen protrude through a weakening in the intercostal space. These contents could include liver, large or small bowel and stomach [7]. While this phenomenon is uncommon it is important to include the condition in the differential diagnosis of a chest wall mass.
Role of imaging
Imaging is the cornerstone for establishing a diagnosis. While these hernias can be visualized on plain radiographs computed tomographic imaging is required to determine the location, extent, identify the contents and look for associated conditions such as rib fractures. The most common abnormality on a plain radiograph is a focal lucency adjacent to the lung; CT demonstrates a protrusion of lung tissue through the chest wall [8]. When initial examination is completely normal additional imaging should be performed with valsalva, inspiration and expiration. Additional views such as oblique images can also aid in the diagnosis. There may be a role for ultrasound in the absence of computed tomography [1,3]. D reconstruction of the computed tomographic image becomes important when surgery is planned.
Treatment options and prognosis
A conservative approach to management is reasonable in most patients in the absence of complicating factors such as strangulation, bleeding or the presence of other visceral contents [9]. However the presence of any of the above complications calls for immediate reduction and closure of the defect [2]. Respiratory distress and enlarging size are also indications for surgical intervention.
Choe et al. emphasizes the importance of follow up imaging in a case report and presents a patient who presented with a mild intercostal lung hernia for which a conservative plan of management was chosen [4]. After 3 months of conservative treatment there was an enlargement of the mass requiring repeat imaging. The transthoracic hernia was complicated by the inclusion of abdominal contents including sub diaphragmatic fat and the hepatic flexure of the colon necessitating emergent surgery, thus highlighting the rationale for follow up imaging in patients.
The options for surgical intervention are several and include wires, soft synthetic patches, judet and sliding staples [3,10]. Soft prosthetic patches have less restriction on the normal mechanics of the thorax when compared to more rigid implants. Bio-prosthetic implants reduce the risk of infection [3,10].
While there is a consensus on how to diagnose the condition there is no uniform criteria for management. Given the rarity of the condition it is unlikely that this will be ever answered with an evidence based approach and we will have to rely on expert opinion for the foreseeable future.
Conclusion
Intercostal lung hernia is an extremely rare disorder in which part of the lung contents herniate through the chest wall. Although lung hernias are rare and usually benign in nature there is a real potential for complications and it is important for physicians to be educated about this condition. Knowledge of the benign nature of lung hernias provides reassurance and avoids unnecessary imaging and invasive procedures.
References
-
Morel-Lavallée (1847) Hernies du poumon. Bull Soc Chir Paris 1: 195.
-
Detorakis EE, Androulidakis E (2014) Intercostal lung herniation--the role of imaging. J Radiol Case Rep.8: 16-24.
-
Mirza A, Gogna R, Kumaran M, Malik M, Martin-ucar A (2011) The surgical management of intercostal lung herniation using bioprosthesis. J Surg Case Rep 1: 6.
-
Choe CH, Kahler JJ ( 2014) Herniation of the lung: a case report. J Emerg Med 46:28-30.
-
Hiscoe DB, Digman GJ (1955) Types and incidence of lung hernias. J Thorac Surg 30: 335-342.
-
Connery A, Mutvalli E (2010) Cough-induced abdominal intercostal hernia. JRSM Short Rep 1: 23.
-
Abunnaja S, Chysna K, Shaikh I, Tripodi G (2014) Acquired abdominal intercostal hernia: a case report and literature review. Case Rep Surg 456053.
-
Zia Z, Bashir O, Ramjas GE, Kumaran M, Pollock JG, Pointon K (2014) Intercostal lung hernia: radiographic and MDCT findings. ClinRadiol 68: e412-417.
-
Bikhchandani J, Balters MW, Sugimoto JT (2012) Conservative management of traumatic lung hernia. Ann Thorac Surg 93: 992-994.
-
Fiscon V, Portale G, Frigo F, Migliorini G (2009) Thoracoscopic repair of lung herniation following minimally invasive cardiothoracic surgery Chir Ital 61: 261-263.