Clinical Medical
Reviews and Case Reports
Giant Cell Arteritis of the Lower Limb Presenting as Peripheral Arterial Disease and Mantle Cell Lymphoma Two Years Later
Sophia Corsava1*, Savvas Psarelis1,2 and Elena Nikiphorou3
1St. George's University of London Medical School, UK
2Rheumatology Department, Nicosia General Hospital, Nicosia, Cyprus
3Rheumatology Department, Cambridge University Hospitals Foundation Trust, UK
*Corresponding author:
Sophia Corsava, St. George's Medical School London UK, Cranmer Terrace, SW17 0RE, London, UK, Tel: +44 (0)20 8672 9944, E-mail: sophiadr@live.com
Clin Med Rev Case Rep, CMRCR-2-034, (Volume 2, Issue 6), Letter to the Editor; ISSN: 2378-3656
Received: May 22, 2015 | Accepted: June 06, 2015 | Published: June 09, 2015
Citation: Corsava S, Psarelis S, Nikiphorou E (2015) Giant Cell Arteritis of the Lower Limb Presenting as Peripheral Arterial Disease and Mantle Cell Lymphoma Two Years Later. Clin Med Rev Case Rep 2:034. 10.23937/2378-3656/1410034
Copyright: © 2015 Corsava S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Letter to the Editor
Sir, A 55-year-old man with a two-year history of peripheral arterial disease (PAD) was urgently referred to rheumatology via the vascular clinic. He was scheduled for a balloon-angioplasty due to bilateral aortoiliac and femoro-popliteal disease and occlusion of the iliac arteries. His past medical history included stent re-vascularisation of the left external iliac artery, endarterectomy of both right common superficial and deep femoral arteries and a polytetrafluroethylene patch (PTFE) graft.
The standard pre-operational check showed a significantly raised White Blood Cell count (30,000/mcL). Clinical examination revealed intermittent lower-limb and jaw claudication bilaterally with ischaemic rest-pain (Fontaine Classification 3), absence of the right radial pulse and a pulseless right temporary artery. Blood pressure difference between the left and right upper limbs was 20mm Hg. Full blood Count, a right temporal artery biopsy, a myelogram, CT-chest and abdomen, and a magnetic resonance angiography of the aorta (MRA) were ordered. In addition ESR and CRP were also ordered. Of note CRP was 3,15mg/L. The autoimmune profiles for rheumatoid arthritis, systemic lupus erythematosus, systemic sclerosis, granulomatosis with polyangiitis and eosinophilic granulomatosis with polyangiitis were negative. The temporal artery biopsy showed positive B-indices (a measure for monoclonal gammopathies) and was negative with CD5 and cyclin-D1 stains. The CD34 staining showed small thin trichoid vessels. There were no biopsy features suggestive of Giant Cell Arteritis (GCA) at that point.
The CSF analysis following the myelogram revealed 20% lymphocytes of medium-size consistent with hyperplastic lymphoid leukaemia. The bone marrow biopsy showed red bone marrow with B-cell lymphocytosis of non-specific immunological phenotype. The immunophenotype findings were suggestive of Mantle Cell Lymphoma (MCL). There were multiple enlarged lymph nodes on CT of the abdomen (Figure 1); CT-chest was unremarkable.
.
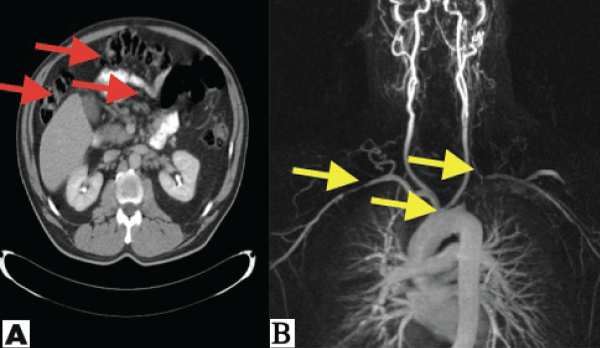
Figure 1: A) CT abdomen with multiple enlarged lymph nodes (red arrows), B) The MRA of the thoracic aorta revealed stenosis of the right subclavian, spinal and of the origin of the left subclavian arteries (yellow arrows).
View Figure 1
Samples from the abdominal aorta, the femoral artery, para-aortic and inguinal lymph nodes were taken for biopsy at the time of balloon-angioplasty following the request of the rheumatology consultant due to the patient's history. These came back positive for GCA. The aorta and femoral arteries sections showed chronic focal inflammation, with giant cells consistent with Giant Cell Arteritis and some minor lymphocyte infiltration. The lymph node biopsy firmly confirmed MCL with immunophenotypes of CD20+, CD79a+, CD3-, CD5+, CD43+, CD10-, bcl2+, bcl6-, CyclinD1-, CD23-, ZAP70>20%, CD38-.
The patient was treated with oral methylprednisolone 40mg once daily, with regular weekly follow-ups. Treatment was withheld for MCL by the haematology-oncologists at this stage, but the patient was scheduled for CHOP chemotherapy (cyclophosphamide, doxorubicin, vincristine, prednisone), as soon as he was able following recovery from his operation [1].
A month later the patient was acutely admitted due to severe angina symptoms and was consented for percutaneous coronary intervention (PCI) catheterisation. The PCI revealed triple-vessel-disease which necessitated surgery. Sadly, the patient died on the operating table.
This report highlights two key-messages. Firstly, it underlines the importance of routinely screening patients with GCA for vascular complications [2-4]. GCA has a well-documented involvement of large arteries; however the cardiovascular risk has not yet been well studied or understood. A review of 3408 GCA patients in 2014 [3] revealed the impact of GCA on cardiovascular and cerebrovascular incidents. These patients had significant incidence of Myocardial Infractions, PAD and Cerebrovascular Incidents. Secondly, emphasizes the need for high vigilance and screening for underlying malignancy especially in atypical presentations [5]. Secondly, emphasizes the need for high vigilance and screening for underlying malignancy especially in atypical presentations. The evidence is conflicting, with some studies reporting that GCA patients do not have increased risk of malignancy and others reporting on GCA preceding malignancy or malignancy preceding GCA. However a recent meta-analysis by Ungprasert et al, shows a low but significant risk of malignancies for these patients [6].
We report the case of a patient with GCA of the lower limbs manifesting as PAD at multiple sites, triple coronary vessel disease and mantle cell lymphoma. There were no clinical manifestations of malignancy until 2 years later. Screening patients presenting with early, recurrent severe PAD for underlying inflammatory vascular conditions such as GCA or other vasculitides should be considered, as well as screening for underlying malignancy.
References
-
Dreyling M, Geisler C, Hermine O, Kluin-Nelemans HC, Le Gouill S, et al. (2014) Newly diagnosed and relapsed mantle cell lymphoma: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol 25 Suppl 3: 83-92.
-
Assie C, Janvresse A, Plissonnier D, Levesque H, Marie I (2011) Long-term follow-up of upper and lower extremity vasculitis related to giant cell arteritis: a series of 36 patients. Medicine (Baltimore) 90: 40-51.
-
Tomasson G, Peloquin C, Mohammad A, Love TJ, Zhang Y, et al. (2014) Risk for cardiovascular disease early and late after a diagnosis of giant-cell arteritis: a cohort study. Ann Intern Med 160: 73-80.
-
Boettinger M, Sebastian S, Gamulescu MA, Grauer O, Ritzka M, et al. (2009) Bilateral vertebral artery occlusion with retrograde basilary flow in three cases of giant cell arteritis. BMJ Case Rep 2009.
-
Turesson C, Matteson EL (2013) Malignancy as a comorbidity in rheumatic diseases. Rheumatology (Oxford) 52: 5-14.
-
Ungprasert P, Sanguankeo A, Upala S, Knight EL (2014) Risk of malignancy in patients with giant cell arteritis and polymyalgia rheumatica: a systematic review and meta-analysis. Semin Arthritis Rheum 44: 366-370.





