Clinical Medical
Reviews and Case Reports
The Contribution of Susceptibility-weighted Imaging (SWI) in Occult Cerebral Vascular Malformations in Pediatric Patients
Neslin Sahin*, Aynur Solak and Liya Alkilic
Department of Radiology, Sifa University School of Medicine, Turkey
*Corresponding author:
Neslin Sahin, Department of Radiology, Sifa University School of Medicine, Fevzipasa Boulevard No. 172/2, 35240, Basmane Izmir, Turkey, Tel: +90-232-343-44-45, Fax : +90-232-343-56-56, E-mail: neslinshn@gmail.com
Clin Med Rev Case Rep, CMRCR-2-032, (Volume 2, Issue 5), Case Report; ISSN: 2378-3656
Received: February 16, 2015 | Accepted: May 24, 2015 | Published: May 26, 2015
Citation: Sahin N, Solak A, Alkilic L (2015) The Contribution of Susceptibility-weighted Imaging (SWI) in Occult Cerebral Vascular Malformations in Pediatric Patients. Clin Med Rev Case Rep 2:032. 10.23937/2378-3656/1410032
Copyright: © 2015 Sahin N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Occult cerebral vascular malformations (CVM) include cerebral cavernous malformations (CCM), developmental venous anomalies, and cerebral capillary telangiectasias (CCT). Conventional magnetic resonance imaging (MRI) has low sensitivity in visualizing these angiographically invisible low-flow vascular lesions. Susceptibility-weighted imaging (SWI), a novel high spatial resolution gradient-echo MRI sequence with both phase and magnitude information, is exquisitely sensitive to blood products and small venous structures. In this article, we illustrated atypical presentations of occult CVMs in pediatric patients; familial CCM as a rare cause of headache and CCT mimicking malignancy in the basal ganglia and discussed the contribution of SWI in the diagnosis through case reports.
Keywords
Capillary telengiectasia, Cavernous malformation, Gradient-echo, Susceptibility-weighted imaging
Introduction
Occult Cerebral Vascular Malformations (CVM) includes cerebral cavernous malformations (CCM), developmental venous anomalies, and cerebral capillary telangiectasias (CCT) [1]. These low-flow vascular lesions have been referred to as "occult," because they are frequently invisible on conventional angiography in contrast to high-flow arteriovenous malformations. Conventional magnetic resonance imaging (MRI) also has low sensitivity in visualizing small low-flow vessels of occult CVMs. Furthermore, small CVMs can be missed because of partial volume effects.
Susceptibility-weighted imaging (SWI) is a novel, high spatial resolution, three-dimensional fully velocity compensated gradient-echo (GE) MRI sequence with an additional phase post-processing [2-4]. SWI is exquisitely sensitive to the susceptibility differences of various substances, including blood, blood products, non-heme iron, and calcification. This technique allows high-resolution depiction of blood products and small venous structures. Therefore, SWI can essentially be helpful to identify and characterize occult CVMs in addition to several potential clinical applications reviewed in adult [2] and pediatric patients [3,4]. T2*-weighted GE sequences with small voxel sizes are effective to reveal small vascular structures, however SWI with both phase and magnitude information improves sensitivity in detecting small vessels that are not visible on conventional MRI [2-5]. Lee et al. [5] reported SWI as the ideal technique for patients with a high clinical suspicion of occult vascular malformations.
The purpose of this article is to illustrate atypical presentations of CCT and CCM in pediatric patients and discuss the contribution of SWI in the diagnosis through case reports.
Case 1
Familial cerebral cavernous malformation as a rare cause of headache
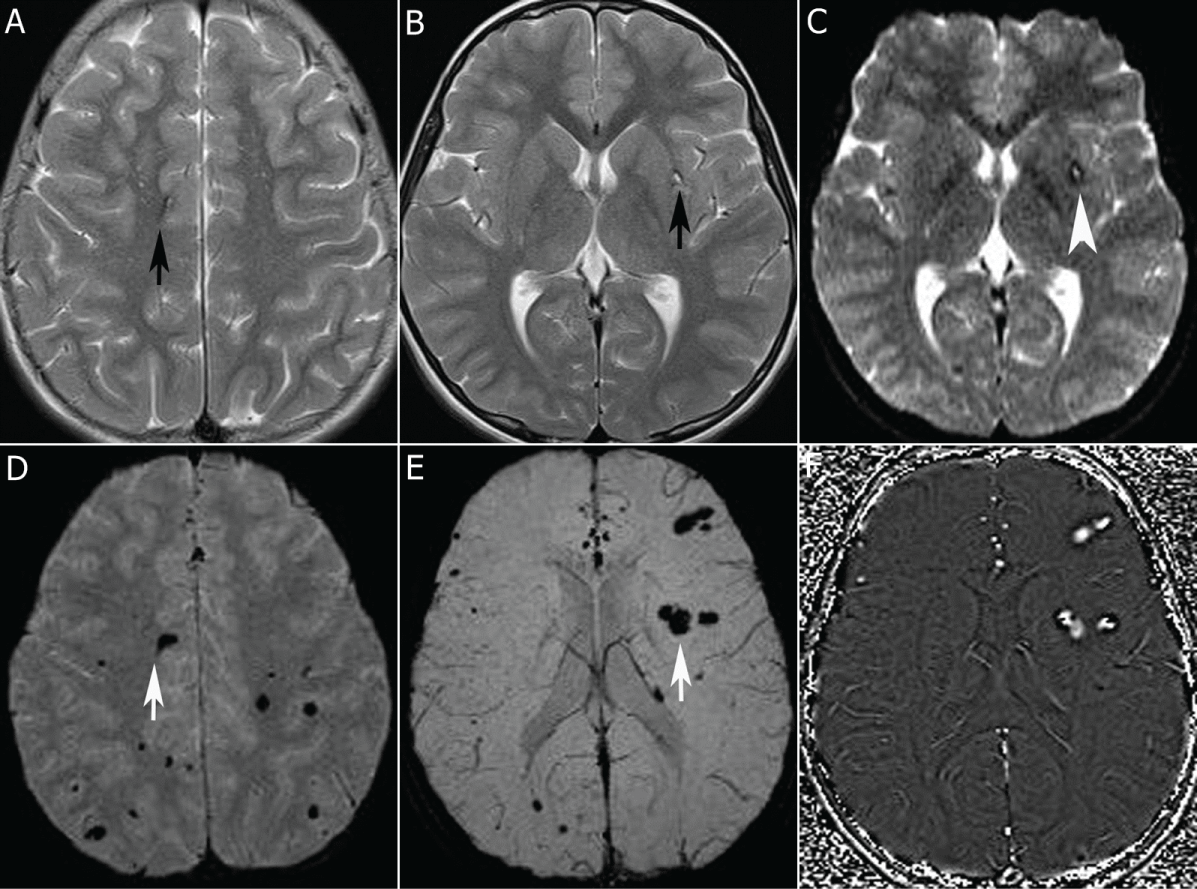
A 12-year-oldgirl presented with a headache increasing in severity over days, fatigue, and confusion since one day ago. The neurologic examination was normal. A cranial MRI showed millimetric hypointense signal intensity changes, one in the right hemisphere and a few in the left hemisphere, on T2-weighted images (Figure 1A). In addition, there was a 10 mm lesion with central hyper intensity and peripheral hypointensity in the left lentiform nucleus on T2-weighted images (Figure 1B). T2*-weighted GE images revealed these lesions as more prominent hypointense signal changes and demonstrated a few more lesions (Figure 1C). On an SWI minimal intensity projection (minIP, Figure 1D,1E), these lesions were hypointense, and they were hyperintense on SWI phase images (Figure 1F), similar to veins. In addition, there were multiple similar small hypointense lesions in both cerebral hemispheres and two lesions in the left cerebellar hemisphere on SWI minIP images. The final diagnosis was familial CCM.
.
Figure 1: 12-year-old girl with familial cerebral cavernous malformation A, B. T2-weighted images show millimetric hypointense signal intensity change in the right subcortical white matter (A, black arrow) and a lesion with central hyperintensity and peripheral hypointensity in the left lentiform nucleus (B, black arrow) which reveals more prominent peripheral hypointensity on T2*-weighted GE image (C, white arrowhead). D, E. SWI minimal intensity projection (minIP) images show multiple small hypointense lesions in both cerebral hemispheres in addition to these lesions (white arrows). F. The lesions are hyperintense on SWI phase images similar to veins.
View Figure 1
CCMs compose 10-20% of all CVMs with an estimated prevalence between 0.4% and 0.8% in children [2-4] . They can occur in sporadic form with a solitary lesion or in autosomal dominant familial form with multiple lesions [6,7]. The familial form represents 10-30% of CCMs [7]. These malformations are often discovered as incidental findings, but commonly present with focal neurological deficits, seizures, severe headache, and recurrent intracranial hemorrhages.
CCM is composed of a mass with thin, varying sizes of single-layered blood vessels and characteristic thrombi of varying age within these vessels [1]. The MRI findings of CCMs are variable, depending on the presence of hemorrhage and calcifications [2,3,6]. Lesions that have previously bled can be easily identified by a characteristic "popcorn-like" appearance due to the mixed-signal intensities, with a central hyperintense reticulated core and a surrounding peripheral hypointense rim of hemosiderin on T2-weighted sequences. In contrast, small CCMs that are intact with no bleeding may be not visible or may demonstrate a faint contrast enhancement, which is often nonspecific.
SWI is exquisitely sensitive to the susceptibility changes caused by intralesional blood products [2-4]. Therefore, CCMs appear very dark on the SWI images, as shown in our patient with multiple cavernomas in Figure 1D,1E. It should be considered likely that the lesions are proportionally larger on SWI than in actual sizes due to artifactually enhanced "blooming" artifacts of hemorrhages on GE sequences.
Recent studies have suggested that SWI was more accurate than T2-weighted and T2*-GE sequences in evaluating the number of CCMs [2,4,6,7]. A study by de Souza et al. [6] included 15 patients with familial CCMs who showed improved sensitivity to SWI in identifying the number of CCMs when compared to T2-weighted fast spin-echo and GE sequences.
In this case, we presented the contribution of SWI in the diagnosis of familial CCM, which is characterized by the presence of multiple lesions. 50-84% of patients with the familial form presented with multiple CCMs (mean 5.8-6.5 lesions) [6]. Small, intact CCMs that have not bled are usually undetectable by conventional MRI. SWI sequence can detect more CCMs than routine MRI sequences, thus differentiating familial forms that should be referred to genetic evaluation from sporadic forms. Therefore, in the presence of a CCM, we propose integrating SWI to MRI protocol in order to accurately identify the prevalence of CCMs, particularly for follow-up imaging of the familial forms, which are especially high risk for bleeding, developing de novo lesions, and increasing in size. In addition, SWI can also be helpful for detecting CCM in cases of atypical intracerebral hemorrhageor "cryptogenic" epilepsy.
Case 2
Cerebral capillary telengiectasia mimicking malignancy in the basal ganglia
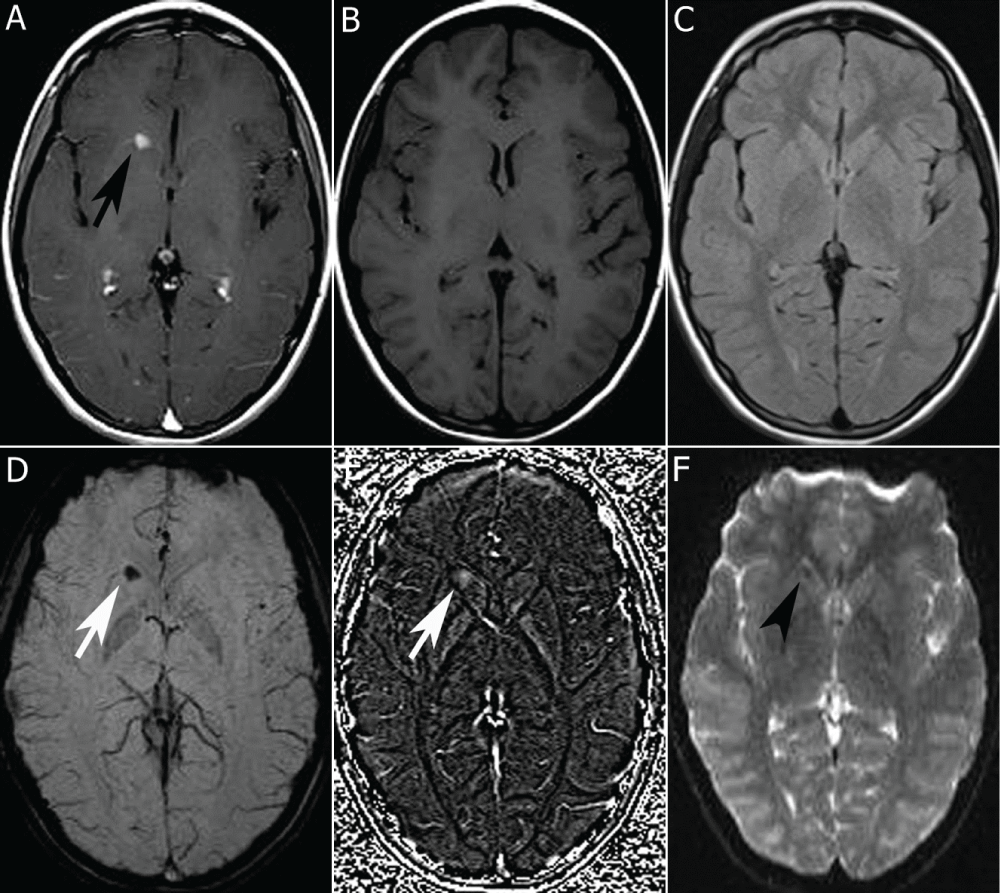
A 12-year-oldgirl had an MRI examination at an outside hospital because of numbness in her right hand. Her complaints lasted for a week, reporting decreasing severity over several days and never repeated again. The patient was had a follow-up by the oncology department at an outside hospital with an initial diagnosis of a glial tumor for 1 year. On the last MRI exam performed by our department, there was a nodular 6 mm contrast enhancement in the head of caudate nucleus without any signal intensity changes on T1-weighted, T2-weighted, and FLAIR sequences (Figure 2A-2C). The lesion was hypointense on SWI minIP (Figure 2D), and hyperintense on SWI phase images (Figure 2E), similar to vessels. The T2*-GE image showed a moderate hypointense signal in the head of the caudate nucleus (Figure 2F). There was no interval change in the lesion on four separate MRI exams in a year. The findings were mostly compatible with capillary telangiectasia, and no intervention was thought for histopathological diagnosis.
.
Figure 2: 12-year-old girl with cerebral capillary telangiectasia. Contrast-enhanced T1-weighted image (A) shows a nodular 6mm contrast enhancement in the head of caudate nucleus (black arrow) without any signal intensity changes on nonenhanced T1-weighted (B) and FLAIR (C) images. The lesion was hypointense on SWI minIP (D, white arrow), and hyperintense on SWI phase images (E, white arrow), similar to vessels. F. The lesion was less hypointense on T2*-GE image (black arrowhead).
View Figure 2
CCTs are clinically benign, small occult CVMs varying in size from a few millimeters to about 2cm [1,8,9]. They are commonly located in the brain stem and rarely reported in children. CCTs are smaller and less common than cavernomas and can also occur as transitional malformations, such as mixed cavernoma/telangiectasia lesions. These sporadic malformations alone may rarely be symptomatic, and symptoms with hemorrhage most likely arise from associated vascular malformations. More extensive lesions associated with syndromes (e.g. hereditary hemorrhagic telangiectasia) or radiation-induced vascular injury may present with subtle neurologic symptoms; however, they may not be identified with conventional imaging [10].
The vast majority of CCTs are almost always managed conservatively, because they consist of small capillaries separated by normal brain parenchyma and are commonly located in the pons [1,9]. An MRI is valuable in providing a diagnosis, as histopathological diagnosis is usually not available [9,11]. On an MRI, isointensity on T1- and isointensity or slightly increased signal intensity on T2-weighted images with a lack of mass effect are commonly shown. The combination of postcontrast enhancement and hypointense appearance on T2*-GE sequences or SWI has been found to be highly specific radiological findings and usually do not require histopathological correlation. CCTs commonly lack calcification and hemorrhage, suggesting that signal intensity loss on T2*-weighted images are related to the presence of deoxyhemoglobin in slow-flowing blood through dilated capillaries. Previous studies reported that SWI could demonstrate small BCTs that were not visible on T2*-GE images [8,9]. In this patient, the T2*-GE sequence revealed the lesion but less prominently than on SWI.
We presented a case of an unusually located presumed capillary telangiectasia involving the basal ganglia in a child mimicking malignancy in which the imaging features of the lesion were identical to those described for capillary telangiectasias of the brain stem. It should be noted that CCTs are usually invisible on conventional MRI sequences, as in this case. These malformations are characteristically benign entities, but they may be overlooked in patients presenting with symptoms such as seizures on conventional MRI. Furthermore, CCTs may mimic subacute ischemia or inflamatory disease and, more importantly, malignancy due to focal contrast enhancement, particularly in less typical locations than the brain stem. This makes an accurate imaging diagnosis extremely important. In such cases, the SWI sequence enables the diagnosis by showing slow vascular flow as a signal-intensity loss in an enhancing focal brain lesion.
Lesions with typical imaging findings of CCT, but in atypical locations other than the brain stem, can be followed, and in the absence of an interval change, the diagnosis of capillary telangiectasia can be suggested.
Conclusion
SWI is a novel MRI sequence with high sensitivity for blood and blood products. This technique can demonstrate occult CVMs by increasing the visibility of small vascular structures which may be undetectable by conventional MR sequences. Therefore, we propose to integrate SWI in the imaging protocols of patients with a high clinical suspicion of occult CVMs.
References
-
Dillon WP (1997) Cryptic vascular malformations: controversies in terminology, diagnosis, pathophysiology, and treatment. AJNR Am J Neuroradiol 18: 1839-1846.
-
Mittal S, Wu Z, Neelavalli J, Haacke EM (2009) Susceptibility-weighted imaging: technical aspects and clinical applications, part 2. AJNR Am J Neuroradiol 30: 232-252.
-
Tong KA, Ashwal S, Obenaus A, Nickerson JP, Kido D, et al. (2008) Susceptibility-weighted MR imaging: a review of clinical applications in children. AJNR Am J Neuroradiol 29: 9-17.
-
Bosemani T, Poretti A, Huisman TA (2014) Susceptibility-weighted imaging in pediatric neuroimaging. J Magn Reson Imaging 40: 530-544.
-
Lee BC, Vo KD, Kido DK, Mukherjee P, Reichenbach J, et al. (1999) MR high-resolution blood oxygenation level-dependent venography of occult (low-flow) vascular lesions. AJNR Am J Neuroradiol 20: 1239-1242.
-
de Souza JM, Domingues RC, Cruz LC Jr, Domingues FS, Iasbeck T, et al. (2008) Susceptibility-weighted imaging for the evaluation of patients with familial cerebral cavernous malformations: a comparison with t2-weighted fast spin-echo and gradient-echo sequences. AJNR Am J Neuroradiol 29: 154-158.
-
de Champfleur NM, Langlois C, Ankenbrandt WJ, Le Bars E, Leroy MA, et al. (2011) Magnetic resonance imaging evaluation of cerebral cavernous malformations with susceptibility-weighted imaging. Neurosurgery 68: 641-647.
-
El-Koussy M, Schroth G, Gralla J, Brekenfeld C, Andres RH, et al. (2012) Susceptibility-weighted MR imaging for diagnosis of capillary telangiectasia of the brain. AJNR Am J Neuroradiol 33: 715-720.
-
Gross BA, Puri AS, Popp AJ, Du R (2013) Cerebral capillary telangiectasias: a meta-analysis and review of the literature. Neurosurg Rev 36: 187-193.
-
Tsui YK, Tsai FY, Hasso AN, Greensite F, Nguyen BV (2009) Susceptibility-weighted imaging for differential diagnosis of cerebral vascular pathology: a pictorial review. J Neurol Sci 287: 7-16.
-
Sayama CM, Osborn AG, Chin SS, Couldwell WT (2010) Capillary telangiectasias: clinical, radiographic, and histopathological features. Clinical article. J Neurosurg 113: 709-714.





