Clinical Medical Reviews and Case Reports
Cerebellar Stroke in Children, Case report from Qatar & Brief Literature Review
Abdulhafeez M Khair* , Mahmoud Elseid, Khalid Mohamed, Rana Al-shami, Khalid Ibrahim and Ahmed Elsotouhy
Section of Pediatric Neurology, Hamad medical Corporation, Qatara
*Corresponding author: Abdulhafeez Mohamed Khair, Specialist & Clinical Fellow, Section of Pediatric Neurology, Hamad medical Corporation, P.O. Box: 3050, Doha, Qatar, E-mail: drabboody@hotmail.com
Clin Med Rev Case Rep, CMRCR-1-005, (Volume 1, Issue 1), Case Report; ISSN: 2378-3656
Received: August 21, 2014 | Accepted: October 22, 2014 | Published: October 27, 2014
Citation: Khair AM, Elseid M, Mohamed K, Al-shami R, Ibrahim K, et al. (2014) Cerebellar Stroke in Children, Case report from Qatar & Brief Literature Review. Clin Med Rev Case Rep 1:005. 10.23937/2378-3656/1410005
Copyright: © 2014 Khair AM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: Cerebro-vascular accidents do happen for both adults & children. Pediatric data in contrary to adult data are clearly deficient & lacking behind. Childhood cerebellar strokes are much more rare & difficult to pick up.
Case Report: We are reporting a toddler girl, who happened to be an ex premature & part of quadruplet. She presented with severe headache & head tilting in the absence of other focalizing CNS symptoms. Her brain MRI showed changes suggestive of cerebellar stroke. Patient improved clinically & radiologically after proper therapy.
Discussion: Cerebellar infarctions are likely to be arterial occlusion as a result of vertebral artery dissection, mainly with PICA involvement. An association with some biomarkers & antibodies like anti-2GPI which has been suggested. Trauma, drugs & CNS infection have all been explored as risk factors for childhood cerebellar strokes. Long term outcomes remain poorly studied.
Conclusion: High index of suspicion is required to diagnose cerebellar strokes in children. Clinical presentation is often non specific. Our case report represents a successful story of diagnosis, treatment 7 improvement. However, our understanding of underlying pathological processes, risk factors, management guidelines & future outcome is very limited. Further large scale studies are apparently needed.
Introduction
In spite of increasing perception by neurologists that cerebrovascular diseases occur more frequently in pediatric age group than previously thought, studies in regard to childhood stroke and adolescents have remained largely descriptive. Pediatricians & pediatric neurologists often encounter children with a cerebrovascular lesion, yet large scale clinical research is difficult because these disorders are less common than in adults and arise from diverse causes. When it comes to Qatar & the entire Middle East region, literature becomes even sparser. We are reporting a toddler child who has been found to have evidence of cerebellar rather than cerebral stroke after interesting clinical presentation & appropriate workup.
Case Report
We are reporting R.A, a previously healthy 4 ½ years old. She is, however a member of quadruplet born at 28 week gestation. Otherwise she had caught developmental milestones smoothly thereafter & there has been no health issue of concern to the family.
She presented to our service with five days history of headache, which was severe enough to awaken her from sleep. That was associated with considerable photophobia & tilting of her head towards right side. There was no abnormal movement however, visual change, behavioral concerns nor muscle weakness. Upon physical examination, she has been observed to be vitally stable with normal pulse & blood pressure. She was comfortably breathing in room air. Her neck was obviously tilted towards right side. Nevertheless, she has equally reactive pupils, full range of eye movements & no facial asymmetry. She did not have obvious signs of meningeal irritation at that time. Her upper & lower limb examination showed normal tone, power & reflexes. Her fundoscopic examination was unremarkable & there were no cerebellar signs.
Her CBC, electrolytes, liver function & inflammatory markers were normal. MRI showed features of infarction of infero-lateral aspect of left cerebellar hemisphere obeying track of left anterior inferior cerebellar artery (PICA) with no evidence of hemorrhage. Thereafter, coagulation studies have been carried out, yielding normal sickling test, electrophoresis, PT, aPTT, INR, protein C/S, immunoglobulins levels, ANA, Anti dsDNA, Anti-cardiolipin, anti-thormbin III & viral serology (Figure 1A,1B).
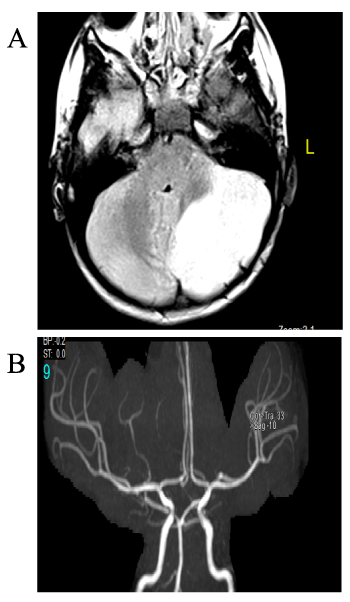
Figure 1A,1B: MRI showing features of infarction of infero-lateral aspect of left cerebellar hemisphere.
The lesion showed high signal intensity in T2 weighted image/FLAR and low signal intensity in T1-weighted image with evidence of some form of restricted
diffusion. No evidence of hemorrhagic transformation is seen.
The lesion showed gyriform pattern of enhancement in the post contrast series.
The intracranial MRA showed outline irregularities and cut off of left AICA.
The MR spectroscopy of the lesion showed elevated lactate and lipid peaks with relatively low level peaks of Choline and N-Acetyl Aspartate.
View Figure 1
Patient has been treated with heparin after involving of hematology team. The patient also received adjuvant course of dexamethasone. The patient showed quick & remarkable response in terms of complete resolution of her symptoms. Her repeat MRI showed improvement of swelling & opening of basal sulci & 4th ventricle. MRA showed some good flow in the AICA. She has then been discharged with tapering dexamethasone regimen & low molecular weight heparin & a plan to repeat her MRI/MRA in 4-6 weeks to ensure regular flow of IACA (Figure 2A,2B).
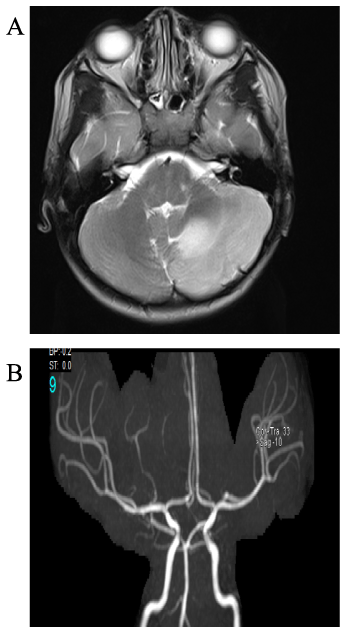
Figure 2A,2B: MRI showing improvement of swelling & opening of basal sulci & 4th ventricle.
Evident regression of the previously seen left inferolateral cerebellar hemisphere edema and associated mass effect. The lesion showed high signal intensity
in T2 weighted image/FLAR and low signal intensity in T1-weighted image while the diffusion study shows pseudo normalization of the previously seen area of
restricted diffusion.
Minimal residual gyriform pattern of enhancement noted in the post contrast series.
The MR spectroscopy of the lesion still shows elevated lactate and lipid peaks with relatively low level peaks of Choline and N-Acetyl Aspartate.
The intracranial MRA showed further reduction in caliber of the left AICA which is hardly visualized suggestive of further regression of the flow.
View Figure 2
Discussion
Deficiency in literature data in regard to childhood stroke is multifactorial. The disease rarity has obviously leaded to physicians being uncomfortable to make such a diagnosis. The same cause has reduced big research centers to conduct large scale, controlled studies. Moreover, the risk factors are so diverse has created a heterogeneous patient population. Deficiency in knowledge & familiarity of clinicians in regard to the suspicion & management of childhood stroke is another encountered obstacle. All those challenges have resulted in most of the childhood cerebrovascular available literature mainly consisting of single case reports or small case series.
With this current believe that strokes are relatively rare in children, it is expected that this culture can lead to significant morbidity and mortality. Clinical presentation of strokes in pediatric age group is clearly different & less profound compared to adults. Clinical symptoms are often unique. A lot of cases might remain none, under- or misdiagnosed. Risk factors of developing strokes in childhood are less ominous than adults. Interestingly, however, management strategies & recommendations are inspired basically from adult studies. There are some existing modifications concerning anticoagulation and & thrombolytic therapy. In the era of deficiency of specific pediatric literature, such recommendations might still be of value. Stressing on specific childhood modifications is ultimately crucial before such application.
Cerebellar strokes are very unusual in childhood. Clinical presentation can be very wide in spectrum. A non conclusive list might include gait ataxia, fine intentional tremors, vertigo, dizziness, nausea, vomiting, visual changes, nystagmus, headache, depressed sensorium level, slurred speech, dysphagia, hearing impairment and issues with pain & temperature perception. No pathognomonic clinical feature exists, however.
When talking about childhood strokes being rare, it is even rarer when it comes to cerebellar ones. The overall incidence of cerebellar artery stroke across all ages is estimated to be 1.5 % with average age of 62 years. In young adults less than 40 years old the most common mechanism of cerebellar infarctions is likely to be arterial occlusion as a result of intracranial vertebral artery dissection (40%), mainly with PICA involvement [1]. It has been observed that isolated Superior Cerebellar Artery (SCA) infarction is quite rare and the mechanism is often not readily apparent [2].
Associations & future sequences of childhood cerebellar strokes remain under-investigated. Cerebellar atrophy is uncommon in childhood arterial ischemic stroke [3]. Association with acute pontine DWI signal may indicate early degeneration of cortico-ponto-cerebellar connections. Nevertheless, the clinical significance of cerebellar atrophy in childhood stroke remains unknown [3].
An association with some biomarkers & antibodies like anti-2GPI which has been associated with recurrent thrombosis and pregnancy morbidity was explored. The major challenge is that prevalence of anti-2GPI in children with cerebral and cerebellar infarction is unknown. Spalice A reported case of childhood cerebellar ischemic stroke with only anti-2GPI but no antibodies detectable in standard anti-phospholipid assays [4].
It is agreed that sickle cell disease is associated with silent cerebral infarction mainly affecting white and cortical grey matter. However, limited data are available in regard to sub-cortical volumes. Kawadler JM has reported a series of specific volumetric differences that were found in the cerebellum [5,6].
A strong theory exists in adult population suggesting that trauma might be a risk factor in developing cerebellar strokes. Moreover, yoga exercises, bow hunting and cervical trauma have all been associated with vertebra-basilar damage and subsequent stroke due to cerebellar infarction. Duval has reported an 11 year old child with cerebellar stroke after bow hunting with apparent hypo-perfusion of the left vertebral artery and occlusion of PICA and AICA [7].
Drugs carry a considerable risk of initiating cerebellar strokes. NSAIDs have been classically considered a risk factor for cerebral stroke in adults; however this assumption has weaker bases in cerebellar strokes. Marijuana use may represent a risk factor for stroke in childhood, particularly in the posterior circulation. Thomas Geller has recently reported 3 young male adolescents who developed cerebellar infarction with acute marijuana use [8].
A well postulated theoretical link between cerebellar infection/inflammation & stroke is development was explored. Viral & post viral cerebellitis might me a risk factor [9]. A wide range of organisms including viruses, bacteria, mycoplasma & chlamydia are thought to be involved. Shanthy has reported cerebellar infarction in a 7 year old girl with HIV/AIDS, probably because of either direct viral invasion or secondary to HIV virus-induced vasculopathy [9].
No data is available regarding long term outcomes in children, but chances of complete resolution versus mild residual impairment appear to be equal [1]. This data deficiency put dark shadows on the process of follow up & counseling.
Conclusion
Strokes in children are largely missed or misdiagnosed. Cerebellar strokes are more challenging as they have very variable clinical presentation & often odd examination findings. We are reporting a toddler girl with vague presentation, but fortunately well investigated. She has been ultimately diagnosed as having cerebellar unilateral strokes. The patient showed good response to thrombolytic therapy. With obvious literature shortage, the need for more epidemiological studies is well clarified.
References
-
Barinagarrementeria F, Amaya LE, Cantu C (1997) Causes and mechanisms of cerebellar infarction in young patients. Stroke 28: 2400-2404.
-
Macdonell RA, Kalnins RM, Donnan GA (1987) Cerebellar infarction: natural history, prognosis, and pathology. Stroke 18: 849-855.
-
Mah S, deVeber G, Wei XC, Liapounova N, Kirton A (2013) Cerebellar atrophy in childhood arterial ischemic stroke: acute diffusion MRI biomarkers. Stroke 44: 2468-2474.
-
Spalice A, Del Balzo F, Perla FM, Papetti L, Nicita F, et al. (2011) Pediatric cerebellar stroke associated with elevated titer of antibodies to ß2-glycoprotein. Med Hypotheses 76: 831-833.
-
Kawadler JM, Clayden JD, Kirkham FJ, Cox TC, Saunders DE, et al. (2013) Subcortical and cerebellar volumetric deficits in paediatric sickle cell anaemia. Br J Haematol 163: 373-376.
-
O'Gorman RL, Siddiqui A, Alsop DC, Jarosz JM (2010) Perfusion MRI demonstrates crossed-cerebellar diaschisis in sickle cell disease. Pediatr Neurol 42: 437-440.
-
Duval EL, Van Coster R, Verstraeten K (1998) Acute traumatic stroke: a case of bow hunter's stroke in a child. Eur J Emerg Med 5: 259-263.
-
Geller T, Loftis L, Brink DS (2004) Cerebellar infarction in adolescent males associated with acute marijuana use. Pediatrics 113: e365-370.
-
Sridhar S, Bruce R, Edelson PJ (1996) Cerebellar stroke in pediatric AIDS. Pediatric Research 39: 381-381.





