Clinical Medical
Reviews and Case Reports
Chorioretinitis as a Rare Presentation of Cat Scratch Disease: A Case Report
Zimmermann1, Nicolas Lefebvre2, Jaulhac B3 and Sauer A1*
1Service d'ophtalmologie, Hopitaux Universitaires de Strasbourg, Nouvel Hôpital Civil, France
2Service de maladies infectieuses et tropicales, Hôpitaux Universitaires de Strasbourg, France
3Service de bactériologie, Hôpitaux Universitaires de Strasbourg, France
*Corresponding author: Sauer A, Service d'ophtalmologie, Hopitaux Universitaires de Strasbourg, Nouvel Hôpital Civil, BP 426, 67091 Strasbourg Cedex, France, Tel : +33 3 69 55 04 37, E-mail: arnaud.sauer@chru-strasbourg.fr
Clin Med Rev Case Rep, CMRCR-2-045, (Volume 2, Issue 7), Case Report; ISSN: 2378-3656
Received: June 30, 2015 | Accepted: July 27, 2015 | Published: July 30, 2015
Citation: Zimmermann, Lefebvre N, Jaulhac B, Sauer A (2015) Chorioretinitis as a Rare Presentation of Cat Scratch Disease: A Case Report. Clin Med Rev Case Rep 2:045. 10.23937/2378-3656/1410045
Copyright: © 2015 Zimmermann, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective: To report a rare presentation of Cat-scratch disease
Design: Case report
Result: A 12-year-old female was referred in our center for management of a chorioretinopathy. Ophthalmologic examination revealed unilateral chorioretinal scar with subretinal detachment. Laboratory evaluation revealed IgG antibodies for Bartonella hensalae. Treatment with oral azithromycin led to regression of lesions, resolution of subretinal detachment, and improvement in visual acuity.
Conclusion: Chorioretinal lesions in Cat-Scratch disease are rare presentation. Serology investigation is important to confirm the diagnosis. Appropriate treatment may improve the outcome.
Keywords
Bartonella henselae, Cat-scratch disease, Chorioretinitis, Toxoplasmosis
Introduction
Cat-scratch disease is an infectious disease caused by Bartonella henselae. The infection is transmitted to humans by cats or dogs [1]. Most of infected cats are asymptomatic whereas dogs are severely impaired (Asthenia, cachexia, endocarditis, death) [2]. The most common human form of the cat-scratch disease is a benign flu-like syndrome or the presence of an inoculation vesiculopustule, followed by persistent adenopathys (2-4 months). The usual clinical signs of ocular involvement are oculo glandular syndrome of Parinaud (granulomatous conjunctivitis followed by adjacent preauricular adenopathy) and Leber's stellate neuroretinitis [2,3]. The diagnostic of cat-scratch disease is often unknown especially in ophthalmological symptoms.
We report an atypical case of Cat-scratch disease presented as chorioretinitis.
Case Report
A 12-year-old female was referred to our center for deteriorating eyesight secondary to a retinochoroiditis: right eye 4/10 Parinaud 4 (left eye, 10/10 Parinaud 2) since one month. She was previously treated for toxoplasmic retinochoroiditis since 3 weeks (Pyriméthamine, sulfadiazine, folinic acid and Corticoid orally). Faced with this aggravation, clinical and laboratory reassessment has been prescribed.
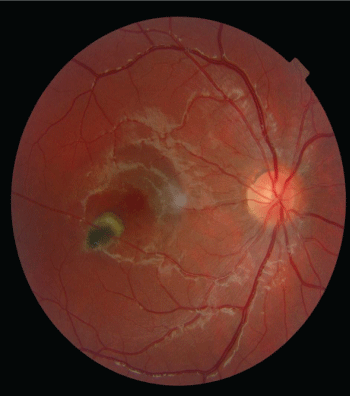
The detailed patient interview found repeated contacts with cats and a low-grade fever six weeks ago. Ophthalmologic examination revealed unilateral chorioretinal scar with sub retinal detachment without hyalitis (Figure 1). The anterior segment was calm and the ocular tension was normal.
.
Figure 1: Right eye's fundus photography. Deeply pigmented paracentral choroiditis scar with a sub-retinal detachment, without adjacent hyalitis.
View Figure 1
Fluorescein Angiography sequences showed a hyper auto fluorescent scar, which take progressively contrast enhancement during the indo cyanine green angiography.
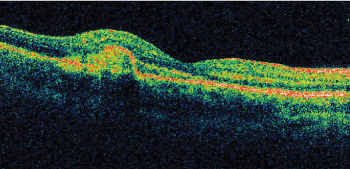
Optical Coherence Tomography (OCT) found a subretinal detachment and an infiltration at the site of chorio-retinal scar (Figure 2).
.
Figure 2: Optic Coherence Tomography through the infected site. Sub-retinal thickening.
View Figure 2
A complete biological work-up was done. The blood count was normal despite a little hyperleucocytosis. She had a negative toxoplasmic serology (repeated at two times with an interval of 1 month) that definitively excluded the former diagnosis of toxoplasmic retinochoriditis, an old immunity against Herpes Simplex virus, Varicella zoster virus and cytomegalovirus, and a vaccinal immunity against hepatitis B virus. The serologies testing were negative for Ebstein- Barr Virus (EBV), Lyme's disease, Human Immunodeficiency Virus (HIV) and leptospirosis. The Antinuclear antibodies research was positive on 1/80 with a speckled appearance. The rest of the blood sample was non-contributory benefits.
The Polymerase Chain Reactive (PCR) on aqueous humor didn't find neither Toxoplamasma gondii, CMV nor HSV.
After the discovery of a large right adenopathy and a cat- scratch scar, a serology of Bartonella henselea was made (IgG IFI, Bartonella henselae strain HOUSTON 1 ATCC 49882), and was positive (1/64) ; confirming the diagnostic with a specificity of 87% and a sensitivity of 78%.
The retrospective interview gave us to discover that, the patient took in a sick kitten two months ago, without the knowledge of her parents, that's why we didn't know this information previously. The kitten scratched her several times, and died few days after his coming.
So a treatment of Azithromycin 250mg per day was prescribed during three weeks with a stop of anti-toxoplasmic's treatment, especially the orally Corticoid. The patient had completely recovered visual acuity (10/10 Parinaud 2), but it remained a paracentral scotoma after 6 months disease's evolution. The serology of Bartonella hensalea went progressively negative, during the following three months (value <1/8).
Discussion
The eye is the non-lymphatic's organ which is the mostly affected during the cat-scratch disease [3]. The Parinaud oculoglandular syndrome, is the most common ocular complication, and affects about 5% of symptomatic patients. Their main complaints are redness and foreign body sensation. The conjunctival damage may extend to necrosis or ulceration. A preauricular adenopathy is frequently found [4-6].
On other classical form of the disease, but rather unusual is the neuroretinitis. It presents as a papillary edema with subretinal detachment and sometimes followed by a macular star 2 or 4 weeks later [7]. It represents approximately 1 to 2% of patients with ocular Bartonella [8]. Simultaneous and consecutive forms of Parinaud oculoglandular syndrome and neuroretinitis are described [9]. Sometimes multifocal retinitis or choroiditis scars are associated with the neuroretinitis. A retinochoroiditis scar without papillary edema, like in our case, is a very unusual form of the disease, and mostly found in immunocompromised patients [10]. Contrary to our case, there is frequently a hyalitis and an anterior chamber reaction. It can be complicated by veinous or arterial occlusion and by a sub-retinal detachment [11]. The principle differential diagnosis of retinochoroiditis is ocular toxoplasmosis. Toxoplasmosis was excluded in our case because of negative serology.
Moreover, as demonstrated in our case, the detection of antibodies against Bartonella henselae is the easier technique to confirm the disease. The serology has however some drawbacks: (i) the antibodies titer depends of antigen's preparation (bacteria growth on agar media or cell culture), (ii) about 10% of patients suffering from cat-scratch disease have no detectable antibodies level (false-negative), (iii) different Bartonellosis strains present antigenic variations, (iv) there are several antigenic cross-reactivities between Bartonella and others bacteria like Coxiella burnettii, Chlamydia trachomatis, Chlamydophila pneumoniae and Chlamydophila psittaci. However, the sensitivity and the specificity of those techniques reach 90% in immunocompetent patients [12]. The PCR reactions have made a lot of progress in the diagnosis of meningeal forms of the disease, but are still not available in ocular forms [13].
Nowadays, there is no recommendation for the treatment of ocular forms of cat-scratch disease. In our case, we prescribed azithromycin during four weeks, as recommended for neuroretinitis or lymphangiopathy during cat-scratch disease. No corticotherapy was prescribed. This treatment seems to improve the local inflammation, leads to a negativation of Bartonella henselae serolgy and shows an excellent tolerance. Finally, this patient only suffered of a paracentral scotoma. In most case of cat-scratch disease, the prognosis is good when an early diagnosis is made. This highlights once again the need for rapid biological work-up including Bartonella henselae serology in case of atypical chorioretinitis.
Conclusion
Chorioretinal lesions in Cat-Scratch disease are rare presentation. Even the most frequently evoked diagnosis is ocular toxoplasmosis, ophthalmogist should think about cat-scratch disease in front of atypical evolution. Serology investigation is important and rather easy to confirm the diagnosis. Appropriate treatment may improve the outcome. Azythromycin, for an extended period seems to be an interessant therapeutic opportunity.
References
-
Spach DH, Koehler JE (1998) Bartonella-associated infections. Infect Dis Clin North Am 12: 137-155.
-
Florin TA, Zaoutis TE, Zaoutis LB (2008) Beyond cat scratch disease: widening spectrum of Bartonella henselae infection. Pediatrics 121: 1413-1425.
-
Carithers HA (1985) Cat-scratch disease. An overview based on a study of 1,200 patients. Am J Dis Child 139: 1124-1133.
-
Tompkins LS (1997) Of cats, humans, and Bartonella. N Engl J Med 337: 1916-1917.
-
Grando D, Sullivan LJ, Flexman JP, Watson MW, Andrew JH (1999) Bartonella henselae associated with Parinaud's oculoglandular syndrome. Clin Infect Dis 28: 1156-1158.
-
Roe RH, Michael Jumper J, Fu AD, Johnson RN, Richard McDonald H, et al. (2008) Ocular bartonella infections. Int Ophthalmol Clin 48: 93-105.
-
Herz AM, Lahey JM (2004) Images in clinical medicine. Optic neuritis due to Bartonella henselae infection. N Engl J Med 350: 351.
-
Suhler EB, Lauer AK, Rosenbaum JT (2000) Prevalence of serologic evidence of cat scratch disease in patients with neuroretinitis. Ophthalmology 107: 871-876.
-
Cunningham ET, Koehler JE (2000) Ocular bartonellosis. Am J Ophthalmol 130: 340-349.
-
Accorinti M (2009) Ocular bartonellosis. Int J Med Sci 6: 131-132.
-
Cohen SM, Davis JL, Gass DM (1995) Branch retinal arterial occlusions in multifocal retinitis with optic nerve edema. Arch Ophthalmol 113: 1271-1276.
-
Dalton MJ, Robinson LE, Cooper J, Regnery RL, Olson JG, et al. (1995) Use of Bartonella antigens for serologic diagnosis of cat-scratch disease at a national referral center. Arch Intern Med 155: 1670-1676.
-
Dong J, Olano JP, McBride JW, Walker DH (2008) Emerging pathogens: challenges and successes of molecular diagnostics. J Mol Diagn 10: 185-197.





