Clinical Medical
Reviews and Case Reports
An Unusual Foreign Body in the Neck: A Case of Sternal Wire Migration
O'Connell BP1, DeNino WF2 and O'Rourke AK1*
1Department of Otolaryngology, Head and Neck Surgery, Medical University of South Carolina, USA
2Division of Cardiothoracic Surgery, Medical University of South Carolina, USA
*Corresponding author: Ashli K O'Rourke, Department of Otolaryngology, Head and Neck Surgery, Medical University of South Carolina, Charleston, South Carolina, USA, E-mail: aorourke@musc.edu
Clin Med Rev Case Rep, CMRCR-2-042, (Volume 2, Issue 7), Case Report; ISSN: 2378-3656
Received: March 30, 2015 | Accepted: July 23, 2015 | Published: July 26, 2015
Citation: O'Connell BP, DeNino WF, O'Rourke AK (2015) An Unusual Foreign Body in the Neck: A Case of Sternal Wire Migration. Clin Med Rev Case Rep 2:042. 10.23937/2378-3656/1410042
Copyright: © 2015 O'Connell BP, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Migration of sternal wires is a rare, but potentially life-threatening, complication of median sternotomy. We present a case of sternal wire migration into the soft tissue of the anterior neck that occurred approximately 3 months following type I thyroplasty with Gor-tex® implantation. Given the rarity of sternal wire migration, initial clinical suspicion was for extrusion of the Gore-Tex® implant. However, computed tomography imaging revealed migration of a superior sternal wire into the neck. After confirmation that the wire was not intimately associated with any major neurovascular structures of the neck, it was successfully removed under monitored anesthesia care without complication.
Keywords
Sternal wire migration, Foreign body, Sternotomy
Abbreviations
CT: Computed Tomography, CXR: Chest X-ray, MAC: Monitored Anesthesia Care, CABG: Coronary Artery Bypass Graft
Introduction
Migration of sternal wires is a rare, but potentially serious, complication of median sternotomy and there are a limited number of reports in the literature regarding such migration [1-5]. Most of these reports document cardiac and/or vascular injuries related to thoracic migration of stainless steel wires [4-6]. Imran et al. reported bilateral pneumothoraces due to lateral displacement of sternal wires [1]. Rungatscher et al. described sternal wire segments adjacent to, and inside of, the sternal insertion of the sternocleidomastoid muscle resulting in an intramuscular hematoma, but the wire itself had not migrated into the cervical region [2]. Given the potential for catastrophic complications secondary to this rare phenomenon, prompt surgical removal is warranted. We report the first case of sternal wire migration superior to the sternal notch and clavicular heads.
Case Presentation
The patient is a 59-year-old female, with a past medical history of coronary artery disease status post Coronary Artery Bypass Grafting (CABG) and mitral valve replacement in November 2011, obesity (status post gastric bypass surgery in June 2013), hypertension, hypothyroid, obstructive sleep apnea, depression, and anxiety. Additional surgical history included cesarean section, cholecystectomy, and bilateral tubal ligation. Following her CABG procedure, she reported progressive dysphonia without dysphagia. She was eventually referred to our institution, at which time video stroboscopy demonstrated left vocal fold immobility with a large glottic gap upon phonation. This was the contributing factor to her dysphonia. She underwent left sided type I thyroplasty with placement of a Gore-Tex® implant in September 2013. Her post-operative course was uneventful. Sutures were removed on post-operative day 7 and no wound infection or dehiscence was noted. Her voice quality following her type I thyroplasty was significantly improved and near normal.
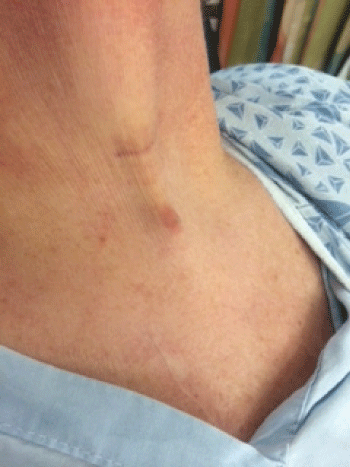
In January 2014, she presented to the Emergency Department at our institution with the primary complaint of a foreign object protruding under her skin, which she had first noticed earlier the same day. She denied cough, change in voice, dysphagia, shortness of breath, stridor or chest pain. Additionally, she denied any recent falls or other trauma. Vital signs were within normal limits. On physical exam, there was a visible protrusion in the midline of the neck approximately four centimeters above the sternal notch (Figure 1). The skin overlying the protrusion was intact but a firm, mobile subcutaneous pinpoint mass could be palpated (Figure 2). Transnasal flexible laryngoscopy was performed. The left vocal cord was immobile, but with good medialization to the midline position. The endoscopy was otherwise within normal limits; in particular there was no sign of Gore-Tex® malposition or mucosal lesion. Her airway was patent.
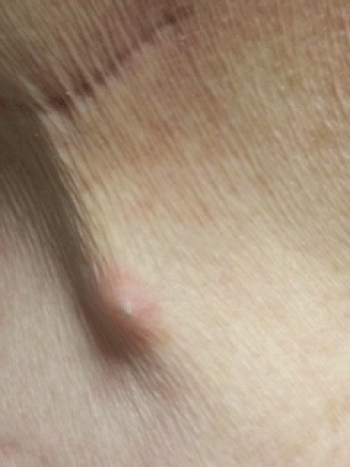
.
Figure 2: Close-up view of the anterior neck; what appears to be a metallic object can be appreciated just under the skin.
View Figure 2
Given her recent thyroplasty surgery, it was initially felt the foreign body may have represented extrusion of her Gore-Tex® implant. Extrusion of a thyroplasty implant is a known, yet rare, complication of type I thyroplasty. However, the pinpoint nature of the mass and prior history of sternotomy prompted further imaging evaluation. A contrasted Computed Tomography (CT) scan of the neck and chest was performed, which demonstrated a metallic wire in the left neck extending from the clavicular head of the left sternocleidomastoid muscle to the skin surface slightly inferior to the level of the hyoid bone; the 3-dimensional CT reconstruction is shown in Figure 3. There was no vascular injury noted, although the distal end of the wire did appear to abut the left inferior thyroid vein (Figure 4). The September 2013 pre-operative chest radiograph (CXR) obtained at the time of thyroplasty was reviewed, which demonstrated seven sternal wires in the usual location, however the most superior wire, while still located in the chest, was untwisted and the ends were not approximated (Figure 5).
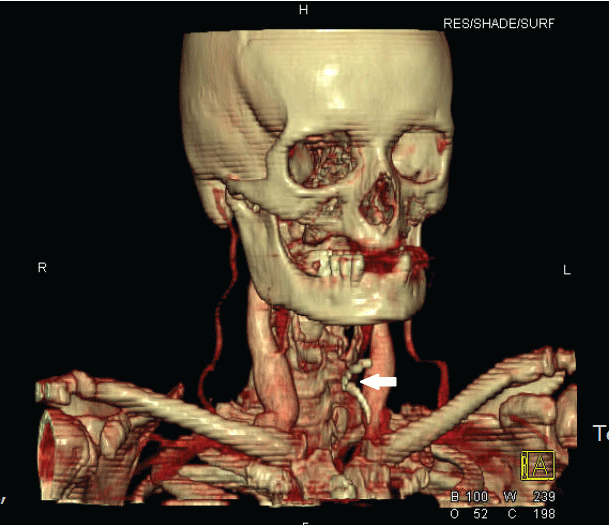
.
Figure 3: 3-dimensional CT reconstruction demonstrating a thin curvilinear object (white arrow), 1.5mm in diameter, in the soft tissue of the anterior neck.
View Figure 3
.
Figure 4: Sagittal neck CT image showing the close proximity of the wire (bright metallic signal) to the left inferior thyroid vein (arrow).
View Figure 4
Consultation with both otolaryngology and cardiothoracic surgery was obtained. Due to the entirety of the wire being present in the cervical region, the decision was made to proceed to the operating room with the otolaryngology service on the evening of presentation. Under monitored anesthesia care (MAC), a 1 cm incision was made directly over the wire that could be readily felt beneath the skin. Sharp dissection was carried down along the length of the wire to an approximate depth of 1.5 cm, removing what appeared to be a fibrous capsule around the wire. With limited dissection, the wire was able to be freed from the surrounding capsule and, at this point, appeared to be fully mobile. It was grasped with a Kelly clamp and removed from the neck with minimal traction (Figure 6). The removed wire was approximately 4 cm in length and 1 mm in diameter. There was no bleeding. The patient tolerated the procedure without complication and was admitted overnight for observation. On post-operative day one, the neck was without edema or signs of vascular anomaly. She had minimal to no pain and was tolerating a regular diet. No subsequent imaging was obtained. She was discharged home with regular follow-up in the otolaryngology clinic. On following visits, her voice quality remained excellent and she had no apparent further issues related to the sternal wire migration.
.
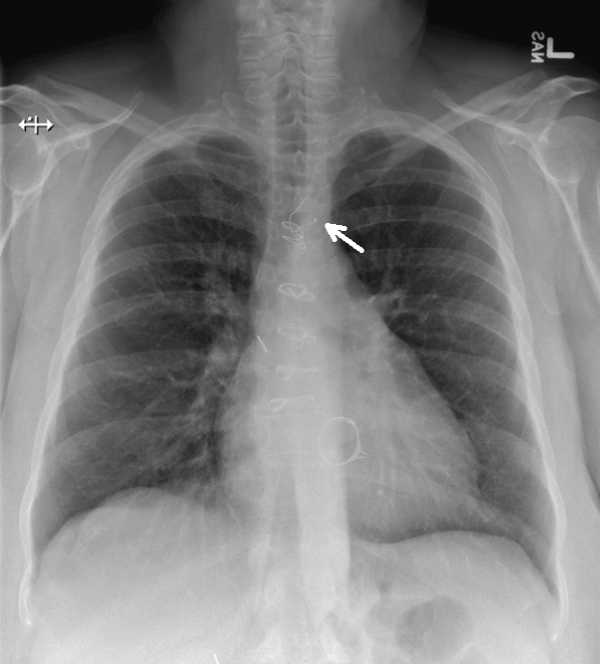
Figure 5: Seven sternal wires in the usual location were present on chest radiograph four months prior to presentation to the emergency department. This was taken before her thyroplasty surgery. The most superior wire (white arrow) was untwisted and both ends were not approximated. A valvular prosthesis in the mitral position was also appreciated.
View Figure 5
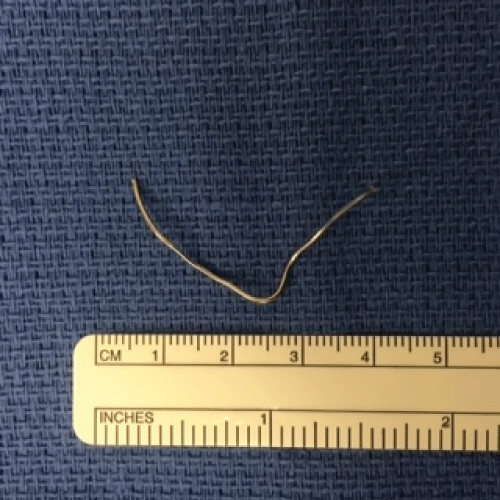
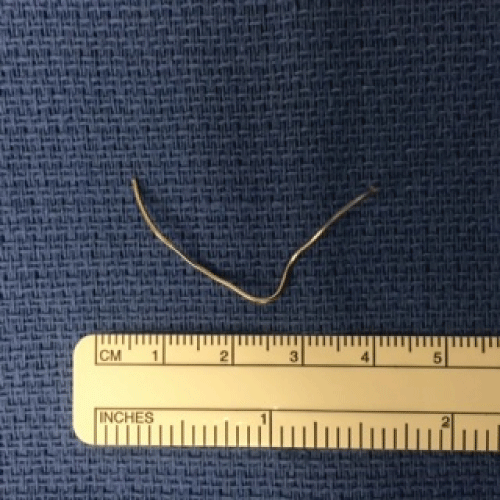
.
Figure 6: The sternal wire after removal from the soft tissue of the anterior neck.
View Figure 6
Discussion
This is the first report, to our knowledge, of sternal wire migration superiorly into the neck over the course of a relatively short period of time without involvement of vascular or muscular structures. The wire was safely removed with limited dissection of the anterior neck space.
In most instances, sternal wire fracture, displacement, or migration can be readily diagnosed on CXR [7]. Nevertheless, sternal wire abnormalities can be easily overlooked on plain film imaging if one's attention is not directed at evaluation of the sternum. As it pertains to this case, no comment was made regarding the untwisted, un-approximated superior sternal wire in the interpretation of her pre-thyroplasty CXR. Although this would not have changed management, as the wire had not yet migrated, the potential morbidity associated with a displaced wire could have been acknowledged and discussed with the patient and the cardiothoracic team. Indentations of the wire seen on the initial CXR, and following its removal, support that the wire was once previously fully approximated. The appearance of the wire on CXR supports that the superior wire was previously approximated and slowly unraveling over time.
CT imaging can be a useful adjunctive study in the work-up of displaced sternal wires as precise wire location, length, and curvature can be determined. This information can facilitate an understanding of the rotation needed to allow a smooth, atraumatic removal of the wire [4]. CT also permits more accurate risk assessment and, in this case, provided reassurance that the wire was not intimately associated with any major vascular structures in the neck [3]. This led us to attempt removal under MAC, which was well tolerated. Had there been concern on imaging for vascular or airway involvement, or had dissection been tedious intra-operatively, endotracheal intubation with general anesthesia would have been preferred.
Radiographic evidence of sternal wire abnormalities has been described in association with sternal dehiscence [7,8]. In fact, an interesting factor in this case may be the patient's significant weight loss (approximately 70 pounds) following her gastric bypass surgery in 2013. Although sternal dehiscence and subsequent non-union is thought to be multifactorial in nature [9], malnutrition that may coexist with precipitous weight loss could have contributed to this complication. Boiselle et al. showed that lateral displacement of sternotomy wires was observed in 84% of patients with dehisced sternotomy wounds, and disruption of wires was found in 21% of patients. Mean distance of maximal displacement lateral to midline was noted to be 20 mm [8]. However, wires have been reported to migrate as far as 25 cm, as reported by Radich et al., in which some wires were found in the posterior-lateral abdominal wall [3]. In our case, the wire migrated 4 cm superior to the sternal notch. As cranial migration of sternal wires above the clavicular heads has not previously been reported, the superior migratory capacity of sternal wires remains unclear, but possible.
Conclusion
Sternal wire migration is a rare but potentially devastating complication of sternotomy. Plain film chest radiography is adequate in the majority of cases to diagnose sternal wire abnormalities. In cases of atypical or marked migration, CT imaging should be considered as it allows for more precise localization of the wire, determines the proximity of vital neurovascular structures, and can assist in risk assessment and pre-operative planning. Prompt surgical removal of migrated wires is warranted to avoid life-threatening complications. Awareness amongst otolaryngologists of the potential for sternal wire migration into the neck is needed, particularly in light of the important neurovascular and airway structures that could be compromised by such migration.
References
-
Imran Hamid U, Gillespie S, Lynchehaun C, Parissis H (2012) Traumatic Bilateral Pneumothoraces due to Sternal Wire Migration. Case reports in medicine 2012: 438429.
-
Rungatscher A, Morjan M, Faggian G (2011) Sternocleidomastoid muscle hematoma due to sternal wire migration. J Card Surg 26: 296.
-
Radich GA, Altinok D, Silva J (2004) Marked migration of sternotomy wires: a case report. J Thorac Imaging 19: 117-119.
-
Levisman J, Shemin RJ, Robertson JM, Pelikan P, Karlsberg RP (2010) Migrated sternal wire into the right ventricle: case report in cardiothoracic surgery. J Card Surg 25: 161-162.
-
Hazelrigg SR, Staller B (1994) Migration of sternal wire into ascending aorta. Ann Thorac Surg 57: 1023-1024.
-
Schreffler AJ, Rumisek JD (2001) Intravascular migration of fractured sternal wire presenting with hemoptysis. Ann Thorac Surg 71: 1682-1684.
-
Hayward RH, Knight WL, Reiter CG (1994) Sternal dehiscence. Early detection by radiography. J Thorac Cardiovasc Surg 108: 616-619.
-
Boiselle PM, Mansilla AV, Fisher MS, McLoud TC (1999) Wandering wires: frequency of sternal wire abnormalities in patients with sternal dehiscence. AJR Am J Roentgenol 173: 777-780.
-
Wu LC, Renucci JD, Song DH (2005) Sternal nonunion: a review of current treatments and a new method of rigid fixation. Ann Plast Surg 54: 55-58.