Clinical Medical Reviews and Case Reports
Cement Powder Ingestion: Case Report and Review of the Literature
Kim Lewis1, Christopher Sheasgreen2 and Waleed Alhazzani1,3*
1Department of Medicine, McMaster University, Hamilton, Canada
2Department of Gastroenterology, Mount Sinai Hospital, Toronto, Canada
3Department of Clinical Epidemiology and Biostatistics, McMaster University, Hamilton, Canada
*Corresponding author:
Waleed Alhazzani, Department of Medicine, McMaster University, 1280 Main Street West, Hamilton, Ontario L8S 4L8, Canada, E-mail: alhazzaw@mcmaster.ca
Clin Med Rev Case Rep, CMRCR-4-152, (Volume 4, Issue 1), Case Report; ISSN: 2378-3656
Received: November 14, 2016 | Accepted: January 27, 2017 | Published: January 30, 2017
Citation: Lewis K, Sheasgreen C, Alhazzani W (2017) Cement Powder Ingestion: Case Report and Review of the Literature. Clin Med Rev Case Rep 4:152. 10.23937/2378-3656/1410152
Copyright: © 2017 Lewis K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Alkaline material ingestions can cause a wide variety of injuries, ranging from mild to fatal. Cement is an alkaline agent and can lead to abrasions, allergic dermatitis, and chemical burns. There are very few case reports of cement ingestion in the literature. The gold standard for assessing the extent of injury after cement ingestionis via an esophagogastroduodenoscopy (EGD) within 12-24h. However, there have been no reports to date on the necessity of early endoscopic intervention in cement ingestions. Here, we report a case of cement ingestion not requiring endoscopic interventions.
Case: A 49-year-old woman was admitted after asuicide attempt where she had admitted to ingesting handfuls of cement powder. An EGD was performed in the emergency room that reveled superficial injury to the mucosa and grey-brown like sledge. However, no interventions were administered. A proton pump inhibitor was prescribed and she was followed both clinically and with serial abdominal radiographs to monitor for obstruction. Four days later, a repeat EGD was performed that showed healing of the superficial mucosal injury.
Conclusion: While cement ingestion may cause serious injury, there is also a possibility of a benign outcome. Therefore, cases of cement ingestion should be treated as corrosive ingestion with early endoscopy for risk stratification, frequent surveillance and clinical monitoring, and in some cases, endoscopic or surgical removal of solid material maybe required. However, not every case of cement ingestion requires intervention.
Keywords
Cement, Ingestion, Esophagogastroduodenoscopy, EGD, Alkaline ingestion
Introduction
Caustic ingestions can cause a wide variety of injuries, ranging from mild to fatal [1]. The vast majority of ingestions occurs in the pediatric population, and is accidental in nature [2]. Unfortunately, caustic ingestions in adults areusually intentional and often associated with suicide attempts; the resultant injuries tend to be more severe than accidental caustic ingestion [3,4]. The extent of tissue injury depends on the concentration of corrosive agent, the pH of the substance, premorbid state of tissue, contact duration, and amount of substance ingested [5].
Alkaline material account for most cases of caustic ingestions in western countries [5]. Typically, alkaline agents are found in cleaning agents such as bleaches, detergents, and drain openers [6]. Most typical cleaners have a pH of 10.8 to 11.4 which can produce mild irritation to the mucosa of the gastrointestinal (GI) tract, and are associated with an increased long term risk of strictures [6]. Alkaline agents with a pH greater than 12 can result in liquefaction necrosis and cause such effects as esophageal perforation [6].
Cement is an alkaline agent. Exposure to cementcan lead to abrasions, allergic dermatitis, and chemical burns [7,8]. There are very few accounts of cement ingestion in the literature [9-11]. The gold standard for assessing the extent of injury after ingestion is via an esophagogastroduodenoscopy (EGD) within 12 to 24 hours post ingestion [12]. However, there have been no reports to date on the necessity of early endoscopic intervention in cement ingestions.
Case Report
Here, we report a case of cement ingestion not requiring endoscopic interventions.
A 49-year-old woman was admitted after a suicide attempt. The patient was found by her family with an opened container of cement powder next to her, which she admitted to ingesting an indeterminate amount. Apart from cement powder around her mouth and superficial cuts on her wrists, her physical exam was unremarkable. She had a leukocytosis of 23 × 109/L, however her hemoglobin was at her baseline of 143 g/L and platelets were 253 × 109/L. The toxicology screen for alcohol, salicylates, and acetaminophen were negative. The anion and osmolar gap were both within normal limits.The serumlactate level was normal, and creatinine was slightly elevated (136 umol/L) secondary to dehydration. A chest radiograph appeared unchanged from baseline. She also had a normal computed tomography (CT) of the brain and abdominal radiograph at time of presentation.
.
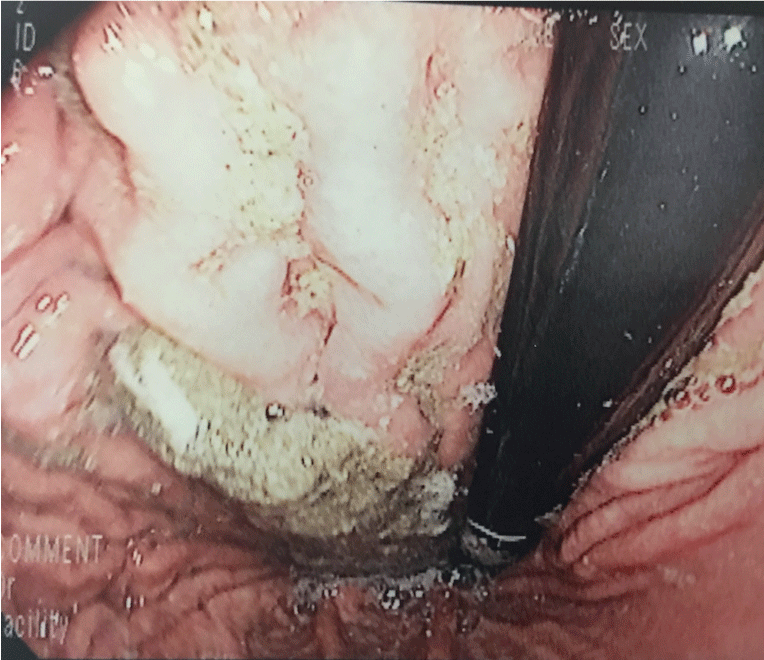
Figure 1A: A picture from the first esophagogastroduodenoscopy that revealed copious amounts of grey-brown sludge-like material consistent with appearance of the cement product in the stomach.
View Figure 1A
The regional Poison Control Centre recommended an EGD to rule out caustic injury to the esophagus and stomach. This revealed erythematous mucosa with superficialabrasions in the stomach, grade 1A esophagitis, and copious amounts of grey-brown sludge-like material in the stomach consistent with appearance of the cement product (Figure 1A, Figure 1B and Figure 1C). We avoided suctioning the cement material or irrigation with water. The patient was admitted to the ward for observation. She was treated supportively by initially making her nil per os and by placing her ona proton pump inhibitor (PPI). She also had serial daily abdominal radiographs and physical examination to monitor for obstruction.
.
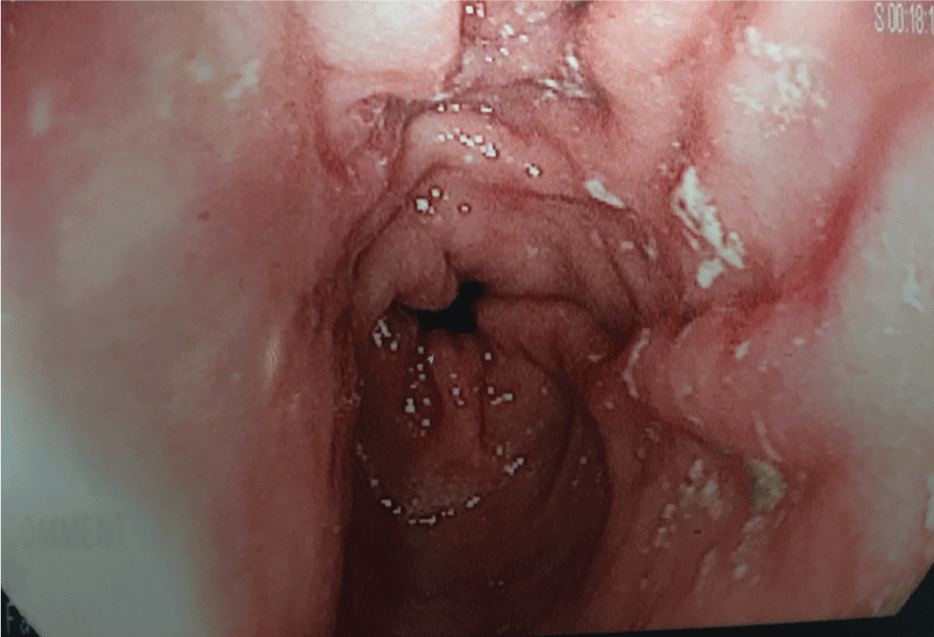
Figure 1B: A picture from the first esophagogastroduodenoscopy that revealed normal gastric folds and mucosa.
View Figure 1B
.
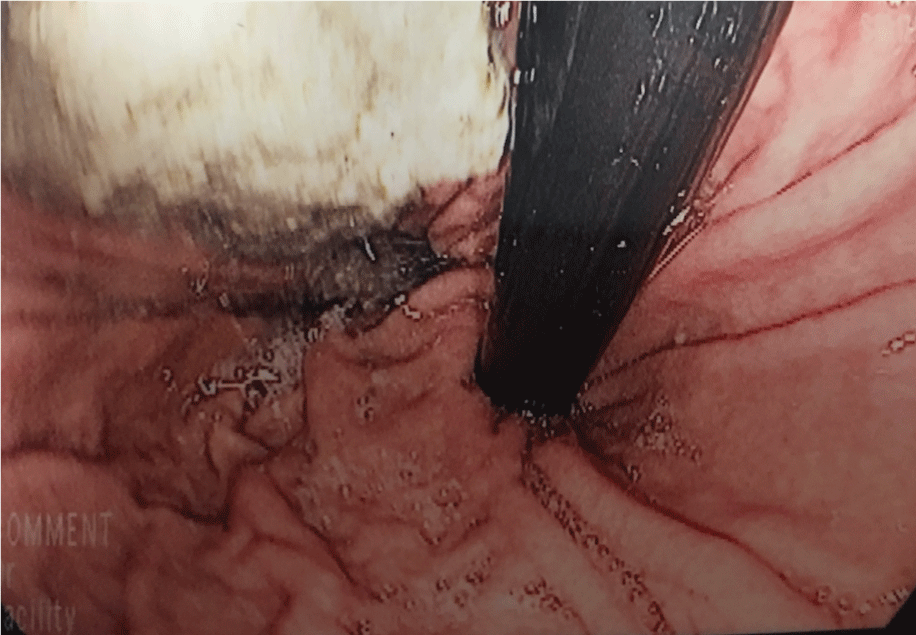
Figure 1C: A picture from the first esophagogastroduodenoscopy that revealed copious amounts of grey-brown sludge-like material consistent with appearance of the cement product in the stomach.
View Figure 1C
A repeat EGD four days later showed short scabs in a linear configuration along the greater curvature of the stomach in keeping with the abrasions seen on the previous EGD and friable esophageal mucosa consistent with caustic injury (Figure 2A and Figure 2B). There were no remnants of cement observed. The patient continued inpatient treatment for suicidality and psychotic depression. She did not develop bowel obstruction or perforation, and continued to have normal bowel movements throughout the hospital stay. She was eventually discharged home.
.
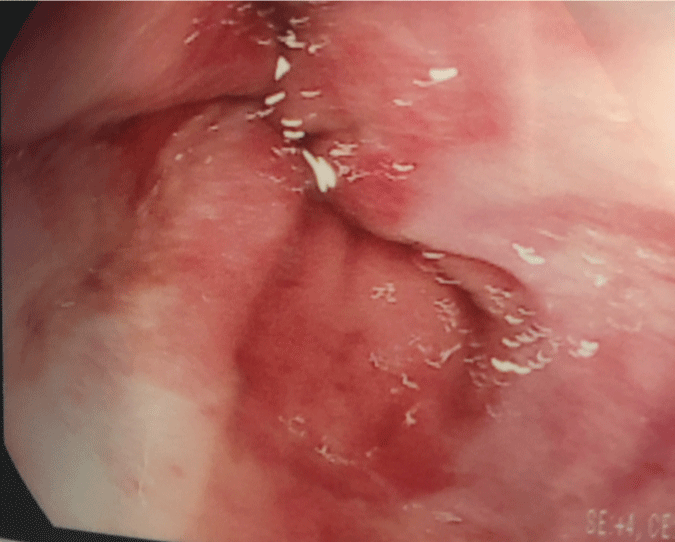
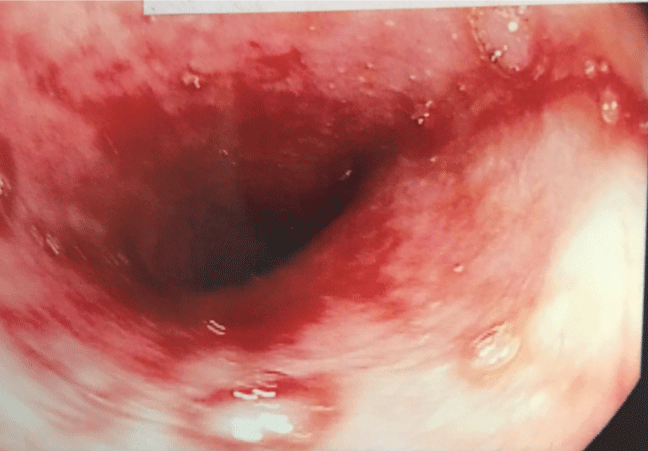
Figure 2A: A repeat esophagogastroduodenoscopy4 days later showed friable esophageal mucosa with superficial erosions.
View Figure 2A
.
Figure 2B: A repeat esophagogastroduodenoscopy 4 days later showed short scabs in a linear configuration and erythema in the antrum but no ulceration visualized.
View Figure 2B
Discussion
Cement is a widely accessible substance. When it is mixed with water, the base of tri-calcium silicate rapidly reacts to release calcium ions, hydroxide ions (causing the pH to rise to 12 or greater), and a large amount of heat [13,14]. The negative sequela of cement-induced topical burns has been well documented in the literature [15-18]. For example, in a case series study, it was found that cement-induce thermal burns can result in full thickness burns that required surgical intervention [17]. However, there has been very little documentation on cement ingestion, and thus, no standard of care has been established.
A previous report by Visvanathan, et al. included six case studies. In this case series, both a 20-year-old patient and a 31-year-old patient had to ultimately have a formal gastrotomy to remove bezoars. The amount of cement each patient ingested was undetermined, however both patients had a radiopaque oval mass in the stomach detected on an upright chest radiograph. None of the remaining four patients had an opacity on their radiographs and ultimately none needed surgery. Visvanathan and colleagues suggested a gastric lavage be performed within three hours of ingestion to allow for dilution of cement and prevention of solidifications [10]. However, given the reaction of cement with water, as described above, lavage with water may induce further injuries.
A recent paper introduced a case where an 83-year-old patient had a seven centimeter hyperdense material noted on CT after an intentional cement ingestion of an unknown amount. They were able to remove the collection of cement by endoscopy, as well as other remaining cement, and the patient made a full recovery [11]. This approach seems appropriate to prevent bezoar formation that will require surgical removal.
The remaining case of a 46-year-old who attempted suicide by ingesting mouthfuls of cement in the literature also performed an EGD but no interventions were required [9]. Given that our patient also lacked any major complications, we suggest that while there is potential for serious injury, there is also a possibility of a benign outcome with cement ingestion. Therefore, cases of cement ingestion should be treated as corrosive ingestion, early endoscopy is required for risk stratification, frequent surveillance and clinical monitoring, and in some cases endoscopic or surgical removal of solid material maybe required. More case series are required to help inform clinical practice.
Disclosure
The authors have no conflict of interest directly relevant to the content of this article.
Acknowledgment
The authors have no acknowledgments.
References
-
Gupta S, Croffie J, Fitzgerald J (2001) Is esophagogastroduodenoscopy necessary in all caustic ingestions? J Pediatr Gastroenterol Nutr 32: 50-53.
-
Gorman R, Khin-Maung-Gyi M, Klein-Schwartz W, Oderda GM, Benson B, et al. (1992) Initial Symptoms as Predictors of Esophageal Injury in Alkaline Corrosive Ingestions. Am J Emerg Med 10: 189-194.
-
Baskin D, Urganci N, Abbasoglu L, Alkim C, Yalçin M, et al. (2004) A standardized protocol for the acute management of corrosive ingestion in children. Pediatr Surg Int 20: 824-828.
-
Satar S, Topal M, Kozaci N (2004) Ingestion of caustic substances by adults. Am J Ther 11: 258-261.
-
Gumaste V, Dave P (1992) Ingestion of corrosive substances by adults. Am J Gastroenterol 87: 1-5.
-
Moore W (1986) Caustic Ingestions. Clin Peds 25: 192-196.
-
Mehta R, Handfield-Jones S, Bracegirdle J, Hall P (2002) Cement dermatitis and chemical burns. Clin Exp Dermatol 27: 347-348.
-
Seyhan N, Keskin M, Savaci N (2012) Contact with wet cement: an unrecognized cause of chemical burn. Ulus Travma Cerrahi Derg 18: 189-191.
-
Keizo S, Tsugawa S, Ohtsuji M, Kondo T, Ohshima T (1995) Severe hyponatremia caused by cement ingestion during carbamazepine therapy. Am J Emerg Med 13: 245-247.
-
Visvanathan R (1986) Cement bezoars of the stomach. Br J Surg 73: 381-382.
-
Kim K, Lee J, Yang S, Lee WS, Sung WY, et al. (2015) Ingestion of Portland Cement. J Emerg Med 49: 19-21.
-
Cheng H, Cheng C, Lin C, Tang J, Chu Y, et al. (2008) Caustic ingestion in adults: the role of endoscopic classification in predicting outcome. BMG Gastroenterol 8: 31.
-
Pike J, Patterson A, Arons M (1988) Chemistry of cement burns: pathogenesis and treatment. J Burn Care and Rehabil 9: 258-260.
-
Alexander W, Gohlan P, Greenwood J (2014) A ten-year retrospective analysis of cement burns in tertiary burn center. J Burn Care Res 35: 80-83.
-
Chung J, Kowal-Vern A, Latenser B, Lewis R 2nd (2007) Cement-related injuries: review of a series, the National Burn Repository, and the prevailing literature. J Burn Care Res 28: 827-834.
-
Feldberg L, Regan P, Roberts A (1992) Cement burns and their treatment. Burns 18: 51-53.
-
Poupon M, Caye N, Duteille F, Pannier M (2005) Cement burns: retrospective study of 18 cases and review of the literature. Burns 31: 910-914.
-
Wilson G, Davidson P (1985) Full thickness burns from ready-mixed cement. Burns Incl Therm Inj 12: 139-145.





