Clinical Medical
Reviews and Case Reports
A Case of Pyonephrosis of an Obstructed Atrophic Kidney
Fareeha Khan1,2*, Rasha Nakhleh3 and Theodore Suh1,2
1Department of Internal Medicine, Division of Geriatric & Palliative Medicine, University of Michigan, USA
2VA GRECC, Ann Arbor VA Hospital, Ann Arbor, USA
3Hurley Medical Center, Department of Internal Medicine, USA
*Corresponding author: Fareeha Khan, MD, MPH, Department of Internal Medicine, Division of Geriatric & Palliative Medicine, University of Michigan, Ann Arbor, MI, USA, E-mail: kfareeha@med.umich.edu
Clin Med Rev Case Rep, CMRCR-3-146, (Volume 3, Issue 12), Case Report; ISSN: 2378-3656
Received: October 17, 2016 | Accepted: December 10, 2016 | Published: December 12, 2016
Citation: Khan F, Nakhleh R, Suh T (2016) A Case of Pyonephrosis of an Obstructed Atrophic Kidney. Clin Med Rev Case Rep 3:146. 10.23937/2378-3656/1410146
Copyright: © 2016 Khan F, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
This case is of a 67-year-old male who presented to the office with multiple symptoms and was treated for a variety of infections before the correct diagnosis of pyonephrosis in the setting of chronic ureteropelvic junction (UPJ) obstruction was made.
Keywords
Pyonephrosis, Pyelonephritis, Chronic hydronephrosis, Obstructed
Introduction
Pyelonephritis is a common abdominal infection in the geriatric population. Pyonephrosis is a rare disease resulting in suppuration in the renal parenchyma. In other words, there is collection of purulent material in a "hydronephrotic" [1] renal collecting system [1]. It can also be referred to as an "obstructed infected kidney" [2].
Case
A 67-year-old male with a past medical history for diabetes mellitus, cognitiv¬¬¬e impairment and chronic sinusitis presented to the office with complaints of sinus congestion and was started on doxycycline. Around 5 days later he developed hematuria and was switched to amoxicillin for suspected urinary tract infection. Urinalysis was positive for trace leukocyte esterase, trace blood, 3+ protein and 1000 mg/dl glucose with negative nitrites and specific gravity of 1.020. Urine culture was negative. Lab workup revealed an elevated prostate specific antigen (PSA) level of 24.4 ng/ml. He returned to the clinic within 4 days with worsening symptoms of urinary urgency, incontinence, new onset diarrhea and fever. He denied dysuria but noted left sided flank pain. Examination was positive for left lower quadrant abdominal tenderness but no costovertebral angle tenderness. Based on symptoms of fever, left lower quadrant abdominal pain and diarrhea, he was started on ciprofloxacin and metronidazole as empiric treatment for suspected diverticulitis. Due to elevated PSA level there was concern for prostatitis or prostate cancer. Rectal exam did not reveal prostate tenderness or nodularity. He was referred to Urology and a cystoscopy was performed which was normal. He was scheduled for a prostate biopsy.
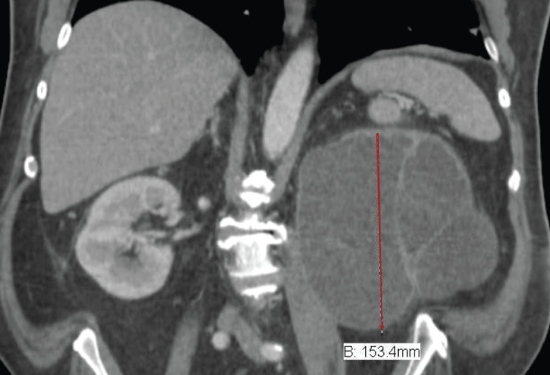
Imaging studies were also ordered; an abdominal computed tomography (CT) scan revealed multiple colonic diverticula with no adjacent inflammatory fat stranding, and significant left hydronephrosis with atrophic renal parenchyma likely secondary to long-standing left ureteropelvic junction obstruction. Urology team at the time felt that the hydronephrosis was chronic. Laboratory workup revealed leukocytosis at 11.0 K/uL, predominantly neutrophils, hemoglobin of 12.4 gm/dl, creatinine of 1.22 mg/dl and urea nitrogen of 24 mg/dl.
He was re-evaluated in the office around a week later with persistent symptoms of urinary incontinence, fever, diarrhea, left lower quadrant abdominal and flank pain, with additional symptoms of fatigue, decreased appetite and weight loss. Laboratory workup revealed leukocytosis at 14.2 K/uL, predominantly neutrophils, hemoglobin of 12.2 gm/dl, creatinine of 1.28 mg/dl and urea nitrogen of 25 mg/dl. A repeat urine culture was negative.
Patient was eventually admitted to the hospital for an inpatient workup due to worsening clinical condition. Laboratory results continued to worsen with leukocytosis at 20.4 K/uL, predominantly neutrophils, hemoglobin of 11.6 gm/dl, creatinine of 1.34 mg/dl and urea nitrogen of 33 mg/dl. Initial infectious workup including blood and urine cultures was negative. He was started on intravenous ceftriaxone and oral metronidazole for suspected diverticulitis. Infectious disease team was consulted and a sputum culture was ordered which was positive for pseudomonas sohe was switched to cefepime.
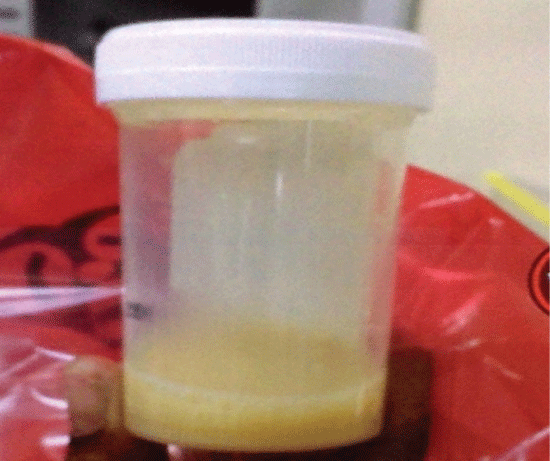
Over the next few days white blood cell (WBC) count was noted to be trending down and patient had been afebrile. However, he continued to have left sided abdominal pain. After repeated examinations a tender mass was palpated in the left lower quadrant. Previous records were obtained from an outside hospital; an abdominal CT scan from 2006 revealed contracted chronic pyelonephritic changes of left kidney with no hydronephrosis. There was concern that the hydronephrotic kidney may be the source of infection, based on the change in the CT scan reports between 2006 and 2015 and patient's current symptoms. After extensive discussions with infectious disease and urology teams, a ureteral stent was placed and thick yellow purulent urine was drained. Immediately after the procedure, patient's left sided abdominal and flank pain improved with resolution of leukocytosis. A repeat urine culture was negative.
Patient was continued on antibiotics post stent placement with complete resolution of his symptoms 2 weeks later. He was re-evaluated by Urology after 4 weeks and the stent was removed. Patient did well until 6 months later when his symptoms of abdominal pain and fever recurred; hence another stent was placed.
Since patient had presented with 2 similar episodes within 6 months, the decision was made to pursue a nephrectomy. He underwent a laparoscopic left nephrectomy 2 months later with no recurrence of his symptoms to date. Over the course of this time his PSA level gradually decreased to 3.01 ng/ml (Figure 1 and Image 1).
Discussion
Pyonephrosis results from acute or chronic obstruction due to stricture, stone, tumor or congenital UPJ obstruction. Patients can be asymptomatic or have a variety of symptoms including fever, flank or loin pain. Chronic pyelonephritic changes in the kidney involve renal scarring and atrophy with cortical thinning and dilatation of the collecting system [2].
Ultrasound, CT and MRI are modalities that can be used for detection. Debris in a dilated collecting system is noted and is the "most reliable sign of pyonephrosis" [2]. CT is the imaging of choice as it provides information about the hydronephrosis and its cause and severity. MRI in addition can differentiate between hydronephrosis and pyonephrosis, as the thick fluid in the later will result in restricted diffusion [2].
Treatment options range from percutaneous nephrostomy tube insertion to ureteric stenting. Flukes, et al. in their prospective analysis report 98% success rate with retrograde ureteric stenting while other authors have reported 98% success rate with percutaneous nephrostomy tube placements. However, with retrograde ureteric stenting there is a risk of instrumentation and potential spread of infection [3].
Patient in this case likely had chronic pyelonephritis of an atrophic kidney, ultimately resulting in pyonephrosis. He was treated for diverticulitis, prostatitis, sinusitis and urinary tract infection with multiple antibiotics over a 2 week time period, before the correct diagnosis of pyonephrosis, in the setting of chronic UPJ obstruction was made.
In a retrospective analysis of 25 patients, aged 32-78 years, Kirk, et al. noted that patients who underwent a nephrectomy for chronic pyonephrosis had presented with a multitude of symptoms ranging from anorexia, weight loss, tiredness, nausea, diarrhea, constipation, pain in legs, abdominal and loin pain. Incidental findings on workup lead to the true diagnosis [4].
Ashmore, et al. presented a case where there was no change in imaging over 1 month. However, based on clinical suspicion appropriate diagnosis was made and management was started, with complete resolution of symptoms. It is pertinent to have a high index of suspicion for pyonephrosis in symptomatic patients with hydronephrosis. It can lead to urosepsis and death if it goes undiagnosed or left untreated [5].
This case highlights the difficulty with diagnosis of chronic hydronephrosis/pyonephrosis in the geriatric population with multiple co-morbidities and multisystem presentation. These challenges often lead to delayed diagnosis and delayed treatment. In this case, serial WBC counts, CT scans, and review of this patient's presentation were helpful in finally determining the correct diagnosis. Series of urine cultures were negative, so cannot be relied on alone.
References
-
Ali Erol, Soner Çoban, Ali Tekin (2014) A Giant Case of Pyonephrosis Resulting from Nephrolithiasis. Case Reports in Urology 2014.
-
(2014) Grainger & Allison's Diagnostic Radiology. Common uroradiological referrals, 850.
-
Flukes S, Hayne D, Kuan M, Wallace M, McMillan K, et al. (2015) Retrograde ureteric stent insertion in the management of infected obstructed kidneys. BJU Int 115: 31-34.
-
Kirk D, Roberts JB, Feneley RC, Gingell JC, Smith PJ (1983) Extraurinary manifestations of chronic pyonephrosis. Journal of the Royal Society of Medicine 76: 740-742.
-
Ashmore AE, Thompson C (2016) Pyelonephritis and obstructive uropathy: a case of acute kidney injury. BMJ Case Rep.