Clinical Medical
Reviews and Case Reports
Percutaneous Coronary Intervention for Single Coronary Artery: Two Case Studies
Yang Zhuo, Yu-qi Fan, Zhao-fang Yin, Li Fan, Zhi-hua Han, Chang-qian Wang* and Zuo-jun Xu
Department of Cardiology, Shanghai Jiaotong University School of Medicine, China
*Corresponding author: Chang-qian Wang, Department of Cardiology, Shanghai Ninth People's Hospital, Shanghai Jiaotong University School of Medicine, Shanghai 200011, China, E-mail: changqianwang@hotmail.com
Clin Med Rev Case Rep, CMRCR-3-138, (Volume 3, Issue 11), Case Series; ISSN: 2378-3656
Received: July 09, 2016 | Accepted: November 07, 2016 | Published: November 09, 2016
Citation: Zhuo Y, Yu-qi F, Zhao-fang Y, Fan L, Zhi-hua H, et al. (2016) Percutaneous Coronary Intervention for Single Coronary Artery: Two Case Studies. Clin Med Rev Case Rep 3:138. 10.23937/2378-3656/1410138
Copyright: © 2016 Zhuo Y, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Single coronary artery (SCA), a congenital and rare anomaly, is defined as a coronary artery arising from the sinus of valsalva and supplying the entire heart. According to modified Lipton's classification criteria, L-1 subtype is the rarest type of SCA. Here we present two L-I subtype cases. In case one, one of the side branches from the first septal artery proceeded as the right coronary artery (RCA). In case two, the distal septal artery and distal circumflex artery together served as the RCA. Both two patients underwent percutaneous coronary intervention because of unstable coronary artery disease.
Keywords
Coronary angiography, Percutaneous coronary intervention, Single coronary artery
Single coronary artery (SCA) is a congenital and rare anomaly, which is defined as a coronary artery that arises from the sinus of valsalva and supplies the entire heart. Relevant literatures have reported that detection of anomalous origin coronary in people who underwent with the coronary angiography was 0.3%-1.2% [1-3]. Yanamaka [1] reports that in a large-scale epidemiological survey (N = 126595), patients with anomalous coronary artery were 1686 cases (1.3%), including coronary origin or abnormal distribution (87%) and abnormal termination (coronary artery fistula, 13%). The rate of detection was 0.0044% in single right coronary artery and 0.022% in left single coronary. In China, Wu Ying [4] reports that in 22636 patients, the rate of anomalous coronary artery was 1.03%. Majority of SCA anomalies are benign and asymptomatic. However, life-threatening symptom can occur in minority of patients [1]. We report here two cases SCA classified as Lipton L-I subtype (anomalous origin of the right coronary artery).
Patient Information
Case one
Without history of diabetes, hypercholesterolemia or hypertension, a 56-years-old male who had been smoking for 40 years was referred to our cardiac center. He complained of recurrent chest pain for 10 years and aggravating symptom for a week. His chest pain episodes used to last for several minutes with intervals of a week. But he suffered from several episodes of chest pain last week, and each episode continued for more than half an hour. The baseline ECG was normal. The echocardiography revealed no hypokinesis of all ventricular walls and the left ventricular ejection fraction was 65%. The cardiac bio-markers of Troponin and CKMB were normal. He was diagnosed as unstable angina and was subjected to CAG two days later after admission.
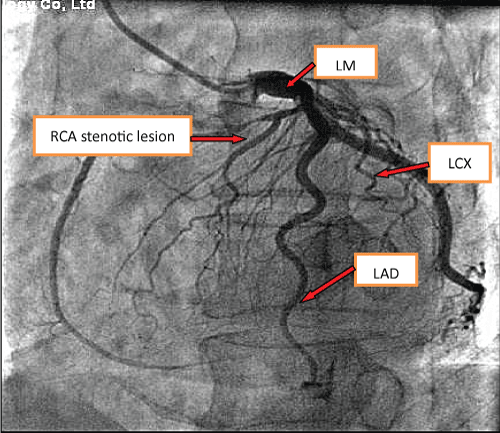
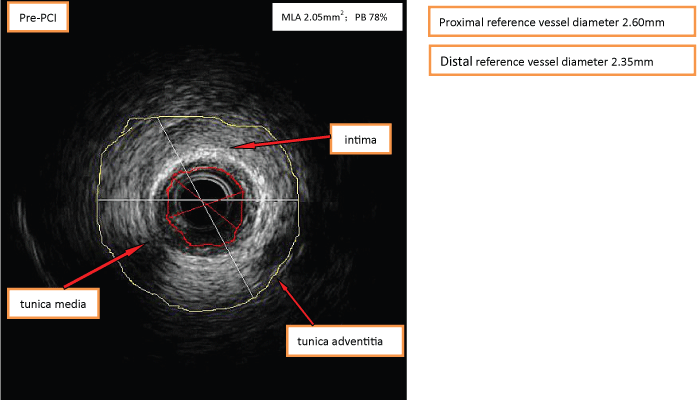
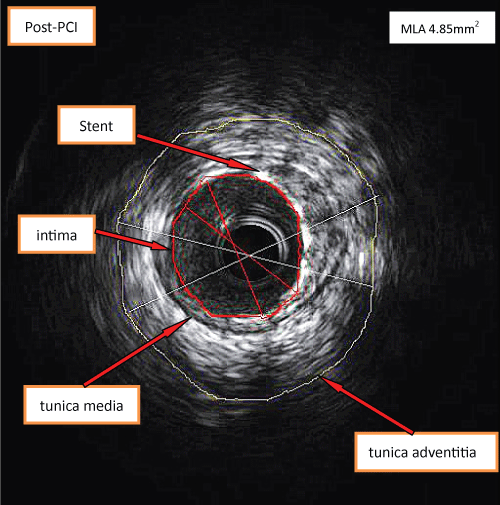
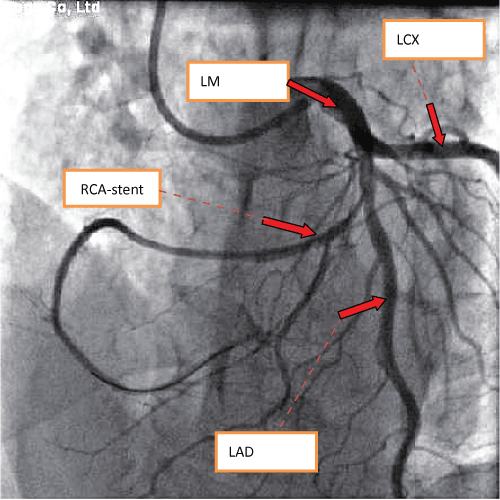
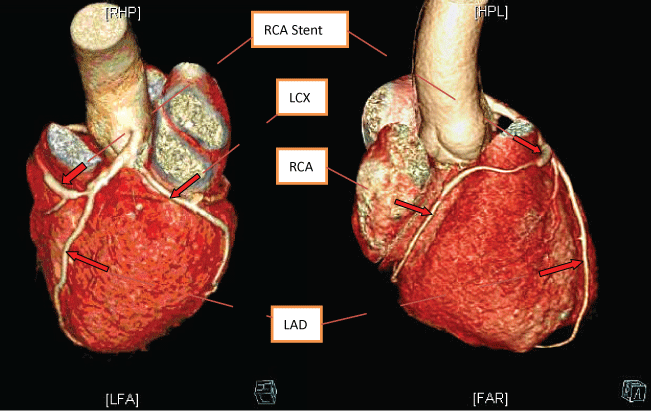
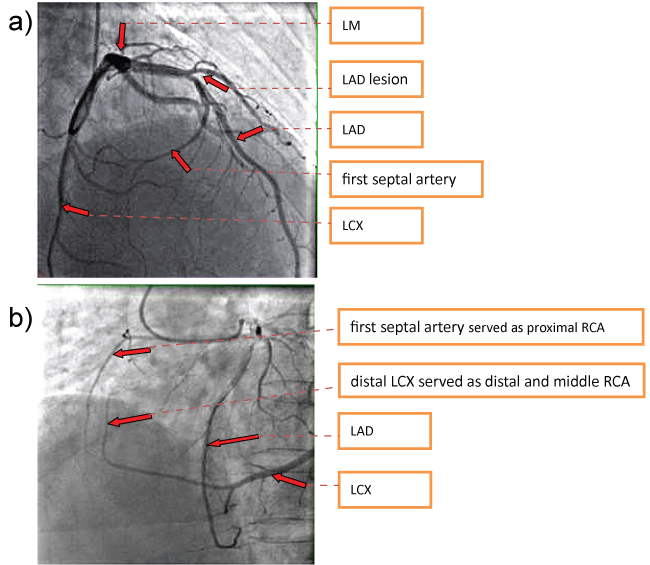
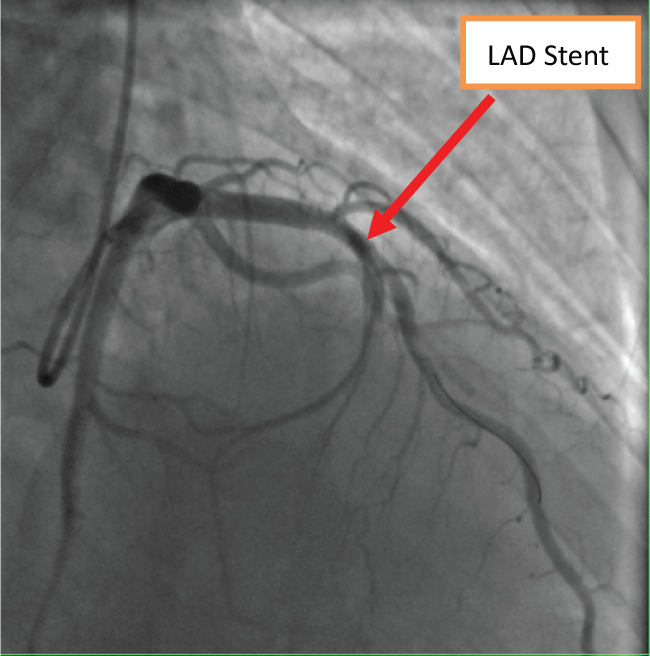
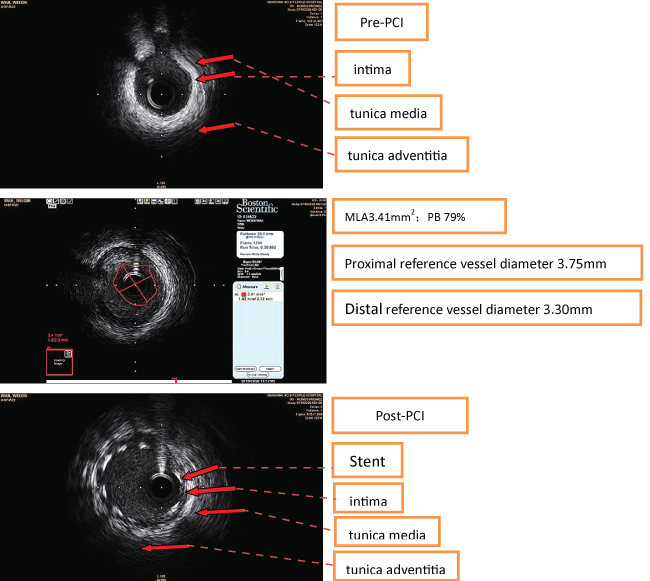
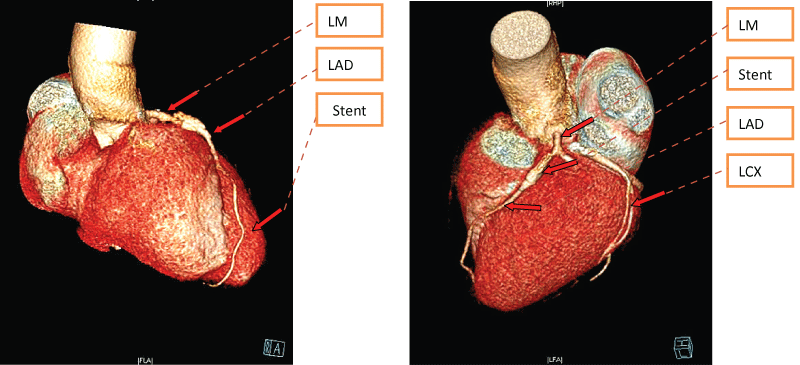
The CAG revealed an absence of the right coronary ostium with an isolated single left coronary artery arising from the left sinus of valsalva. The left main trunk divided into the left anterior descending (LAD) and left circumflex (LCX) arteries normally. At the proximal portion of first septal artery, it divided into two side branches. One branch proceeds as the right coronary artery (RCA) (Figure 1). At the proximal "RCA", a severe stenosis was observed. Intravascular ultrasound (40 MHz, Boston, USA) was performed subsequently, which showed a minimal lumen area of 2.05 mm2, plaque burden with 78% (Figure 2a and Figure 2b). The intima of RCA was complete, and the 3-layer's structure (intima, tunica media, tunica adventitia and tunica adventitia surrounding tissue) was clear (Figure 2a and Figure 2b). One stent (Xience Prime Drug-Eluting Stent 2.25 × 18 mm, Abbott, USA, released at 14 atm) was implanted (Figure 3). Post dilation was performed with Sprinter NC (2.5 mm × 12 mm, release at 14-16 atm). Two days after PCI, the patient undertook a 64-slice coronary computed tomography (MSCT, GE, USA) test, which further confirmed the absence of the right coronary ostium, as shown in figure 4. Seven days after PCI, the patient was discharged with dual anti-platelet therapy (Aspirin 100 mg/day, Clopidogrel 75 mg/day). In 12 months' follow-up, the patient did not suffer from any chest pain.
Case two
A 62-years-old male patient was admitted due to recent onset and multiple episodes of chest pain for a week. He had a history of hypertension but no history of diabetes, stroke, or smoking. EKG result was normal. Laboratory tests did not show any significant alterations of cardiac biomarkers. No segmental ventricular wall movement disorder was observed in echocardiogram. LVEF was 65%. He was diagnosed as unstable angina and subjected to CAG. Coronary angiography showed that right coronary artery was congenitally absent. A single left coronary artery aroused from the left sinus of valsalva (Figure 5a and Figure 5b). The left main trunk divided into the left anterior descending (LAD) and left circumflex (LCX) arteries normally. The first septal artery crossed to the right anterior ventricle and proceeded as the proximal right coronary artery (RCA). The distal LCX proceeded into the left posterior atrioventricular groove and went on to the crux of the heart. Which served as posterior descending artery (PDA) and distal/middle RCA (Figure 5a and Figure 5b). There was a severe stenosis in the proximal LAD, which located in the ostia of the first septal arteries. Intravascular ultrasound (40 MHz, Boston, USA) showed a minimal lumen area of 2.05 mm2, plaque burden of 79% in LAD lesion. The 3-layer's anatomical structure of "RCA" was normal. One stent (Abbott, Inc. Xience Prime Drug-Eluting Stent 4.0 × 18 mm, 12 atm release) was implanted (Figure 6). Post-dilation was performed (Quantum 4.5 mm × 12 mm, released at 16 atm). CTA after coronary angiography confirmed the absence of right coronary artery from the right coronary sinus. The patient was discharged without the symptom of chest pain. Coronary angiography result shown in figure 5, PCI in figure 6, IVUS in figure 7, the coronary CTA in figure 8.
Discussion
Single coronary artery, with or without other congenital heart diseases, is a rare congenital cardiovascular malformation. The presumable mechanism of SCA is embryonic artery developing disorder or congenital coronary artery occlusion. Arteagad [5] demonstrates that the detection of single coronary in people who has undergone CAG were 0.024%-0.09%. In recent years, more cases have been reported about the congenital absence of right coronary artery.
CTA is very important in determining the diagnosis and treatment strategy of SCA cases. Our two cases, according to Lipton typing methods [6], were LI type single coronary artery malformation. Such patients may develop atherosclerosis, angina, myocardial infarction, congestive heart failure, arrhythmias, syncope and sudden death [1]. In both two cases, considering the possibility of RCA CTO, we performed CTA. As we can't see any sign of the ostium of RCA form the right valsava, we believed that the possibility of RCA CTO was extremely rare and these two cases should be Lipton I type SCA. To the best of our knowledge, these kinds of anomaly are extremely rare. Furthermore, our CTA results ruled out the possibility of those "RCA" running between the aorta and the pulmonary artery, which favored coronary artery bypass over PCI to prevent the stent from being crushed after implantation.
In both cases, we performed left coronary angiography immediately when we discovered the possibility of absence of the RCA. This action avoided blindly repetition of angiography and extensive use of contrast agents.
Currently, ESC and AHA coronary intervention guidelines do not have the specific instruction for malformed coronary intervention strategies. In these cases, FFR may be a better strategy to determine the functional stenosis. However, because of the economic burden, our patients refused the FFR examination (FFR expense was not covered by their insurance policies, but CAG, IVUS PCI were.). Thus, we performed IVUS to direct our PCI procedure. First, IVUS provided more details of the stenotic lesion (MLA, reference vessel diameter, stene diameter, stent length). Second, IVUS helped to determine whether the structure of those "RCAs" were normal or not. Congenital RCA malformations may lead to the abnormality of artery wall structure, which is characterized as being weak and defective. For those patients, interventionists should always be cautious of the releasing pressure of balloon and stent to avoid the dissection or rupture of blood vessels. With the direction of IVUS, the stents were implanted successfully (released at 14 atm). In 12 months' follow-up, both 2 patients survived well without suffering from chest discomfort. Interestingly, two similar cases have been reported in which RCA origined from left coronary artery and PCI was performed [7,8].
In conclusion, we present two rare cases of SCA underwent PCI under the guidance of IVUS. Although the prevalence of SCA is low, performing intervention of a SCA is challenging for cardiologist. Severe complications may be catastrophic. Without established treatment guidelines, proper appraisal of coronary artery, selection of instruments, and adequate expertise of the operator are crucial to perform this kind of intervention.
References
-
Yamanaka O, Hobbs RE (1990) Coronary artery anomalies in 126,595 patients undergoing coronary arteriography. Cathet Cardiovasc Diagn 21: 28-40.
-
Kardos A, Babai L, Rudas L, Gaál T, Horváth T, et al. (1997) Epideniology of congenital coronary artery ananalies a coronary arte-riography study on a central European population. Cathet Cardiovasc Diagn 42: 270-275.
-
Garg N, Tewari S, Kapoor A, Gupta DK, Sinha N (2000) Primary congenital anomalies of the coronary arteries a coronary arteriographic study. Int J Cardiol 74: 39-46.
-
WU Ying, YAO Min, GAO Run-lin (2004) Analyses of anomalies origin of coronary artery in 22636 adult patients undergoing coronary arteriography. Chin J Cardiol 32: 587-591.
-
Arteaga RB, Tronolone J, Mandawat M (2006) Single coronary ostium a right coronary artery arising from the left main coronary artery. J Invasive Cardiol 18: 241-243.
-
Lipton MJ, Barry WH, Obers I, Silverman JF, Wexler L (1979) Isolated single coronary artery: diagnosis, angionosis, angiographic classification and clinical signification. Radiology 130: 39-47.
-
Diana R, Nikola T, Boris S (2010) Percutaneous coronary intervention of an anomalous right coronary artery originating from the left coronary artery. Wien Klin Wochenschr 122: 508-510.
-
Jian D, Osamu K, Eisho K, Xun JZ (2014) Percutaneous intervention in a patient with a rare single coronary ar-tery from the left coronary sinus of valsava. J Res Med Sci 19: 375-377.