Clinical Medical
Reviews and Case Reports
Pseudoxanthoma Elasticum: An Unusual Cause of Hypertension in Child. About Three Cases Reports
A Dibi1*, M ElFahime2, N Mouane3, R Dafiri4 and A Bentahila1
1Pediatric IV service, Children's Hospital, Mohamed V University, Morocco
2Biological analysis Service/PGF/UATRS/CNRST, 10102 Rabat, Morocco
3Pediatric III service, Children's Hospital, Mohamed V University, Morocco
4Pediatric Radiology service, Children's Hospital, Mohamed V University, Morocco
*Corresponding author: Asmaa Dibi, Pediatrician, Pediatric Cardiology Unit, Children's Hospital, Mohamed V University, Rabat, Morocco, Tel: 00212661205221, E-mail: asmaadibi@gmail.com
Clin Med Rev Case Rep, CMRCR-3-129, (Volume 3, Issue 9), Case Series; ISSN: 2378-3656
Received: July 08, 2016 | Accepted: September 06, 2016 | Published: September 10, 2016
Citation: Dibi A, ElFahime M, Mouane N, Dafiri R, Bentahila A (2016) Pseudoxanthoma Elasticum: An Unusual Cause of Hypertension in Child. About Three Cases Reports. Clin Med Rev Case Rep 3:129. 10.23937/2378-3656/1410129
Copyright: © 2016 Dibi A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: Pseudoxanthoma elasticum (PXE), is an heritable multisystem disorder. PXE patients seem to develop cardiovascular events and complications, at a younger age than the normal population. We report three pediatrics cases of hypertension reveled Pseudoxanthoma elasticum.
Case report 1: A 11-years-old boy was hospitalized for haematemesis. Clinical examination found a high blood pressure ranging at 170/90 mmHg. Renin activity was very high at 1825 mIU/l. The genetic study has identified 2 ABCC6 mutations in the composite state, what has allowed to confirm the diagnosis of PXE.
Case report 2: A 6-years-old girl was hospitalized for haematemesis. The clinical examination showed a high blood pressure at 160/90 mmHg and a skin lesions punctiform yellowish at the side of the neck. Renin activity was high at 1042 mIU/l. The genetic study has identified an homozygous mutation of ABCC6 gene confirming the diagnosis of PXE.
Case report 3: A 8-years-old girl was presented seizures complicated by coma. Clinical examination found a high blood pressure at 160/100 mmHg. The brain scan showed diffuse cerebral calcifications with parenchymal ischemic lesions. Renin activity was high at 2150 mIU/l. The patient kept neurological sequelae with extrapyramidal syndrome and appearance during evolution yellowish skin lesions. The genetic study found a mutation of ABCC6 gene in exon 28 confirming the diagnosis of PXE.
Conclusion: Despite the rarity of this pathology, one must be aware of the need for early diagnosis in child, for adequate handling and better management of the associated complications, making periodical cardiovascular follow-ups imperative.
Keywords
Pseudoxanthoma elasticum, Arterial hypertension, Vascular calcification, ABCC6 gene, Child
Introduction
Pseudoxanthoma elasticum (PXE; OMIM 264800, prevalence 1/25000 to 1/50000) is a multisystem disorder [1] and an autosomal recessive disease resulting from mutations in ABCC6 (ATP-binding cassette subfamily C member 6) that encodes an ATP-binding cassette transporter mainly expressed in the liver and kidneys [2-4]. Mutations in the ABCC6 gene are demonstrated in about 90% of patients who are genotyped [5]. It characterized by aberrant mineralization of soft connective tissue resulting in fragmentation of elastic fibers, involving primarily the skin, eyes and cardiovascular system [6]. PXE patients therefore seem to develop cardiovascular events and complications at a younger age than the normal populational though without obvious cardiovascular risk factors [7,8]. We report in this work three pediatric cases of hypertension revealing a PXE.
Case Report 1
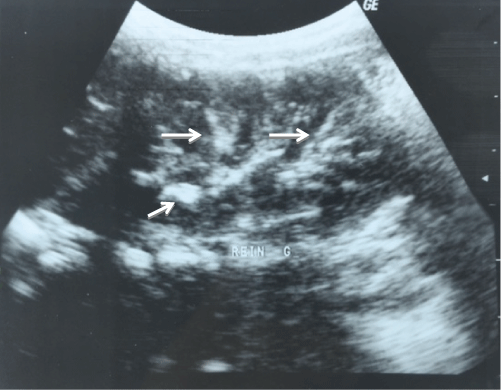
A 11-years-old moroccan boy, from a non-consanguineous marriage. Without family history of hypertension. He was hospitalized for haematemesis. Clinical examination found a constant high blood pressure ranging between 150/80 and 170/90 mmHg. The skin examination was normal and the rest of the clinical examination. Complete blood count showed anemia to 10.4 g/dl. The phosphate balance and renal function were normal. Renin activity was very high at 1825 mIU/l (2.8-39.9 mIU/l). Upper gastrointestinal endoscopy showed a hemorrhagic gastrointestinal bulbite. Abdominal ultrasound showed diffuse linear calcifications in the kidneys (Figure 1), spleen and pancreas. Cervical ultrasound also revealed calcification of both parotid gland and right maxillary gland. Echocardiography showed hyperechoic pillars and a moderate left ventricular hypertrophy. Ophthalmologic examination with retinal angiography revealed bilateral retinal hemorrhage with superficial presence angioid streaks. Renal arteriography didn’t show any vascular obstruction. The patient was put under omeprazole. Clinical course was marked by the bleeding stops. The equilibration of the blood pressure was obtained by nicardipine, captopril, and Atenolol. The genetic study has identified 2 ABCC6 mutations in the composite state: c.2263G > A (p.G755R) on exon 18 and c.3421C > T (pR1141X) in exon 24, what has allowed to confirm the diagnosis of PXE.
Case Report 2
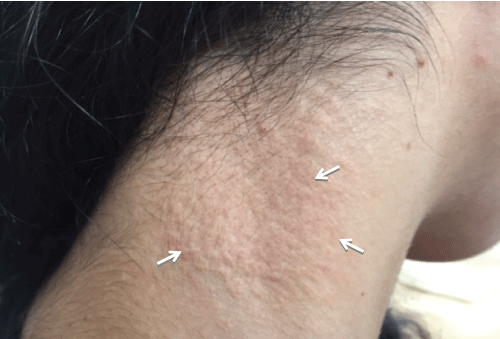
A 6 years old moroccan girl, from a consanguineous marriage, without family history of hypertension. She was hospitalized for haematemesis. The clinical examination showed a high blood pressure at 160/90 mmHg, the rest of the clinical examination was normal. The blood count showed anemia to 9.8 g/dl. The phospho-calcium balance was normal, the hemostasis tests were normal and the renal function were normal. The gastroesophageal endoscopy showed no mucosal lesions. Abdominal ultrasound showed diffuse linear calcifications in the kidneys and spleen (Figure 2). Echocardiography found hypertrophy of the left ventricle. Ophthalmologic examination was normal. Renin activity was high at 1042 mIU/l (2.8-39.9 mUI/l). Renal arteriography was normal. Normalization of blood pressure was provided by nicardipine and captopril. And she was put under Omeprazole. During evolution, there was the appearance of skin lesions punctiform yellowish at the side of the neck (Figure 3). That is why the genetic study was performed and has identified the homozygous mutation c.4021G > A, R1164Q on exon 24 of the ABCC6 gene, thus confirming the diagnosis of PXE.
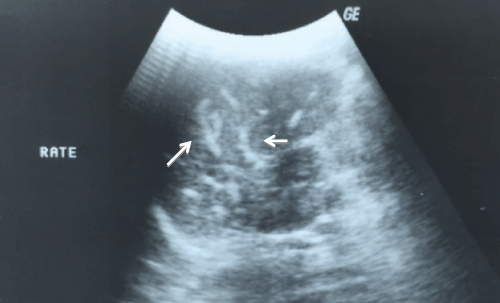
.
Figure 2: Abdominal ultrasound showed diffuse linear calcifications in the spleen in case 3.
View Figure 2
Case Report 3
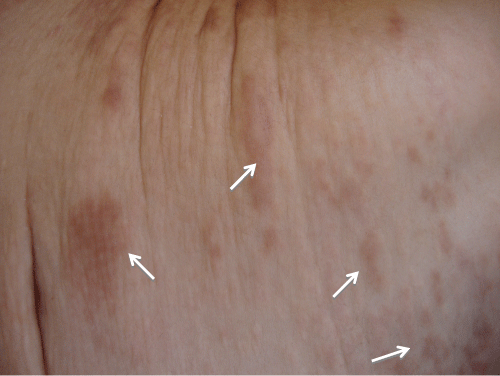
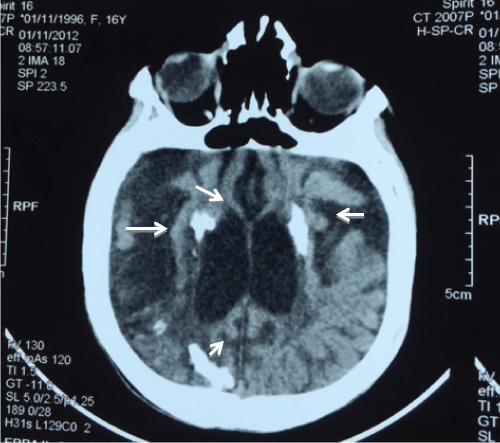
A 8-years-old moroccan girl, from a consanguineous marriage, without family history of hypertension. She was presented seizures complicated by coma with a high blood pressure at 160/100 mmHg. The blood count showed anemia to 9.4 g/dl, the hemostasis tests were normal, the phospho-calcium balance was normal, and the renal function were normal. The brain scan showed diffuse cerebral calcifications with parenchymal ischemic lesions (Figure 4). Abdominal ultrasonography showed linear calcification in the spleen, pancreas (Figure 5), parotid gland, submandibular and the kidneys. Echocardiography showed a concentric hypertrophic cardiomyopathy of the left ventricle with preserved ventricular function (Figure 6), and a hyperechoic appearance of the mitral valve and pillars. The upper gastrointestinal endoscopy was normal. Ophthalmologic examination was normal. Renin activity was high at 2150 mIU/l (2.8-39.9 mUI/l). Renal arteriography could not be done. Blood pressure was balanced by anti hypertensive treatment with nicardipine, captopril and Atenolol. However the patient kept neurological sequelae with extrapyramidal syndrome and gradual appearance of yellowish skin lesions increasing in size in the trunk with excess skin (Figure 7). In this context the skin biopsy was not performed. The genetic study found an homozygous mutation of ABCC6 gene in exon 28: c.4016G > A, R1339Q confirming the diagnosis of PXE.
.
Figure 4: Brain scan showed Diffuse cerebral calcifications with parenchymal ischemic lesions in case 3.
View Figure 4
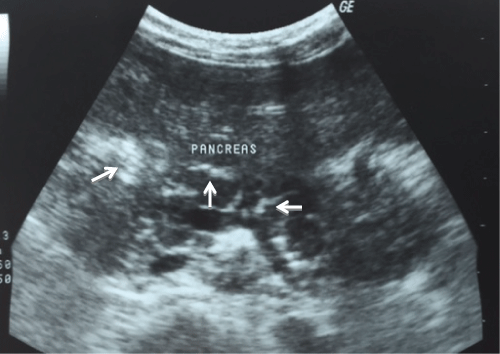
.
Figure 5: Abdominal ultrasound showed linear calcification in the pancreas in case 3.
View Figure 5
Discussion
In most cases the diagnosis of PXE is based on the combination of cutaneous and ophthalmologic findings. The main dermatological features include yellowish papules and loss of skin elasticity as that we found in cases 2 and 3. Eye lesions consist of angioid streaks which often lead to retinal hemorrhages and the loss of central vision.
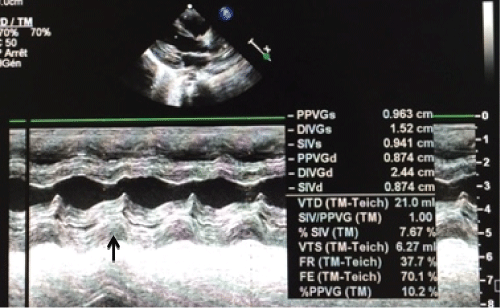
.
Figure 6: Echocardiography showed concentric hypertrophic cardiomyopathy of the left ventricle with preserved ventricular function in case 3.
View Figure 6
PXE has been associated with an increased risk of several cardiovascular complications including hypertension, intermittent limb claudication, mitral valve prolapse or stenosis, coronary artery disease, stroke, and sudden death [9,10]. Most PXE patients do not experience cardiovascular problems before their third or fourth decade, however onset as early as 9 years has been described [11].
Renovascular hypertension has been reported in 25% of patients with PXE and commonly occurs in adults. There are few reports of hypertension in children [12]. Due to calcification of the interlobar and arcuate arteries a characteristic pattern of dotted increased echogenicity is seen in the corticomedullary junction by renal ultrasonogoraphy. This increased echogenicity can also be seen in the spleen, pancreas and others organsas in our patients. The increased renin activity was likely explained on the basis of a renal artery stenosis or increased arterial stiffness. However the impact of calcification and elastic fiber fragmentation on arterial stiffness in PXE is unclear.
It was suggested a complex and unique remodeling of the arterial wall including possible changes in vascular reactivity or at least changes in local blood flow supply. However to date, the impact of ABCC6 deficiency on arterial reactivity especially in the small sized vasculature remains largely unknown [13]. Unspecific microangiopathy has been reported in the finger microcirculation [14] but over clinical microcirculatory abnormalities have not yet been reported in this context. Our patients did not have vascular obstruction on renal arteriography; it is possible that in the early stages of the disease changes are undetectable by conventional imaging.
To this day there is no specific treatment and the therapeutical management is based in prevention, tracking and monitoring of complications associated with the disease. Complementary exams such as blood count, lipid profile, echocardiogram, and ophthalmologic monitoring should be made during follow-up of these patients.
Conclusion
Despite the rarity of this pathology, one must be aware of the need for early diagnosis in child for adequate handling and better management of the associated complications, making periodical cardiovascular follow-ups imperative.
Conflict of Interest
None.
References
-
Marconi B, Bobyr I, Campanati A, Molinelli E, Consales V, et al. (2015) Pseudoxanthoma elasticum and skin: Clinical manifestations, histopathology, pathomechanism, perspectives of treatment. Intractable Rare Dis Res 4: 113-122.
-
Li Q, Jiang Q, Pfendner E, Varadi A, Uitto J (2009) Pseudoxanthoma elasticum: clinical phenotypes, molecular genetics and putative pathomechanisms. Exp Dermatol 18: 1-11.
-
Scheffer GL, Hu X, Pijnenborg AC, Wijnholds J, Bergen AA, et al. (2002) MRP6 (ABCC6) detection in normal human tissues and tumors. LabInvest 82: 515-518.
-
Belinsky MG, Kruh GD (1999) MOAT-E (ARA) is a full-length MRP/cMOAT subfamily transporter expressed in kidney and liver. Br J Cancer 80: 1342-1349.
-
Pfendner EG, Uitto J, Gerard GF, Terry SF (2008) Pseudoxanthoma elasticum: Genetic diagnostic markers. Expert Opin Mol Diagn 2: 63-79.
-
Uitto J (2012) Rare heritable skin diseases: Targets for regenerative medicine. J Invest Dermatol 132: 2485- 2488.
-
Donas KP, Schulte S, Horsch S (2007) Balloon angioplasty in the treatment of vascular lesions in pseudoxanthoma elasticum. J Vasc Interv Radiol 18: 457-459.
-
Leftheriotis G, Kauffenstein G, Hamel JF, Abraham P, Le Saux O, et al. (2014) The Contribution of Arterial Calcification to Peripheral Arterial Disease in Pseudoxanthoma Elasticum. PLoS One 9: e96003.
-
Mendelsohn G, Bulkley BH, Hutchins GM (1978) Cardiovascular manifestations of Pseudoxanthoma elasticum. Arch Pathol Lab Med 102: 298-302.
-
Prunier F, Terrien G, Le Corre Y, Apana ALY, Bière L, et al. (2013) Pseudoxanthoma Elasticum: Cardiac Findings in Patients and Abcc6-Deficient Mouse Model. PLoS One 8: e68700.
-
Schachner L, Young D (1974) Pseudoxanthoma elasticum with severe cardiovascular disease in a child. Am J Dis Child 127: 571-575.
-
Eskim M, Tumer N, Atmaca L, Anadolu R, Salih M, et al. (1998) Pseudoxanthoma elasticum: a rare cause of hypertension in children. Pediatr Nephrol 12: 183-185.
-
Kauffenstein G, Pizard A, Le Corre Y, Vessières E, Grimaud L, et al. (2014) Disseminated Arterial Calcification and enhanced myogenic response are associated with abcc6 deficiency in a mouse model of pseudoxanthoma elasticum. Arterioscler Thromb Vasc Biol 34: 1045-1056.
-
Perdu J, Champion K, Emmerich J, Fiessinger JN (2004) Microvascular involvement in pseudoxanthom aelasticum. Capillaroscopic findings. Presse Med 33: 518-521.