Clinical Medical
Reviews and Case Reports
Variant Angina Induced Life-Threatening Ventricular Arrhythmias: does Dual Calcium Channel Blocker Eliminates the Indication for Implantable Cardioverter Defibrillator?
Maroun Matar1*, Elie Chammas2 and Samer Nasr3
1PGY III internal medicine resident, Lebanese University, Lebanon
2Lebanese Society of Cardiology, Division of Cardiology, Lebanese University, Lebanon
3Department of Cardiology, Mount Lebanon Hospital, Lebanon
*Corresponding author: Maroun Matar, PGY III internal medicine resident, Lebanese University, Lebanon, E-mail: matar.g.maroun@gmail.com
Clin Med Rev Case Rep, CMRCR-3-111, (Volume 3, Issue 6), Case Report; ISSN: 2378-3656
Received: May 09, 2016 | Accepted: June 22, 2016 | Published: June 24, 2016
Citation: Matar M, Chammas E, Nasr S (2016) Variant Angina Induced Life-Threatening Ventricular Arrhythmias: does Dual Calcium Channel Blocker Eliminates the Indication for Implantable Cardioverter Defibrillator?. Clin Med Rev Case Rep 3:111. 10.23937/2378-3656/1410111
Copyright: © 2016 Matar M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Introduction
Variant angina (Prinzmetal's angina, periodic angina) is characterized by episodic recurrent chest pain that usually occurs spontaneously and is accompanied by transient ST-segment elevation. The prognosis of variant angina is usually excellent in patients who receive medical therapy. However, a prolonged vasospasm may result in complications such as myocardial infarction (MI), high degree atrio-ventricular (AV) block, life-threatening ventricular tachycardia/fibrillation (VT/VF), or sudden cardiac death (SCD) [1,2] challenging therefore the treatment that can range from simple calcium channel blockers with or without concomitant nitrate therapy [3] to dual calcium channel blockers of different classes [4] and ultimately to implantable cardioverter defibrillator (ICD) or pacemaker installation to prevent SCD and life-threatening arrhythmias.
The current guidelines [5] are silent with respect to use of an ICD in patients with coronary artery vasospasm. Although the results of the report of Matsue et al. [6] support the use of ICD therapy in patients with coronary artery vasospasm who have survived an episode of life-threatening VT/VF.
We report a case of coronary artery spasm induced long QT with ICD terminated recurrent ventricular fibrillation, that resolved once a second calcium channel blocker was added to the treatment.
Case Report
A 49-year-old white female tailor that works for a subcontractor at Clemenceau medical center, had in 25/10/2010, a severe substernal chest pain with left shoulder and bilateral arm pain, followed by near collapse. Nursing staff at the hospital who is very well acquainted with her, since she is an extremely gentle person, rushed and connected her to a monitor that showed a polymorphic ventricular tachycardia followed by ventricular fibrillation. Electrical cardioversion with 100 joules biphasic shockwas done and normal sinus rhythm restored.
.
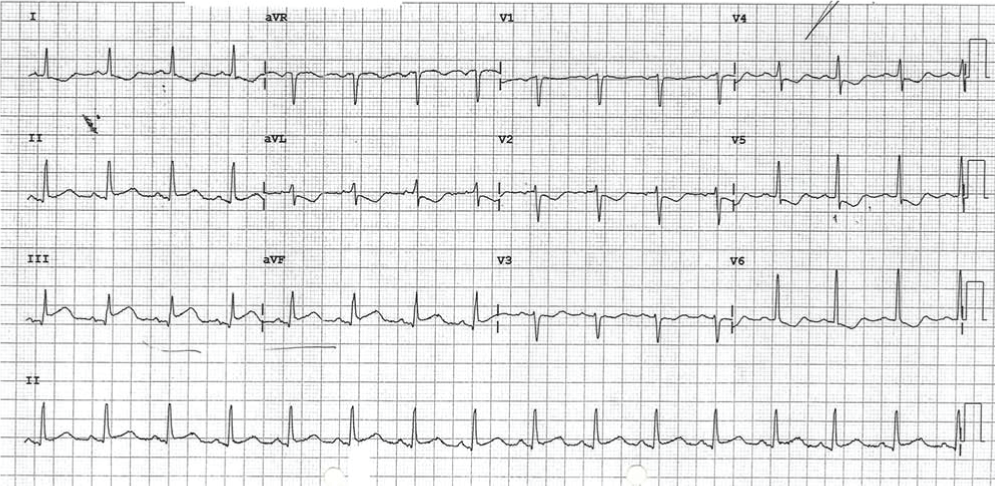
Figure 2: EKG post cardioversion 25/10/10 at 07:49:16 am. The patient still having chest pain. ST elevation in leads II, III, aVF QTc 498 msec. Cardiac enzymes were negative.
View Figure 2
Her past medical history is significant for a similar episode one year ago. At that time she had chest pain, and contacted her cardiologist who asked her to come to the hospital for check up and to undergo an exercise stress test since she had no risk factors. She presented an hour later to emergency department with a cardiac arrest that was appropriately resuscitated. Echocardiogram, cardiac catheterization was normal. Severe vasospasm diagnosed and she was started on calcium blockers, nitrates, and antiplatelet agents and did well during the interim period.
.
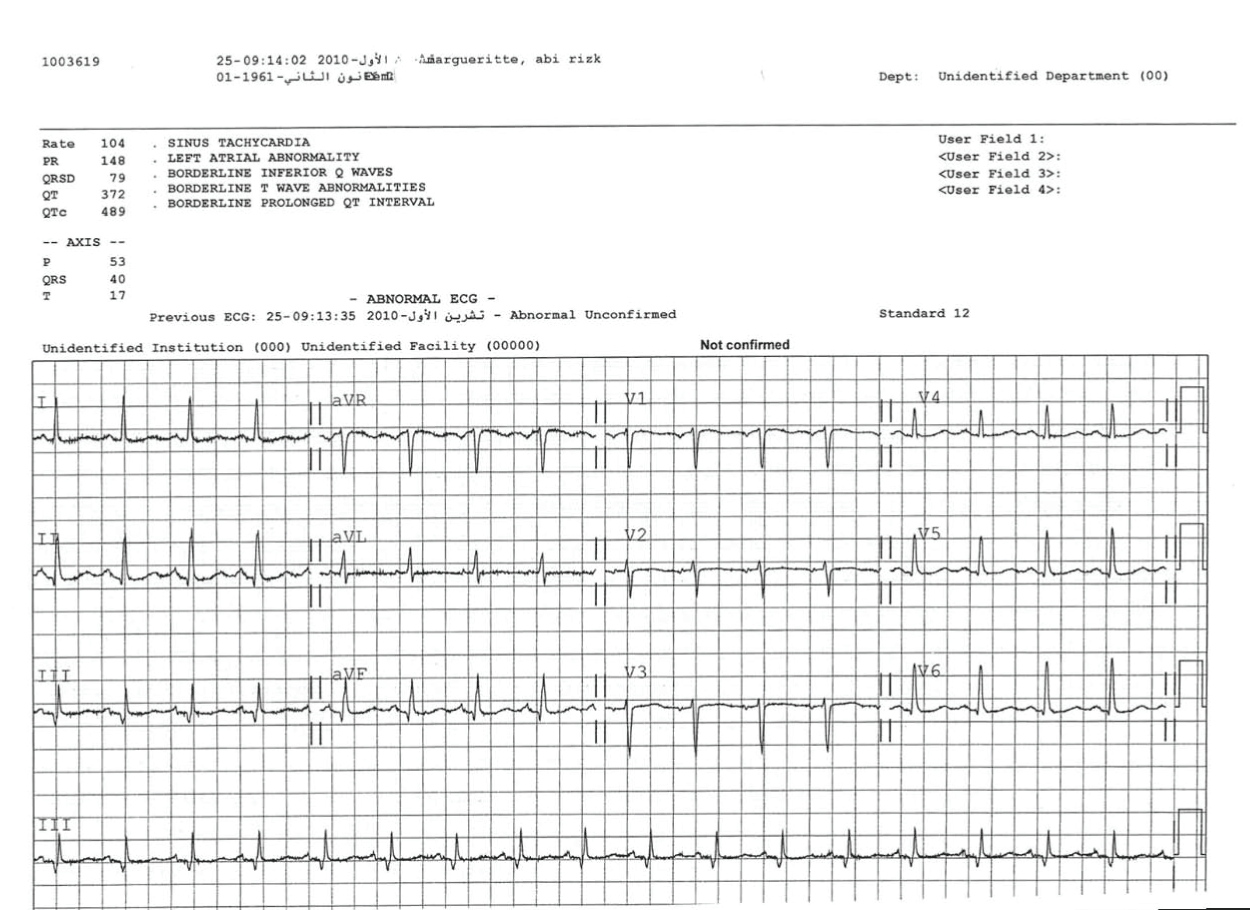
Figure 3: EKG at 09:14:02 am. Resolution of chest pain and ST elevation in inferior leads. QTc 489 msec.
View Figure 3
.
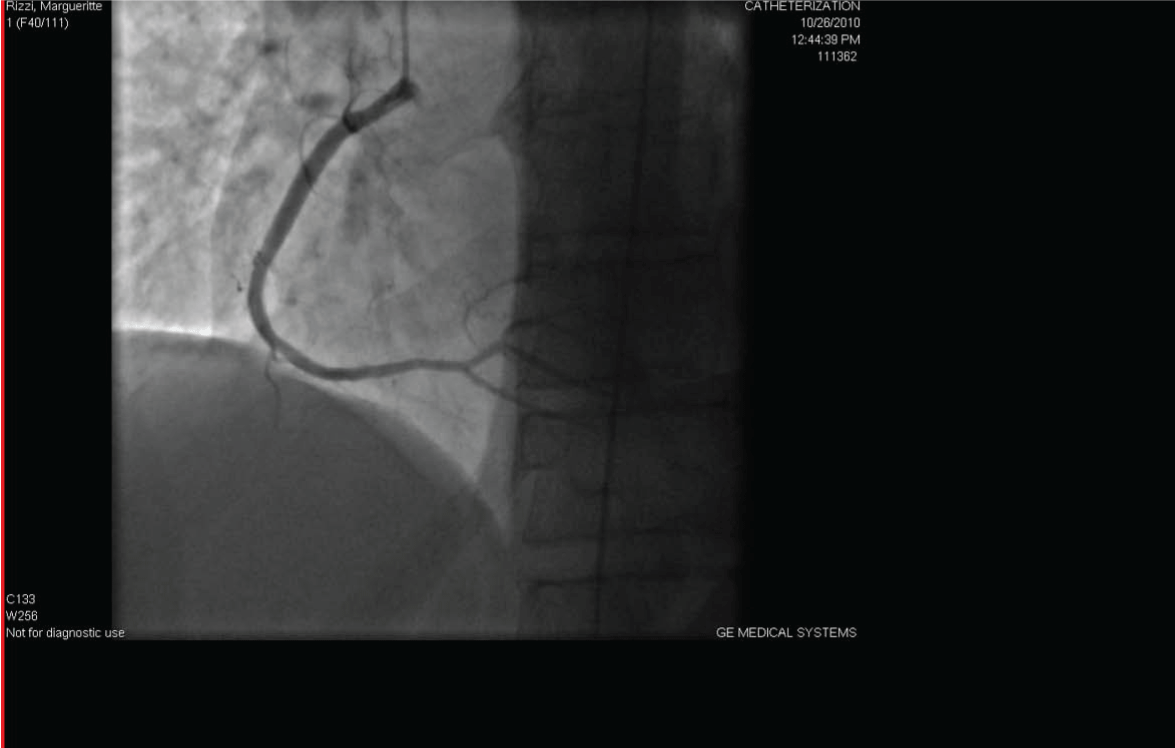
Figure 4: Cardiac catheterization was done and did not reveal any significant stenosis.
View Figure 4
She is on Amlodipine 5 mg once daily, Molsidomine 4 mg TID and Aspirin 100 mg once daily. Family history is significant for an aunt from her father's side that died at age 22 with an unknown cause. She has no known allergies (Figure 1, Figure 2, Figure 3, Figure 4, Figure 5 and Figure 6). The angiography showed diffuse coronary artery spasm, and our interventional cardiologist did not performed a stimulation test since the procedure will be risky for the patient.
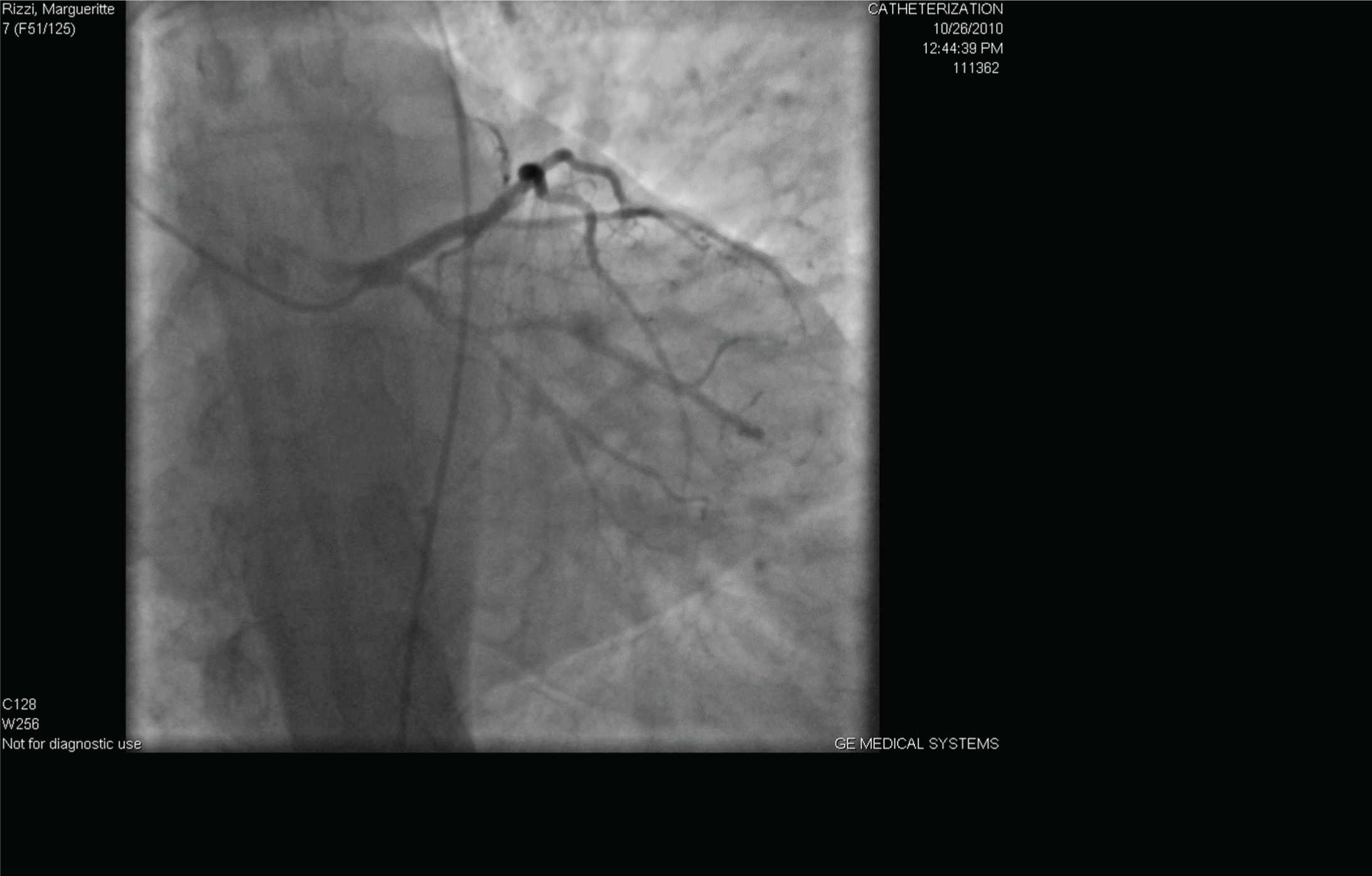
.
Figure 5: Cardiac catheterization was done and did not reveal any significant stenosis.
View Figure 5
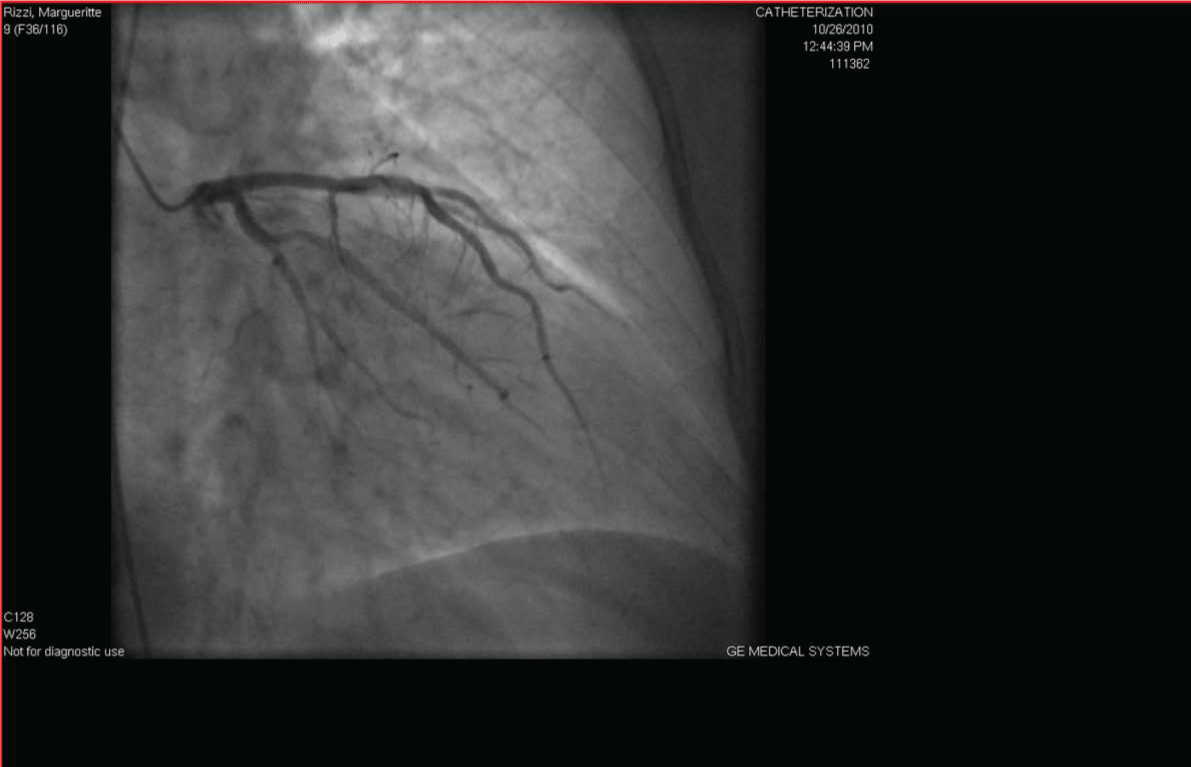
.
Figure 6: Cardiac catheterization was done and did not reveal any significant stenosis.
View Figure 6
Transthoracic echocardiography showed preserved left ventricular ejection fraction. Considered to have an episode of variant angina and an ICD was implanted in October 2010 for secondary prevention of ventricular tachyarrhythmia (Figure 7, Figure 8 and Figure 9). In front of the recurrent ventricular fibrillation, her medical treatment was optimized to include a combination of calcium channel blocker: amlodipine 10 mg once daily and diltiazem 300 mg once daily Since then (November 2010) no more ventricular arrhythmias occurred (Figure 10).
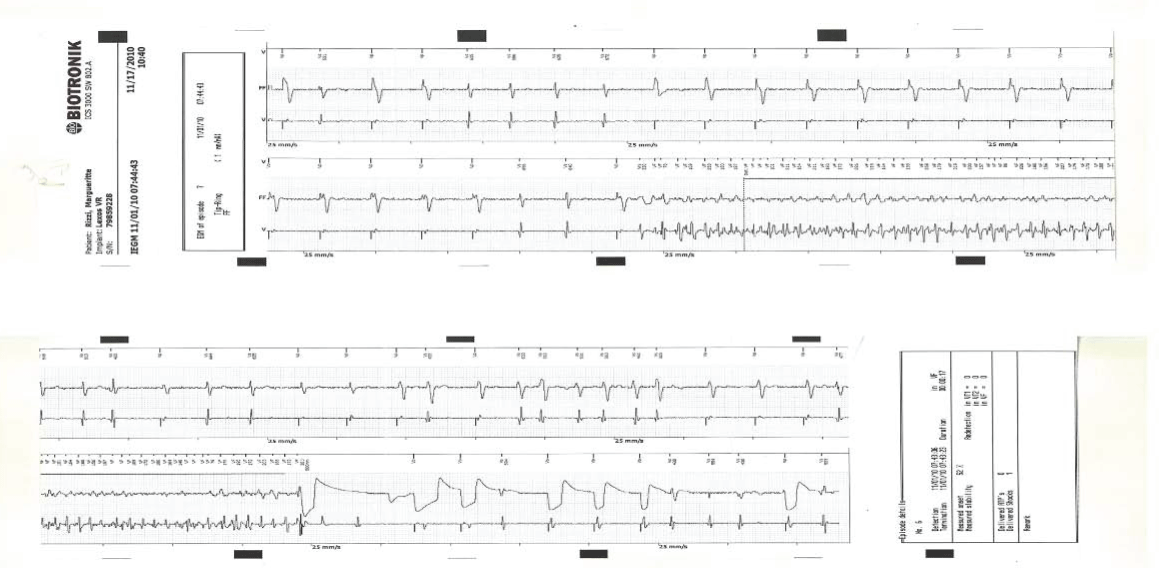
.
Figure 7: In November 2010, she experienced an episode of chest pain and presented for evaluation.
ICD records showed a recurrent ventricular fibrillation that was successfully terminated.
View Figure 7
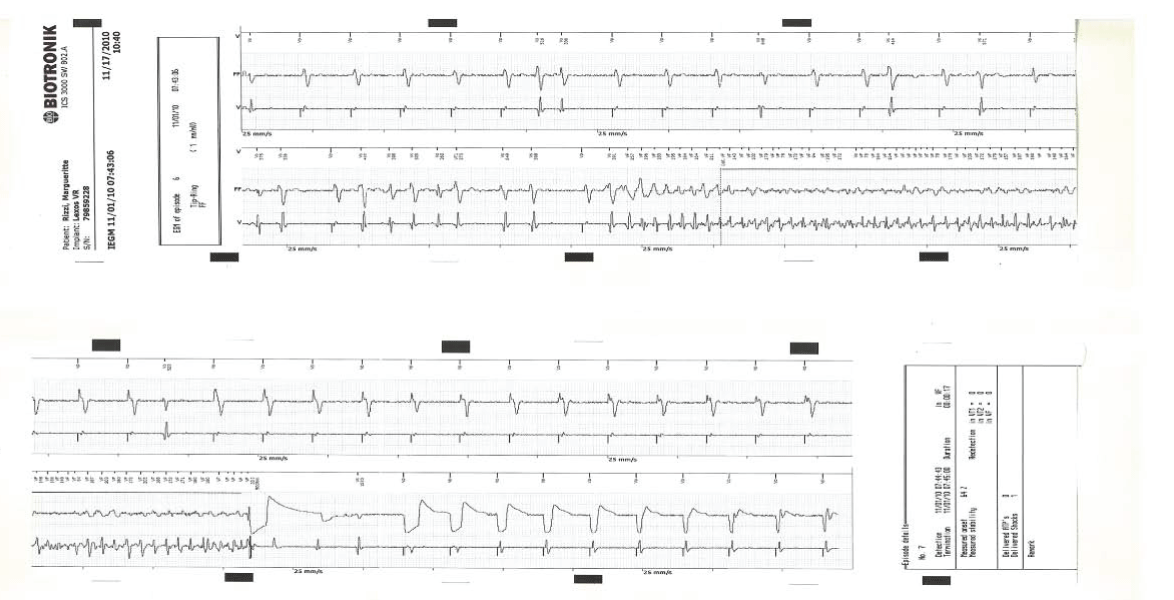
.
Figure 8: In November 2010, she experienced an episode of chest pain and presented for evaluation.
ICD records showed a recurrent ventricular fibrillation that was successfully terminated.
View Figure 8
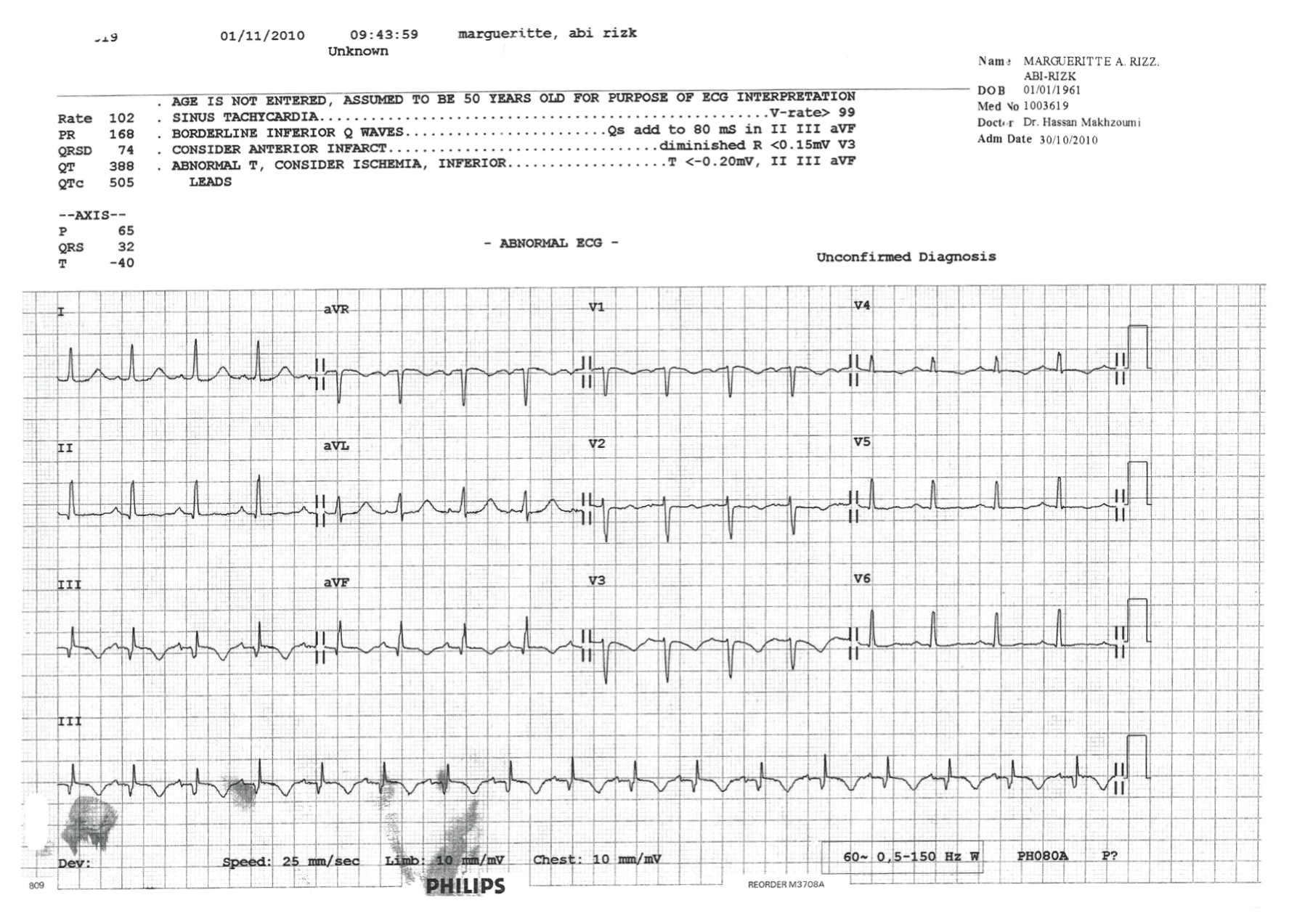
.
Figure 9: EKG at that time showed long QTc (505 ms), Q wave and T wave inversion in leads III, aVF.
View Figure 9
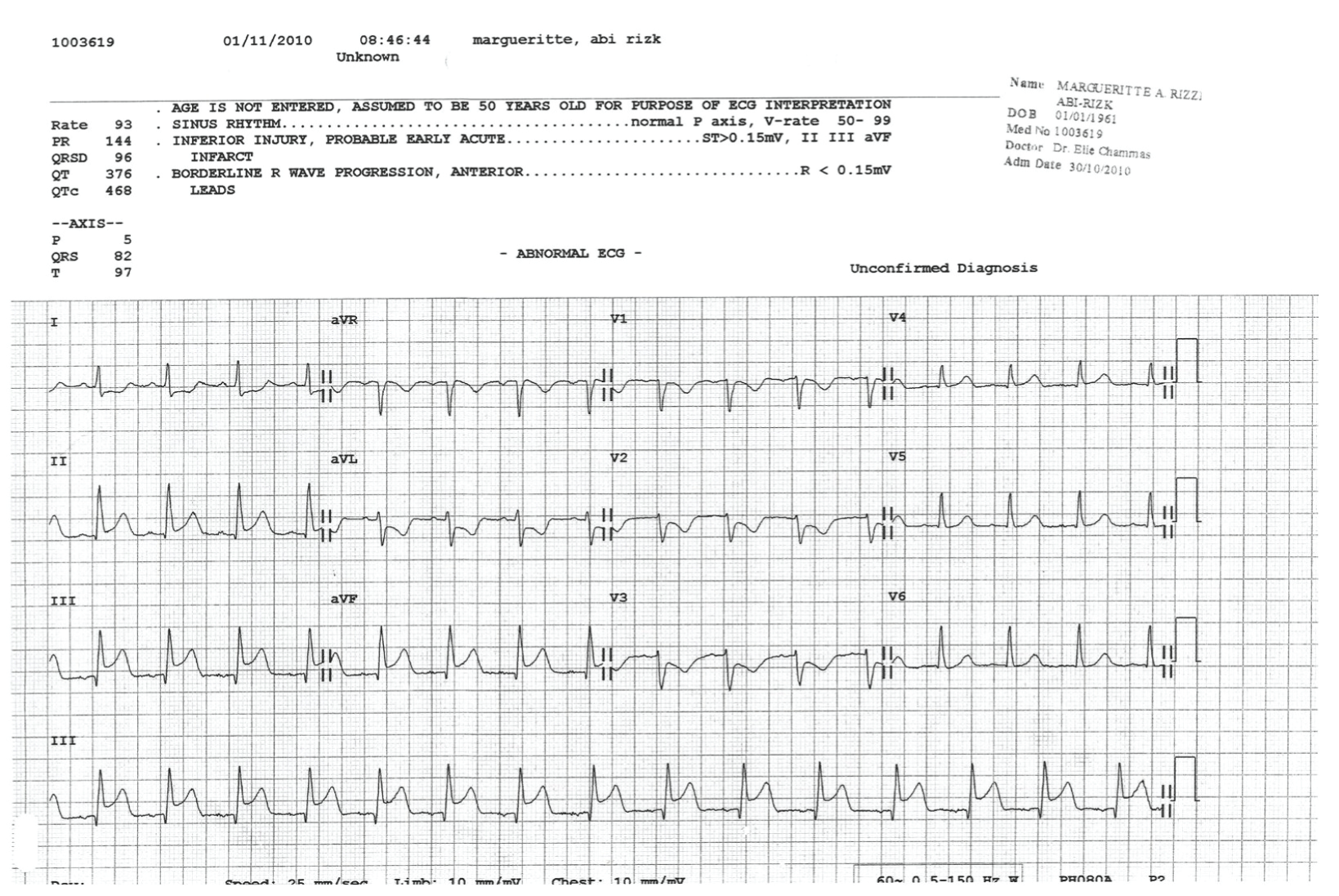
.
Figure 10: Follow-up EKG 4 years later, showed no signs of infarction (normalization of the inferior leads Q waves), with a QTc of 456 ms, and first degree AV block.
View Figure 10
Discussion
So we were in front of a case of coronary artery spasm induced long QT with ICD terminated recurrent ventricular fibrillation that resolved once a second calcium channel blocker was added to the treatment.
Coronary spasm-induced Ischemia by itself can cause ventricular fibrillation, and in all case we have to prevent and treat ischemia. It is important though to identify the mechanism of ventricular fibrillation; if it is due to QT prolongation, then special care should be taken to avoid all drugs that prolong QT and this will be of great importance.
QT prolongation may be primary or in response to myocardial ischemia. If it is due to ischemia, then the longest QT should be present in EKG recorded at time of chest pain. This was true in our patient, where the EKG of figure 2 and figure 9, recorded at time of chest pain and showing signs of ischemia, revealed the longest QT ( 498 ms and 505 ms respectively).
The prognosis of variant angina is usually excellent but eventually MI, ventricular arrhythmias and SCD may occur. Yasue et al. [7] reported an 89% to 97% overall 5-year survival rate in a 7-year follow-up in approximately 300 patients, with 3.6 % incidence of SCD and 6.5 % incidence of MI [7]. Induced ischemia may result in transient AV block or ventricular arrhythmias imposing the need for pacemaker or defibrillator respectively [4].
Sudden death and ventricular tachyarrhythmias have been well documented in patients with variant angina [8].
Previous studies demonstrated a difference between variant angina patients who die suddenly and those with uncomplicated variant angina or other sudden death patients, and found some factors leading to this difference and permitting risk-stratification of patients and thus to important therapeutic implications [9].
Miller et al. [9] and Kerin et al. [10] concluded that the degree of ischemia during attacks and therefore the degree of ST elevation was an important factor characterizing variant angina patients with serious arrhythmias and higher risk for SCD during spontaneous attacks from other variant angina patients. Other factors predicting SCD may include Severe multivessel spasm, daytime ST-segment changes, and younger age [11].
Another important factor reported in studies was the increased QTc dispersion in asymptomatic patients with variant angina reflecting a greater inhomogeneity of ventricular refractoriness, imposing a higher risk of life-threatening arrhythmias [12-14]. An increased endogenous adenosine may be the mediator of this ventricular repolarization disparity [15].
Thus, if the attacks of coronary vasospasm that provoke life threatening arrhythmias can be eliminated, sudden death should not occur, raising the importance of calcium antagonists that may resolve vasospastic episodes [16,17].
Diltiazem was associated with a decrease in angina episodes and nitroglycerin consumption, as well as reduction in ST segment deviation [18-21]. Thus, it is not surprising that diltiazem would reduce the cardiovascular event rate by reducing angina frequency as was shown by the results of Schroeder et al. [18].
Clinical guidelines do not recommend the implantation of an ICD because the variant angina induced arrhythmia are secondary to an acute ischemia that may be controlled by medical therapy [22]. This issue can be corroborated by the finding that relapses and inefficient ICD treatments was most likely related to insufficient medical treatment and extensive ischemia [23]. Observational trials of patients with coronary artery vasospasm who are receiving medical treatment with calcium antagonists report an annual cardiac arrest or sudden cardiac death risk of approximately 0.6% per year [24].
The results of Matsue et al. [6], although it has some limitations, support the use of ICD therapy in coronary artery vasospasm that survived a life threatening VT/VF.
Matthijs L. Hendriks et al. indicates that a combination of calcium blocking agents and ICD implantation isthe most appropriate option, for variant angina-induced potential lethal arrhythmias [25]. Our case that responded well to the combination of calcium channel blocker with cessation of the arrhythmia occurrence, leads us to re-evaluate the indication for ICD implantation if this dual therapy may abort the appearance of those life-threatening arrhythmias. Thus, It is necessary to carry out studies that evaluate the indication criteria for ICD as secondary prevention of potentially lethal arrhythmias due to coronary vasospasm [22].
References
-
Fukai T, Koyanagi S, Takeshita A (1993) Role of coronary vasospasm in the pathogenesis of myocardial infarction: study in patients with no significant coronary stenosis. Am Heart J 126: 1305-1311.
-
MacAlpin RN (1993) Cardiac arrest and sudden unexpected death in variant angina: complications of coronary spasm that can occur in the absence of severe organic coronary stenosis. Am Heart J 125: 1011-1017.
-
Stern S, Bayes de Luna A (2009) Coronary artery spasm: a 2009 update. Circulation 119: 2531-2534.
-
Anderson Jeffrey L, Adams Cynthia D, Antman Elliott M, Bridges Charles R, Califf Robert M, et al. (2013) "2012 ACCF/AHA focused update incorporated into the ACCF/AHA 2007 guidelines for the management of patients with unstable angina/non-ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines." Circulation 127: e663-e828.
-
Epstein AE, DiMarco JP, Ellenbogen KA, Mark Estes NA, Freedman RA, et al. (2008) ACC/AHA/HRS2008 guidelines for device-based therapy of cardiac rhythm abnormalities: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committeeto Revise the ACC/AHA/NASPE 2002 Guideline Update for Implantationof Cardiac Pacemakers and Antiarrhythmia Devices). J Am Coll Cardiol 51: e1-62.
-
Matsue Y, Suzuki M, Nishizaki M, Hojo R, Hashimoto Y, et al. (2012) Clinical implications of an implantable cardioverter-defibrillator in patients with vasospastic angina and lethal ventricular arrhythmia. J Am Coll Cardiol 60: 908-913.
-
Yasue H, Takizawa A, Nagao M, Nishida S, Horie M, et al. (1988) Long-term prognosis for patients with variant angina and influential factors. Circulation 78: 1-9.
-
Di Cori A, Gemignani C, Bini R, Zucchelli G, Caravelli P, et al. (2004) "Torsade de pointes" in a patient with variant angina." Ital heart J 5: 554-558.
-
Miller DD, Waters DD, Szlachcic J, Theroux P (1982) Clinical characteristics associated with sudden death in patients with variant angina. Circulation 66: 588-592.
-
Kerin NZ, Rubenfire M, Maini M, Wajszczuk WJ, Pamatmat A, et al. (1979) Arrhythmias in variant angina pectoris. Relationship of arrhythmias to ST-segment elevation and R-wave changes. Circulation 60: 1343-1350.
-
Togashi I, Sato T, Soejima K, Takatsuki S, Miyoshi S, et al. (2013) Sudden cardiac arrest and syncope triggered by coronary spasm. Int J Cardiol 163: 56-60.
-
Surawicz B (1996) Will QT dispersion play a role in clinical decision-making? J Cardiovasc Electrophysiol 7: 777-784.
-
Suzuki M, Nishizaki M, Arita M, Ashikaga T, Yamawake N, et al. (1998) Increased QT dispersion in patients with vasospastic angina. Circulation 98: 435-440.
-
Parchure N, Batchvarov V, Malik M, Camm AJ, Kaski JC (2001) Increased QT dispersion in patients with Prinzmetal's variant angina and cardiac arrest. Cardiovasc Res 50: 379-385.
-
Ashikaga T, Nishizaki M, Arita M, Yamawake N, Suzuki M, et al. (1999) Effect of dipyridamole on QT dispersion in vasospastic angina pectoris. Am J Cardiol 84: 807-810.
-
Kimura E, Kishida H (1981) Treatment of variant angina with drugs: asurvey of 11 cardiology institutes in Japan. Circulation 63: 844-848.
-
Waters DD, Szlachcic J, Theroux P (1981) Prognosis of variant anginapatients treated with calcium antagonist drugs. Am J Cardiol 47: 463.
-
Schroeder JS, Lamb IH, Bristow MR, Ginsburg R, Hung J, et al. (1983) Prevention of cardiovascular events in variant angina by long-term diltiazem therapy. J Am Coll Cardiol 1: 1507-1511.
-
Rosenthal SJ, Ginsburg R, Lamb IH, Baim DS, Schroeder JS (1980) Efficacy of diltiazem for control of symptoms of coronary arterial spasm. Am J Cardiol 46: 1027-1032.
-
Pepine CJ, Feldman RL, Whittle J, Curry RC, Conti CR (1981) Effect of diltiazem in patients with variant angina: a randomized double-blind trial. Am Heart J 101: 719-725.
-
Johnson SM, Mauritson DR, Willerson JT, Hillis LD (1981) A controlled trial of verapamil for Prinzmetal's variant angina. N Engl J Med 304: 862-866.
-
Guzzo-Merello G, Romero-Tejero C, Garcia-Cosio F, Martinez-Elbal L (2009) Indication for defibrillator implantation in a patient with Prinzmetal's angina and syncopes. Rev Esp Cardiol 62: 820-821.
-
Letsas KP, Filippatos GS, Efremidis M, Sideris A, KardarasF (2007) Secondary prevention of sudden cardiac death in coronaryartery spasm: Is implantable cardioverter defibrillator alwaysefficient? Int J Cardiol 117: 141-143.
-
Aoki M, Koyanagi S, Sakai K, Irie T, Takeshita A, et al. (1990) Exercise-induced silent myocardial ischemia in patients with vasospastic angina. Am Heart J 119: 551-556.
-
Hendriks ML, Allaart CP, Bronzwaer JG, Res JJ, de Cock CC (2008) Recurrent ventricular fibrillation caused by coronary artery spasm leading to implantable cardioverter defibrillator implantation. Europace 10: 1456-1457.