Clinical Medical
Reviews and Case Reports
Rx for Disaster: When Medication Non-adherence becomes an Emergency
Lindsay S. Leech1*, Nicole G. Tasker2 and Julie L. Welch3
1Indiana University School of Medicine, IN, USA
2Emergency Medicine Residency R1, Department of Emergency Medicine, University of Tennessee Chattanooga College of Medicine, TN, USA
3Department of Emergency Medicine, Indiana University School of Medicine, IN, USA
*Corresponding author: Lindsay S. Leech, Indiana University School of Medicine, 7475 Quincy Ct, Indianapolis, IN 46254, USA, Tel: 765-376-0900, E-mail: lleech@iupui.edu
Clin Med Rev Case Rep, CMRCR-3-100, (Volume 3, Issue 4), Case Report; ISSN: 2378-3656
Received: March 07, 2016 | Accepted: April 11, 2016 | Published: April 13, 2016
Citation: Leech LS, Tasker NG, Welch JL (2016) Rx for Disaster: When Medication Nonadherence becomes an Emergency. Clin Med Rev Case Rep 3:100. 10.23937/2378-3656/1410100
Copyright: © 2016 Leech LS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
This case report describes a 35-year-old woman who presented to the Emergency Department (ED) after a seizure. Her evaluation revealed a rare cause of her seizures, confounded by medication non-adherence. She was emergently treated and admitted for further management. With standard patient education, social services, and outpatient follow-up, she did well for three years, however had two subsequent admissions for recurrent seizures from non-adherence. This case demonstrates a rare but treated cause of seizures and the unfortunate scenario of medical non-adherence. It explores possible interventions to facilitate healthcare providers' ability to improve patient adherence.
Keywords
Hypocalcemia, Seizures, Hypoparathyroidism, Medication non-adherence, Motivational interviewing, Mobile intervention
Introduction
Emergency medicine physicians are often faced with the undifferentiated seizure patient and must rapidly stabilize the patient, while identifying and treating the underlying cause. We present the case of a patient with hypoparathyroidism who presented to the emergency department with hypocalcemic seizures confounded by medication non-adherence. With standard patient education, social services, and outpatient follow-up, she did well for three years, however had two subsequent admissions for recurrent seizures from non-adherence. This case highlights the difficulty providers often face in both communicating the importance of and ensuring outpatient medical adherence. We discuss implications and explore potential intervention strategies to facilitate healthcare providers' ability to improve patient adherence.
Case Report
A 34-year-old female presented to the Emergency Department (ED) after having a witnessed tonic-clonic seizure while sitting on her sister's porch that lasting less a few minutes. She lost control of her bladder. She had a mild headache after the seizure. She recalled several weeks of muscle fatigue, mouth and hand twitching, and perioral tingling. She denied trauma, fever, neck pain, or prior seizure disorder. Review of systems was otherwise negative. She was postictal initially with no medical records in our system, thus her past medical history was obtained by contacting her sister and her primary care physician in a town 3 hours away. This revealed a history of hypoparathyroidism since age 19 with secondary hypocalcemia, cerebral calcifications, and kidney stones. No history of neck surgery or radiation. No allergies. She was prescribed the following medications: Citracal calcium with vitamin D 630 mg/500 IU, 2 tablets BID; calcitriol 0.5 mcg BID; and magnesium oxide 400 mg BID. The patient admitted that she was not taking her medications as directed and was "stretching" them out, because she was running low. She recently lost her job and moved here to live with family last month. She was waiting on her Medicaid (public insurance) to be switched to a new physician in town. She denied using tobacco, alcohol, or illicit drugs. Her family history was significant for diabetes. On physical examination her vital signs were stable with a heart rate of 73 beat per minute, blood pressure of 111/54, respiratory rate 19, temperature of 36.8 C, and room air saturation of 96%. She was awake, alert, and oriented to person, place, and date. The only significant findings on her examination were diminished deep tendon reflexes in all four extremities, positive Chvostek's and Trousseau's signs, and mild exophthalmos. The remainder was benign.
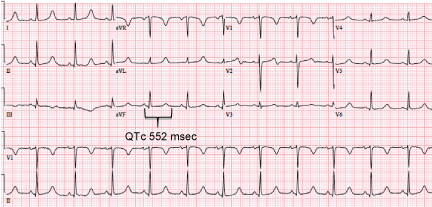
Emergency department evaluation revealed an EKG with normal sinus rhythm with a prolonged QTc of 552 msec (Image 1). Laboratory evaluation (Table 1) revealed a normal complete blood count (CBC), a basic metabolic panel (BMP) with hypokalemia 3.0 mmol/L (3.5-5.5 mmol/L), hypocalcemia 4.3 mg/dL (8.5-10.5 mg/dL), and hypomagnesemia 1.3 mg/dL (1.6-2.9 mg/d). Urinalysis was positive for nitrites, leukocyte esterase, and hemoglobin. A Head CT scan demonstrated extensive basal ganglia calcifications, consistent with hypoparathyroidism and stable from an outside comparison.
Emergent treatment was initiated in the emergency department for her severe hypocalcemia with associated seizure and EKG abnormalities. She was given calcium gluconate 10 ml IVPB over 15 minutes. Additional electrolytes were replaced and antibiotics initiated for her urinary tract infection (UTI).
![]()
Table 1: Significant Laboratory Rest Results.
View Table 1
She was admitted to the hospital for further evaluation and management of her severe hypocalcemia, medication non-adherence, electrolyte imbalance, and UTI. Endocrinology was consulted and concluded that primary hypoparathyroidism was the cause of her hypocalcemia. While closely monitoring her electrolytes, she was transitioned to oral calcitriol, calcium carbonate, and magnesium oxide. The patient's hospital stay remained uncomplicated and she was counseled daily on her progress by her healthcare providers.
At the time of discharge from the hospital, she received face-to-face instructions from her physician and primary nurse on her diagnoses, medications, and outpatient follow-up recommendations. She was given prescriptions for calcium carbonate 1500 mg orally TID, calcitriol 0.5 mcg orally BID, and magnesium oxide 400 mg orally BID. She was instructed that she could substitute the calcium carbonate for TUMS antacid tablets (each 500 mg) if this as a more affordable option. The discharge nurse called her prescriptions into a local pharmacy and verified the next day that the patient day picked up the prescriptions. Social services assisted with reassigning a primary care physician to the local area through Medicaid (public insurance) and setting up an outpatient appointment in one week with the Endocrinologist. Although the patient failed to show up for her Endocrinology appointment, she did well for nearly three years, however was re-admitted on two subsequent ED visits for severe hypocalcemic seizures due to medication non-adherence.
Discussion
This case highlights the importance of patient adherence to medical therapy in a chronic disease state when the risk of non-adherence leads to potentially life threatening consequences. We will discuss the pathophysiology and management of severe hypocalcemia, outline factors that influence patient non-adherence with standard educational strategies to reduce non-adherence, and explore innovative interventions that healthcare providers might employ to improve sustained medical adherence.
Severe hypocalcemia
Severe hypocalcemia is a life threatening condition, defined as an ionized calcium level < 1.1 mmol/L. If left untreated, severe hypocalcemia may lead to tetany, muscle spasms, altered mental status, seizures, prolonged QT interval on EKG, bradycardia, ventricular arrhythmias, and/or cardiac collapse [1]. Tetany results from a direct increase in peripheral muscular excitability and may lead to peri-oral and acral paresthesias, stiffness, myalgia, muscle spasms/cramps, diaphoresis, bronchospasm, and biliary colic [2,3]. The classic physical findings are Trousseau's sign, the induction of carpopedal spasm by inflation of a blood pressure cuff above systolic blood pressure for three minutes, and Chvostek's sign, contraction of the ipsilateral facial muscles when tapping the facial nerve anterior to the ear [4]. Hypocalcemia can also lead to seizures of all types, of which both spikes and bursts of high-voltage paroxysmal slow waves characterize the EEG [2,5]. From a cardiovascular perspective, hypocalcemia characteristically causes QT prolongation (Image 1) by prolonging phase two of the action potential [6,7]. This prolongation is associated with early after repolarizations and may lead to dysrhythmias such as torsades de pointes [6,7].
As the physiologic consequences of severe hypocalcemia are life threatening, it is important to rapidly recognize and treat the condition and then work to discern the underlying etiology in order to prevent future episodes [8,9]. Treatment of severe, symptomatic hypocalcemia, as well as asymptomatic patients with a serum calcium of < 1.9 mmol/L, is 1-2 g of IV calcium gluconate in 50 mL of 5% dextrose over 10-20 minutes followed by a slow infusion of either 10% calcium gluconate or 10% calcium chloride at 50 mL/hour until the patient can tolerate an effective oral regimen of calcium and vitamin D.
In this case, the underlying cause of the hypocalcemia was hypoparathyroidism complicated by non-adherence to medical therapy. In healthy patients parathyroid hormone (PTH) plays a major role in calcium homeostasis by increasing extracellular calcium concentrations. However, as in this case, a mutation in the calcium sensing receptors sends an erroneous signal to suppress PTH secretion leading to hypocalcemia [10].
While the emergent management of severe hypocalcemia involves inpatient intravenous replacement with calcium, the outpatient management of hypocalcemia is rather simple requiring at minimum twice a day oral calcium carbonate replacement. Calcium carbonate is a common mineral supplement that does not require a prescription and is sold at any pharmacy, health food store, or supermarket. In fact, it is found in the common antacid TUMS, which can be substituted to reduce patient cost.
Significance of non-adherence
This case represents the unfortunate scenario of a medical emergency due to medication non-adherence. Non-adherence is associated with not only increased morbidity and mortality but also higher health care costs in the United States [11-15]. The total annual cost of non-adherence is estimated at $1 billion, and, furthermore, one-third to two-thirds of all medication related hospitalizations are believed to be the result of medication non-adherence [13]. Contributing to this is the 12-22% of patients discharged from emergency departments that do not fill their prescriptions and the 40% who do not take their prescriptions as directed. Emergency departments are often the safety net of medical care for socioeconomically disadvantaged patients who often face challenges in obtaining or affording medication despite the desire to adhere [11].
Non-adherence is a multifactorial problem that can be contributed to a variety of factors such as psychological state, comorbidity, education, attitude, medication side effects, social support, socioeconomics, complex dosing, resources, and forgetfulness [11-14,16]. In our case, several of these factors potentially played a role the patient's non-adherence. Specific examples include the following: loss of a job; lack of financial resources to afford medications and healthcare; necessity to move to a new town for housing; distance to primary care physician; reliance on public insurance to re-assign a new primary care physician; lack of understanding that her medications were readily available without a prescription. It is not apparent why the patient failed to follow up with her Endocrinology appointment, and records do not indicate if they attempted to make contact with the patient.
Strategies to reduce & sustain adherence
As in this case, when non-adherence is recognized as a confounding factor, patient education strategies are employed in an attempt to improve medication adherence; however, it remains an ongoing challenge. In our case, there were several strategies used the improve adherence during her admission (i.e., daily patient updates and social services consult) and at the time of discharge (i.e., verbal and written discharge instructions, telephoning prescriptions to the pharmacy, ensuring patient pick up at pharmacy, and offering less expensive medication alternatives). These yielded relative success for three years, however non-adherence was not sustained past that time.
The literature demonstrates that traditional written and verbal discharge instructions are alone often not totally effective in combating non-adherence. Studies show that patients receiving information pamphlets and counseling prior to discharge regarding their specific medications have no significant improvement in adherence [11,13]. Factors contributing to this might include literacy and language barriers, lack of comprehension and retention of information, internal/external stressors inherent to the hospital environment [17].
In an attempt to further enhance patient adherence for a sustained impact, additional patient education strategies are being used. Cognitive-behavioral therapy or motivational interviewing offers promising improvement in patient adherence [13,18-20]. In cognitive-behavioral therapy patients are helped to recognize the link between medication adherence, symptom reduction, and personal health [13,20]. Motivational interviewing, initially developed as a technique for addressing addictions, is patient-centered and revolves around understanding what triggers change and resolving ambivalence towards medication adherence. It prompts the patient to discuss the pros and cons of complying or not complying with their medication regimen [13,19]. The ultimate goal of this technique is for the patient to discover an intrinsic, autonomous motivation to change and to develop a plan to instrument that change [19].
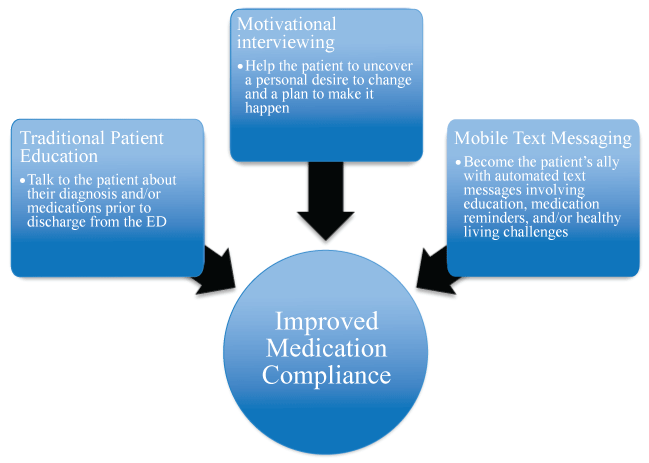
Another strategy to improve adherence is the use of mobile health interventions such as daily text messages after patient discharge. Evidence indicates that implementing mobile health interventions could prove beneficial in the management of chronic disease and medication adherence. An estimated 83% of adults living in the United States operate a mobile phone and three-fourths of these individuals use text messaging; thus implementing a large mobile health program is both feasible and cost-friendly [15,21]. These succinct messages can include education, medication reminders, or healthy living challenges addressing the patient's specific disease as well as his/her overall wellbeing [21]. Technology is advanced to a point that tailoring these messages to a specific time of day, content, and language is relatively uncomplicated making such a program simple for both the provider and the patient [16,21]. One study found that after six months of a trial TExT-MED program for diabetes patients there was a statistically significant improvement in medication adherence, a 16.1% reduction in visits to the emergency department, and 100% of patients recommended the program [21]. A recent met-analysis of 16 randomized controlled trials to assess the effect of mobile text messaging on medication adherence found that text messaging increases the odds of medication adherence in chronic disease from 50% to 67.8% [22]. Not only do these messages provide education and serve as daily reminders, but they provide frequency of interaction and personal touch which have shown to enhance patient confidence in reaching a goal [21,23]. Ultimately, a combination of these techniques-traditional education, motivational interviewing, and/or mobile interventions-could offer a symbiotic effect on patient adherence (Figure 1).
Conclusion
This case highlights the impact of non-adherence to medical therapy (i.e., oral calcium replacement) in a chronic disease state (i.e., hypocalcemia) leading to potentially life threatening consequences. Hypocalcemia secondary to hypoparathyroidism is a physiologically complex condition with severe complications when left untreated, including seizures and cardiac arrhythmia. Prompt recognition and treatment of severe hypocalcemia is imperative in the acute setting. Once stabilized, the provider and patient can work together to address the factors influencing non-adherence and establish an ongoing management plan. Unfortunately, traditional patient education strategies do not always lead to sustained compliance. Future research is needed to examine the role of incorporating additional interventions, such as motivational interviewing and/or mobile text messaging, into patient education and measuring the sustained impact on clinical outcomes and patient adherence.
References
-
https://www.arupconsult.com/content/hypocalcemia
-
Macefield G, Burke D (1991) Paraesthesiae and Tetany Induced by Voluntary Hyperventilation: Increased Excitability of Human Cutaneous and Motor Axons. Brain 114: 527-540.
-
Tohme JF, Bilezikian JP (1993) Hypocalcemic emergencies. Endocrinol Metab Clin North Am 22: 363-375.
-
Cooper MS, Gittoes NJ (2008) Diagnosis and management of hypocalcaemia. BMJ 336: 1298-1302.
-
Swash M, Rowan AJ (1972) Electroencephalographic criteria of hypocalcemia and hypercalcemia. Arch Neurol 26: 218-228.
-
Benoit S, Mendelsohn A, Nourjah P, Staffa JA, Graham DJ (2005) Risk factors for prolonged QTc among US adults: Third National Health and Nutrition Examination Survey. Eur J Cardiovasc Prev Rehabil 12: 363.
-
Meyer T, Ruppert V, Karatolios K, Maisch B (2007) Hereditary long QT syndrome due to autoimmune hypoparathyroidism in autoimmune polyendocrinopathy-candidiasis-ectodermal dystrophy syndrome. J Electrocardiol 40: 504-509.
-
Skugor M (2009) Hypocalcemia. Cleveland Clinic Medical Publications: Disease Management Project.
-
Wysolmerski JJ, Insogna KL (2007) The Parathyroid Glands, Hypercalcemia, and Hypocalcemia Goldman: Cecil Medicine 23.
-
Copstead L, Banasik J (2010) Pathophysiology. Saunders/Elsevier, St. Louis, MO.
-
McCarthy ML, Ding R, Roderer NK, Steinwachs DM, Ortmann MJ, et al. (2013) Does providing prescription information or services improve medication adherence among patients discharged from the emergency department? A randomized controlled trial. Ann Emerg Med 62: 212-223.
-
Suffoletto B, Yealy DM (2013) The trouble with medication adherence after emergency care. Ann Emerg Med 62: 235-236.
-
Julius RJ, Novitsky MA Jr, Dubin WR (2009) Medication adherence: a review of the literature and implications for clinical practice. J Psychiatr Pract 15: 34-44.
-
Hohl CM, Abu-Laban RB, Brubacher JR, Zed PJ, Sobolev B, et al. (2009) Adherence to emergency department discharge prescriptions. CJEM 11: 131-138.
-
Suffoletto B, Calabria J, Ross A, Callaway C, Yealy DM (2012) A Mobile Phone Text Message Program to Measure Oral Antibiotic Use and Provide Feedback on Adherence to Patients Discharged From the Emergency Department. Academic Emergency Medicine 19: 949-958.
-
Vervloet M, Linn AJ, van Weert JCM, de Bakker DH, Bouvy ML, et al. (2012) The effectiveness of interventions using electronic reminders to improve adherence to chronic medication: a systematic review of the literature. J Am Med Inform Assoc 19: 696-704.
-
Wei HG, Camargo CA Jr (2000) Patient education in the emergency department. Acad Emerg Med 7: 710-717.
-
de Lusignan S, Chan T, Tejerina Arreal MC, Parry G, Dent-Brown K, et al. (2013) Referral for psychological therapy of people with long term conditions improves adherence to antidepressants and reduces emergency department attendance: Controlled before and after study. Behaviour Research and Therapy 51: 377-385.
-
Butterworth SW (2008) Influencing patient adherence to treatment guidelines. J Manag Care Pharm 14: 21-24.
-
Weiden P (2011) The Adherence Interview: Better Information, Better Alliance. Psychiatry Annals 41: 279-285.
-
Arora S, Peters AL, Burner E, Lam CN, Menchine M (2013) Trial to Examine Text Message–Based mHealth in Emergency Department Patients With Diabetes (TExT-MED): A Randomized Controlled Trial. Ann Emerg Med 63: 745-754.
-
Thakkar J, Kurup R, Laba TL, Santo K, Thiagalingam A, et al. (2016) Mobile Telephone Text Messaging for Medication Adherence in Chronic Disease: A Meta-analysis. JAMA Intern Med 176: 340-349.
-
de Jongh T, Gurol-Urganci I, Vodopivec-Jamsek V, Car J, Atun R (2012) Mobile phone messaging for facilitating self-management of long-term illnesses. Cochrane Database Syst Rev 12: CD007459.