Clinical Medical
Reviews and Case Reports
Socket Reconstruction after Firework Explosion Injury
Reili Rebane, Mari Tamsalu and Artur Klett*
East Tallinn Central Hospital Eye Clinic, Tallinn, Estonia
*Corresponding author: Artur Klett, East Tallinn Central Hospital Eye Clinic, Tallinn, Estonia, Tel: +372-6207130, E-mail: Artur.Klett@itk.ee
Clin Med Rev Case Rep, CMRCR-3-095, (Volume 3, Issue 3), Case Report; ISSN: 2378-3656
Received: February 10, 2016 | Accepted: March 11, 2016 | Published: March 14, 2016
Citation: Rebane R, Tamsalu M, Klett A (2016) Socket Reconstruction after Firework Explosion Injury. Clin Med Rev Case Rep 3:095. 10.23937/2378-3656/1410095
Copyright: © 2016 Rebane R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
We report a challenging case of orbital socket reconstruction. A 49- year-old man presented two weeks after fireworks exploded in his face. He had multiple orbital bone fractures on the right and the globe was enucleated because of severe damage. No primary orbital implant was used due to infection risk. One month after the trauma he suffered from infection of the conjunctival sac and periorbital skin despite initial intravenous and oral antibiotics. Because of inability to wear a cover shell eye prosthesis the socket reconstruction was started ten months after trauma. First a free fat graft was inserted to restore volume. The second operation was a bone graft, to elevate the orbital contents. Thirdly a canthoplasty was done. Then dermis-fat graft insertion was needed for further volume augmentation. Orbital reconstruction after firework injury is often a long process and numerous interventions are required to achieve a good cosmetic result.
Keywords
Orbital trauma, Firework injury, Socket reconstruction, Dermis-fat graft, Bone graft, Canthoplasty
Introduction
The use of fireworks to celebrate New Year's Eve is a worldwide tradition. Unfortunately this is an accident-prone environment that can lead to severe injuries. According to a systematic review by Wisse et al., 2010, victims of firework trauma are 77% male and often innocent bystanders (47%). Most of the trauma is usually mild and temporary. Penetrating eye trauma, globe contusions and burns accounted for 18.2%, with a 3.9% enucleation rate [1]. Post-enucleation socket reconstruction after severe firework trauma is challenging due to numerous long term complications of the anophthalmic socket, including generalized volume deficiency, lower eyelid laxity with poor prosthesis support, orbital implant migration if used, upper eyelid ptosis, chronic conjunctivitis and mucoid discharge [2]. A successfully rehabilitated anophthalmic socket must hold and support a prosthetic device that mimics the contralateral globe; the main goal is symmetry [3]. Usually multiple surgeries to attain the best end-result are required.
Case Report
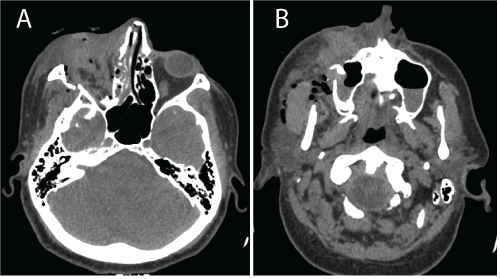
A 49- year-old man celebrated New Year's Eve. Shortly after midnight, one pyrotechnic device malfunctioned and he leaned over it. At that moment the device exploded and launched directly to the right side of his face. The patient suffered from a severe head trauma, lost consciousness, and an ambulance was called immediately. He was admitted to the neurosurgery department. A CT scan showed brain contusion and a small subarachnoid haemorrhage in the right frontal lobe. He also had right-sided multiple facial bone fractures and irregular shaped right globe (Figure 1 (A & B)). The craniofacial surgeons decided that no operation for reconstruction is needed.
.
Figure 1 (A & B): Head CT scan one hour after trauma shows multiple right sided fractures of orbita, zygomatic arch, nasal bone, maxillary sinus and ethmoidal cells, oedema of soft tissues and air in the orbit. Blood is present in both maxillary sinuses. Ocular contents are indiscernible on the right.
View Figure 1
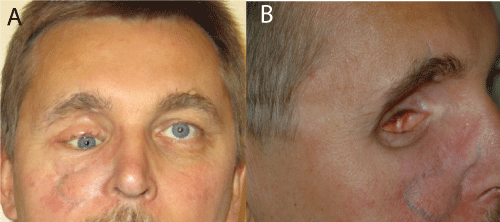
An ophthalmologist was consulted, who confirmed that there were no ocular contents in place, no hope for globe preservation and high infection risk. The left eye was normal. Six hours after the clinical workup the ophthalmologist enucleated the right globe in general anesthesia without primary implant. The patient was discharged one week later, after recovering from brain contusion. Two weeks after the trauma he had translucent yellowish fluid excretion from the socket, cerebrospinal fluid leakage was suspected, but not confirmed by neurologists. The patient had a second setback one month after the trauma when despite of initial intravenous antibiotics at the hospital, followed by an oral course, new infection caused further volume loss in the orbit. The secondary infection was treated with a week course of intravenous antibiotics, no surgical revision was needed. Five months after trauma the patient could not be properly fitted with a cover shell prosthesis due to severe volume loss (Figure 2 (A & B)). He needed complex reconstructions to substitute the volume and shape the orbit. These were not started until ten months after the trauma.
.
Figure 2 (A & B): Patient 5 months after the trauma with severe enophthalmos, hypotropia and scarred fornices on the right.
View Figure 2
The choice was to use available and autologous materials. All options and possible complications where discussed with the patient.
First a free fat graft (FFG) was inserted. The autograft was derived from the patient's left lower abdomen, above the pubic hairline. The aim was to have fast volume augmentation with a relatively simple operation in local anesthesia before targeting hypotropia.
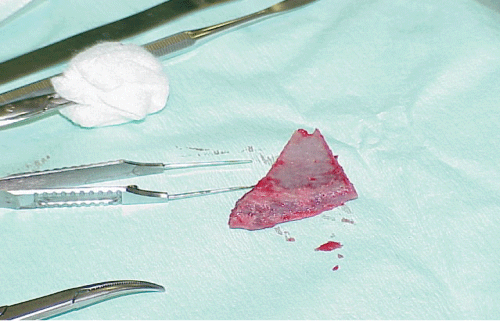
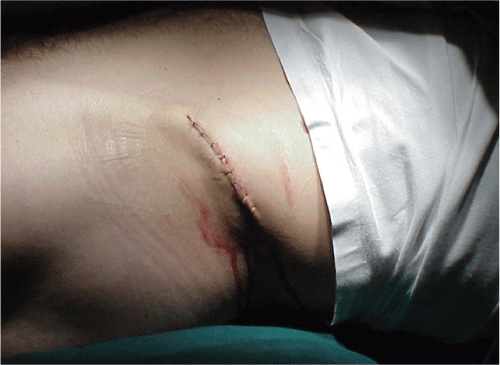
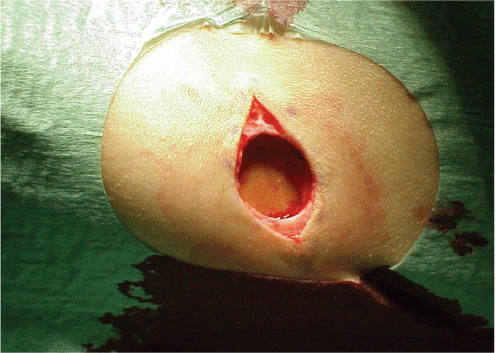
Five months after starting reconstruction a bone graft from his left pelvic bone - anterior superior iliac spine - was taken (Figure 3 and Figure 4). The graft was put on the orbital floor and fixated with 5-0 Vicryl. A good elevation of the orbital contents was achieved (Figure 5). Medial and lateral canthoplasty and temporal lower lid ligament fixation to periosteum was performed ten months after starting reconstruction. Another seven months later, lateral lower lid ligament was refixated to periosteum. Apparent volume deficit on the upper eyelid was substituted with dermis-fat graft (DFG) from the patient`s left lower abdomen (Figure 6). There was no need to restore the conjunctiva with dermis.
To date, four years after the trauma, despite numerous efforts to replace the volume, the patient still needs volume augmentation. He can wear a prosthesis, but possibilities for further reconstruction are being investigated (Figure 7).
.
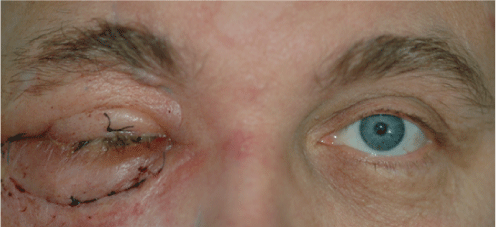
Figure 5: Patient following bone graft insertion to the right. Tarsorrhaphy is done.
View Figure 5
.
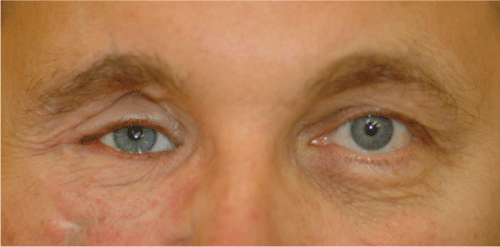
Figure 7: Patient four years after the trauma with deep right sulcus and enophthalmos. Further reconstruction to restore volume is needed.
View Figure 7
Discussion
Enucleation and evisceration introduce anophthalmic socket syndrome, which consists of enophthalmos due to orbital tissue shrinkage, deep superior sulcus, and shallow fornix and affects the cosmetic acceptance and also the opportunity to wear prosthesis [4].
Although cosmetically the best result is usually achieved if an orbital implant is inserted at the time of the enucleation, there may be occasions e.g. in a very sick patient or high infection risk after trauma, when the quickest and simplest complete excision of the eye is indicated. These are also the reasons why in this case no primary implant was used [2].
FFG and DFG are a good treatment option for anophthalmic socket reconstruction and an alternative to the widely used alloplastic orbital implants. DFG can be used as a primary implant or as a secondary implant for the correction of a contracted socket or a post enucleation socket syndrome [5]. For patients whose eyeballs were removed, local pedicled flaps, vascular fascial flaps, skin grafts, and cartilage grafts can also be used for orbital volume augmentation [2]. Smith et al., 1983 have proposed that the advantage of the DFG lies in its ability to replace the orbital volume, while, at the same time, maintaining the fornix and conjunctiva [6]. Autogenous deepithelialized skin with subcutaneous fat is implanted into the socket and dermis is sutured to the periosteum [2]. DFG survives the best, with little loss of volume, when grafts are placed within Tenon's capsule immediately following the removal of the globe and when the rectus muscles (and anterior ciliary arteries) are anastomosed to the dermal edge of the graft [3]. One of the main disadvantages of DFG is a graft reabsorption rate of 15% to 70% [7,8]. Most complications occur in patients with severely traumatized sockets, who have undergone extensive ocular surgery earlier, or who have a systemic disease contributing to defective wound healing [9]. In this situation DFG insertion gave a very good result in increasing volume without anastomoses, while having a lower reabsorption rate than a FFG and filling more space. We accounted the reabsorption rate of the DFG to be around 30 %, the size of the graft was measured accordingly.
In this case due to lower orbital wall fractures the orbital contents were hypotropic and needed to be lifted. In this situation synthetic materials like porous polyethylene, and polydioxanone could have also been used [10]. We decided to use autogenous pelvic bone to minimize synthetic material related complications like rejection and extrusion. Bone grafts have regained the favour of many craniofacial surgeons in orbital floor reconstructions due to their biocompatibility [11]. With a secondary surgical site there is a higher risk of infection and scarring, but a big advantage in this case was that the size and shape of the available graft could be measured according to needs.
One of the main anatomic deformities of anophthalmic socket is marked laxity and elongation of the lateral canthal tendon. The tarsal strip procedure is ideal for correcting or improving these deformities simultaneously with one simple procedure [12]. In this case medial and lateral canthoplasty was done and during that procedure temporal lower lid ligament was fixated to periosteum. The patient again needed a refixation of the temporal ligament seven months after the first procedure, because the first operation did not give a sufficient result. The main issue of this was that the patient had a right lateral orbital wall fracture with displacement, which was decided not to be corrected by craniofacial surgeons. So to achieve any symmetry was challenging.
In conclusion, we have reported our experience in using autogenous transplants in a post-traumatic anophthalmic socket reconstruction. Nowadays the use of synthetic materials is usually a standard treatment, but the use of autogenous materials should also be considered in selected cases. Unfortunately, the ideal material and the perfect sequence of operations for socket reconstruction still remain elusive.
This case illustrates that firework trauma can cause severe ocular injuries and the therapy to achieve a symmetric result is usually long-term. Restrictive firework legislation use [1] and repetitive education of the public is necessary to minimize the occurrence of similar accidents in the future.
Financial Disclosure
Nothing to declare.
References
-
Wisse RP, Bijlsma WR, Stilma JS (2010) Ocular firework trauma: a systematic review on incidence, severity, outcome and prevention. Br J Ophthalmol 94: 1586-1591.
-
Collin JRO (2006) A Manual of Systematic Eyelid Surgery. (3rd edn), Butterworth-Heinemann Elsevier, Philadelphia, Pennsylvania.
-
Bosniak SL (1987) Reconstruction of the anophthalmic socket: state of the art. Adv Ophthalmic Plast Reconstr Surg 7: 313-348.
-
Babar TF, Hussain M, Zaman M (2009) Clinico-pathologic study of 70 enucleations. J Pak Med Assoc 59: 612-614.
-
Hintschich CR, Beyer-Machule CK (1996) [Dermal fat transplant as autologous orbital implant]. Klin Monbl Augenheilkd 208: 135-141.
-
Smith B, Bosniak S, Nesi F, Lisman R (1983) Dermis-fat orbital implantation: 118 cases. Ophthalmic Surg 14: 941-943.
-
Guberina C, Hornblass A, Meltzer MA, Soarez V, Smith B (1983) Autogenous dermis-fat orbital implantation. Arch Ophthalmol 101: 1586-1590.
-
Conley JJ, Clairmont AA (1978) Dermal-fat-fascia grafts. Otolaryngology 86: ORL-641-9.
-
Shore JW, McCord CD Jr, Bergin DJ, Dittmar SJ, Maiorca JP, Burks WR, et al. (1985) Management of complications following dermis-fat grafting for anophthalmic socket reconstruction. Ophthalmology 92: 1342-1350.
-
Avashia YJ, Sastry A, Fan KL, Mir HS, Thaller SR (2012) Materials used for reconstruction after orbital floor fracture. J Craniofac Surg 23: 1991-1997.
-
Mok D, Lessard L, Cordoba C, Harris PG, Nikolis A (2004) A review of materials currently used in orbital floor reconstruction. Can J Plast Surg 12: 134-140.
-
Anderson RL (1981) Tarsal strip procedure for correction of eyelid laxity and canthal malposition in the anophthalmic socket. Ophthalmology 88: 895-903.