Trauma Cases and Reviews
Kirschner Wire Migration from Proximal Humerus into the Lung: Brief Report
Guy Aristide Bang1*, Albert Nana Muluem1, Blondel Nana Oumarou1, Marie Ange Ngo Yamben2 and Daniel Hany Eone3
1Surgery Unit, National Social Insurance Fund Health Center of Yaoundé, Cameroon
2Orthopedic Unit, Yaoundé University Teaching Hospital, Cameroon
3Orthopedic Unit, Central Hospital of Yaoundé, Cameroon
*Corresponding author: Bang Guy Aristide, Surgery Unit, National Social Insurance Fund Health center of Yaoundé, Cameroon, E-mail: guyaristidebang@yahoo.fr
Trauma Cases Rev, TCR-3-050, (Volume 3, Issue 1), Case Report; ISSN: 2469-5777
Received: October 16, 2016 | Accepted: February 24, 2017 | Published: February 27, 2017
Citation: Bang GA, Nana Muluem A, Nana Oumarou B, Ngo Yamben MA, Handy Eone D (2017) Kirschner Wire Migration from Proximal Humerus into the Lung: Brief Report. Trauma Cases Rev 3:050. 10.23937/2469-5777/1510050
Copyright: © 2017 Bang GA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Although uncommon, migration of wires to solid organs or body cavities has been reported in the literature with potentially lethal complications. Wire migration into the lung is rare.
Case presentation: Herein, we report a case of a 26-year-old woman with Kirschner wire migration from the right shoulder to the thorax, piercing through the upper lobe of the right lung with hemopneumothorax and atelectasis. The wire was later removed through thoracotomy approach. The postoperative course was significant about an acute respiratory distress syndrome (ARDS) managed successfully.
Conclusion: As the migration of wires during orthopedic surgery can occurred with severe complications, they should be used cautiously and followed closely when inserted. A migrated Kirschner wire into the lung can be a challenging case for physicians especially in postoperative period.
Keywords
Kirschner wire migration, Lung traumatism, ARDS
Introduction
Orthopedic metallic wires and pins are frequently used for the fixations of fractures, especially fractures and dislocations of the shoulder girdle including the proximal humerus, clavicle, acromioclavicular joint and sternoclavicular joint. Kirschner wires (K-wire) are one of the earliest modalities introduced in the earliest 20th century by Martin Kirschner [1]. Although uncommon, migration of wires to solid organs or body cavities has been reported in the literature. A migrated wire can have dire consequences, prompt recognition and immediate retrieval of the implant is paramount to avert these complications [2]. Herein, we present a case of a 26-year-old woman in whom a K-wire, previously placed for fixation of a two-part proximal humerus fracture, migrated into the right lung parenchyma and was removed successfully via thoracotomy.
Case Presentation
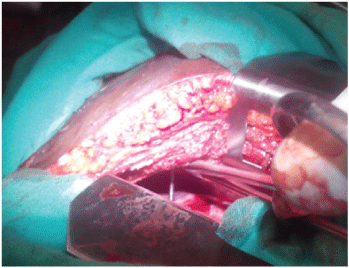
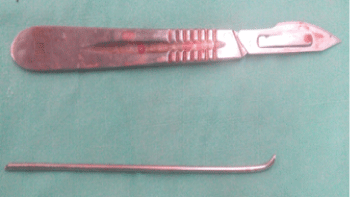
A 26-year-old woman presented, after convulsions due to severe malaria, a fracture-dislocation of the right shoulder associating a subglenoid anterior glenohumeral dislocation with a two-part fracture of the proximal humerus (surgical neck). She then underwent, through a deltopectoral approach, an open reduction and internal fixation with two K-wires (Figure 1) at another hospital. Four weeks later, she presented intermittent right thoracic pains associated sometimes with dyspnea. A reoperation for K-wires removal was performed 6 weeks after their insertion, without preoperative X-ray, and only one wire was found during the surgery. A postoperative X-ray was realized and revealed the second K-wire migrated into the thorax (Figure 2) and the patient was transferred to our department for removal. At admission, she complained about dyspnea and physical assessment showed a normal blood pressure, a pulse of 110 min-1 and a respiratory rate of 24 min-1. A thoracic CT-Scan revealed that the wire pierced through the upper lobe of the right lung with its proximal extremity located under the hull (Figure 3A), behind the pericardium and in front of the descending aorta, leading to an atelectasis of the right lung with a hemopneumothorax (Figure 3B). An emergency postero-lateral right thoracotomy was performed. After removing blood clots inside the pleural cavity, we discovered an adhesion binding the upper lobe of the right lung to the chest wall; palpation of this adhesion found at its base a hard consistency advocating the presence of the wire. After adhesiolysis, the proximal extremity of the K-wire became visible (Figure 4). The pin was then removed through axial traction (Figure 5), the lung tear was sutured with 4/0 Prolène and a thoracic drainage was performed with 2 drains. The postoperative course was significant of an acute respiratory distress syndrome (ARDS) and the patient was kept in intensive care unit under orotracheal intubation during 3 days with mechanical ventilation and sedation. The thoracic drainage was removed at postoperative day 5 and the patient was discharged at day 7. The patient was returned to the orthopedic surgeons for evaluation of the shoulder.
.
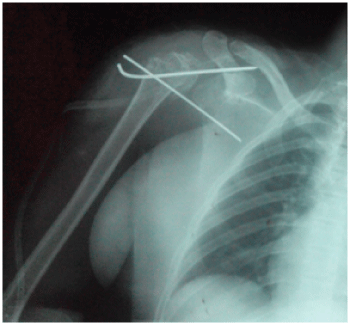
Figure 1: Postoperative osteosynthesis shoulder radiograph showing the 2 K-wires placed.
View Figure 1
.
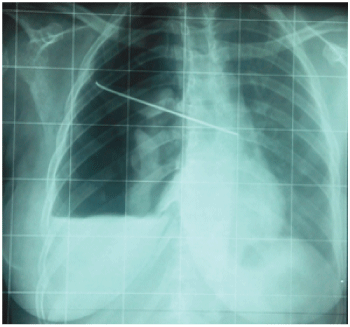
Figure 2: Postoperative chest radiograph showing intrathoracic migration of one of the K-wires with a right hemopneumothorax.
View Figure 2
Discussion
Metallic orthopedic fixation devices (pins and wires) have been used since the 1930s but the incidence of their migration is unknown. On reviewing articles from databases including PubMed, Elsevier, Cochrane library, EMBASE and Web of sciences from 1943 to 2015, Tan, et al [1] found 102 cases of orthopedic wire migration. The most common primary site of fixation where migration often occurred is the sternoclavicular joint, followed by the clavicle, the acromioclavicular joint and the proximal humerus [3]. However, a few cases originated from the pelvic bone [4], the finger [5], the femur [6] and the rib [7] have been reported. Migrating K-wire has been reported as early as the day after fixation and as late as 2 years [8]. The final reported resting position of the migrated K-wire involved vascular structures (ascending aorta, pulmonary artery, heart [9]), lung, mediastinum, oesophagus, spinal column, posthepatic retroperitoneal space, spinal canal and the spleen (which a K-wire reached from the right shoulder within 12 hours) [1,10,11].
.
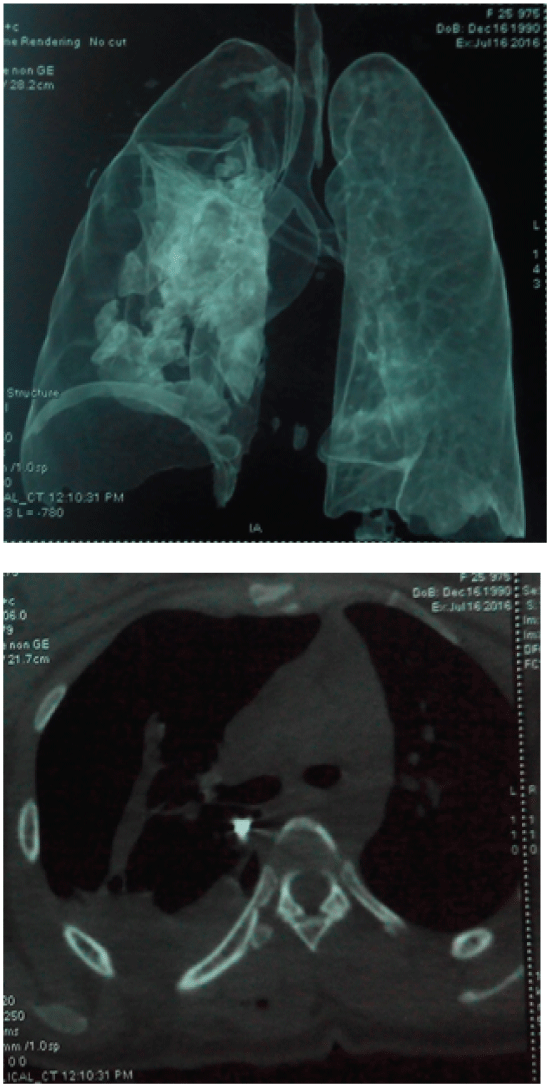
Figure 3: Thoracic CT-scan showing A) Proximal extremity of the migrated wire (blue arrow) under the hull in front of the descending aorta, leading to an atelectasis of the right lung; B) Proximal extremity of the migrated wire (blue arrow) behind the pericardium with hemopneumothorax.
View Figure 3
Various causative mechanisms of wire migration into the thorax have been proposed including: muscle action, the great freedom of movement of the shoulder, negative intrathoracic pressure associated with respiration, regional resorption of bone, gravitational force and even capillary action [1,12]. The type of wire, smooth, threaded or bent, seems not to be a factor in incidence [8].
In our case, the migrated K-wire had an unusual position since it pierced through the upper lobe of the right lung with atelectasis of the involved lung, the proximal extremity of the wire being in front of important vascular structures. Thus justify the emergency removal of the wire. The postoperative ARDS was revisable in regard of the preoperative lung injuries and is a life-threatening condition associated with a high mortality rate. Fortunately our patient survived after intensive resuscitation care with prolonged intubation. In the 102 cases of migrating wires reported since 1943 [1], 11 deaths from catastrophic cardiovascular events were reported with 1 due to a migration into the lung. Video-assisted thoracoscopy can be an approach for removal for experienced surgeons but wasn't used in this case due to the localization of the wire and the possible tears of big vessels during extraction.
The present report draws attention to the risk of severe complications due to a migrated K-wire. The most important recommendations for preventing lethal complications of K-wire migrations are [8], to bend the exposed part of the wire/pin after fixation, close clinical follow-up with frequent postoperative radiographs (lacking in our case), removal of the wire as soon as the treatment period is over, immediate removal of a migrating wire and restricted used of wire/pin as possible.
Conclusion
A migrated wire/pin can cause potentially lethal complications. Surgeons need to be aware especially when wires are used for shoulder girdle fractures. A migrated wire should be removed immediately.
Ethical Statement
Written informed consent was obtained from our patient for publication of this case report and accompanying images. Our institutional ethical committee board approved this work.
Authors' Contributions
The patient was admitted under the care of Blondel Nana Oumarou. She was operated by Albert Nana Muluem and Guy Aristide Bang. All authors contributed in writing the manuscript, read and approved the final draft.
References
-
Tan L, Sun DH, Yu T, Wang L, Zhu D, et al. (2016) Death due to intra-aortic migration of Kirschner wire from the clavicle. Medicine 95: e3741.
-
Sergides NN, Nikolopoulos DD, Yfadopoulos DK, Novi EA, Kanata MP (2009) Intrathoracic migration of a Steinman wire: a case report and review of the literature. Cases J 2: 8321.
-
Freund E, Nachman R, Gips H, Hiss J (2007) Migration of a Kirschner wire used in the fixation of a subcapital humeral fracture, causing cardiac tamponade: case report and review of literature. Am J Forensic Med Pathol 28: 155-156.
-
Park SY, Kang JW, Yang DH, Lim TH (2011) Intracardiac migration of a Kirschner wire: case report and literature review. Int J Cardiovasc Imaging 27: 85-88.
-
Haapaniemi TA, Hermansson US (1997) Cardiac arrhythmia caused by a Kirschner wire inside the heart: an unusual complication of finger osteosynthesis. J Hand Surg Br 22: 402-404.
-
Ono M, Goerler H, Boethig D, Breymann T (2010) Surgical removal of Kirschner wire from the right ventricle, migrated from the femur. Eur J Cardiothorac Surg 37: 486.
-
Weizhi Z, Fenglin S, Yifeng Y, Jingqun T (2014) Asymptomatic intracardiac migration of a Kirschner wire from the right rib. Interact Cardiovasc Thorac Surg 18: 525-526.
-
Kumar P, Godbole R, Rees GM, Sarkar P (2002) Intrathoracic migration of a Kirschner wire. J R Soc Med 95: 198-199.
-
Hedon C, Khoueiry Z, Verges M, Pasquie JL (2015) Late intracardiac orthopedic wire presenting as tamponade and stroke. Eur Heart J 36: 1546.
-
Rajesh PB, Nair KK (1991) Unusual migration of a Kirschner wire. Eur J cardiothoracic Surg 5: 164.
-
Mankowski B, Polchlopek T, Strojny M, Grala P, Slowinski K (2016) Intraspinal migration of a Kirschner wire as a late complication of acromioclavicular joint repair: a case report. J Med Case Rep 10: 66.
-
Lyons FA, Rockwood CA Jr (1990) Migration of pins used in operation on the shoulder. J Bone Joint Surg 72: 1262-1267.