Trauma Cases and Reviews
Delayed-Onset Pericarditis in Non-penetrating Blunt Force Trauma: A Case Report
Andrew Mc Cague, Kerala Serio and Joanne Leibe*
Natividad Medical Center, California, USA
*Corresponding author: Joanne Leibe, Natividad Medical Center, 1441 Constitution Blvd, Salinas, California 93912, USA, E-mail: hotlightscoldsteel@gmail.com
Trauma Cases Rev, TCR-2-047, (Volume 2, Issue 3), Case Report; ISSN: 2469-5777
Received: July 18, 2016 | Accepted: December 20, 2016 | Published: December 24, 2016
Citation: Mc Cague A, Serio K, Leibe J (2016) Delayed-Onset Pericarditis in Non-penetrating Blunt Force Trauma: A Case Report. Trauma Cases Rev 2:047. 10.23937/2469-5777/1510047
Copyright: ©2016 Mc Cague A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
There have been rare documented instances where blunt-force trauma has been suspected to cause a delayed disease process that manifests days or weeks after the initial injury. This is a case report of a 30 year old male who suffered blunt chest trauma during a motor vehicle accident.
On hospital day five the patient began to complain of significant chest pain, an increase in pain with each heartbeat, increased pain when sitting up, shortness of breath and experienced a syncopal episode in the shower. His EKG was suggestive of pericarditis and the etiology was suspected to be secondary to acute chest trauma. The patient was started on conservative management and his symptoms resolved prior to discharge. At one year follow up there was no recurrence of symptoms.
This case represents a rare case of delayed-onset post-traumatic pericarditis, and is additionally unique in that took place in the absence of pericardial effusion, setting it apart from previously documented cases. This report contains a brief literature review of previously documented causes of delay-onset pericarditis, a description of the patient's hospital course and discussion of treatment choices and clinical reasoning.
Introduction
First described by Dressler, et al in 1956 [1], pericarditis has been found to have many well-documented causes that vary from viral and bacterial infections, radiation exposure, neoplasms, cardiac injury, autoimmune disorders, drug exposure and metabolic disease. In the same year, Baker, et al reported a case of a man who developed late constrictive pericarditis following hemopericardium from a stab wound [2]. Since then, there have been rare documented instances where blunt-force trauma has been suspected to cause a delayed disease process that manifests days or weeks after the initial injury [2].
The case presented here describes pericarditis which presented five days after blunt chest injury and resolved with conservative treatment. This case is unique in that it represents a rare case of traumatic pericarditis in the absence of pericardial effusion.
Case Description
The patient is a 30-year-old male who was the driver in a head-on motor vehicle collision in a sedan with speeds in excess of 60 mph. Emergency crews reported airbag deployment, seat belt use, and 10 inch passenger space intrusion due to crumpling of the dashboard and steering column. The patient self-extricated and reported loss of consciousness of unknown duration. He was transported to the emergency room by helicopter and presented with left leg pain and pain with inspiration. ATLS protocol was followed finding airway intact, lungs were clear, regular rate and rhythm without muffled heart sounds, and GCS was 15, without neurological compromise. Further radiographic work-up on CT Chest/Abdomen/Pelvis revealed a left femur fracture and possible bilateral pulmonary contusions and a small amount of fluid around the left lobe of the liver; no evidence of aortic aneurysm or acute traumatic aortic injury was seen. He underwent open reduction internal fixation of his left femur fracture.
His hospital course was complicated by a left popliteal deep vein thrombosis requiring anticoagulation and mild rhabdomyolysis with total creatinine kinase of 9400 U/L. CT Chest obtained to rule out pulmonary embolism noted stable heart size without acute aortic pathology.
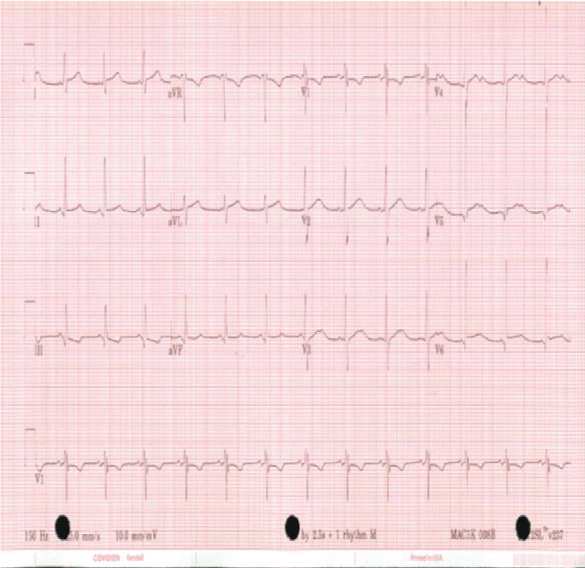
On hospital day five the patient began to complain of significant chest pain, an increase in pain with each heartbeat, increased pain when sitting up, and shortness of breath. He also experienced a syncopal episode in the shower. Labs showed a slight increase in troponin (0.06). At this time all other lab values were within normal limits except an increase in Lactic Acid to 8.2 mmol/L from 1.54 mmol/L the previous day, and diminished but stable Hemoglobin of 8.1 g/dL and Hematocrit of 23.2%. Cardiac exam revealed a 3-component pericardial rub. EKG was suggestive of pericarditis with diffuse ST elevation (Figure 1). Echocardiogram showed no evidence of pericardial effusion with normal ventricular size and function, and mild pulmonary hypertension and right atrial enlargement reflecting lung contusion. Etiology is suspected to be secondary to acute chest trauma.
The patient was started on indomethacin 50 mg PO Q8 hours and colchicine 0.5 mg PO twice daily. He was also given proton pump inhibitor for GI prophylaxis because of the concomitant use of anticoagulation. By hospital day nine the patient's symptoms had resolved and he was discharged to an acute rehabilitation unit for further physical therapy with a 3-week prescription of colchicine.
At one year follow-up the patient remains to be symptom free.
Discussion
This is a case of pericarditis which presented five days after blunt chest injury and resolved with treatment. This case represents a rare case of traumatic pericarditis in the absence of pericardial effusion.
The pathophysiology of post-traumatic pericarditis has been suggested to be of autoimmune origin [3]. In instances of hemopericardium, which is more common with penetrating injuries, it is suggested that the entrance of blood into the pericardium incites an inflammatory reaction that sparks an autoimmune process [4]. The connection between blunt force trauma and pericardial inflammation remains unclear but a similar mechanism may play a role in areas of inflammation.
Documented instances of pericardial injury following blunt force trauma include an account of acute pericarditis in a 19-year-old male. This patient suffered from a 40 feet fall causing orthopedic fractures and splenic injury. He later developed symptomatic pericarditis with effusion and tamponade requiring pericardectomy twelve days after the initial injury [5]. An account of constrictive pericarditis has been described in a 72-year-old male patient who developed dyspnea and lower extremity edema one year after striking his sternum on a trailer hitch during a fall [6]. Another case of constrictive pericarditis was documented in a 21-year-old man who presented with a 7 month history of progressively worsening dyspnea, lower extremity edema and ascites [7]. While a specific blunt force injury was not listed in the case report, the authors assumed that, given the patient's age and gender, and absence of other causes, that blunt chest injury was a likely factor for disease process [7].
To compare to Khidir, et al. account of the 19-year-old who suffered a 40 foot fall, our patient's echocardiogram did not reveal pericardial effusion. This could be due to the presence of a seat belt which softened the impact during the crash, or due to a difference in direction of initial impact (anterior to posterior versus unknown). Two of the aforementioned cases of constrictive pericarditis (Anderson, et al. and Erkan, et al.) are suggestive of a more chronic disease process in the absence of accounts of acute inflammatory process. While it's possible that trauma-induced pericarditis can be either acute or chronic, it is also possible, or perhaps more likely, that there is a spectrum of combinations of the two, and those acute symptoms may very likely be masked by the musculoskeletal injury accompanying the initial trauma.
In the above case, the diagnosis of acute pericarditis was established based on physical exam and EKG. Diagnostic guidelines suggest that acute pericarditis is likely when a patient has at least two of the following symptoms or signs: chest pain consistent with pericarditis, pericardial friction rub, typical ECG changes, or a pericardial effusion of more than trivial size [8]. Given the vast differential for chest pain, the additional diagnostic tools (Echo, EKG) become integral tools for diagnosis. In this case the mechanism is presumed to be due to blunt trauma given the absence of other inciting factors (infectious etiology, recent viral illness, neoplasm, metabolic disease). The possibility remains that the cause is idiopathic; however, given the significant blunt chest trauma sustained by the patient, this is the most likely inciting factor.
The patient was treated with indomethacin 50 mg every eight hours by mouth and colchicine 0.5 mg by mouth twice daily. Aspirin or NSAIDs are considered current standard of care for initial treatment [9]. The most commonly used agents are ibuprofen (600 to 800 mg every 6 to 8 hours), indomethacin (25 to 50 mg every 8 hours), and aspirin (2 to 4 g daily in divided doses) [9]. While 70% to 90% of cases of acute pericarditis resolve completely, recurrent pericarditis is a troubling complication [9]. Colchicine has been associated with decreased incidence of recurrent pericarditis in addition to greater symptom relief in the acute phase [10,11]. In this case, diagnosis and treatment of post-traumatic pericarditis do not differ from pericarditis of a non-traumatic origin. Other treatments of pericarditis include pericardial drainage and pericardectomy (pericardial window) in the case of significant pericardial effusion and recurrent episodes leading to constrictive pericarditis [12,13]. If left untreated, complications of pericarditis include cardiac tamponade, constrictive pericarditis and effusive-constrictive pericarditis [14,15].
This unusual presentation of pericarditis was treated conservatively and the patient resolved without recurrence of symptoms.
Conclusion
This case report is an account of pericarditis following blunt force trauma. Though diagnosis remains challenging, clinicians should maintain a high level of suspicion for the disease process in patients presenting with delayed on-set chest pain following blunt force trauma. Early detection and treatment are integral for preventing a chronic disease process that can lead to constrictive pericarditis and heart failure.
Conflict of Interest
Joanne Leibe DO, Kerala Serio MD and Andrew Mc Cague DO declare that they have no conflict of interest.
Compliance with Ethical Requirements
All human and animal studies have been approved by the appropriate ethic committee and have therefor been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
References
-
William Dressler (1956) A Post-Myocardial-Infarction Syndrome: 160: 1379-1383.
-
Raker JW, Langfeld SB, Gowen GF (1958) Traumatic hemopericardium producing late constrictive pericarditis; report of a case. Ann Surg 148: 134-138.
-
Qureshi I, Durrani N (2010) Cardiac tamponade resulting from trauma--induced effusive pericarditis. Am Surg 76: 1020-1021.
-
Chong HH, Plotnick GD (1995) Pericardial effusion and tamponade: evaluation, imaging modalities, and management. Compr Ther 21: 378-385.
-
Khidir HH, Bloom JP, Hawkins AT (2015) Delayed recurrent pericarditis complicated by pericardial effusion and cardiac tamponade in a blunt trauma patient. J Emerg Trauma Shock 8: 49-51.
-
Eric M Anderson, Dawn E Jaroszewski, Francisco A Arabial (2011) Blunt trauma as a suspected cause of delayed constrictive pericarditis: a case report. J Med Case Rep 5: 76.
-
Erkan Kaya, Kubilay Karabacak, Murat Kadan, Murat Celik, Uygar Cagdaş Yuksel, et al. (2015) PP-068 Physiological Significant Constrictive Pericarditis After Blunt Trauma: A Case Report. The American Journal of Cardiology S127-S128.
-
Bernhard Maisch, Petar M Seferović, Arsen D Ristić, Raimund Erbel, Reiner Rienmüller, et al. (2004) Guidelines on the Diagnosis and Management of Pericardial Diseases Executive Summary. European Heart Journal 25: 587-610.
-
Martin M LeWinter (2014) Acute Pericarditis. N Engl J Med 371: 2410-2416.
-
Alabed S, Cabello JB, Irving GJ, Qintar M, Burls A, et al. (2014) Colchicine for pericarditis. Cochrane Database Syst Rev 28: CD010652.
-
Massimo Imazio, Antonio Brucato, Roberto Cemin, Stefania Ferrua, Stefano Maggiolini, et al. (2013) A Randomized Trial of Colchicine for Acute Pericarditis. N Engl J Med 369: 1522-1528.
-
Khandaker MH, Schaff HV, Greason KL, Anavekar NS, Espinosa RE, et al. (2012) Pericardiectomy vs medical management in patients with relapsing pericarditis. Mayo Clin Proc 87: 1062-1070.
-
Imazio M, Adler Y (2013) Management of pericardial effusion. European Heart Journal 16: 1186-1197.
-
Permanyer-Miralda G, Sagrista-Sauleda J, Soler-Soler J (1985) Primary acute pericardial disease: a prospective series of 231 consecutive patients. Am J Cardiol 56: 623-630.
-
Zayas R, Anguita M, Torres F, Giménez D, Bergillos F, et al. (1995) Incidence of specific etiology and role of methods for specific etiologic diagnosis of primary acute pericarditis. Am J Cardiol 75: 378-382.