Trauma Cases and Reviews
Isolated Dislocation of the Tarsal Navicular without Fracture: Case Report
Maicon Bonaldo Dias1*, Bruna Zagonel1, Melissa Sofia Dickel1, Jessica Arsego Talheimer1, Isabel Schuster Argenton1, Jeniffer Charlene Silva Dalazen1, Bruno Vicenzo Thomas Bresolin1, Gabriel Alves Martinelli1, Osvaldo Iha Yoshida1, Patrícia Tirelli Lena1, Romualdo de Lima Pilecco1, Vitor Hugo Peijo Galerani1, Ana Cristina Eickhoff1, Eduardo Rosa Otharan2 and Rafael Duvelius Ott3
1Centro Universitário Univates, Rio Grande do Sul, Brazil
2Hospital Estrela, Estrela, Rio Grande do Sul, Brazil
3Hospital São Lucas da PUCRS, Porto Alegre, Rio Grande do Sul, Brazil
*Corresponding author: Maicon Bonaldo Dias, Medical Student, Centro Universitário Univates, Rio Grande do Sul, Brazil, E-mail: maicondias5@hotmail.com
Trauma Cases Rev, TCR-2-045, (Volume 2, Issue 3), Case Report; ISSN: 2469-5777
Received: September 01, 2016 | Accepted: November 24, 2016 | Published: November 28, 2016
Citation: Dias MB, Zagonel B, Dickel MS, Talheimer JA, Argenton IS, et al. (2016) Isolated Dislocation of the Tarsal Navicular without Fracture: Case Report. Trauma Cases Rev 2:045. 10.23937/2469-5777/1510045
Copyright: © 2016 Dias MB, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Isolated dislocation of the tarsal navicular bone is a rare lesion. The mechanism of this specific trauma is still not well to understood, due to the strength needed in different ways and directions for its occurrence, in a complex way. Few cases of an isolated dislocation of the navicular reported in medical literature, and there is little information about complications how the patients evolve after years of postoperative. The authors present a case of a woman, 39-years-old, who suffered a complete dislocation of the talus-navicular of her left foot, due to a fall. After initial k-wire fixation, the patient presented herself 6 weeks later with chondrolysis of the tarsus articulations and submitted to selective arthrodesis of talus navicular and cuneiform medial-talus-navicular (TN + CTN). Having passed 13 years of post-surgery, the patient presents a good clinical evolution and articulation functionality. It concluded that the isolated navicular dislocation, even though promptly and adequately reduced and stabilized, may develop complications, such as chondrolysis, and the correct handling by selective arthrodesis enables a satisfactory functional and clinical outcome.
Keywords
Isolated dislocation of the tarsal navicular, Chondrolysis, Arthrodesis
Introduction
The navicular is a flat bone, concave, ship-shaped localized between the head of the talus and the three cuneiform, and is rigidly stabilized by a large network of plantar and dorsal ligaments [1,2]. The strategic location of the bone in the upper portion of the mid tarsal infers great importance in controlling body weight during ambulation [3]. Due to the large portion of ligaments and their anatomical structure, isolated dislocation of the tarsal navicular is a lesion with very low incidence, associated with navicular or other mid tarsal fractures [2-4]. Because of the rarity of presentations, there is low knowledge about the mechanism of the injury. It was related the necessity of forces in different directions, reflecting a complex mechanism and a complicated way to decide the correct diagnosis and treatment process [3-6].
This study aims to report a case of long clinical follow-up of an isolated tarsal navicular dislocation without fracture, including diagnosis, treatment and complications.
Case Report
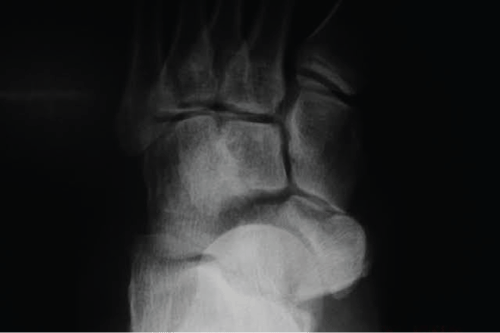
Patient of 39-years-old, female, business woman of the transport branch, was admitted to the emergency room, after suffering a truck fall, reporting that she was wearing high heels at the time of the fall. She presented a sprain in her left foot with severe edema. Normal neurovascular physical examination. An X-ray performed, which showed isolated dislocation of the navicular and rupture of the dorsal talonavicular, calcaneonavicular and cuneonavicular ligaments (Figure 1). No lesion on the posterior tibial tendon reported. According to the AO and Tscherne classification of closed fractures, it was a closed fracture grade 0 (Fr. C 0) [7].
.
Figure 1: Preoperative X-ray showing isolated dislocation of the tarsal navicular.
View Figure 1
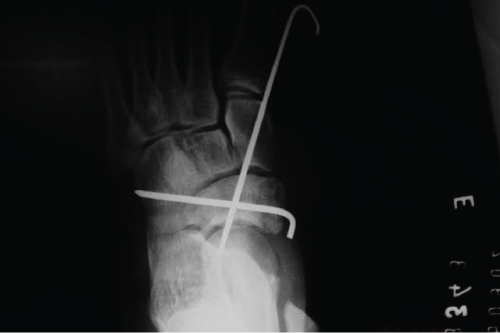
The patient underwent surgery on the same day, with open reduction and fixation with two Kirchner wires. The first one, crossed between the medial cuneiform, navicular and talus, and the other fixed between the navicular and cuboid (Figure 2).
.
Figure 2: Fixation with two crossed K-wires. One between the medial cuneiform, navicular and talus, and another between the navicular and cuboid.
View Figure 2
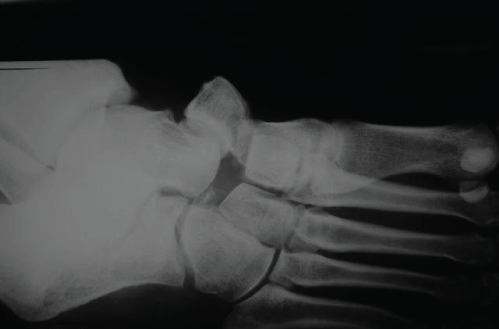
The K-wires maintained for 7 weeks after the first surgery, together with the use of a plaster boot. Patient, then, had the wires removed (Figure 3), referred to physiotherapy and had total load liberated 7 weeks after the wire removal. Patient developed a complete recovery from foot range of motion and discharged asymptomatically.
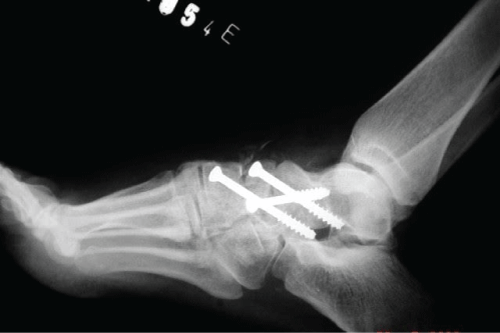
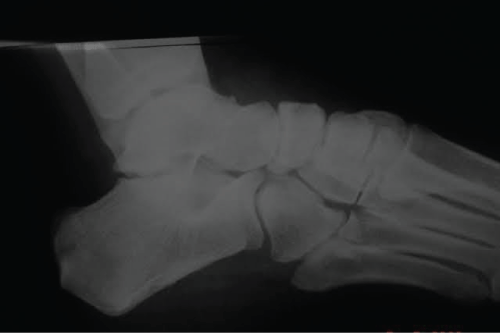
About five months after the initial injury, the patient had a medical appointment again, due to pain and edema in the left tarsus, especially in the late afternoon, after normal work routine that involved intense walks in high heels. Radiography performed, it showed signs of chondrolysis (Figure 4)-a complication also described in the literature, which is cartilage degeneration with reduced blood supply, causing avascular necrosis of this structure and subluxation of the navicular [2]. CT scan performed, which confirmed the chondrolysis with degenerative changes in the talusnavicular and cuneiform joints. Because of this injury, the patient was submitted to selective arthrodesis with in situ fusion of the left tarsus [8] (Figure 5) - procedure performed to cause bone fusion in a joint, thereby causing immobility-with three cannulated cancellous screws of 4.5 mm, with very satisfactory final result. The open reduction internal fixation done through dorsomedial surgical access over the navicular with arthrodesis of talus navicular and cuneiform medial-talus-navicular (TN+CTN). Postoperatively the plaster boot used for 9 weeks. Subsequently, the X-ray showed consolidated arthrodesis, and the patient liberated to ambulation with hard shoes for another 60 days. About a year later, the removal of the screws done.
.
Figure 4: X-ray showing chondrolysis in talusnavicular and navicular cuneiform joints.
View Figure 4
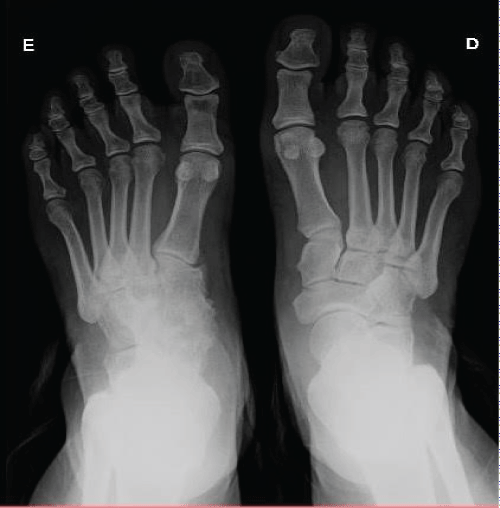
Thirteen years after the initial injury, the patient consulted again with no complaint in operated tarsus, reporting being able to dance and walk normally. Radiography and ultrasonography performed on both feet, and they demonstrated that arthrodesis consolidated on the left foot (Figure 6). The consolidation is as expected and it does not cause major movement limitation to the patient.
.
Figure 6: Antero-posterior plain X-ray 13 years after ORIF showing the consolidation in her left foot.
View Figure 6
Summary and Conclusion
Isolated dislocation of the tarsal navicular is an unusual event [2]. Usually, fractures or other damage were associated with it, as fracture-dislocations of the navicular or associated with fractures, subluxation or dislocation of talus, cuneiform, cuboid and other tarsal bones [9,10]. The rarity of this injury attributed to the rigid bone and ligamentous support surrounding the navicular, which usually undergoes fracture and dislocation rather than pure dislocation of the navicular [11]. The majority of the cases constituted of a displacement of the medial and plantar navicular to its normal position, with neuropathic or dorsal instability, as an example of acute trauma [2]. The most common trauma mechanism appears to be constituted of an initial hyper-plantar flexion of the forefoot with subsequent axial load. Typically, there is a rupture of the involved ligaments, first as the naviculocuneiform, followed by the plantar naviculocuneiform. The ligaments of plantar talonavicular support are the last ones to suffer [12].
The objective of tarsus lesions treatments is the functional structure maintenance. Therefore, the structure stability and the normal relation of load support surfaces of the hindfoot to the forefoot maintenance is of great importance. There are other publications of similar cases successfully treated by open reduction and arthrodesis of the naviculocuneiform and calcaneocuboid joints [13]. There are also different methods of existent treatments, mainly when navicular tarsal fracture exists. One could mention closed reduction, opened reduction and external fixation, merger process, triple arthrodesis and partial or total excision [14]. Management includes accurate reduction and fixation along with regular physiotherapy. They are at increased risk of specific set of complication, like osteonecrosis and chondrolysis [4-6,8-15,16]. Avascular necrosis of the navicular bone is the most described complication, it is estimated at nearly (25%) from all reported cases [17].
Open reduction and fixation with K-wire followed by physical therapy is the best treatment for navicular dislocation, providing good functional evolution of the foot. However, chondrolysis of the joints is a complication of this type of injury [2]. In our report, was evidenced chondrolysis of the talusnavicular and naviculocuneiform joints, 5 months after K-wire reduction.
The recognition of the navicular injuries vary since clear deformities to loss of function and chronic pain [16]. The CT is essential on the diagnoses and on the classification of the injuries in a complex foot trauma. In our case, the CT performed 5 months after the acute trauma, given the patient complaint and the chondrolysis signs on the X-ray. Due to the time that the lesion and the service occurred (2003), there is no saved data about the CT. However, it is good to highlight that the initial practice (K-wire reduction) and the arthrodesis performed after the chondrolysis evincement would not be different.
In our case, we can evaluate the patient 13 years post-surgery and it is evidenced that the tarsus selective arthrodesis through the cannulated screws makes a satisfactory final result possible, determining an arthrodesed functional foot and with great clinical result [16].
Acknowledgment
Ms. Rafael Moreno Ferro de Araújo, teacher at Univates.
References
-
Eric E Coris, John A Lombardo (2003) Tarsal navicular stress fractures. Am Fam Physician 67: 85-90.
-
MS Dhillon, ON Nagi (1999) Total dislocations of the navicular: are they ever isolated injuries? J Bone Joint Surg Br 81: 881-885.
-
M.A.Q. Ansari (2016) Isolated complete dislocation of the tarsal navicular without fracture: A rare injury. Tzu Chi Medical Journal 28: 128-131.
-
Singh VK, Abhishek Kashyap, Gauresh Vargaonkar, Ramesh Kumar (2015) An isolated dorso-medial dislocation of navicular bone: A case report. J Clin Orthop Trauma 6: 36-38.
-
Filgueira, Eriko G Chiesa, Fabricio L Lima, Oton N (2000). Luxacao isolada do navicular: relato de caso. Rev bras ortop 35: 266-267.
-
Main BJ, Jowett RL (1975) Injuries of the midtarsal joint. J Bone Joint Surg 57-B: 89-97.
-
RuEdi TP, Murphy WM (2007) AO principles of fracture management. Stuttgart and Thieme, New York, USA.
-
Canale ST, Beaty JH (2013) Campbells operative orthopaedics. (12 edn) Elsevier Health Sciences, USA.
-
Williams DP, Hanoun A, Hakimi M, Ali S, Khatri M (2009) Talonavicular dislocation with associated cuboid fracture following low-energy trauma. Foot Ankle Surg 15: 155-157.
-
Rockwood CA, Green DP (2010) Fractures and dislocations of the midfoot and Forefoot. In: Bucholz RW, Heckman JD, CourtBrown CM, Tornetta III P, Rockwood and Green's Fractures in Adults. ((7th edn), Lippincott Williams & Wilkins, Philadelphia, USA.
-
Davis, Adrian T, Kuldjanov D (2013) Complete Medial Dislocation of the Tarsal Navicular without Fracture: Report of a Rare Injury. J Foot Ankle Surg 52: 393-396.
-
Bucholz RW, Heckman JD, Court-Brown CM, Tornetta P (2011) Fractures in adults. (7th edn), Wolters Klumer Health, Spain.
-
Rao H (2012) Complete Open Dislocation of the Navicular: A Case Report. J Foot Ankle Surg 51: 209-211.
-
Mathesul AA, Sonawane DV, Chouhan VK (2012) Isolated tarsal navicular fracture dislocation: a case report. Foot Ankle Spec 5: 185-187.
-
Yoshino N, Noguchi M, Yamamura S, Takai S, Hirasawa Y (2001) Bilateral isolated tarsal navicular fracture dislocation: a case report. J Orthop Trauma 15: 77-80.
-
Dhillon MS, Gupta R, Nagi ON (1999) Inferomedial (subsustentacular) dislocation of the navicular: a case report. Foot Ankle Int 20: 196-200.
-
Hamdi K, Ben Ghozlen Hazem, Zitoun Yadh, Abid Faouzi (2015) Isolated dorsal dislocation of the tarsal naviculum. Indian J Orthop 2015 49: 676-679.