Trauma Cases and Reviews
Cyst-Like Cortical Defects Following Fractures in Children: Series of 5 Cases
Inmaculada González Pérez1*, José T López Salinas1, Luis A Gómez Navalón1, Patrick Pilkington Woll2 and Patricia Vivar del Hoyo1
1University General Hospital of Ciudad Real, Spain
2University Hospital 12 de Octubre, Madrid, Spain
*Corresponding author: Inmaculada González Pérez, MD, University General Hospital of Ciudad Real, Obispo Rafael Torija, s/n, 13005 Ciudad Real, Spain, Tel: +34 926 27 80 00, E-mail: inmaglezp86@gmail.com
Trauma Cases Rev, TCR-2-040, (Volume 2, Issue 2), Clinical Cases; ISSN: 2469-5777
Received: May 22, 2016 | Accepted: August 12, 2016 | Published: August 14, 2016
Citation: Pérez IG, Salinas JTL, Navalón LAG, Woll PP, del Hoyo PV (2016) Cyst-Like Cortical Defects Following Fractures in Children: Series of 5 Cases. Trauma Cases Rev 2:040. 10.23937/2469-5777/1510040
Copyright: © 2016 Pérez IG, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Purpose: The cyst-like defect following a fracture is an uncommon lesion with a few cases described in the literature. We want to present a series of 5 cases showing up in different locations, with treatment required for one of the defects.
Methods: We present a series of 5 cases of cyst-like defect following fractures in children. The cyst-like defects were in different locations.
Results: One cyst-like defect needed treatment because of progressive increase in size and risk of fracture, another required biopsy to determine their lineage and the rest did not require any treatment.
Conclusion: The cyst-like defect post fracture in children are uncommon lesions, and despite being the radius the most common location and rarely requiring treatment we can find atypical locations and in some cases surgery is needed to prevent fractures or to confirm its histopathology.
Keywords
Cyst-like cortical defects, Post fracture injury, Lytic lesion, Benign lesion, Fracture in children
Introduction
The cyst-like cortical defect is a common lesion. In many cases it is an incidental finding without clinical manifestation and does not require treatment.
However, despite being a frequent injury, it is uncommon to find it following a fracture. This phenomenon can occur in children after suffering a non-displaced fracture or a fracture with discreet displacement. The most frequent location is the distal radius.
There are not many cases reported in the literature, the largest series is of nine cases [1]. In our work we will present a series of five cases in different anatomical locations.
Clinical Cases
We present a series of five cases of children with ages between 6 and 11-years-old. All the patients went to the emergency room after suffering an accidental fall, the caused fractures in different location.
Clinical case no 1
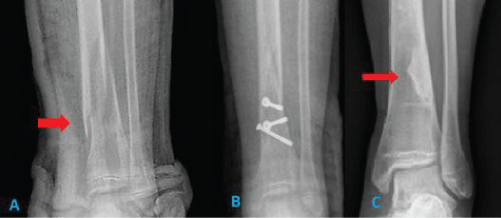
An 11-year-old girl with a fracture on the distal tibia treated conservatively with plaster. After suffering secondary displacement, it required fixation with screws. On follow-up she showed a cyst-like cortical defect in the same location (Figure 1), which didn't need treatment. After 8 years it persisted radiographically, although it was smaller than before.
.
Figure 1: a) Fracture on the distal tibia; b) Postoperative radiography; c) Cyst-like cortical defect after six years.
View Figure 1
Clinical case no 2
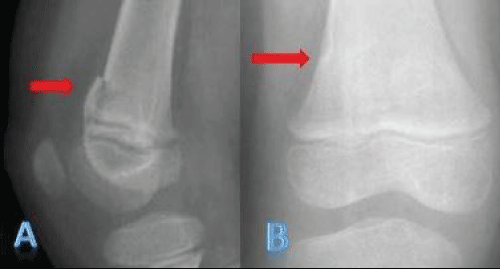
A 6-year-old boy with distal femoral fracture, treated conservatively. A cyst-like cortical defect was observed at two months (Figure 2), which disappeared after two and a half years. No treatment was required.
.
Figure 2: a) Fracture on the distal femur; b) Cyst-like cortical defect after two months.
View Figure 2
Clinical case no 3
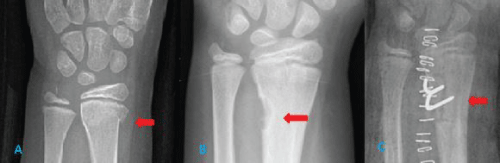
Eleven year old boy with distal radius fracture treated conservatively. On subsequent monitoring a cyst-like cortical defect appeared after 2 months. Because of the progressive increase in lesion size TC was performed, where cyst-like cortical defect was observed, which would endanger the integrity of the radius and increase the risk of fracture (Figure 3), so surgery was performed by curettage, filling with graft and more osteosynthesis (Figure 4). The histopathological diagnosis confirmed a cyst-like cortical defect (in the sample, compact and spongy bone tissue was seen as well as dark brown elastic tissue and a grey-like membranous tissue).The patient had a good evolution with complete filling and disappearance of the lesion.
.
Figure 4: a) Fracture on the distal radius; b) Cyst-like cortical defect after one year; C) Postoperative radiography.
View Figure 4
Clinical case no 4
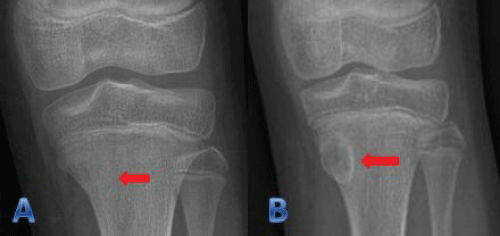
Another eleven year old child with proximal tibia fracture treated conservatively. On subsequent studies a poorly defined lesion appeared. An MRI study reported an infiltrating lytic lesion with no clear diagnosis. Biopsy was performed for histopathology study, which was reported as a cyst-like cortical defect. It didn't require treatment and it disappeared after 2 years (Figure 5).
.
Figure 5: a) Fracture on the proximal tibia; b) Cyst-like cortical defect after nine months.
View Figure 5
Clinical case no 5
A 10-year-old child who suffered distal tibia fracture and was treated by closed reduction and immobilization. In radiographic controls the appearance of cystic-like cortical defect was observed after 5 weeks, it didn't require treatment and it disappeared spontaneously after 2 years.
Discussion
The appearance of a cyst-like cortical defect after fracture is an uncommon finding. It can be found in children between 2 and 15 years old and it occurs after an undisplaced or minimally displaced fracture [2]. This injury sometimes appears during the consolidation process of the fracture [3].
At the time, and to our knowledge, no more than 30 cases have been reported in the literature. Of these, over 80% are post-fracture on the distal radius, which is the most frequent location [1], however, in our series, we showed uncommon and varied locations. They don't usually exceed 10 mm in size, are osteolytic, intracortical, not expansive, rounded or slightly oval and it can sometimes be multiple [4].
Its aetiology is unclear. Phillips and Keats attribute the cause to an intraosseous hematoma that when reabsorbed, forms the lesion [5]. On the other hand, Malghem and Maldague postulated that within the hematoma there is some fat accumulated because of the fracture, and that it remains trapped by the integrity of the periosteum. This theory is supported by TC scan findings, where the fat droplets were visible before the hematoma calcification [3,6]. Ball, et al. hypothesise that intramedullary fat is mixed with blood from the hematoma, and when it is reabsorbed, the lesion becomes radiologically visible [7].
Although it is considered a benign lesion that does not require treatment and disappear after 1 or 2 years, in our series we found one case which required surgical treatment because the defect increased in size, increasing the risk of new fracture. Furthermore, surgery allowed us to reach a definitive pathological diagnosis.
The differential diagnosis must be made with the aneurismal bone cyst, simple bone cyst, eosinophilic granuloma and infection. Biopsy is rarely necessary for diagnosis, because radiographic study is sufficient. Nevertheless, in our series, we needed pathological study for the final diagnosis of the proximal tibia defect.
Conclusion
The cyst-like cortical defect post fracture is an uncommon injury without many cases published in the literature. It usually appears after slightly displaced fractures and its most frequent location is the distal radius. Nevertheless, in our series, we describe this lesion presenting on different locations and with different types of fractures (displaced and non-displaced, with conservative treatment and with surgical treatment). Although it is a benign and self-limiting lesion, we have presented a case that required surgical treatment.
References
-
Pfister-Goedeke L, Braune M (1981) Cyst-like defects following fractures in children. Pediatr Radiol 11: 83-86.
-
Valverde Villar AM, Salcedo Montejo M (2012) Defecto cortical postraumático. A propósito de un caso. Rev Esp Cir Ortop Traumatol 56: 482-485.
-
Malghem J, Maldague B, Claus D, Clapuyt P (1990) Transiet cyst-like cortical defects following fractures in children. Medullary fat within the subperiosteal haematoma. J Bone Joint Surg Br 72: 862-865.
-
Wass AR, Sloan JP (1996) Cortical bone cyst following a greenstick radial fracture. J Accid Emerg Med 13: 64-68.
-
Philips CD, Keats TE (1986) The development of post-traumatic cystlike lesions in bone. Skeletal Radiol 15: 631-634.
-
Malghem J, Maldague B (1986) Transient fatty cortical defects following fractures in children. Skeletal Radiol 15: 368-371.
-
Ball CM, Dawe CJ (2001) Transient posttraumatic cyst-like lesions of bone. J Pediatr Orthop 21: 9-13.