Trauma Cases and Reviews
Outcome of Bilateral Simultaneous Fracture Neck of Femur in Patients with Low Socioeconomic Status
Mahmoud A Hafez*, Fouad Z Sadek, Hosamuddin Hamza and Ahmed Mounir Al-Dars
The Orthopaedic Department, October 6 University, Cairo, Egypt
*Corresponding author: Mahmoud A Hafez, The Orthopaedic Department, October 6 University, Cairo, Egypt, Tel: (+20) 38362483, E-mail: mhafez@msn.com
Trauma Cases Rev, TCR-2-038, (Volume 2, Issue 2), Research Article; ISSN: 2469-5777
Received: April 12, 2016 | Accepted: June 24, 2016 | Published: June 27, 2016
Citation: Hafez MA, Sadek FZ, Hamza H, Al-Dars AM (2016) Outcome of Bilateral Simultaneous Fracture Neck of Femur in Patients with Low Socioeconomic Status. Trauma Cases Rev 2:038. 10.23937/2469-5777/1510038
Copyright: © 2016 Hafez MA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: Fracture neck of femur (NoF) is a rare injury but represents a serious condition in low-income countries. It results from major or minor-repetitive trauma(s) or from different pathological conditions such as parathyroid or renal dysfunction, antiepileptic medication, seizure and tumors. Similarly to other hip fractures, the diagnosis of this condition can be missed where management becomes more complicated. The present study was conducted in a country with low socioeconomic status to assess the prognosis of such injury.
Patients and methods: Six patients suffering from neglected fracture NoF were observed. They presented after failure of primary diagnosis and treatment other facilities (public sector). Five patients suffered bilateral simultaneous fracture NoF and one patient had unilateral fracture. A decision of total hip arthroplasty (THA) or not has been taken accordingly.
Results: All patients had suboptimal outcomes with mortality and morbidity.
Conclusions: Fracture NoF needs early and proper management with advanced imaging setup and well-trained health personnel to avoid high risk of complications and worse symptoms.
Keywords
Neglected fracture, Fracture neck of femur, Low socioeconomic status
Introduction
Bilateral simultaneous fracture neck of femur (NoF) is considered a rare injury. Few case reports in literature have described this injury to be a result of high-energy, major or multiple minor trauma(s), seizure or electric shock [1,2]. It is common in patients with severe osteoporosis, metabolic diseases and other pathological conditions that affect bone structure and quality. For example, renal dysfunction presents a risk factor for NoF as it causes hypocalcaemia that even delays the union of the fracture [3]. A traumatic fracture is the common type of bilateral simultaneous fracture NoF and it results from high energy trauma due to falls or accidents [4].
Malpractice, misdiagnosis and mismanagement of hip fractures have very deleterious effects on individuals' health, leading to continuous symptoms and further displacement, and making the patient prone to limb shortening and abnormal walking as a result of delayed union or nonunion [3]. In some cases, osteonecrosis of the femoral head following fracture NoF may occur due to the increased interosseous pressure in the femoral head which ends up with bone death [4].
In low-income countries, bilateral simultaneous fracture NoF turns up to a life-threatening condition causing lifelong disability and affecting individuals' workability with intolerable financial and social consequences. The limited availability of diagnostic measures, the high risk of infection and the low follow-up rates present challenges for orthopedic surgeons to properly assess their treatment plans and to determine the long-term outcome [5]. Also, due to the high incidence of fractures compared to hospitals' capacities, patients with fractures admit firstly the emergency units where diagnostic measures are usually limited to plain radiographs which comprise difficult utility to identify hip fractures, especially bilateral fracture NoF. Inexperienced junior doctors and young residents may be unable to provide complete clinical examination and thorough speculation of bilateral hip fractures which also leads to diagnostic errors at emergency units [6]. Nevertheless, many patients refuse to do surgeries due to their limited income, the lack of comprehensive medical insurance, the limited knowledge about the nature of orthopedic surgeries as well as fear from surgery and potential complications [7].
Prior to any intervention with patients with bilateral simultaneous NoF, proper assessment of underlying bone or metabolic diseases should be done. NoF fracture is initially managed with CRIF or fixation. Advanced cases can be treated with bone grafting and osteotomy, while more severe cases may need hip arthroplasty (either hemi- or total arthroplasty), especially for old-age individuals and for patients with arthritis or other comorbidities (e.g. rheumatoid arthritis or Paget's disease) [8]. Postoperatively, bone healing and union must be observed for long follow-up period, and conservative means of treatment can be considered in some cases (e.g. oral supplements of calcium for patients with multiple comorbidities) [9].
The aim of this study is to evaluate the prognosis (morbidity and mortality) of patients who had delayed or missed diagnosis and failure of primary treatment of bilateral simultaneous fracture NoF (neglected fractures) in countries with low socio-economic status.
Patients and Methods
Six patients presented to our academic orthopedic department (The Orthopedic Department, October 6 University, Cairo, Egypt) between 2011 and 2014, with neglected fracture NoF. Ethical approval was obtained for management of patients and to record their details. Five out of six patients had bilateral simultaneous fractures, while only patient (number 4) had unilateral fracture. All patients presented late at our unit after achieving primary treatment at other health-care facilities. Patient records were anonymized and de-identified prior to analysis. Demographic data and characteristic information of the patients are shown in table1. All patients had traumatic fractures due to accidents or falls except patient #4 who had pathological fracture.
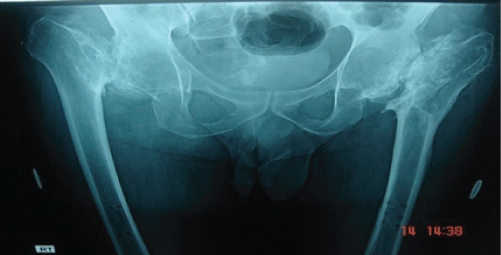
.
Figure 1: X-ray demonstrates neglected bilateral simultaneous fracture NoF with superior migration of proximal femur.
View Figure 1
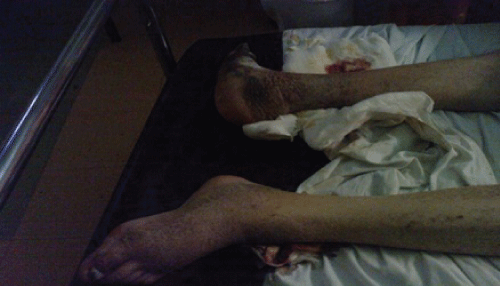
.
Figure 2: X-ray demonstrates neglected bilateral simultaneous fracture NoF with superior migration of proximal femur.
View Figure 2
Primary management
On primary treatment, two patients had received treatment of hip fracture of one side while the other side was overlooked. Two patients got medical advice for the necessity of surgical intervention but they refused surgery due to their low socioeconomic status. One patient had fixation by dynamic hip screw two months after the initial trauma; this delay led to failure of this primary treatment because the patient was young and needed osteotomy rather than hip replacement. One patient had pathological bilateral fracture with unknown primary source of tumor; the cause of delay is insignificant trauma.
![]()
Table 1: Demography and characteristics for the patients with bilateral fracture NoF.
View Table 1
Secondary management
At our service, the patients were advised to perform total hip arthroplasty (THA) to relief pain and improve the limb function. Four patients refused any surgical intervention due to bad history with surgery or due to financial concerns. Two patients accepted THA (numbers 3 and 6); preoperative planning using digital hip templating was done as the cases were complex due to leg length discrepancy, malunion and distorted anatomy of the hip joint.
Patients' assessment included comprehensive history taking, proper examination, inspection for external rotation deformity or leg length discrepancy as well as routine plain X-rays including AP (Figure 3) and lateral views of the hips; CT scanning was required for some cases to diagnose occult or missing fractures.
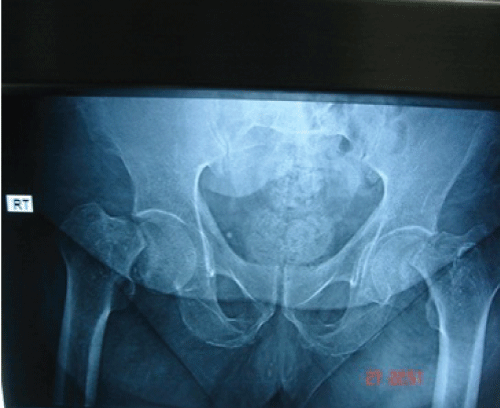
.
Figure 3: X-ray demonstrates neglected bilateral simultaneous fracture NoF with superior migration of proximal femur.
View Figure 3
Results
All cases had suboptimal outcome: five patients had poor outcome and only one patient showed some improvement (Table 2).
![]()
Table 2: Intervention and outcome for the patients with a bilateral fracture NoF.
View Table 2
Discussion
Neglected fracture NoF has been increasingly reported in low-income communities [10]. The outmost result of treating fracture NoF is to achieve stable fixation and to return the limb to normal physical activities within reasonable duration [11].
In this work, the authors report a number of cases that were misdiagnosed and improperly managed on the first onset of the trauma which led to neglected fractures that needed further intervention. Four patients refused making surgery due to bad history with surgeries or because of their associated comorbidities. The patients were of low socioeconomic status and they lacked comprehensive medical insurance while the surgery was relatively costly for them. Also, the patients and their families were hopeless in any improvement in their disability.
After primary treatment, patient number 1 had poor function after surgical fusion of both hips by girdle stone surgery. He had inability to sit down in addition to leg length discrepancy and inability to move his hips for proper walking, hygiene or sex. He had several operations previously so he refused THA as a secondary treatment at our service.
Patient number 2, on primary treatment, had bilateral hemi-arthroplasty which has failed and the patient became bed ridden for 1.5 years. He refused further surgical intervention at our service as a secondary treatment. Finally, severe bed sore developed and he died 3 months postoperatively.
On primary treatment, patient number 3 was investigated and found to have bilateral traumatic fracture NoF. However, the diagnosis was delayed and leg length discrepancy was a sequel of delayed management. At our service, the patient underwent revision THA and the outcome was relatively better but the patient still had mild pain and used to walk with a stick.
Patient number 4 had pathological unilateral fracture NoF. She admitted to our service and was found to have painful hip, inability to walk and leg length discrepancy. Our diagnosis revealed that the patient had fracture of lesser trochanter and deposits in the right proximal femur which was painful with inability to weight-bearing. This was an impending fracture NoF that required prophylactic fixation. The patient refused the surgery and was referred to an oncologist (Figure 4).
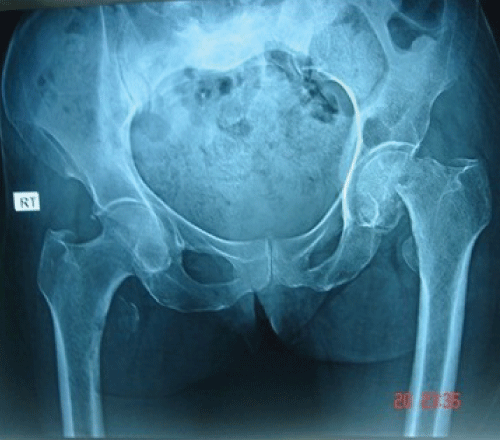
.
Figure 4: X-ray demonstrates neglected bilateral simultaneous fracture NoF with superior migration of proximal femur.
View Figure 4
Patient number 5 presented late with several complications following the primary treatment. Dynamic hip screw for left NoF and hemiarthroplasty for right NoF were done on primary treatment (Figure 5), but he showed inferior results after surgery. His family refused any further surgical intervention due to the bad history.
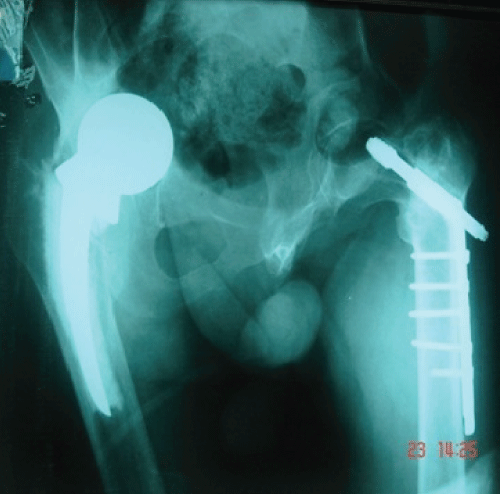
.
Figure 5: Plain X-ray demonstrates failure of dynamic hip screw for left NoF and hemi-arthroplasty for right side.
View Figure 5
For patient number 6, on primary treatment, cannulated screws in both hips and osteotomy with blade plate after nonunion were done. Then, at our service, a decision was taken to do left THA due to her OA and leg length deformity (3 cm shortening resulted from previous osteotomies). Later on, the patient had bad prognosis, she was unable to bear weight for 2 years following THA. In other words, the final result was failed THA.
Socioeconomic status was found to influence the incidence of hip fractures. The socioeconomic factors are not only limited to the financial income but also include education, lifestyle and comorbidities. There are other factors which influence the decision of making THA such as the concern of postoperative pain, expectation of surgical procedure and patients' concerns about inability to continue their work [10]. These concerns may delay the patients to consult the orthopedic surgeon causing their fractures to become neglected ones which require special intervention such as in situ-fixation, ORIF, open fixation with valgus intertrochanteric osteotomy or bilateral simultaneous or staged THA [8].
There are several cases reported in literature on neglected femoral neck fractures. None of literature has presented a group of patients with neglected fractures but only individual cases. The focus of this study was on bilateral simultaneous fracture NoF in light of patients' socioeconomic status.
When dealing with fracture NoF, management options and prognosis vary according to the onset of diagnosis (e.g. hemi-arthroplasty following immediate diagnosis or primary internal fixation after delayed diagnosis) [12]. Another key factor for choosing the appropriate management option is the patient's medical profile. For example, patients on dialysis can be managed by bilateral hemi-arthroplasty while others with narcotic drug abuse can be managed by bilateral single-stage hemi-arthroplasty [8]. However, the appropriate treatment should also depend on the viability of the femoral head, size of the remnant femoral neck, extent of osteoporosis, duration of the disease and state of the joint space [13].
There is a variety of treatment options for neglected fracture NoF including arthroplasty and osteosynthesis (valgus osteotomy, fibular grafting with internal fixation, vascularized bone grafting, muscle pedicle bone grafting and McMurray displacement osteotomy) [14]. Nonetheless, there is no guidelines for choosing one treatment option over another for a particular fracture [15]. Malpractice with fracture NoF (e.g. incorrect internal fixation) may lead to shortening of the femoral head and affect gait parameters [16].
THA was the treatment option selected for all patients included in this series for best possible outcome. However, for 2 patients underwent the surgery, the outcome was still suboptimal. The main outcome was measured by morbidity and mortality, which are easy to evaluate.
The limitation of this study is that each case presented with complex diagnostic and treatment decisions and it is difficult to present such a mixed group of patients and reach a conclusion that applies to the overall group. However, these patients still have common features: mainly, the nature of injury (neglected fracture, mostly bilateral simultaneous), the delayed presentation, the refusal of treatment and the low socioeconomic status. Another common feature of these patients is the type of deformity, that is, leg length discrepancy.
In our country, diagnostic tests are relatively available but there could be some financial limitations.
The overall conclusion of this work is that malpractice and neglecting NoF fractures would likely lead to further displacement and permanence of symptoms. Fracture NoF (especially bilateral simultaneous) requires high inspection facilities such as MRI or CT scans which are of limited availability in public hospitals at low-income countries, especially local district hospitals where most of fracture patients are transferred to at the time of trauma incidence.
Conclusion
The outcome of treatment of fracture NoF is variable and is usually encountered with severe complications such as nonunion and a vascular necrosis [17]. The management is more difficult when the fracture is misdiagnosed at its first onset and when improper primary treatment is delivered. The condition is fatal by itself and when it results from metastasis in the pelvic region. Early intervention is a key of success for treating such kind of injury.
Disclosure
The authors have nothing to disclose.
Conflict of Interests
The authors declare there is no conflict of interests.
Authors' Contribution
The authors have equally contributed to the writing and study design of this work.
References
-
Schroder J, Marti RK (2001) Simultaneous bilateral femoral neck fractures: case report. Swiss Surg 7: 222-224.
-
Annan IH, Buxton RA (1986) Bilateral stress fractures of the femoral neck associated with abnormal anatomy: a case report. Injury 17: 164-166.
-
Chadha M, Balain B, Maini L, Dhal A (2001) Spontaneous bilateral displaced femoral neck fractures in nutritional osteomalacia-a case report. Acta Orthop Scand 72: 94-96.
-
Grimaldi M, Vouaillat H, Tonetti J, Merloz P (2009) Simultaneous bilateral femoral neck fractures secondary to epileptic seizures: treatment by bilateral total hip arthroplasty. Orthop Traumatol Surg Res 95: 555-557.
-
Young S (2014) Orthopaedic trauma surgery in low-income countries. Acta Orthop Suppl 85 :1-35.
-
Guly HR (2001) Diagnostic errors in an accident and emergency department. Emerg Med J 18: 263-269.
-
Abdulrasheed Ibrahim, Ekundayo Stephen Garba, Malachy Eneye Asuku (2012) Challenges in disclosure of adverse events and errors in surgery; perspectives from sub-Saharan Africa. Pan Afr Med J 12: 82.
-
Alireza Hootkani, Ali Moradi, Ehsan Vahedi (2010) Neglected simultaneous bilateral femoral neck fractures secondary to narcotic drug abuse treated by bilateral one-staged hemiarthroplasty: a case report. J Orthop Surg Res 5:41.
-
S. Terry Canale, James H. Beaty (2008) Campbell's Operative Orthopaedics (11th edn).
-
Roshan A, Ram S (2008) The neglected femoral neck fracture in young adults: review of a challenging problem. Clin Med Res 6: 33-39.
-
Hou SM, Hang YS, Liu TK (1993) Ununited femoral neck fractures by open reduction and vascularized iliac bone graft. Clin Orthop Relat Res 294: 176-180.
-
Kalender AM, Dogan A, Cakar A, Turkoz T (2010) Neglected bilateral femoral neck fracture associated with pregnancy and primary hyperparathyroidism. Acta Orthop Belg 76: 559-563.
-
Hung KH, Lee CT, Gau YL, Chen JB (2001) Neglected bilateral femoral neck fractures in a patient with end-stage renal disease before chronic dialysis. Ren Fail 23: 827-831.
-
Hofmann A, Wyatt R (1984) Missed Subcapital Fractures. Ann Emerg Med 13: 951-955.
-
Parker MJ (1992) Missed hip fractures. Arch Emerg Med 9: 23-27.
-
Zielinski SM, Keijsers NL, Praet SF, Heetveld MJ, Bhandari M, et al. (2013) Femoral Neck Shortening after Internal Fixation of a Femoral Neck Fracture. Orthopedics 36: e849-e858.
-
Ernst LFB Raaymakers, René K Marti (2008) Nonunion of the femoral neck: Possibilities and limitations of the various treatment modalities. Indian J Orthop 42: 13-21.





