Trauma Cases and Reviews
Acute Compartment Syndrome Following Anterior Cruciate Ligament Reconstruction with Autologous Hamstring Graft
Benjamin Wheatley1* and Matthew Oetgen2
1Department of Orthopedic Surgery, Walter Reed Military Medical Center, USA
2Department of Orthopedic Surgery, Children’s National Medical Center, USA
*Corresponding author:
Benjamin M Wheatley, MD, Department of Orthopedic Surgery, Walter Reed Military Medical Center, USA, E-mail: ben.m.wheatley@gmail.com
Trauma Cases Rev, TCR-2-035, (Volume 2, Issue 1), Case Report; ISSN: 2469-5777
Received: February 03, 2016 | Accepted: March 21, 2016 | Published: April 01, 2016
Citation: Wheatley B, Oetgen M (2016) Acute Compartment Syndrome Following Anterior Cruciate Ligament Reconstruction with Autologous Hamstring Graft. Trauma Cases Rev 2:035. 10.23937/2469-5777/1510035
Copyright: © 2016 Wheatley B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Compartment syndrome is an extremely rare complication described in association with anterior cruciate ligament (ACL) reconstruction. Previous reports have described this complication as a result of extravasation of fluid into dependent compartments. One proposed mechanism is from a capsular defect that allows irrigation fluid to flow from the joint into lower leg muscular compartments. However, no reports could be found linking the development of compartment syndrome to bleeding from the graft harvest site. To our knowledge, this is the first report of compartment syndrome following ACL reconstruction with utilization of hamstring autograft.
Keywords
Compartment syndrome, ACL reconstruction, Complication
Introduction
Compartment syndrome is an extremely rare complication described in association with anterior cruciate ligament (ACL) reconstruction [1]. Previous reports have described this complication as a result of extravasation of fluid into dependent compartments [2-7]. There has also been report of compartment syndrome following ACL reconstruction due to anterior tibial artery injury during tibial tunnel placement [8]. One proposed mechanism is from a capsular defect that allows irrigation fluid to flow from the joint into lower leg muscular compartments. However, no reports could be found linking the development of compartment syndrome to bleeding from the graft harvest site. To our knowledge, this is the first report of compartment syndrome following ACL reconstruction with utilization of hamstring autograft.
Case Report
The patient is a 16 year old male, who suffered a right (ACL) injury while playing football in September, 2013. He was seen and evaluated at an outside facility and an MRI of the right knee showed disruption of the posterior bundle of the ACL with partial disruption of the anterior bundle. He is an otherwise healthy, athletic individual with no significant past medical history. His family history is non-contributory and of note there is no history of bleeding diathesis.
On December 23rd, a femoral nerve block was placed with ropivicaine and he was then taken to the operating room. Diagnostic arthroscopy confirmed disruption of the ACL with a positive intraoperative Lachman test. The ACL was debrided and a standard notchplasty was performed. The scope was then removed and an extremity tourniquet was inflated. The semitendinosus and gracilis tendons were harvested and prepared. The graft was inserted without difficulty and placed with the use of a femoral button and tibial interference screw. The tourniquet remained inflated for the duration and was deflated immediately prior to the end of the case after a total of 64 minutes. The patient was then transferred to the PACU and was discharged home in good condition on the same day.
He reports that approximately 8 hours after the conclusion of the case he began to experience increasing pain in his right calf. On post-operative day 1 his pain continued to increase and he began to notice swelling of the right calf. On post-operative day 2 the swelling continued to increase and the pain became unbearable around 1800 at which time he was taken to a local Emergency Room for further evaluation. An ultrasound of the right leg was performed which was unable to adequately visualize the popliteal or distal veins. There was concern for compartment syndrome and he was transferred to our institution for further evaluation.
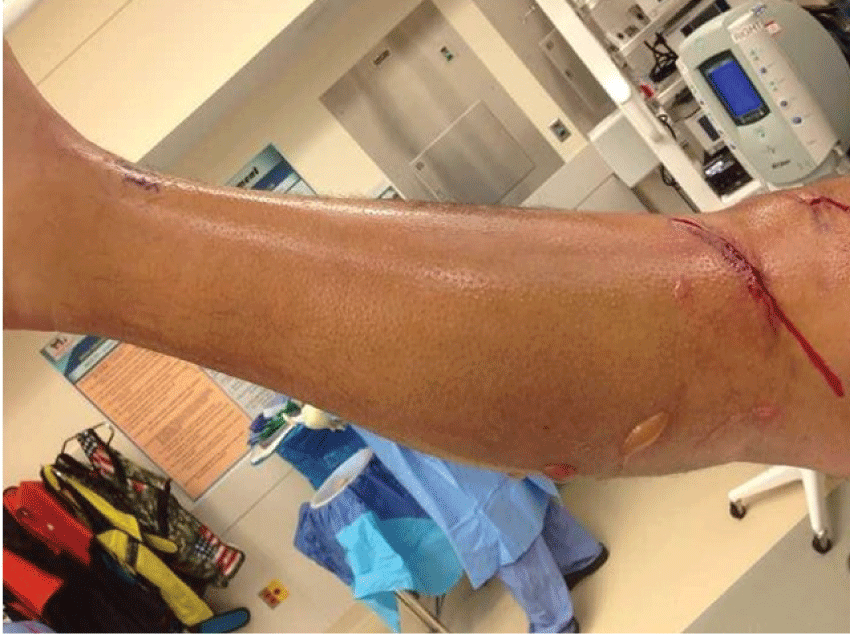
The patient arrived to the hospital at approximately 2306 on December 25th. He was seen and evaluated by the emergency room staff and orthopedics on-call. Exam revealed a large, athletic male in apparent distress with significant pain. His right calf was noticeably larger than the left and the skin appeared tight and shiny with 3-4 blisters on the posterior aspect of the lower leg (Figure 1). All four compartments were tense and non-compressible. The patient was unable to perform active motion at the knee, ankle or toes secondary to pain. Passive range of motion at the ankle and great toe elicited severe pain in the calf. Sensation was decreased in the leg to the level of the mid-calf. Dorsalis pedis pulse was diminished but palpable and the posterior tibial pulse was dopplerable at the ankle. Intra-compartmental pressure was taken in the anterior compartment with Stryker compartment pressure monitor which measured 65 mmHg, the patient’s diastolic blood pressure at the time of measurement was 52 mmHg.
.
Figure 1: Demonstrates blistering of the skin in the proximal medial and posterior aspects of the leg prior to surgery.
View Figure 1
The patient was taken to the operating room at 0025 on December 26th for a four compartment fasciotomy. A lateral incision was made first with release of the anterior and lateral compartments. Muscle bellies were protruding but appeared pink and were contractile. A medial incision was then made and the superficial and deep posterior compartments were released. The muscle had a dusky appearance but was contractile and no debridement was performed. A significant amount of hematoma was noted tracking from the hamstring graft harvest site to the superficial compartment. The skin was left open and wound vacs were applied to the medial and lateral incisions. The patient was then transferred to the inpatient ward.
Later that night, the patient reported the pain in his right leg had improved. Over the course of the next day, his pain continued to improve and repeat ultrasound of the right lower extremity was performed which showed no evidence of occlusive clot and normal compression of all vessels with satisfactory waveforms. He was taken back to the operating room on December 28th for irrigation and debridement, wound vac exchange and partial closure. On December 30th, he underwent delayed primary closure of the medial and lateral incisions. He was discharged on January 2nd in good condition and his pain was well controlled.
On January 5th, the patient was readmitted to our service due to acute pain exacerbation. An ultrasound of the lower extremity was performed which showed a large heterogeneous collection in the medial calf consistent with a complex hematoma and no evidence of deep venous thrombosis. The pain service was consulted for management of neuropathic pain and the patient was started on gabapentin. On January 6th, there was persistent draining of dark blood from the hamstring graft harvest site. The Hematology service was consulted to rule out possible bleeding diathesis. A von Willebrand’s panel, factor VIII level, platelet function assay and thromboelastography study were obtained. The factor VIII level was 206%, vWF 45%, collagen/epinephrine was within normal limits at 190 sec and ADP was elevated at 141 sec. Coagulation review showed there is no coagulation factor deficiency, abnormal clot formation or abnormal lysis by thromboelastography. On January 9th, the patient returned to the operating room for irrigation and debridement of the hamstring graft harvest site due to continued drainage from the surgical site. Cultures obtained showed no evidence of infection and the drainage subsequently subsided.
The patient was subsequently discharged. At final follow-up, the patient was doing well. The surgical sites had healed without complication. His sensation had returned to normal and he suffered no motor deficits.
Discussion
Compartment syndrome is described as the increase in pressure within a confined space secondary to any cause. The resultant increase in pressure can reduce the perfusion pressure gradient thereby reducing oxygen delivery to local tissues. The pressure can also compress veins decreasing venous drainage further reducing perfusion pressure and leading to direct compression on nerves [9-11]. Reduced oxygen delivery can cause ischemic necrosis of muscle and nerve tissue resulting in irreversible injury within 6-10 hours of onset. Compartment syndrome is most commonly related to fractures with tibial diaphyseal, distal radius and forearm being the most common underlying cause [11]. Compartment pressures 20-30 mmHg below the diastolic pressure have been shown to be the critical tissue pressure threshold. Compartment syndrome is primarily a clinical diagnosis with the cardinal signs of pain with passive motion and paresthesias. Intra-compartmental pressure monitors have allowed for objective findings to aid in the diagnosis.
Arthroscopy is an extremely common tool within orthopedics with a wide variety of surgeries being performed with minimally invasive techniques. The majority of complications in arthroscopic ACL reconstruction stem from technical errors including tunnel placement, graft fixation and damage to surrounding structures [12,13]. Previous studies have reported an approximately 5-10% complication rate with less than 1% having therapeutic consequences [14,15]. The formation of DVT has been reported as a common complication in up to 10% of patients when routine screening is performed, however, the majority of these are distal and clinically insignificant [16]. The use of an infusion pump during arthroscopy has also been cited as a source of complications in which fluid has extravasated out of the knee during surgery and has rarely been associated with the development of compartment syndrome [17]. Studies have been performed with intra-compartmental pressure monitoring during and after arthroscopic knee surgery with mixed results where some report demonstrate increases in pressure post-operatively while others report no significant difference [18,19]. While complications do exist in association with arthroscopic ACL reconstruction, acute compartment syndrome has only rarely been described and is most commonly attributed to the extravasation of irrigation fluid.
Previous reports of compartment syndrome have been described in association with peripheral nerve blocks [20,21]. Therapeutic and prophylactic anticoagulation has been associated with increased risk of bleeding and compartment syndrome following the placement of a nerve block [20]. Peripheral nerve blocks have been more commonly described in delaying the diagnosis of compartment syndrome that developed as a result of other causes [22].
Another potential cause of acute compartment syndrome in arthroscopic ACL reconstruction lies in the use of a tourniquet. Serious complications as a result of the use of a tourniquet are rare and are seldom found when used correctly and for a short duration [22-24]. Complications have been described with prolonged use and care must be taken to ensure the tourniquet is not left inflated for extended periods of time with allowing for rest [13].
Compartment syndrome following ACL reconstruction has previously been reported due to anterior tibial artery injury due to tibial tunnel placement [8]. The intraoperative finding of clot originating at the graft harvest site and extending into the superficial posterior compartment led us to believe that this case of compartment syndrome may have resulted from bleeding at the harvest site. According to the operative report, the tourniquet was released immediately prior to the conclusion of the case. It is possible that adequate hemostasis was not obtained prior to closure and bleeding into the posterior compartment resulted in compression of the local vasculature. Hemostasis is an essential component of any surgery and can be complicated in hamstring harvest for ACL reconstruction due to poor direct visualization of the harvest site. This could have potentially been avoided by ensuring there was adequate control of bleeding after the tourniquet was released, prior to the conclusion of the case.
References
-
Mayr HO, Stoehr A (2016) Complications of knee arthroscopy. Orthopade 45: 4-12.
-
Marti CB, Jakob RP (1999) Accumulation of irrigation fluid in the calf as a complication during high tibial osteotomy combined with simultaneous arthroscopic anterior cruciate ligament reconstruction. Arthroscopy 15: 864-866.
-
Siegel MG (1997) Compartment syndrome after arthroscopic surgery of the knee. A report of two cases managed nonoperatively. Am J Sports Med 25: 589-590.
-
Fruensgaard S, Holm A (1988) Compartment syndrome complicating arthroscopic surgery: brief report. J Bone Joint Surg Br 70: 146-147.
-
Nillius A, Rööser B (1983) Acute compartment syndrome in knee arthroscopy. Lakartidningen 80: 590.
-
Peek RD, Haynes DW (1984) Compartment syndrome as a complication of arthroscopy. A case report and a study of interstitial pressures. Am J Sports Med 12: 464-468.
-
Keskinbora M, Yalcin S, Oltulu I, Erdil ME, Ormeci T (2016) Compartment syndrome following arthroscopic removal of a bullet in the knee joint after a low-velocity gunshot injury. Clin Orthop Surg 8: 115-118.
-
Kim SB, Lim JW, Seo JG, Ha JK (2016) Injury to the Anterior Tibial Artery during Bicortical Tibial Drilling in Anterior Cruciate Ligament Reconstruction. Clin Orthop Surg 8: 110-114.
-
von Keudell AG, Weaver MJ, Appleton PT, Bae DS, Dyer GS, et al. (2015) Diagnosis and treatment of acute extremity compartment syndrome. Lancet 386: 1299-1310.
-
Weinmann M (2003) Compartment syndrome. Emerg Med Serv 32: 36.
-
McQueen Margaret M (2009) Acute Compartment Syndrome. In: Rockwood, Charles A. Lippincott, Rockwood and Green’s Fractures in Adults (7th edition) 689-705.
-
Safran MR, Greene HS (2006) Avoidance and management of intra-articular complications of anterior cruciate ligament reconstruction. Instr Course Lect 55: 475-488.
-
Heard WM, Chahal J, Bach BR Jr (2013) Recognizing and managing complications in ACL reconstruction. Sports Med Arthrosc 21: 106-112.
-
Crawford DC, Hallvik SE, Petering RC, Quilici SM, Black LO, et al. (2013) Post-operative complications following primary ACL reconstruction using allogenic and autogenic soft tissue grafts: increased relative morbidity risk is associated with increased graft diameter. Knee 20: 520-525.
-
Reigstad O, Grimsgaard C (2006) Complications in knee arthroscopy. Knee Surg Sports Traumatol Arthrosc 14: 473-477.
-
Ilahi OA, Reddy J, Ahmad I (2005) Deep venous thrombosis after knee arthroscopy: a meta-analysis. Arthroscopy 21: 727-730.
-
Bomberg BC, Hurley PE, Clark CA, McLaughlin CS (1992) Complications associated with the use of an infusion pump during knee arthroscopy. Arthroscopy 8: 224-228.
-
Amendola A, Faber K, Willits K, Miniaci A, Labib S, et al. (1999) Compartment pressure monitoring during anterior cruciate ligament reconstruction. Arthroscopy 15: 607-612.
-
Jerosch J, Castro WH, Geske B (1991) Intracompartmental pressure in the lower extremity after arthroscopic surgery. Acta Orthop Belg 57: 97-101.
-
Parziale JR, Marino AR, Herndon JH (1988) Diagnostic peripheral nerve block resulting in compartment syndrome. Case report. Am J Phys Med Rehabil 67: 82-84.
-
Egert R (1988) Diagnostic peripheral nerve block resulting in compartment syndrome. Am J Phys Med Rehabil 67: 230.
-
Sorrentino F, Eggli S, Stricker U, Ballmer FT, Hertel R (1998) Missed compartment syndrome after anterior cruciate ligament-plasty following continuous peridural anesthesia. Unfallchirurgm 101: 491-494.
-
Luk KD, Pun WK (1987) Unrecognised compartment syndrome in a patient with tourniquet palsy. J Bone Joint Surg Br 69: 97-99.
-
Palmer AK (1986) Complications from tourniquet use. Hand Clin 2: 301-305.





