Trauma Cases and Reviews
Investigation of Intraventricular Hemorrhage Volume in Motor Vehicle Crash Occupants
Jillian E Urban1,2*, Christopher T Whitlow2,3,4 and Joel D Stitzel1,2
1Center for Injury Biomechanics, Virginia Tech-Wake Forest University, USA
2School of Medicine, Wake Forest University, USA
3Department of Radiology (Neuroradiology), Wake Forest University, USA
4Translational Science Institute, Wake Forest University, USA
*Corresponding author: Jillian E Urban, Ph.D, Medical Center Blvd, Winston-Salem, NC 27157, USA, Tel: (336) 716-0947, Fax: (336)-716-5491, E-mail: jurban@wakehealth.edu
Trauma Cases Rev, TCR-1-021, (Volume 1, Issue 4), Original Article; ISSN: 2469-5777
Received: October 01, 2015 | Accepted: December 15, 2015 | Published: December 17, 2015
Citation: Urban JE, Whitlow CT, Stitzel JD (2015) Investigation of Intraventricular Hemorrhage Volume in Motor Vehicle Crash Occupants. Trauma Cases Rev 1:021. 10.23937/2469-5777/1510021
Copyright: © 2015 Urban JE, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Motor vehicle crashes (MVCs) are a leading cause of traumatic intracranial injuries which often have devastating impacts on morbidity and mortality. Intraventricular hemorrhage (IVH) is one type of head injury that is identified on post-traumatic computed tomography (CT) scans. IVH is observed less frequently in patients with head trauma, however it is often associated with severe head trauma and negative prognostic outcomes and causation of traumatic IVH is not well-understood. The severities of injuries are often quantified by geometric and volumetric measurements. Studying the relationship between these measurements and MVC severity and occupant data may reveal important determinants of occupant head injury. The objective of this study was to quantify the volume of IVH of 30 occupants from the Crash Injury Research and Engineering Network (CIREN) database and evaluate how volumetric measurements of IVH relate to crash characteristics and occupant parameters. Significant relationships were observed between IVH volume, total head injury severity, occupant size (height, weight, and BMI), and ΔV/BES. Larger volumes of IVH were observed in occupants with SAH and/or DAI, both of which were found to a commonly associated injury. The work presented in this study provides a brief case series demonstrating the associations between IVH volume, crash characteristics, and occupant parameters. This work may lead to improved methods to predict and prevent IVH and highlight the utility of combining clinical neuroimaging with occupant demographics and mechanical crash data for investigating mechanisms of TBI.
Keywords
Intraventricular hemorrhage, Motor vehicle crash, Computed tomography, Head injury
Introduction
Motor vehicle crashes are the leading cause of traumatic brain injury (TBI) related hospitalization and death [1]. Of the 1.7 million people who sustain a TBI per year, only 3% of these injuries result in death. Although the number of people who die from head injury appears to be relatively small, the cognitive effects from TBI can cause devastating impacts on quality of life and those who sustain a TBI may result in premature mortality [2-4]. Intraventricular hemorrhage (IVH) is one type of head injury that is identified on post-traumatic computed tomography (CT) scans. It is thought to be the result of a shearing injury of the subependymal veins along the walls of the ventricles, extension of adjacent intraparenchymal hemorrhage, or intraventricular extension of SAH [5]. Patients with IVH often have visible radiologic signs of intraparenchymal injuries, as well as extra-axial masses [6]. Although IVH is less common, resulting in nearly 0.4 to 4% of patients with head trauma, it is often indicative of severe head trauma and is associated with negative prognostic outcomes [7-9]. There is currently a paucity of existing literature on the causation of traumatic IVH.
Clinical case reports of patients often rely on patient and/or observer information to determine the causation of the injury [10]. The Crash Injury Research and Engineering Network (CIREN) database contains detailed vehicle, crash, and medical data on injured MVC occupants [11] and has proven to be a valuable resource for documenting and understanding the mechanisms of injuries. It contains pre-crash information, along with data from detailed scene and vehicle investigation, as well as medical images, injury causation scenario (ICS), and patient outcome data. Patient injuries are coded using the Abbreviated Injury Scale (AIS) and International Classification of Diseases (ICD)-9 [12-14]. The CIREN database is unique in that it contains medical images documenting the intracranial injury, as well as vehicle evidence and full case review linking the mechanical insult to the injury. This has ultimately created a research paradigm in which researchers are able to relate information about the crash to the kinematics and loading of the occupant and resulting injury.
There are two AIS (version 2005) codes for IVH severity which are each classified by the presence and length of coma (AIS post dot code 2: not associated with coma > 6 hours and AIS post dot code 4: associated with coma > 6 hours) [13]. While coma may be indicative of IVH severity, the volume of hemorrhage has been previously shown to be the most significant prognostic sign of brain injury [15]. It is not well-understood, however, how IVH volume relates to crash parameters or occupant characteristics associated with the injury; each of which may reveal important determinants of occupant head injury and IVH severity. Previous studies have utilized the CIREN database to understand relationships between volumetric measurements of injury and crash and occupant parameters [16-18]. However, this research has been primarily focused on MVC-related pulmonary contusion [16], and only one study to date focused on volumetric analysis of MVC-related SDH [19]. This study aims to better understand these relationships and inform injury mechanisms by correlating the volume of IVH to total head injury severity, crash characteristics, and occupant parameters. This information is useful for the engineering design of countermeasures to mitigate or prevent such injuries in the future, and may help guide clinical management of a patient for which crash characteristics are known.
Methods
Scan collection
Axial non-contrast head CT data and associated radiology reports obtained within the first 24 hours post-crash were collected for cases with CT data within the CIREN database demonstrating intracranial injury based on 1998 [12] and 2005 [13] AIS coding. Soft tissue algorithm CT data were selected for this study to optimize visualization of intracranial blood products [20]. Scans were excluded if they compromised the visualization and/or volume calculation of the injury (i.e., motion artifact or poor scan resolution).
Detailed data regarding the occupant, injury, vehicle, and crash were also collected. These data included: age, gender, height, weight, seating position, and the involved physical component (IPC) in the vehicle attributed to the head injury. Vehicle data included: vehicle year, make, model, manual belt use, collision deformation classification (CDC) code, and maximum crush of the vehicle (Cmax). Crash type, change in velocity (ΔV), and barrier estimate speed (BES) were also collected for the highest severity impact. Rollover cases were excluded from the analysis due to complicated impact scenarios. Data were collected using the CIREN SQL interface and SQL developer (Oracle, Redwood Shores, CA). All cases selected underwent a full case review with medical, engineering, and crash reconstruction specialists to determine injury causation. Quality control checks have been undertaken, and the cases are designated as "complete" in the database.
Segmentation
Head CT scans were segmented using manual and semi-automated techniques within Mimics version 14 and version 16 (Materialise, Leuven, Belgium) (Figure 1). IVH was identified from descriptions within the radiology report and was individually segmented at the appropriate window level to identify the hemorrhage within the ventricular space. Injury segmentations were reviewed by three board certified radiologists, two Neuroradiology Fellows and one Neuroradiology Attending, to ensure proper volume identification of the hemorrhage. Because the focus was on the IVH volume, additional intracranial injuries were not isolated in this analysis.
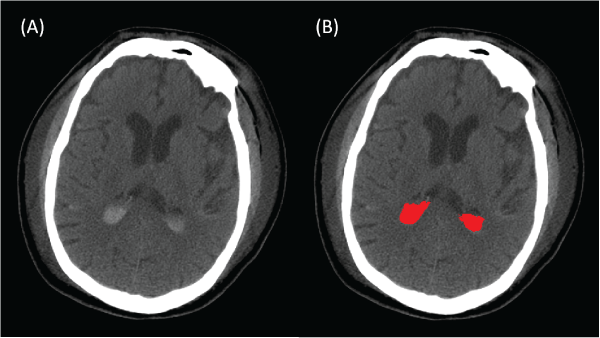
.
Figure 1: Image segmentation example. (A) Axial CT image of occupant with IVH; (B) Image segmentation of IVH shown in red.
View Figure 1
Statistical analysis
IVH volume was evaluated by total head injury severity, occupant parameters, and crash characteristics. Total head injury severity was computed by combining the post-dot AIS code (version 2005) of all head injuries (skeletal, intraparenchymal, extra-axial) to compute the summed head injury AIS score. Linear regression was performed to calculate regression coefficients and associated p-values with respect to the slope of the regression line between injury characteristics, head injury severity, occupant parameters, and crash characteristics. Independent variables included total head injury severity, age, height, weight, body mass index (BMI), Cmax, and ΔV/BES. BES was used only if ΔV was not available from the crash reconstruction. The volume (mm3) of IVH was logarithmically transformed to satisfy the assumptions of normality. The Mahalanobis distance was computed to remove outliers from the linear regression analysis. The level of statistical significance was 0.05.
Results
There were 187 cases identified from occupants in the CIREN database with designated head injury that had adequate soft tissue CT data collected within 24 hours post-crash demonstrating the injury. Out of the total data set, there were 38 cases identified with evidence of IVH. Eight cases were excluded to further narrow the scope to frontal and side collisions. Fifty percent of the remaining cases were occupants involved in frontal collisions, with the remaining 30% involved in near-side collisions and 20% in far-side collisions. A summary of the crash, occupant, and injury data is provided in table 1. IVH volume was segmented for each occupant. The distributions of volumes were right skewed with the median volume of 0.36 cm3 and a 95th percentile volume of 21.23 cm3. There was no significant difference in IVH volume by crash type.
![]()
Table 1: Summary of the crash, occupant, and injury data collected for the 30 IVH occupants. Data for age, ΔV/BES, and Cmax presented as mean (standard deviation). Data for IVH volume presented as median (95th percentile). B/NB = Belted/Non-Belted; IVH = Intraventricular hemorrhage.
View Table 1
Intracranial injuries associated with MVCs often present as a mixture of intra-axial and extra-axial injuries. Intra-axial injuries, those occurring within the brain parenchyma, include diffuse axonal injury (DAI), cerebral contusion, and intraparenchymal hemorrhage (IPH). Extra-axial injuries, those occurring outside the brain parenchyma, include epidural hemorrhage (EDH), subdural hemorrhage (SDH) and subarachnoid hemorrhage (SAH). Although each is classified as intracranial hemorrhage, the head experiences a number of different forces during an MVC, and the mechanisms of injury resulting in these different patterns of hemorrhage vary. Twenty-eight (93%) of the occupants had other head injuries coded in addition to IVH, many of which were combinations of intraparenchymal and extra-axial injuries. SAH was identified in 56.7% (n = 17) of the occupants, DAI was identified in 33.3% (n = 10) of the occupants, and 23.3% (n = 7) had both SAH and DAI. Seven out of the 10 occupants with IVH and DAI were in frontal collisions. Of the occupants with SAH and IVH, there was a nearly even distribution between all crash types (Frontal, n = 6; Near-Side, n = 5; Far-Side, n = 4) and an even distribution was observed between crash types for those occupants with SDH and IVH (Frontal, n = 3; Near-Side, n = 3; Far-Side, n = 3). Skull fracture was identified in 23.3% (n = 7) of the occupants. The associated head injuries for each occupant are provided in figure 2. Cerebral edema, soft tissue contusions, and scalp abrasions and lacerations were commonly coded injuries for the occupants evaluated in this study; however these injuries are not represented in figure 2.
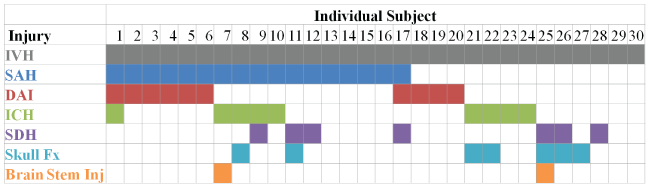
.
Figure 2: Injury distribution of the cases evaluated for this study. IVH = Intraventricular Hemorrhage; SAH = Subarachnoid Hemorrhage; DAI = Diffuse Axonal Injury; ICH = Intracerebral Hemorrhage; SDH = Subdural Hematoma; Fx = Fracture; Inj = Injury
View Figure 2
Figure 3 shows the logarithmic transform of the measured IVH volume plotted by the associated head injury for each subject. As shown in figure 2, many subjects had intra-axial and/or extra-axial head injuries in addition to IVH. In figure 3, each occupant is represented by a single color circle. The volume of IVH for a single occupant with multiple head injuries is connected by a matching color line to demonstrate the measured IVH volume associated with the respective combination of head injuries. Occupants with SAH and DAI had higher volumes of IVH. A trending positive correlation was observed between IVH volume and total head injury severity (Figure 4).
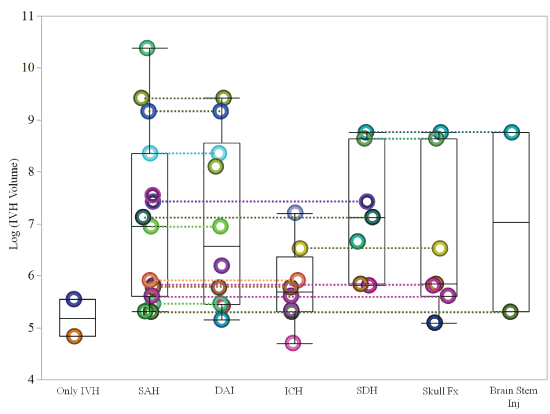
.
Figure 3: Volume distribution and box and whisker plots of the cases evaluated for this study by associated injury. Circles connected by a matching color line are from the same case. IVH = Intraventricular Hemorrhage; SAH = Subarachnoid Hemorrhage; DAI = Diffuse Axonal Injury; ICH = Intracerebral Hemorrhage; SDH = Subdural Hematoma; Fx = Fracture, Inj = Injury.
View Figure 3
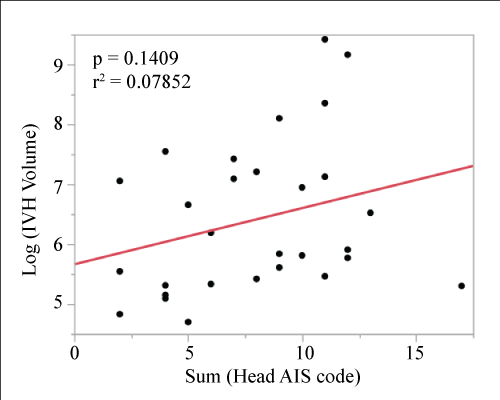
.
Figure 4: Regression plot of the log transformed IVH volume (mm3) and total head injury severity. The solid regression line is fit to all data within the plot (p = 0.1409, r2 = 0.0785).
View Figure 4
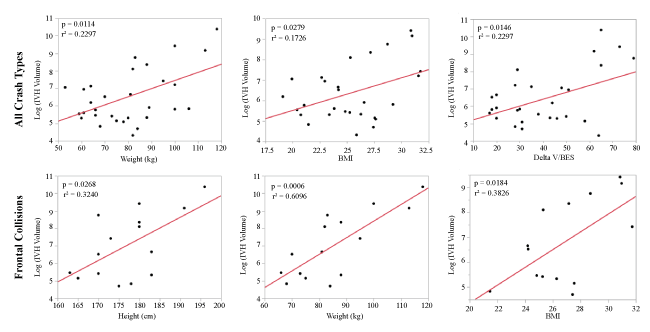
Linear regression was performed to assess the relationship between occupant parameters, crash characteristics, and IVH volume. The p-values and r2 values for correlations with occupant parameters are provided in table 2 and those with crash characteristics are provided in table 3. Linear regression plots with best fit lines of the significant relationships are provided in figure 5. IVH volume was found to be correlated primarily with occupant size (height, weight, and BMI). There was a significant relationship observed between delta-V and IVH volume for all crash types. The strongest correlation was observed between IVH volume and weight in frontal collisions, resulting in an r2 value of 0.6096.
.
Figure 5: Regression plots for the significant relationships between the log transformed IVH volume (mm3) and occupant parameters (top) and crash characteristics (bottom).
View Figure 5
![]()
Table 2: P-values and r2 values of the linear regression with occupant parameters.
Near-Side and Far-Side crashes were not evaluated due to the small number of cases.*Statistically significant.
View Table 2
Discussion
This study related IVH volume to head injury severity, occupant parameters, and crash characteristics. Of the 30 occupants included in the study, half of them were in frontal collisions. The most common injuries associated with IVH were SAH and DAI. IVH volume was greater in those occupants who sustained SAH and/or DAI and volume IVH was greatest in frontal collisions.
![]()
Table 3: P-values and r2 values of the linear regression with crash parameters.
Near-Side and Far-Side crashes were not evaluated due to the small number of cases.*Statistically significant.
View Table 3
The incidence of IVH in head injury has been recognized as concomitant with severe head trauma but is less frequently studied in injury biomechanics. The etiology of IVH is thought to be a shearing injury of the vessels along the walls of the ventricles or intraventricular extension of SAH or neighboring intraparenchymal injuries. Hallevi et al has previously reported a relationship between increased intracranial hemorrhage volume and the presence of IVH, with many of the subjects sustaining intraparenchymal injuries near the ventricular system [21]. Considering the anatomic location of the injury and association with high severity intraparenchymal injuries, such as DAI, one may hypothesize that IVH is associated with strains experienced within the neighboring brain parenchyma resulting from contact-induced rotational loads [22-25]. Further studies of real-world cases are needed to fully understand the mechanical-basis of IVH and the association with intraparenchymal injuries, such as DAI. There are currently no biomechanical injury metrics developed to specifically predict the risk of IVH. Additionally, it is unknown how kinematic injury criterion, such as HIC [26] and BrIC [25], are associated with the risk of IVH. Further analysis involving case reconstruction and finite element modeling may elucidate the aforementioned hypotheses associated with IVH and further improve our understanding of the biomechanical basis of this injury.
Occupant parameters evaluated in this study included age, height, weight, and BMI. Age has been previously reported as a dependable predictor for MVC-associated mortality and has been shown to be of importance when considering the incidence of extra-axial head injuries. However, the relationship between age and IVH severity is unknown. In this study, age was not found to be significantly correlated with IVH volume and, in fact, resulted in the lowest regression coefficient and associated p-value (r2 = 0.0025, p = 0.8033, respectively). However, further analysis with a larger number of real-world occupants is warranted to fully understand this relationship. Height and weight were strongly correlated with IVH volume, especially in frontal collisions. Tagliaferri et al has previously reported that the obese population have nearly double the probability of having a higher maximum head injury in frontal collisions than their non-obese counter-parts [27]. Conflicting studies suggest have suggested that BMI does not play a role in head injury severity and that obesity may have a protective effect on the head [28,29]. Only five occupants in this study were obese (BMI ≥ 30), however the data presented in this study support that occupant size may be a risk factor for increased head injury severity, specifically for IVH. This may be due to the increased loading to contact surfaces within the vehicle during the crash, however the relationship between body size and head acceleration is also not fully understood.
Crash severity metrics, such as ΔV and maximum crush, have been identified as reliable predictors of MVC occupant injury severity in individuals with head trauma [19,30-33] and without head trauma [16,34]. Many of the previous studies have investigated only injury incidence and mortality, with few exploring how specific crash characteristics affect MVC-associated head injury [27,30]. Analysis was performed to determine whether there was a significant correlation between IVH volume and crash characteristics for all crash types and by crash type. Delta-V was found to be significantly correlated with IVH volume, however maximum crush of the vehicle was not. The average ΔV for occupants in this study was 43 kph and the largest mean ΔV was observed in frontal collisions (52.0 kph). The average observed in this study is slightly higher than the average ΔV reported in occupants with SDH (41.3 kph) [19] and DAI (41.2 kph) [35]. A previous study from Yoganandan et al reported the average ΔV of MVC survivors with severe head trauma ranged from 32-35 kph and fatalities with severe head trauma ranged from 42-44 kph [30]. The range of ΔV for the cases evaluated in this study was 17-107 kph. The increased ΔV for those occupants evaluated in this study and significant positive correlation with IVH volume supports that IVH may be associated with higher severity crashes and that severity of this injury may increase with the severity of the crash.
Limitations
This retrospective observational study is subject to lack of control over study conditions and the bias that results. The labor-intensive process of image segmentation allows for inter-observer variability, which was minimized by using multiple independent observers and review of label maps by a board-certified neuroradiologist. Although there were a small number of subjects evaluated in this study, trends were observed which may encourage future evaluation of the contributing factors to head injury volume and severity. Lastly, there may be additional factors that contribute to the volume of the head injury and morbidity/mortality associated with the crash. Patients with underlying disease processes or trauma to multiple body regions may increase the risk of shock, injury severity, and death rate.
Conclusions
This study aimed to relate IVH volume to head injury severity, crash characteristics, and occupant parameters. Significant relationships were observed between IVH volume, total head injury severity, occupant size (height, weight, and BMI), and ΔV/BES. Most of the occupants evaluated in this study were found to have complex combinations of intraparenchymal and extra-axial injuries, with SAH and DAI being the most commonly associated injury. Additionally, subjects with these particular injuries had higher volumes of IVH. Further research into the presence of combined or complex injury presentations could provide a better understanding of injury patterns in MVCs, as well as injury mechanisms.
This type of work may lead to improved methods to predict and prevent specific serious injuries that may be life threatening or have an increased morbidity. Additionally, translational and rotational acceleration-based injury risks [36-38], safety rating systems based on these tools [39] and finite element-based injury metrics and criteria [22,25,40] can all be informed by this work. Consideration needs to be made for those cases with isolated injuries versus those sustaining multiple injuries [41]. Volumetric injury data with known exposure, such as that presented herein, will enable researchers to validate and improve engineers' ability to predict and mitigate or prevent brain injury.
These data highlight the utility of combining clinical neuroimaging with occupant demographics and mechanical crash data for investigating mechanisms of TBI. Such data may also be used in the future to design safer cars and to inform diagnosis and treatment algorithms for MVC-related head trauma. Although little information is provided upon arrival to the Emergency Department (ED), results from this and further studies may aid in the triaging of patients prior to arrival to the ED. Moreover, increased knowledge of crash and associated head injury severity may help guide emergent imaging and neurosurgical decision making.
Acknowledgments
Work was performed for the Crash Injury Research and Engineering Network (CIREN) Project at Wake Forest University School of Medicine in cooperation with the United States Department of Transportation/National Highway Traffic Safety Administration (USDOT/NHTSA). Funding has been provided by National Highway Traffic Safety Administration under Cooperative Agreement Number DTNH22-09-H-00265 and DTNH22-10-H-00294. Views expressed are those of the authors and do not represent the views of NHTSA. Previous funding of the Wake Forest University CIREN center has been provided by Toyota Motor North America Inc under Cooperative Agreement Number DTNH22-05-H-61001.
The authors would like to acknowledge Kathryn Loftis and Ashley Weaver for help with scan acquisition and SQL data download; Colston Edgerton, M.D., Rachel Austin, Kavya Reddy, M.D., Andrew Chambers, Pavani Thotakura, M.D., Nicole Angelo, Amanda Dunn, and Mireille Kelley for assistance in image segmentation; and Landon Edwards, M.D. and Ervin Lowther, M.D. for assistance in review of the image segmentations. Additionally, thank you to the CIREN collaborating centers.
References
-
Faul M, Xu L, Wald MM, Coronado VG (2010) Traumatic brain injury in the United States: emergency department visits, hospitalizations, and deaths. Centers for Disease Control and Prevention.
-
Ventura T, Harrison-Felix C, Carlson N, Diguiseppi C, Gabella B, et al. (2010) Mortality after discharge from acute care hospitalization with traumatic brain injury: a population-based study. Arch Phys Med Rehabil 91: 20-29.
-
Brown AW, Leibson CL, Malec JF, Perkins PK, Diehl NN, et al. (2004) Long-term survival after traumatic brain injury: a population-based analysis. NeuroRehabilitation 19: 37-43.
-
Fazel S, Wolf A, Pillas D, Lichtenstein P, Langstrom N (2014) Suicide, Fatal Injuries, and Other Causes of Premature Mortality in Patients With Traumatic Brain Injury: A 41-Year Swedish Population Study. JAMA Psychiatry 71: 326-333.
-
Cooper PR (1993) Post-traumatic intracranial mass lesions. In: Cooper PR Head Injury. Williams and Wilkens, Baltimore 275-329.
-
Cordobes F, de la Fuente M, Lobato RD, Roger R, Perez C, et al. (1983) Intraventricular hemorrhage in severe head injury. J Neurosurg 58: 217-222.
-
Atzema C, Mower WR, Hoffman JR, Holmes JF, Killian AJ, et al. (2006) Prevalence and prognosis of traumatic intraventricular hemorrhage in patients with blunt head trauma. J Trauma 60: 1010-1017.
-
Oliff M, Fried AM, Young AB (1978) Intraventricular hemorrhage in blunt head trauma. J Comput Assist Tomogr 2: 625-629.
-
LeRoux PD, Haglund MM, Newell DW, Grady MS, Winn HR (1992) Intraventricular hemorrhage in blunt head trauma: an analysis of 43 cases. Neurosurgery 31: 678-684.
-
Post A, Hoshizaki TB, Gilchrist MD, Brien S, Cusimano M, et al. (2015) Traumatic brain injuries: the influence of the direction of impact. Neurosurgery 76: 81-91.
-
NHTSA (2010) Crash Injury Research and Engineering Network Coding Manual. In: Department of Transportation, National Highway Traffic Safety Administration.
-
AAAM (2001) Abbreviated Injury Scale 1990 (Updated 1998). Association for the Advancement of Automotive Medicine.
-
AAAM (2008) Abbreviated Injury Scale 2005 (Updated 2008). Association for the Advancement of Automotive Medicine.
-
Geraci JM, Ashton CM, Kuykendall DH, Johnson ML, Wu L (1997) International Classification of Diseases, 9th Revision, Clinical Modification codes in discharge abstracts are poor measures of complication occurrence in medical inpatients. Med Care 35: 589-602.
-
Hemphill JC 3rd, Bonovich DC, Besmertis L, Manley GT, Johnston SC (2001) The ICH score: a simple, reliable grading scale for intracerebral hemorrhage. Stroke 32: 891-897.
-
Weaver AA, Danelson KA, Armstrong EG, Hoth JJ, Stitzel JD (2013) Investigation of pulmonary contusion extent and its correlation to crash, occupant, and injury characteristics in motor vehicle crashes. Accid Anal Prev 50: 223-233.
-
Danelson KA, Chiles C, Thompson AB, Donadino K, Weaver AA, et al. (2011) Correlating the extent of pulmonary contusion to vehicle crash parameters in near-side impacts. Ann Adv Automot Med 55: 217-230.
-
Gayzik FS, Martin RS, Gabler HC, Hoth JJ, Duma SM, et al. (2009) Characterization of crash-induced thoracic loading resulting in pulmonary contusion. J Trauma 66: 840-849.
-
Urban JE, Whitlow CT, Edgerton CA, Powers AK, Maldjian JA, et al. (2012) Motor vehicle crash-related subdural hematoma from real-world head impact data. J Neurotrauma 29: 2774-2781.
-
Bruce DA (2000) Imaging after head trauma: why, when and which. Childs Nerv Syst 16: 755-759.
-
Hallevi H, Dar NS, Barreto AD, Morales MM, Martin-Schild S, et al. (2009) The IVH score: a novel tool for estimating intraventricular hemorrhage volume: clinical and research implications. Crit Care Med 37: 969-974.
-
Weaver AA, Danelson KA, Stitzel JD (2012) Modeling Brain Injury Response for Rotational Velocities of Varying Directions and Magnitudes. Ann Biomed Eng 40: 2005-2018.
-
Kleiven S, Hardy WN (2002) Correlation of an FE Model of the Human Head with Local Brain Motion--Consequences for Injury Prediction. Stapp Car Crash J 46: 123-144.
-
Ommaya AK, Goldsmith W, Thibault L (2002) Biomechanics and neuropathology of adult and paediatric head injury. Br J Neurosurg 16: 220-242.
-
Takhounts EG, Craig MJ, Moorhouse K, McFadden J, Hasija V (2013) Development of brain injury criteria (BrIC). Stapp Car Crash J 57: 243-266.
-
Mertz HJ, Irwin AL, Prasad P (2003) Biomechanical and scaling bases for frontal and side impact injury assessment reference values. Stapp Car Crash J 47: 155-188.
-
Tagliaferri F, Compagnone C, Yoganandan N, Gennarelli TA (2009) Traumatic brain injury after frontal crashes: relationship with body mass index. J Trauma 66: 727-729.
-
Arbabi S, Wahl WL, Hemmila MR, Kohoyda-Inglis C, Taheri PA, et al. (2003) The cushion effect. J Trauma 54: 1090-1093.
-
Moran SG, McGwin G Jr, Metzger JS, Windham ST, Reiff DA, et al. (2002) Injury rates among restrained drivers in motor vehicle collisions: the role of body habitus. J Trauma 52: 1116-1120.
-
Yoganandan N, Baisden JL, Maiman DJ, Gennarelli TA, Guan Y, et al. (2010) Severe-to-fatal head injuries in motor vehicle impacts. Accid Anal Prev 42: 1370-1378.
-
Nance ML, Kallan MJ, Arbogast KB, Park MS, Durbin DR, Winston FK (2010) Factors associated with clinically significant head injury in children involved in motor vehicle crashes. Traffic Inj Prev 11: 600-605.
-
Weninger P, Hertz H (2007) Factors influencing the injury pattern and injury severity after high speed motor vehicle accident--a retrospective study. Resuscitation 75: 35-41.
-
Yoganandan N, Fitzharris M, Pintar FA, Stemper BD, Rinaldi J, et al. (2011) Demographics, Velocity Distributions, and Impact Type as Predictors of AIS 4+ Head Injuries in Motor Vehicle Crashes. Ann Adv Automot Med 55: 267-280.
-
Richter M, Krettek C, Otte D, Stalp M, Wiese B, et al. (2001) Correlation between crash severity, injury severity, and clinical course in car occupants with thoracic trauma: a technical and medical study. J Trauma 51: 10-16.
-
Yoganandan N, Gennarelli TA, Zhang J, Pintar FA, Takhounts E, et al. (2009) Association of contact loading in diffuse axonal injuries from motor vehicle crashes. J Trauma 66: 309-315.
-
Rowson S, Brolinson G, Goforth M, Dietter D, Duma S (2009) Linear and angular head acceleration measurements in collegiate football. J Biomech Eng 131: 061016.
-
Rowson S, Duma SM, Beckwith JG, Chu JJ, Greenwald RM, et al. (2012) Rotational head kinematics in football impacts: an injury risk function for concussion. Ann Biomed Eng 40: 1-13.
-
Rowson S, Duma SM (2013) Brain injury prediction: assessing the combined probability of concussion using linear and rotational head acceleration. Ann Biomed Eng 41: 873-882.
-
Rowson S, Duma SM (2011) Development of the STAR evaluation system for football helmets: integrating player head impact exposure and risk of concussion. Ann Biomed Eng 39: 2130-2140.
-
Takhounts E, Hasija V, Ridella SA, Rowson S, Duma S (2011) Kinematic Rotational Brain Injury Criterion (BRIC). 22nd Enhanced Safety of Vehicles Conference Preceedings.
-
Stitzel JD, Kilgo PD, Danelson KA, Geer CP, Pranikoff T, et al. (2008) Age thresholds for increased mortality of three predominant crash induced head injuries. Ann Adv Automot Med 52: 235-244.





