Trauma Cases and Reviews
Early Stage Tibia Osteomyelitis Despite The Use of Hydroxyapatite Schanz Screws: A Case Report
Ali Çagri Tekin, Murat Çakar*, Müjdat Adas, Mehmet Kürsad Bayraktar, Haluk Çabuk, Ali Yüce and Yusuf Özcan
Okmeydani Research and Training Hospital, Orthopaedics and Traumatology Clinic, Turkey
*Corresponding author: Murat Çakar, Okmeydani Research and Training Hospital, Orthopaedics and Traumatology Clinic, Ìstanbul, Turkey, Tel: +905052702922, E-mail: drmuratcakar@gmail.com
Trauma Cases Rev, TCR-1-004, (Volume 1, Issue 1), Case Report; ISSN: 2469-5777
Received: April 02, 2015 | Accepted: July 14, 2015 | Published: July 16, 2015
Citation: Tekin AC, Çakar M, Adas M, Bayraktar MK, Çabuk H, et al. (2015) Early Stage Tibia Osteomyelitis Despite The Use of Hydroxyapatite Schanz Screws: A Case Report. Trauma Cases Rev 1:004. 10.23937/2469-5777/1510004
Copyright: © 2015 Çakar M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
In a 7-year old patient with a right cruris Grade 1 open fracture, an external fixator was applied using hydroxyapatite-covered Schanz screws. After 6 weeks the fixator and screws were removed. Two months after the removal of the fixator, the patient presented with pain in the proximal of the medial pin site and osteomyelitis was determined in the proximal right cruris. Surgical debridement was applied and from the pathology examination of material taken intraoperatively, osteomyelitis was determined. As a result of culture implantation, methicillin-sensitive staphylococcus aureus was reproduced. Treatment was applied of antibiotic sensitive to that micro-organism. In a 1-year postoperative follow-up, the patient was seen to recover.
Keywords
Hidroxyapatite Schanz screw, Tibia fracture, Osteomyelitis
Introduction
The most common complication resulting from the use of external fixators in orthopaedics and traumatology operations is the development of pin and Schanz screw tract infections. Subsequent to the development of pin and Schanz screw tract infection, osteomyelitis in that area is occasionally seen. Infection rates can be reduced with the use of hydroxyapatite Schanz screws and appropriate surgical technique [1-4].
The case is here presented of a patient treated with external fixator and hydroxyapatite Schanz screws for a tibial fracture, who then developed osteomyelitis. To the best of our knowledge, this occurrence has not been previously reported in literature.
Case
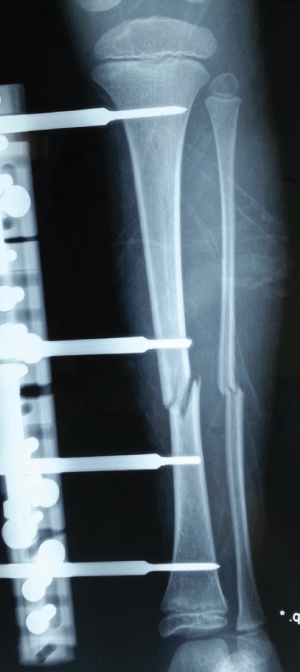
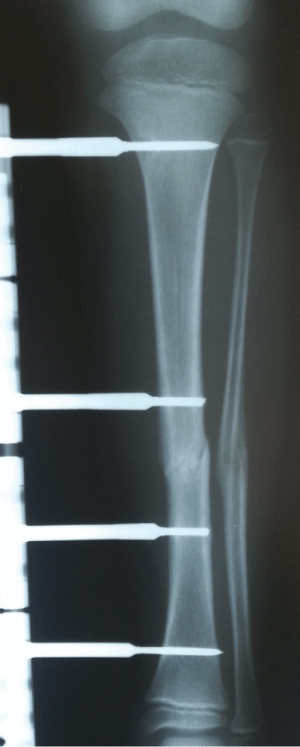
A 7-year old male patient presented at hospital after being struck by a motor vehicle and the first examination determined a Grade 1 open tibia fracture. The patient underwent surgery and an LRS-type external fixator was applied with 4 hydroxyapatite covered Schanz screws of 3mm diameter (Figure 1). With polyclinic follow-up examinations, union was observed in the fracture in the 6th week (Figure 2).
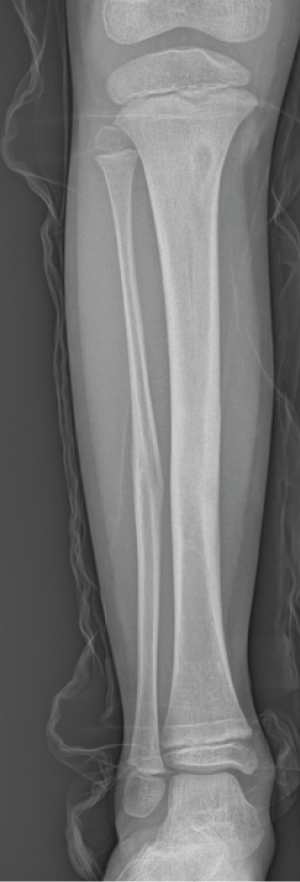
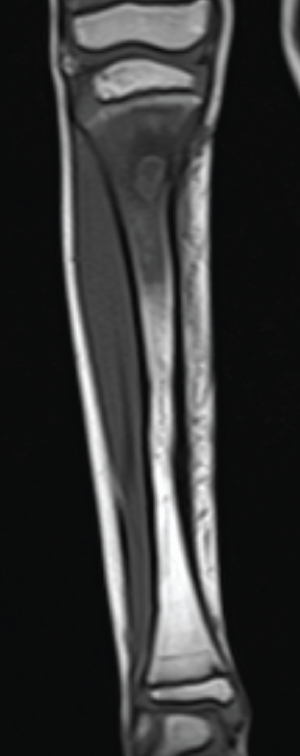
The fixator was removed and the patient was discharged. Two months after the removal of the fixator, the patient presented at the polyclinic with complaints of pain in the operated leg. In the physical examination, the patient's general status was good. The temperature of the patient was 37℃ and pulse was measured as 80/min. There was pain in the right cruris proximal anterior medial in the site of the first Schanz screw. No temperature increase or redness was determined in the area. No neurological or vascular deficit was determined. The results of routine laboratory tests were white cells 7500/mm3, erythrocyte sedimentation rate 20mm/hr, C-reactive protein (CRP) 6 and other biochemical parameters were within normal limits. On direct radiographs and magnetic resonance imaging (MRI) an appearance was determined consistent with osteomyelitis in the proximal right tibia at the location of the hydroxyapatite-covered Schanz screw (Figures 3,4).
As the pain continued, surgical intervention was applied with fenestration debridement and curettage. Culture and pathology samples were taken intraoperatively and were sent to the microbiology laboratory. At the end of the operation, a long-leg splint was applied to the extremity. After the operation, a paediatric infectious diseases physician was consulted. As a result of the histopathological examination, a report was given as consistent with osteomyelitis. The culture-antibiogram resulted in reproduction and the pathogen agent was seen to be methicillin-sensitive staphylococcus aureus. Treatment of antibiotic sensitive to that micro-organism was applied for 3 weeks parenterally and thereafter orally. There was immediate postoperative pain relief and in the follow-up period the patient was seen to recover. In the radiological examinations, a complete recovery was observed.
Discussion
Unilateral external fixators held to the bone with single plane Schanz screws are robust and light external fixators. With the observation of healing over time, fracture healing is increased to a dynamic state in a short time, generally in 3-4 weeks thus achieving union at least 2 weeks earlier [5,6].
Large Schanz screws have a greater potential to create screw site infection compared to small Schanz screws, which is the main reason for early termination of this treatment [3].
In respect of infection and loosening in the application of external fixators, there are beneficial effects of hydoxyapatite Schanz screws compared to normal Schanz screws [7]. Among the important features of hydroxyapatite-covered Schanz screws is the excellent biological compatability. The osteoconductive properties of hydroxyapatite provide the environment and possibility of holding the implant tight to the bone. In some animal experiments, following the application then removal 6-9 weeks after surgery of hydroxyapatite Schanz screws, no radiolgical or clinical complications have been determined. These screws have been recommended for use in patients where a tibial external fixator is to be applied [7,8].
This paper presents the case of a 7-year old patient in whom early pin site infection resulted in osteomyelitis despite the use and removal of hydroxyapatite Schanz screws and who was successfully surgically treated.
References
-
Rommens P, Gielen J, Broos P, Gruwez J (1989) Intrinsic problems with the external fixation device of Hoffmann-Vidal-Adrey: a critical evaluation of 117 patients with complex tibial shaft fractures. J Trauma 29: 630-638.
-
Clifford RP, Lyons TJ, Webb JK (1987) Complications of external fixation of open fractures of the tibia. Injury 18: 174-176.
-
Mahan J, Seligson D, Henry SL, Hynes P, Dobbins J (1991) Factors in pin tract infections. Orthopedics 14: 305-308.
-
Magyar G, Toksvig-Larsen S, Moroni A (1997) Hydroxyapatite coating of threaded pins enhances fixation. J Bone Joint Surg Br 79: 487-489.
-
Ates Y, Ömeroglu H, Uçar HD, Korkusuz Z (1994) Tibia cisim kiriklarinda farkli tedavi metodlarinin karsilaitirilmasi. Acta Orthopedica Travmatologica Turcica 28: 90-93.
-
Krettek C, Haas N, Tscherne H (1989) Results of treatment of 202 fresh tibial shaft fractures, managed with unilateral external fixation (monofixateur). Unfallchirurg 92: 440-452.
-
Augat P, Claes L, Hanselmann KF, Suger G, Fleischmann W (1995) Increase of stability in external fracture fixation by hydroxyapatite-coated bone screws. J Appl Biomater 6: 99-104.
-
Moroni A, Faldini C, Pegreffi F, Giannini S (2002) Fixation strength of tapered versus bicylindrical hydroxyapatite-coated external fixation pins: an animal study. J Biomed Mater Res 63: 61-64.