Trauma Cases and Reviews
Primary Total Elbow Arthroplasty in the Treatment of Complex Elbow Fracture: A Case Report
Pedro Miguel Campos1*, Bárbara Rosa1, André Barros1, Carlos Durão2, Glória Magalhães2, Clara Júlio2 and Pedro Quinaz Neto2
1Orthopaedic Resident, Department of Orthopaedic Surgery, Hospital Vila Franca de Xira, Portugal
2Orthopaedic Surgeon, Department of Orthopaedic Surgery, Hospital Vila Franca de Xira, Portugal
*Corresponding author: Pedro Miguel Campos, Orthopaedic Resident, Department of Orthopaedic Surgery, Hospital Vila Franca de Xira, Vila Franca de Xira, Portugal, E-mail: pedro.mrcampos@gmail.com
Trauma Cases Rev, TCR-1-005, (Volume 1, Issue 1), Case Report; ISSN: 2469-5777
Received: April 30, 2015 | Accepted: July 30, 2015 | Published: August 01, 2015
Citation: Campos PM, Rosa B, Barros A, Durão C, Magalhães G, et al. (2015) Primary Total Elbow Arthroplasty in the Treatment of Complex Elbow Fracture: A Case Report. Trauma Cases Rev 1:005. 10.23937/2469-5777/1510005
Copyright: © 2015 Campos PM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: Some elbow fractures are very complex with inadequate bone stock, so it is not possible to perform a stable fixation. However, loss of basic elbow function can severely affect daily living activities. There are few alternatives to internal fixation, but arthroplasty can be a reasonable option. The aim of this case report is to evaluate the role of primary total elbow arthroplasty in the treatment of complex elbow fractures
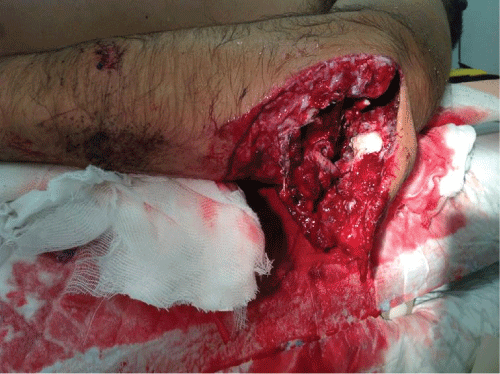
Case study: A 54-year-old male patient presented at our emergency department in the sequence of a motorcycle accident, which caused an open fracture of the left elbow, classified as type IIIB of Gustilo and Anderson. The X-ray showed comminuted fractures of distal humerus and proximal ulna with bone loss from both epiphysis. He started antibiotherapy and was submitted to immediate surgical debridement, provisional fixation with an external fixator and skin closure. The external fixator was removed 2 months after, when the patient presented with great elbow instability. The X-ray and the Computed Tomography showed signals of malunion and bone loss, which prevented any kind of fixation. Therefore, 3 months after, the patient was submitted to elbow joint replacement. A posterior approach was used, in which the triceps was reflected and was applied a linked arthroplasty - Coonrad-Morrey total elbow arthroplasty. On the second week after surgery, passive motion was started and by the fourth week, progressed to active motion. Six months after, he presented without significant pain and with a range of motion of 0° to 135°.
Conclusions: Although rarely used, total elbow arthroplasty may be the choice in selected patients with elbow fractures with loss of bone. As shown in this case, this treatment can lead to a satisfactory functional recovery. Despite having some complications, more recent studies encourage its use in the future.
Keywords
Elbow, Comminuted fractures, Arthroplasty
Introduction
In the past, the indications for elbow arthroplasty were quite limited and included cases of rheumatoid arthritis and post-traumatic arthrosis [1,2]. Even in those cases, it was recommended in elderly patients with a low functional demand, due to its low durability [3,4]. Nevertheless, in the last few years, a reasonable evolution has occurred in terms of its indications and outcomes [5-7]. Nowadays, the use of elbow arthroplasty may be necessary in selected cases of complex fractures of the elbow, with good functional results [8,9]. The aim of this case report is to evaluate the role of elbow arthroplasty as a primary option in complex fractures of the elbow.
Case Study
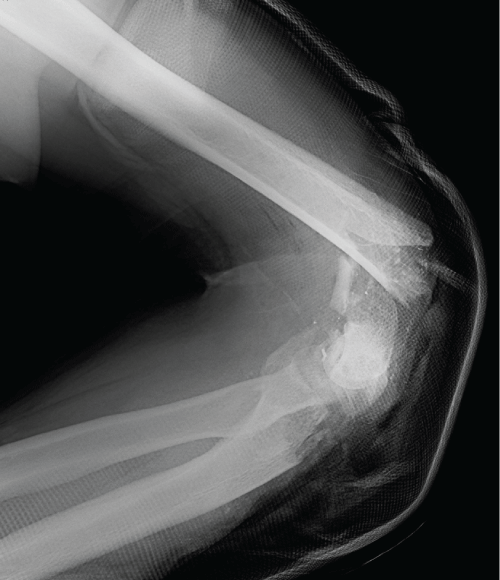
We describe the case of a 54-year-old male patient, waiter of profession, who presented to our Emergency Department with a left elbow trauma in the sequence of a motorcycle accident. He presented an open fracture classified as type IIIB of Gustilo and Anderson (Figure 1). The X-ray revealed comminution of the distal humerus and proximal ulna with important bone loss of the articular surface of both (Figure 2). He began antibiotherapy with Gentamicin and Ceftriaxone and was submitted to immediate surgery. In what concerns soft tissue injury, he presented a great destruction of the medial and lateral collateral ligaments while nervous and vascular structures were intact. It was classified as type II of Tscherne. We performed surgical debridement, provisional fixation with an external fixator and skin closure. Favorable wound healing was verified and he finished the monitorized protocol two weeks later.
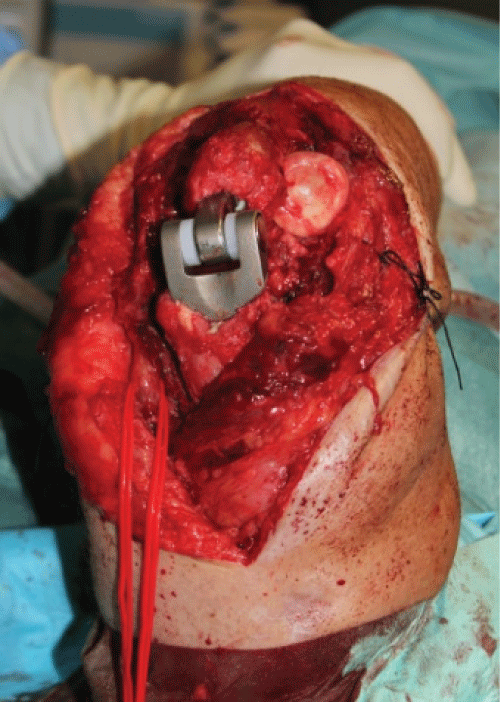
In order to exclude possible infection, we monitorized the C-reactive protein levels, which decreased gradually. Two months later, the X-ray and the Computed Tomography showed signals of malunion (Figure 3) and the external fixator was removed. In the postoperative period we noticed an important elbow instability and reduced mobility. We considered multiple treatment options and concluded that internal fixation would not be possible given the absence of adequate articular surfaces. In this sense, we decided to perform a total elbow arthroplasty three months after the accident. By a posterior approach, the triceps was externally reflected, the distal humeral extremity was regularized, the bone sequestra were removed and the ulna was prepared. A linked arthroplasty was applied - Coonrad-Morrey total elbow arthroplasty. The extensor apparatus was inserted directly over the prosthesis (Figure 4). Ulnar nerve transposition was not necessary.
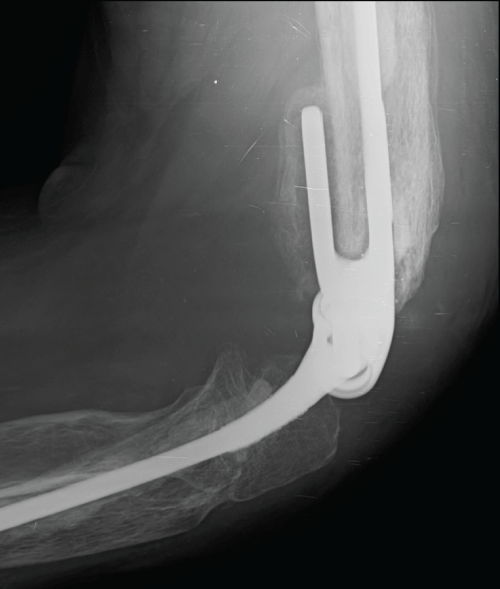
In the postoperative period, we verified adequate healing and the X-ray revealed correct prosthesis implantation (Figure 5). Two weeks later, the patient began rehabilitation with passive elbow motion that gradually progressed to active motion. Six weeks after surgery, the patient was capable of feeding himself and began strength exercises. We verified a progressive increase in strength and in range of motion. Six months after arthroplasty, the patient resumed his laboral activity and presented with no pain or sensory alterations. Furthermore, he presented a range of motion of 0-135°, with a light supination deficit and a moderate muscular strength decrease.
Discussion
The presented case refers to a patient with the diagnosis of an open elbow fracture with important distal humeral and proximal ulna bone loss. After initial fracture stabilization with an external fixator, it became mandatory to find a therapeutic alternative that permitted to restore elbow function and stability. Although osteosynthesis should be the first option, in this case, the huge bone loss (mainly articular) turned it unfeasible. Some last resort procedures have been described, such as immobilization with orthosis, arthrodesis or amputation [10]. However, these are associated with functional limitations and with worse aesthetic outcomes [11]. In this sense, a procedure that permits the reestablishment of the limb structural integrity, with pain remission and with strength and function improvement, is desirable. The total elbow arthroplasty emerges as a viable option in these cases. In contrast with previous reports, several authors have recently shown favorable results with this procedure in traumatic injuries [11-14]. The Coonrad-Morrey total elbow arthroplasty allows to make up for the bone defects, to correct the limb structure and alignment and to stabilize the joint. Despite some pronation-supination limitations and strength deficits, satisfactory motion, that permits daily activities, can be obtained [15].
Historically, it was considered that elbow arthroplasty was related to low survival. This was one of the main reasons against its use. However, using recently developed materials, a 5-year-survival rate of 97,7% and a 10-year-survival rate of 91,0% are described [16]. Other described complications include ulnar and radial nerve injury, infections, delayed wound healing and periprosthetic fractures [16-18].
In this case, of an active young patient with a non- reconstructable fracture, last resort procedures would lead to an important functional loss with an associated worse quality of life. The elbow arthroplasty allowed pain remission and functional recovery with a high satisfaction index. We recommended the patient to avoid strength activities and plan to follow him on an annual basis, with clinical and radiological assessments.
Conclusion
Total elbow arthroplasty is a good alternative for elbow complex fractures. The indications for total elbow replacement in traumatic injuries included classic complications and sequelae of elbow fractures. However, more recent studies encourage its use as primary treatment in complex fractures. Despite having some complications, elbow arthroplasties can have good functional results, as we show in this case, with a prompt return to daily living activities.
References
-
Kokkalis ZT, Schmidt CC, Sotereanos DG (2009) Elbow arthritis: current concepts. J Hand Surg Am 34: 761-768.
-
Hargreaves D, Emery R (1999) Total elbow replacement in the treatment of rheumatoid disease. Clin Orthop Relat Res 366: 61-71
-
Mansat P, Adams RA, Morrey BF (2004) Allograft-prosthesis composite for revision of catastrophic failure of total elbow arthroplasty. J Bone Joint Surg Am 86: 724-735.
-
Prasad N, Dent C (2010) Outcome of total elbow replacement for rheumatoid arthritis: single surgeon's series with Souter-Strathclyde and Coonrad-Morrey prosthesis. J Shoulder Elbow Surg 19: 376-383.
-
Corradi M, Frattini M, Panno B, Tocco S, Pogliacomi F (2010) Linked semi-constrained total elbow prosthesis in chronic arthritis: results of 18 cases. Musculoskelet Surg 94: 11-23.
-
Cobb TK, Morrey BF (1997) Total elbow arthroplasty as primary treatment for distal humeral fractures in elderly patients. J Bone Joint Surg 79: 826-832.
-
Gambirasio R, Riand N, Stern R, Hoffmeyer P (2001) Total elbow replacement for complex fractures of the distal humerus: an option for the elderly patient. J Bone Joint Surg 83: 974-978.
-
Ducrot G, Ehlinger M, Adam P, Di Marco A, Clavert P, et al. (2013) Complex fractures of the distal humerus in the elderly: Is primary total elbow arthroplasty a valid treatment alternative? A series of 20 cases. Orthop Traumatol Surg Res 99: 10-20.
-
McKnee MD, Veillette CJ, Hall JA, Schemitsch EH, Wild LM (2009) A multicenter, prospective, randomized, controlled trial of open reduction - internal fixation versus total elbow arthroplasty for displaced intra- articular distal humeral fractures in elderly patients. J Shoulder Elbow Surg 18: 3-12.
-
Kalicke T, Weber O, Backhaus M, Muhr G, Citak M (2010) Salvage procedures of the elbow: Alternatives to elbow arthroplasty. Unfallchirurg 113: 990-995.
-
Franke A, Bieler D, Hentsh S, Johann M, Kollig E (2014) Reconstruction of an elbow joint after blast injury by arthroplasty with a custom-made modified total elbow prosthesis: a case report. J Shoulder Elbow Surg 23: 81-87.
-
Maheshwari R, Vaziri S, Helm RH (2012) Total elbow replacement with Coonrad-Morreyprosthesis: our medium to long-term results. Ann R Coll Surg Engl 94: 189-192.
-
Prasad N, Dent C (2008) Outcome of total elbow replacement for distal humeral fractures in the elderly. J Bone Joint Surg Br 90: 343-348.
-
Pogliacomi F, Galavotti C, Cavaciocchi M, Corradi M, Rotini R (2014) Total elbow artroplasty following traumas: mid-term results. Acta Biomed 84: 212-218.
-
Chalidis B, Dimitrou C, Papadopoulos P (2009) Total elbow artrhoplasty for the treatment of insuficiente distal humeral fractures. A retrospective clinical study and review of the literature. Injury 40: 582-590.
-
Mansat P, Bonnevialle N, Rongières M, Mansat M, Bonnevialle P (2013) Experience with theCoonrad-Morrey total elbow arthroplasty: 78 consecutive total elbow arthroplasties reviewed with an average 5 years of follow-up. J Shoulder Elbow Surg 22: 1461-1468.
-
Morrey BF (2000) Complications of elbow replacement surgery. The elbow and its disorders: 667-676.
-
Shi LL, Zurakowski D, Jones DG, Koris MJ, Thornhill TS (2007) Semiconstrained primary and revision total elbow arthroplasty with use of Coonrad-Morrey prosthesis. J Bone Joint Surg Am 89: 1467-1475.