Obstetrics and Gynaecology Cases - Reviews
Diagnosis and Management of Embryonal Rhabdomyosarcoma in a Woman with Prolapsing Cervical Mass
Elizabeth V. Connor1* and Paul A. Disilvestro2
1Department of Obstetrics and Gynecology, Women and Infants Hospital of Rhode Island, USA
2Division of Gynecologic Oncology, Women and Infants Hospital of Rhode Island, USA
*Corresponding author: Elizabeth V. Connor, MD, Department of Obstetrics and Gynecology, Women and Infants Hospital of Rhode Island, 101 Dudley Street, Providence, RI 02905, USA, Tel: 401-274-1122, E-mail: econnor@wihri.org
Obstet Gynecol Cases Rev, OGCR-2-050, (Volume 2, Issue 4), Case Report; ISSN: 2377-9004
Received: June 09, 2015 | Accepted: July 07, 2015 | Published: July 10, 2015
Citation: Connor EV, Disilvestro PA (2015) Diagnosis and Management of Embryonal Rhabdomyosarcoma in a Woman with Prolapsing Cervical Mass. Obstet Gynecol Cases Rev 2:050. 10.23937/2377-9004/1410050
Copyright: © 2015 Connor EV, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Cervical rhabdomyosarcoma is very rare, comprising less than 1% of cervical cancers in adult women. Less than 40 cases of cervical rhabdomyosarcoma have been reported in adult women in the last 50 years. Due to the rarity of this disease, management guidelines are non-existent.
Case: We present a 36-year-old woman who presented with pelvic pain and a vaginal mass. The mass was excised, and pathology confirmed poorly differentiated embryonal type rhabdomyosarcoma. She then underwent total laparoscopic hysterectomy and bilateral salpingectomy followed by adjuvant chemotherapy with vincristine, actinomycin-D, and cyclophosphamide (VAC) alternating with etoposide and ifosphamide.
Conclusion: Due to the rare incidence of cervical embryonal rhabdomyosarcomas in adult women, management guidelines are lacking. Typical management consists of surgical excision of the tumor followed by adjuvant chemotherapy and possible radiation.
Keywords
Cervical cancer, Cervical mass, Embryonal rhabdomyosarcoma
Introduction
Squamous cell carcinoma is the most common type of cervical cancer, followed by adenocarcinoma, adenosquamous carcinoma, and neuroendocrine carcinomas [1]. Cervical rhabdomyosarcoma is very rare, comprising less than 1% of all cervical cancers, and about half of these are embryonal type [1]. Further, rhabdomyosarcoma of the cervix most commonly presents in pre-pubertal women or in reproductive age women in their teens and twenties. Classic histopathologic features of rhabdomyosarcoma include variable cellularity with primitive cells in the perivascular region and below the epithelium, a background of loose myxoid stroma, and mesenchymal cells in various stages of maturation called rhabdomyoblasts [2]. Embryonal rhabdomyosarcoma is classically distinguished by polypoid or grape-like clusters of edematous and nodular tissue [3]. Diagnosis is confirmed by staining for vimentin, desmin, actin, myoglobin, MyoD1, and myogenin on immunohistochemistry [4]. Due to the rarity of rhabdomyosarcoma in older women, firm management guidelines are non-existent. Additionally, prognostic information for patients is lacking. We present the case of a woman in her thirties diagnosed with cervical embryonal rhabdomyosarcoma.
Case Report
A 35-year-old woman, gravida 2 para 2, presented to the emergency room with pelvic pain and a mass prolapsing from the vagina. She reported that the mass had grown within the preceding two weeks. Her medical and surgical histories were negative, and she had two prior uncomplicated vaginal deliveries. She was a nonsmoker with normal Pap smears as recently as 1 year prior to this presentation. Family history was negative for breast, ovarian, and colon cancers. A cervical exam performed at her annual visit four months earlier demonstrated a normal parous cervix.
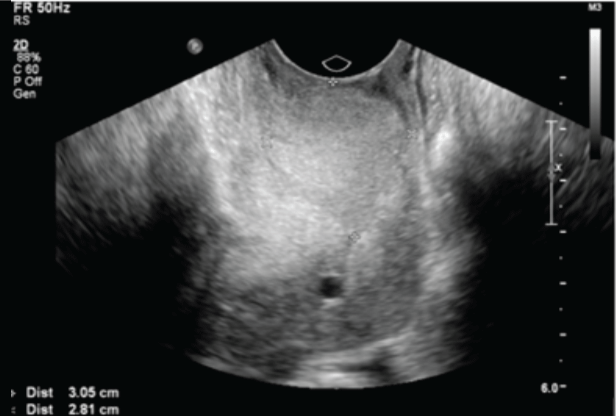
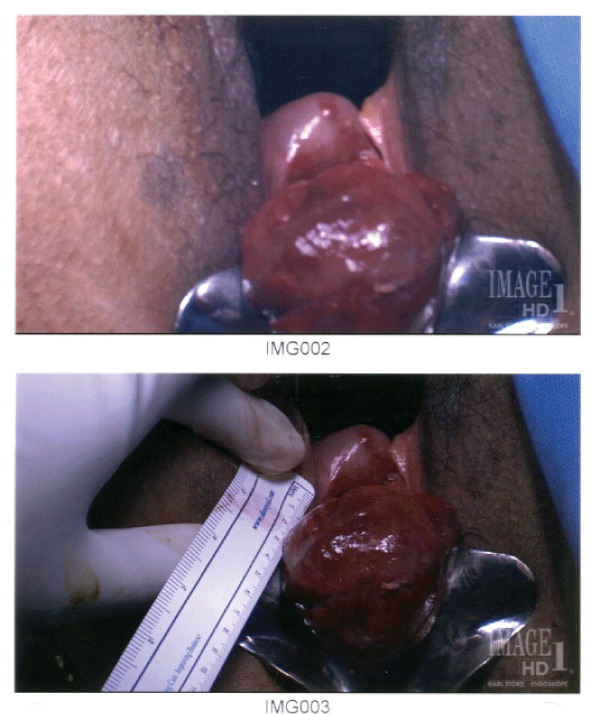
Pelvic examination demonstrated a heterogeneous 5cm mass protruding into the vagina and was considered consistent with a prolapsing polyp or fibroid. The uterus was easily palpated and was mobile with normal contour. A transvaginal ultrasound demonstrated a 3 x 2.8 x 4cm vascular mass protruding into the vagina. The uterus was noted to be of normal size and contour with no fibroids documented. The ovaries were normal in appearance (Figure 1). Exam under anesthesia was notable for a cervical mass emerging from the posterior lip of the cervix (Figure 2). The uterus and adnexae including the uterosacral ligaments and rectovaginal space were normal on exam. Differential diagnosis prior to excision included endocervical polyp, prolapsed uterine leiomyoma or leiomyosarcoma, benign or malignant rhabdomyoma, and benign or malignant adenomyoma.
.
Figure 2: Intraoperatively, the cervical mass is shown to be contiguous with the posterior lip of the cervix, protruding through the introitus.
View Figure 2
The mass was excised at the level of the external os. Intraoperative frozen section was concerning for cervical stromal neoplasm versus sarcoma. Final pathology confirmed a 5.5 x 3.0cm high grade embryonal type rhabdomyosarcoma which demonstrated increased stromal cellularity with spindle cell morphology, striated rhabdomyoblasts, and prominent nucleoli with numerous mitoses and increased proliferative activity. Surgical margins were negative and there was no lymphovascular space invasion. Immunohistochemistry staining was positive for MyoD-1 and desmin, supporting a diagnosis of rhabdomyosarcoma. Immunohistochemistry staining also demonstrated Ki-67, suggesting high proliferation. The tumor was negative for CD34, cytokeratin, caldesmon, and S-100 protein.
Postoperative MRI of the pelvis demonstrated normal appearing uterus, ovaries, and no ascites or adenopathy. No residual mass was noted. PET CT demonstrated only slightly increased activity in the right adnexa and lower uterus most likely related to her recent surgery. Her case was presented at a multidisciplinary tumor board with recommendation for complete metastatic evaluation, hysterectomy with ovarian conservation and referral to medical oncology for adjuvant chemotherapy.
She underwent total laparoscopic hysterectomy and bilateral salpingectomy with ovarian conservation. Pathology was negative for residual sarcoma. Postoperative course was routine and she was discharged to home postoperative day 1. She was subsequently referred to medical oncology for consultation and received adjuvant chemotherapy with vincristine, actinomycin-D, and cyclophosphamide (VAC) alternating with ifosfamide and etoposide every 3 weeks.
Discussion
There are three subtypes of rhabdomyosarcoma: embryonal, alveolar, and undifferentiated or pleomorphic [5]. 58% of all rhabdomyosarcomas are of the embryonal subtype [6]. On histology, the embryonal subtype is distinguished by the appearance of rhabdomyoblasts of varying differentiation within a myxoid stroma [7]. The International Rhabdomyosarcoma Study Group's staging criteria include tumor size greater or less than 5cm, extension to surrounding tissue, lymph node and distant metastasis. Early stage disease, embryonal subtype, younger age, and exophytic features all suggest a more favorable prognosis [6].
While rhabdomyosarcoma is a common malignancy in children, comprising 50% of all soft tissue sarcomas, only 0.5% of these are located within the cervix [8]. Rhabdomyosarcoma of the cervix is even rarer among adult women. Approximately 1% of all adult malignancies are sarcomas, and rhabdomyosarcomas account for less than 5% of all sarcomas in this age group [9,10]. There are less than 40 reported cases of cervical embryonal type rhabdomyosarcoma in adult women in the last 50 years and long term clinical outcome data are lacking [5]. Consequently, there is no general consensus on the management of adult women with rhabdomyosarcoma of the cervix and outcome data are derived from the pediatric population due to the higher incidence of disease in this group.
The surgical management of pediatric patients with rhabdomyosarcoma has shifted away from primary radical surgery to local excision of tumor, lowering the overall morbidity of treatment without significantly affecting overall survival [5,11]. Currently in the pediatric population, surgical management focuses on complete primary resection of the tumor with a surrounding margin, as well as appropriate lymph node sampling. In the Intergroup Rhabdomysarcoma Study (IRS), pediatric patients with gross residual disease after surgery had a 5-year survival rate of 70% compared to a >90% 5-year survival rate for patients with no residual disease [11]. Case reports of adult women with cervical rhabdomyosarcoma have similarly been treated with primary surgical excision of tumor. Ferguson et al published a case series of adult women with rhabdomyosarcoma of the genital tract which included eight women with cervical disease. Clinical follow-up information was available for 7 of the 8 women, all of which were managed primarily with surgery. Six women presented with localized disease and underwent hysterectomy, bilateral salpingo-oophorectomy, pelvic and para-aortic lymph node dissection. The remaining patient presented with advanced stage disease and underwent pelvic and para-aortic lymph node dissection only with ovarian transposition prior to adjuvant chemotherapy. Three of the seven women died of their disease within 2 years, including the patient with advanced disease at presentation. One woman recurred at 19 months, and the remaining three women were without evidence of disease for a mean follow-up of 24 months [5]. Daya and Scully published a case series of 13 women with rhabdomyosarcoma. Three of these women underwent fertility-sparing surgery with either polypectomy or trachelectomy and adjuvant chemotherapy. These women had comparable outcomes to women who underwent more radical surgeries within the case series [12]. While the data seem to support conservative surgical management directed at tumor excision, it is difficult to derive meaningful conclusions from such small cohorts.
Adjuvant chemotherapy is commonly used for patients with rhabdomyosarcoma due to the potential for hematogenous spread even in presumed early stage disease. Common regimens for low to intermediate risk disease include vincristine, actinomycin-D, and cyclophosphamide (VAC) [6,11]. Cyclophosphamide has been found to improve progression-free survival but not overall survival [11]. Etoposide and ifosphamide have been used to treat higher risk presentations [11]. Adjuvant radiation therapy is typically reserved for patients with residual disease after surgery [11]. There are no prospective data on the adjuvant treatment of adults with rhabdomyosarcoma. Interestingly, progression-free and overall survival are significantly poorer in adult women than in the pediatric population. It is unknown if this disparity is due to variable response to treatment of adult versus pediatric types, or whether adult patients are not treated adequately [13].
Clearly, more information regarding treatment and survival outcomes for adult women with cervical rhabdomyosarcoma is needed. A database with clinical and survival data may be a useful adjunct in determining management of these patients in the future. With the current understanding of disease, primary surgical management with local resection of tumor followed by targeted multi-agent chemotherapy such as VAC is a reasonable approach to management.
Ethical Statement
This case report is waived from our institution's Institutional Review Board. The patient signed a consent form approving the use of her case including photographs for educational purposes.
References
-
Khosla D, Patel FD, Kumar R (2013) Sarcomas of the uterine cervix: a united and multidisciplinary approach is required. Womens Health (Lond Engl) 9: 501-504.
-
Enzinger FM (1995) Rhabdomyosarcoma. In: Weiss SW. Soft Tissue Tumors. (3rd edn). St Louis: CV Mosby: 539-577.
-
Hilgers RD (1975) Pelvic exenteration for vaginal embryonal rhabdomyosarcoma: a review. Obstet Gynecol 45: 175-180.
-
Morotti RA, Nicol KK, Parham DM, Teot LA, Moore J, et al. (2006) An immunohistochemical algorithm to facilitate diagnosis and subtyping of rhabdomyosarcoma: the Children's Oncology Group experience. Am J Surg Pathol 30: 962-968.
-
Ferguson SE, Gerald W, Barakat RR, Chi DS, Soslow RA (2007) Clinicopathologic features of rhabdomyosarcoma of gynecologic origin in adults. Am J Surg Pathol 31: 382-389.
-
Kriseman ML, Wang WL, Sullinger J, Schmeler KM, Ramirez PT, et al. (2012) Rhabdomyosarcoma of the cervix in adult women and younger patients. Gynecol Oncol 126: 351-356.
-
Bernal KL, Fahmy L, Remmenga S, Bridge J, Baker J (2004) Embryonal rhabdomyosarcoma (sarcoma botryoides) of the cervix presenting as a cervical polyp treated with fertility-sparing surgery and adjuvant chemotherapy. Gynecol Oncol 95: 243-246.
-
Jayi S, Bouguern H, Fdili FZ, Chaara H, Chbani L, et al. (2014) Embryonal rhabdomyosarcoma of the cervix presenting as a cervical polyp in a 16-year-old adolescent: a case report. J Med Case Rep 8: 241.
-
Adams BN, Brandt JS, Loukeris K, Holcomb K (2011) Embryonal rhabdomyosarcoma of the cervix and appendiceal carcinoid tumor. Obstet Gynecol 117: 482-484.
-
Lagh R, Krapcho M, Mariotto A, Miller BA, Feuer EJ, et al. (2006) SEER Cancer Statistics Review, 1975-2003. Bethesda: National Cancer Institute.
-
Villella JA, Bogner PN, Jani-Sait SN, Block AM, Lele S (2005) Rhabdomyosarcoma of the cervix in sisters with review of the literature. Gynecol Oncol 99: 742-748.
-
Daya DA, Scully RE (1988) Sarcoma botryoides of the uterine cervix in young women: a clinicopathological study of 13 cases. Gynecol Oncol 29: 290-304.
-
Ferrari A, Dileo P, Casanova M, Bertulli R, Meazza C, et al. (2003) Rhabdomyosarcoma in adults. A retrospective analysis of 171 patients treated at a single institution. Cancer 98: 571-580.