Obstetrics and Gynaecology Cases - Reviews
Liposarcoma of the Vagina
Mieczyslaw R. Gajda1*, Masoud Mireskandari1, Harald Winzer2, Herbert Diebolder2, Matthias Regensberger2, Ingo B. Runnebaum2 and Iver Petersen1
1Institute of Pathology, University Hospital Jena, Germany
2Department of Gynecology and Obstetrics, University Hospital Jena, Germany
*Corresponding author: Mieczyslaw Gajda, MD, Universit�tsklinikum Jena - Bachstrasse 18 - D-07743 Jena Die gesetzlichen Pflichtangaben finden Sie unter, Germany, E-mail: Mieczyslaw.Gajda@med.uni-jena.de
Obstet Gynecol Cases Rev, OGCR-2-046, (Volume 2, Issue 3), Case Report; ISSN: 2377-9004
Received: March 25, 2015 | Accepted: June 25, 2015 | Published: June 28, 2015
Citation: Gajda MR, Mireskandari M, Winzer H, Diebolder H, Regensberger M, et al. (2015) Liposarcoma of the Vagina. Obstet Gynecol Cases Rev 2:046. 10.23937/2377-9004/1410046
Copyright: © 2015 Gajda MR, et al This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Liposarcoma is the most common soft tissue sarcoma in adults. It typically occurs in retroperitoneum or extremities. However, this malignant tumor is very rare in the female reproductive system.
In this article we present detailed clinical and histopathologic features of a case with liposarcoma of vagina and review the literature on this theme using PUBMED database.
The tumor was presented as a rapidly growing mass in the vagina in a 50 year old woman. Pathological evaluation of the biopsy specimen showed the presence of a well differentiated liposarcoma. The tumor measured 13.6 x 10.4 x 6.4cm and was completely removed at operation. Histopathological evaluation of the resected vaginal tumor showed a dedifferentiated liposarcoma of the vagina. By our knowledge this is the first case report of a vaginal liposarcoma.
Introduction
Malignant vaginal tumors are essentially considered as infrequent gynecologic malignancies. The incidence of these tumors is not clearly known in Germany [1]. The sarcomas of vagina compose 2% of all detected malignancies in this area and are considered as rare tumors. The extremely rare sarcomas of vagina are fibrosarcoma, stromasarcoma, angioblastic endothelioma or malignant neurofibroma. Alveolar soft part sarcoma and synovial sarcoma of vagina are known only as isolated case reports [2-4].
Leiomyosarcoma is the most common sarcoma of vagina in adult females. They are detected first when they reach the size of 10 cm in largest dimension. The clinical manifestations are bloody discharge as well as urinary bladder and intestinal problems. The patients' age at the time of tumor detection varies between 31 and 69 years. The histologic features are similar to uterine leiomyosarcoma. Expectedly the low grade sarcomas have a better prognosis in compare with less differentiated ones. Since the radiation sensitivity is low, an operative management is necessary [5-7].
The dominant form of vaginal sarcoma in childhood and young adults is embryonal rhabdomyosarcoma (sarcoma botryoides, RMS). Up to 95% of RMS is detected in patients in first 5 years of life and the oldest reported patient was 21 years old. The tumor growths exophytically fills the vaginal space and produces a macroscopic appearance similar to bunches of grapes. These tumors grow rapidly, invade early in disease course the cervix, urinary bladder and urethra and metastasize through lymphatic and hematogenous routes. The histologic appearance of tumor can be in some areas unsuspicious. Accordingly the diagnosis of RMS has to be considered in any child with a polypoid vaginal tumor and these tumors should be analyzed completely [5,8].
Vaginal soft tissue tumors with lipoid differentiation are known only as case reports of single cases [9,10]. To our knowledge the present case is the first report of a vaginal liposarcoma.
Case Description
The 50 years old woman was admitted on 25.09.2008 because of an acute urinary retention. The patient said that she experienced an episode of urinary retention for the first time on 23.09.2008. She also said that she had on her 50th birthday about 4-6 weeks before the present admission problems with urination. She noticed voiding dysfunction with frequency and urging for urination even by small amount of urine. She reported no problem with defecation. The cystoscopic evaluations showed no pathologic changes. In urinary bladder there was about 1000 ml rest urine. The clinical neurologic examination at that time revealed no specific neurologic deficit. Over the course of time she developed a vaguely demarcated sensory deficit at the level of lower thoracic vertebrae as well as a bilateral Struempell sign and a left sided questionable Babinski sign.
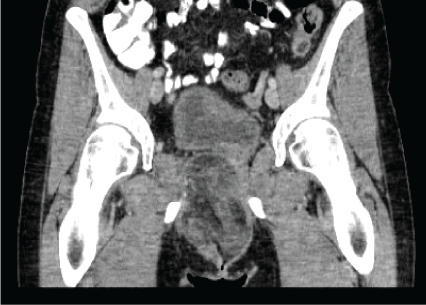
The cause of above mentioned symptoms was likely myelitis with accompanying central urinary bladder voiding dysfunction. The myelitis was suggested to be autoimmune or infectious/parainfectious due to a borreliosis infection with marginal IgM serum levels. In addition there was a vitamin B12 deficiency. This was followed by steroid therapy with administration of 1000mg Methylprednison over 5 days and substitution of vitamin B12. A sonographic examination at clinic for gynecology and obstetrics in Weimar revealed a 10 x 10cm large, inhomogeneous tumor in right paravaginal area. On 12.11.2008 an incisional biopsy was carried out. The specimen was composed of four yellow elastic to firm tissue fragments measured together 2.5 x 2.5 x 0.9cm. The first diagnosis was liposarcoma grade 2. According to the immunohistochemical findings (only focal positive reaction against S100-antibody and low proliferative activity in Ki67 immunostaining) the diagnosis of liposarcoma was revised and the specimen was sent to institute of pathology of university hospital Jena for consultation. The diagnosis of a well differentiated liposarcoma was established and the patient was operated in the clinic of gynecology of university hospital Jena. After five years of follow up no tumor recurrence has been detected.
Macroscopy
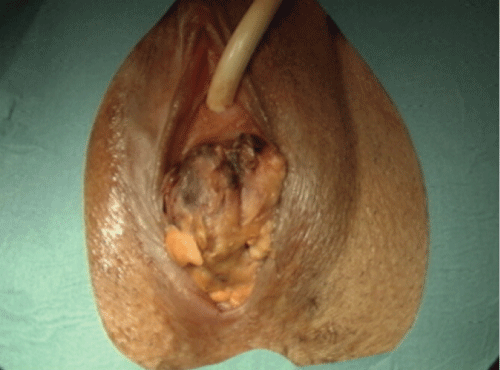
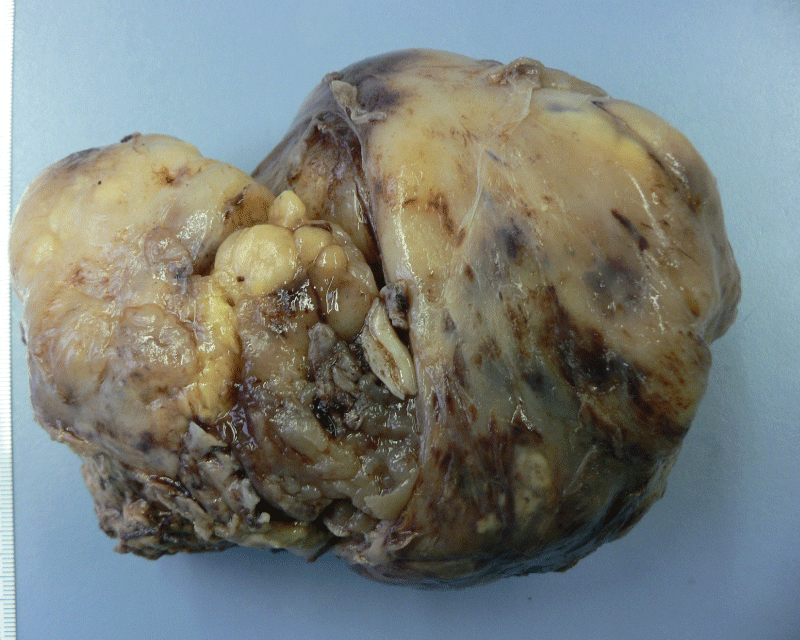
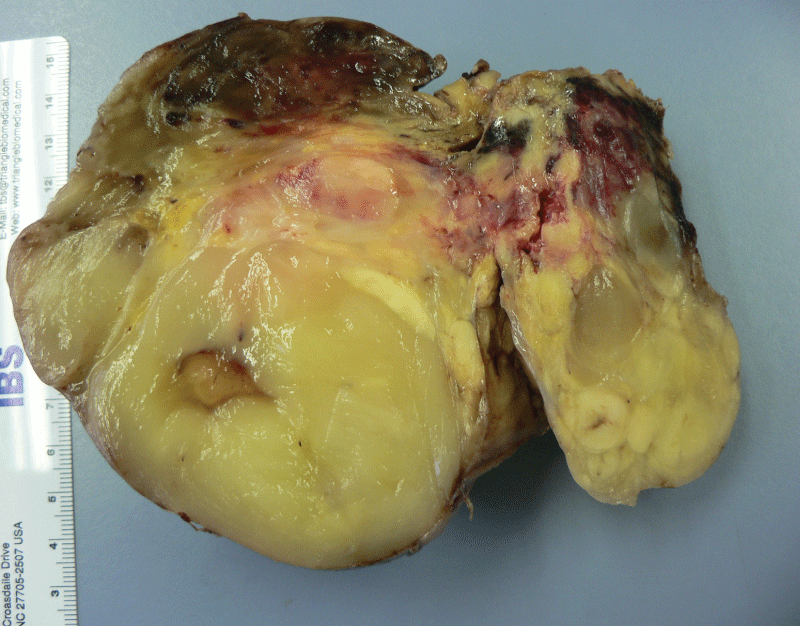
The tumor was lobulated, yellow to grey, focally covered by fibrotic capsule and measured 480g in weight and 13.6 x 10.4 x 6.4cm in dimensions. In serial sections the tumor was evidently lipomatous and showed yellow, glassy, multinodular and lobulated cut surface with large areas of haemorrhage (Figure 1A-1D).
Microscopy
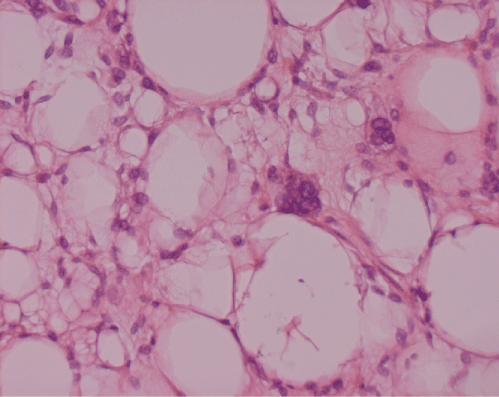
The microscopic evaluation revealed a predominantly spindle cell tumor. The tumor cell nuclei were basically small to medium sized. In some foci the large atypical and bizarre nuclei were detectable. In the background there was a fibrillary stroma with focal edema and hemorrhage. In addition within adipose tissue there were atypical tumor cells that displayed inclusion like intranuclear vacuoles as well as uni- and multivaculated cytoplasm. Focally regressive changes including edema, hemorrhage and small areas of necrosis were detectable. The inked tumor margin showed focally a covering of thin fibrous capsule (Figure 2,3).
.
Figure 2: Liposarcoma. Small to medium sized and focal bizarre nuclei. The tumor cells show nuclear vacuoles as well as uni- and multivacuolar cytoplasm. Inside the fatty tissue there are atypical cells at the edge of fatty vacuoles. H&E 200x.
View Figure 2
.
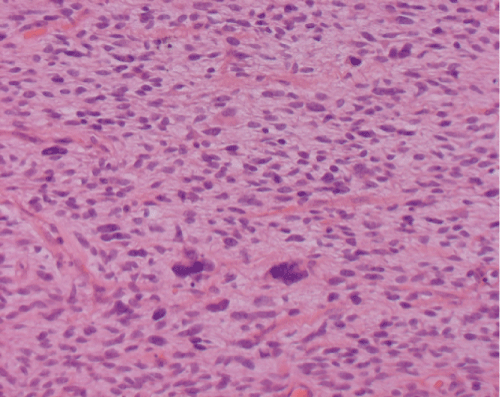
Figure 3: Liposarcoma. Spindle cell differentiation of tumor cells with scattered bizarre nuclei. H&E 200x
View Figure 3
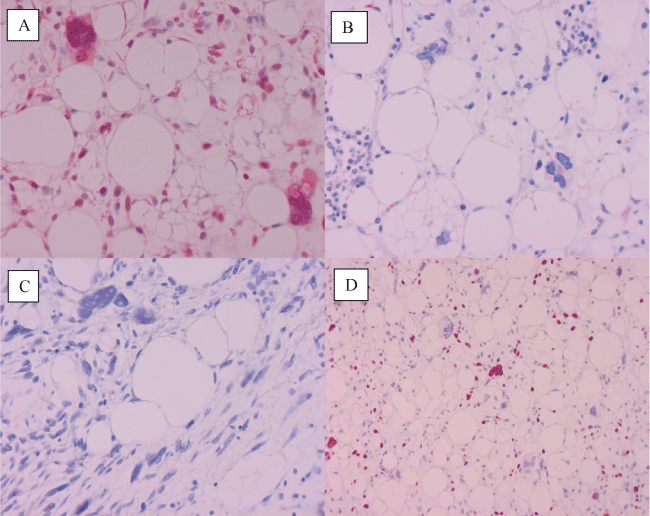
Immunohistochemically there was no clear expression of S100 as well as mdm-2 but a distinct and local nuclear CDK4 expression (Figure 4). A diagnosis of dedifferentiated liposarcoma grade 2 was established and the patient was handled with radiation of tumor resection bed.
.
Figure 4: Immunohistochemistry. A. Distinct positive reaction against CDK4, B. no reaction against mdm-2 and C. S100 200x. D. About 10% of nuclei of tumor cells show reaction against Ki67 100x.
View Figure 4
Discussion
Soft tissue sarcomas are rare tumors and constitute about 1% of all malignant neoplasms of adulthood. They can appear in any part of body [11-13].
Liposarcoma represents a relatively common malignant soft tissue tumor of adults and constitutes about 10-16% of these tumors. Most liposarcomas are located in lower extremities, trunk, shoulder and pelvic girdle, upper extremities and Retroperitoneum. This tumor happens indeed very rarely in female genital tract [14,15].
Liposarcomas are classified according to the WHO classification in the following groups: well differentiated, myxoid/round cell, dedifferentiated and pleomorphic. They display t(12;16) (q13;p11.2) [14,15].
The present case is a dedifferentiated liposarcoma of vagina grade 2. To our knowledge a liposarcoma of vagina has not been reported yet. Although there is some report of casuistic relationship between liposarcoma and lipoma, they are hardly separable solely based on clinical and medical imaging findings [14,15]. The differential diagnosis between atypical lipomatous tumors was discussed elsewhere [16].
According to the presenting symptoms this patient has received in the time of admission a urologic and not a gynecologic examination and was handled for her neurologic symptoms.
The local relapse rate is variable, generally is dependent on the anatomical localization of tumor and reaches the rate of 40-50% in visceral sarcomas [12,14]. The most frequent form of local relapse of tumor is detection of small satellite tumors near to the location of main tumor and is seen in 60% of cases. Accordingly a wide tumor excision with safe margins is a recommended approach even for vaginal sarcomas. In presented case the postoperative controls revealed no complication. Follow up of the patient by medical imaging showed no sign of local relapse after two years.
Enzinger reported local relapse of liposarcomas even after 30 years [14]. That means in comparison with carcinomas a markedly longer follow up control is needed.
The vaginal sarcomas are very rare. They have to be removed surgically. Despite a profuse blood and lymph vessel supply the distant metastases appear lately in the disease course. This finding supports again considering the surgical removal of the tumor as a preferred therapeutic approach.
References
-
Horn LC, Schierle K (2009) Pathologie der Pr�kanzerosen und der Karzinome von Vulva und Vagina sowie morphologische Prognosefaktoren. Onkologe 15: 15-27.
-
Norris HJ, Taylor HB (1966) Melanomas of the vagina. Am J Clin Pathol 46: 420-426.
-
Davos I, Abell MR (1976) Sarcomas of the vagina. Obstet Gynecol 47: 342-350.
-
Jellett H, Earl C (1904) Primary Sarcoma of the Vagina in the Adult, with the Notes of a Case. J Obstet Gynaecol 22: 222-235.
-
Eiermann W, Ataseven B, Ga� O (2013) Sarkome 509-524 in Die Gyn�kologie Kaufmann M, Costa SD, Scharl A.
-
Suh MJ, Park DC (2008) Leiomyosarcoma of the vagina: a case report and review from the literature. J Gynecol Oncol 19: 261-264.
-
Tavassoli FA, Norris HJ (1979) Smooth muscle tumors of the vagina. Obstet Gynecol 53: 689-693.
-
Shy SW, Lee WH, Chen D, Ho SY (1995) Rhabdomyosarcoma of the vagina in a postmenopausal woman: report of a case and review of the literature. Gynecol Oncol 58: 395-399.
-
Chen KT (1990) Angiomyolipoma of the vagina. Gynecol Oncol 37: 302-304.
-
Costantini E, Cochetti G, Porena M (2008) Vaginal para-urethral myxoid leiomyoma: case report and review of the literature. Int Urogynecol J Pelvic Floor Dysfunct 19: 1183-1185.
-
Fletcher CDM, Unni K, Mertens F (2002) World Health Organization Classification of Tumours: Pathology & Genetics of Tumours of the Soft Tissues and Bones. IARC Press: Lyon 2002.
-
Hoos A, Lewis JJ, Brennan MF (2000) Soft tissue sarcoma: prognostic factors and multimodal treatment. Chirurg 71: 787-794.
-
Miettinen MM (2003) Diagnostic Soft Tissue Pathology. Churchill Livingstone, New York, Edinburgh, London, Philadelphia.
-
Enzinger FM, Weiss SW (2001) Liposarcoma. In: Weiss SW, Goldblum JR, Enzinger FM. Enzinger and Weiss�s Soft Tissue Tumors. St Louis, Mosby: 641-693.
-
Evans HL (1988) Liposarcomas and atypical lipomatous tumours: a study of 66 cases followed for a minimum of 10 years. Surg Pathol 1: 41-54.
-
Gajda M, Hommann M, B�ttcher J, Henning K, Kaiser WA, et al. (2007) Primary liposarcoma of the liver--a rare mesenchymal tumor. Z Gastroenterol 45: 1241-1244.