Obstetrics and Gynaecology Cases - Reviews
Fertility Sparing Surgery for Management of Serous Cystadenoma: Surgical Technique and Follow Up
Islam Fahmi1,2, Mili Thakur3*, Ahmed Abdelaziz1,2, Mohammed Ashraf1,2 and Mostafa I. Abuzeid1,2
1Department of Obstetrics and Gynecology, Hurley Medical Center, USA
2Michigan State University College of Human Medicine, Flint Campus, USA
3Division of Reproductive Endocrinology and Infertility, Department of Obstetrics and Gynecology, Detroit Medical Center/Wayne State University, USA
*Corresponding author: Mili Thakur, MD, Division of Reproductive Endocrinology and Infertility, Department of Obstetrics and Gynecology, Detroit Medical Center/Wayne State University, 3990 John R. Street, Box 158, Detroit, Michigan 48201, USA, Tel: (313) 993-4049, E-mail: mthakur@med.wayne.edu
Obstet Gynecol Cases Rev, OGCR-2-044, (Volume 2, Issue 3), Case Report; ISSN: 2377-9004
Received: February 26, 2015 | Accepted: June 11, 2015 | Published: June 14, 2015
Citation: Fahmi I, Thakur M, Abdelaziz A, Ashraf M, Abuzeid MI (2015) Fertility Sparing Surgery for Management of Serous Cystadenoma: Surgical Technique and Follow Up. Obstet Gynecol Cases Rev 2:044. 10.23937/2377-9004/1410044
Copyright: © 2015 Fahmi I, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Ovarian cysts are commonly encountered adnexal masses by gynecologists, with a reported incidence of 5-15% of all reproductive age women. Large ovarian cysts are usually treated by surgical excision with cystectomy or oophorectomy. Laparoscopic ovarian cystectomy in large ovarian cysts has been underutilized. This report discusses the surgical technique of fertility sparing laparoscopic cystectomy for serous cystadenoma and subsequent follow up of these patients.
Cases: We present a series of three reproductive age women with large ovarian cysts where laparoscopic fertility sparing techniques were used for cystectomy with ovarian preservation. Pre-operative clinical, laboratory and ultrasonographic features did not show any signs of malignancy. Laparoscopic cystectomy was performed carefully with preservation of the ovary in all the cases. The abdominal cavity was inspected during the procedure and there were no signs of malignancy. Histopathological examination showed ovarian serous cystadenoma. No borderline tumors or malignancies were identified. The patients have been closely followed with no evidence of recurrence. Two of the women subsequently conceived using assisted reproductive techniques.
Conclusion: Laparoscopic fertility sparing ovarian cystectomy is safe and applicable to large ovarian cystic masses, which are presumed to be benign pre-operatively, such as ovarian serous cystadenomas. It should be considered as the preferred surgical approach for adolescents and young women for conservation of ovarian tissue.
Keywords
Large ovarian cysts, fertility sparing surgery, ovarian preservation, and serous cystadenoma.
Introduction
Ovarian cysts are commonly encountered adnexal masses by gynecologists, with a reported incidence of 5-15% of all reproductive age women [1,2]. An estimated 200, 000 women are admitted annually for benign ovarian cysts and this constitutes a third of admissions for gynecologic disease [3]. Benign ovarian cysts include physiologic ovarian cysts, corpus luteum cysts, endometriotic cysts, inflammatory cysts and benign ovarian neoplasms. Benign serous cystadenoma is the second most common benign primary ovarian tumor in women <50 years of age, benign cystic teratoma is the most common (66%) [4].
The symptoms caused by the cyst depend on its size, rate of growth and position in the pelvis. While small physiologic ovarian cysts are usually asymptomatic, common symptoms of ovarian cysts include abdominal and pelvic pain, dysmenorrhea, dyspareunia and bloating. Ultrasonography remains a valuable tool in differentiating benign from malignant ovarian cysts. Benign ovarian cysts are usually characterized by unilateral, mobile, smooth walled cystic masses with no solid areas or irregularities and absence of ascites. A combination of clinical impression, ultrasound features, age, menopausal status and level of biomarkers like CA-125 are used to discriminate between benign from malignant lesions [5].
Management of ovarian cystic masses is mandated when the cyst is symptomatic or there is a suspicion of malignancy (size larger than 6cm, elevated tumor markers or presence of solid component). The management depends on the age, tumor size, ultrasonographic features and intraoperative findings. Surgical excision with cystectomy or oophorectomy is usually performed. Laparoscopic technique has been shown to be safe for both ovarian cystectomy and oophorectomy [6,7]. However laproscopic cystectomy and oophorectomy are often underutilized due to concern for rupture of the cyst with tumor spill and limited workspace. Recent studies have also shown that there is evidence of decreased ovarian reserve following ovarian cystectomy [8,9]. Hence the optimal management of benign ovarian cysts including benign serous cystadenoma remains a subject of debate. This is especially true if the patient is young and fertility preservation is a concern [10].
We present 3 cases of serous cystadenoma where laparoscopic fertility sparing techniques were used. The article discusses the surgical technique and the follow up for these patients.
Cases
Case 1
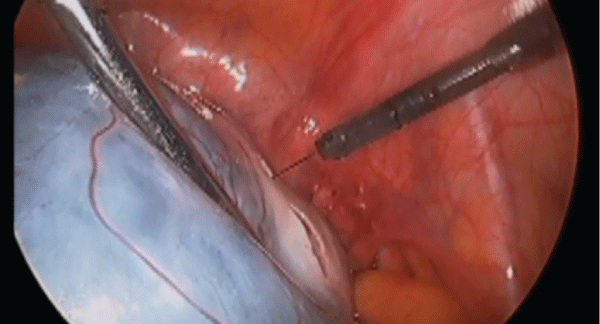
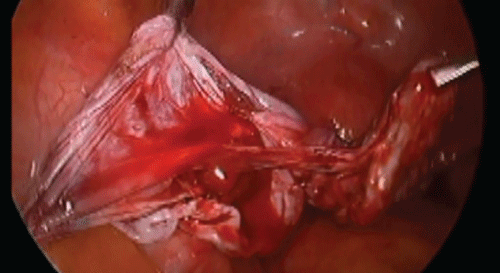
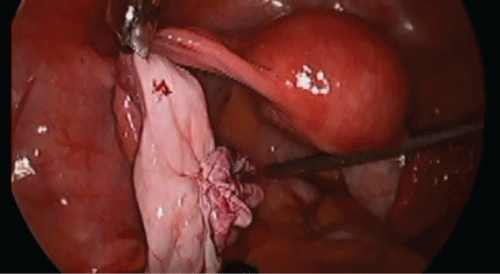
A 25-year-old nulliparous woman presented with intermittent abdominal pain. Transvaginal ultrasound (TVUS) showed a uni-locular, 10cm large left ovarian cyst with sonolucent content with a well-defined wall. All these characteristics were suggestive of a benign lesion. Tumor markers including cancer antigen 125 (CA-125), lactate dehydrogenase (LDH), beta human chorionic gonadotropin (bHCG) and alpha fetoprotein (AFP) were not elevated. Laparoscopic left ovarian cystectomy was performed. Using a monopolar diathermy needle tip an incision was made in the ovarian cortex (Figure 1). An attempt of ovarian cystectomy without opening the cyst wall was not successful. A clear serous fluid was seen coming from the cyst upon opening the cyst wall, so the decision was made to extend the incision to evacuate the fluid. The fluid was sent for cytology and cell block and was found to be negative for malignancy. A plane of cleavage was obtained separating the cyst from the ovarian tissue. Counter-traction was maintained using 2 atraumatic forceps while traction was obtained using a toothed forceps (Figure 2). The atraumatic forceps were repositioned every now and then, and the cyst wall was gently stripped from the underlying normal ovarian cortex (Figure 3). The ovarian incision was reapproximated with vertical mattress sutures using 4-0 Vicryl stitch with intracorporeal knots (Figure 4). The patient was followed up for 2 years with no evidence of recurrence. In this case, given the patient's young age, preservation of her ovarian function was maintained should she decide to have children in future.
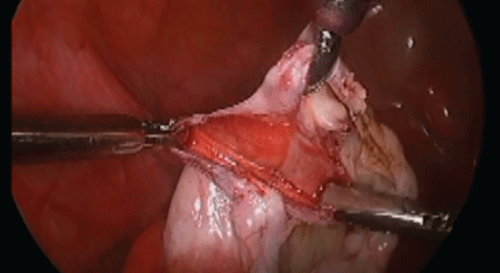
.
Figure 2: Traction-counter traction being used for separating the cyst wall from the ovarian cortex.
View Figure 2
Case 2
A 43-year-old nulliparous woman presented with primary infertility. The TVUS showed 6cm left ovarian cyst, endometrial polyp and possible adenomyosis. The cyst was uni-locular with sonolucent content and a well-defined wall; which were suggestive of a benign lesion. Tumor markers including CA-125, LDH, bHCG and AFP were not elevated. Patient underwent successful laparoscopic left ovarian cystectomy, right fimbrioplasty with tubal perfusion, hysteroscopic polypectomy and division of short septum. Cystectomy was performed using the same technique described in Case 1. The patient was able to conceive successfully after 15 months from the surgery, with the help of Assisted Reproductive Technology (ART) and delivered a healthy baby via Cesarean Section. This patient was followed up for 4 years and did not show any signs of recurrence.
Case 3
A 32-year-old nulliparous female presented with primary infertility. TVUS showed a 5cm right ovarian cyst, and small uterine fibroid versus adenomyosis. The ultrasonographic characteristics included: uni-locular cyst with sonolucent content and well defined edges; which were suggestive of a benign lesion. Tumor markers including CA-125, LDH, BHCG and AFP were not elevated. The patient underwent successful laparoscopic right ovarian cystectomy and left paratubal cystectomy, bilateral fimbrioplasty with tubal perfusion, hysteroscopy with dilatation and curettage. Cystectomy was performed using the same technique described in Case 1. On follow-up the patient was able to conceive successfully twice with the help of ART. The first pregnancy was conceived 2 months after surgery. She delivered a healthy baby via Cesarean Section in both pregnancies.
In all the three cases, the histopathological evaluation showed serous cystadenoma. None of them were a borderline tumor. The patients have been closely followed with TVUS with no evidence of recurrence.
Discussion
In this paper, we present 3 patients with large benign ovarian serous cystadenoma in which laparoscopic cystectomy with preservation of the ovary were performed. We demonstrate that laparoscopic fertility sparing procedures could be performed successfully with large ovarian cysts such as serous cystadenomas, providing ultrasound features suggest a benign nature. This is important in cases where ovarian preservation is required like in children, adolescents and young women.
Careful pre-operative evaluation of the mass is essential. Family history in combination with the sonomorphological features of an adnexal lesion is critical in management of ovarian masses. On TVUS assessment, simple ovarian cysts have a much lower risk of malignancy (0-0.8%) compared to cysts with solid parts (17-46%). [6,11]. Multilocular or multiple cysts, thick or irregular septa or walls, solid components, irregularities inside the cyst, mural nodules and echogenic elements should raise the suspicion of malignancy. Peripheral vascularization is more common in benign masses, whereas malignant tumors have more centrally located vessels. Multiparametric scoring systems combining morphologic and Doppler information have also been developed [12]. The risk of malignancy index that incorporates CA 125, ultrasound and menopausal status is the most widely used [5]. However no single test or scoring system exists so far that precisely differentiates between benign and malignant ovarian tumors in premenopausal women. [6].
Tumor markers, most importantly CA125, have also been used to discriminate benign ovarian cysts from malignant tumors. CA125 is a glycoprotein antigen, normally expressed in tissues derived from coelomic epithelia (ovary, fallopian tube, peritoneum, pleura, pericardium, colon, kidney, stomach). It is a well established tumor marker for advanced epithelial ovarian cancer, however an elevated level is more significant in predicting epithelial ovarian malignancy in a postmenopausal woman than in a premenopausal woman where other causes like pregnancy, endometriosis, fibroids and pelvic inflammatory disease could cause an increase [13].
If clinical, laboratory or radiological evaluation meets any of the criteria from the guidelines presented by American College of Obstetrics and Gynecologists [7], the patient should be referred to gynecologic oncologist. These include elevated CA125 (>200U/ml for premenopausal women and >35U/ml for postmenopausal women), ascites, evidence of abdominal and distant metastasis and family history of ovarian cancer in a first degree relative.
If the clinical impression and pre-operative evaluation indicates that the ovarian cyst is likely to be benign, the treatment will depend on the age of the patient, size of the lesion, patient's desire to preserve fertility, presenting symptoms and operative findings. When malignancy is not suspected prior to surgery or during the procedure, laparoscopic management of ovarian cysts has shown multiple advantages over laparotomy [14]. Laparoscopic surgery offers significant advantages such as reduced hospital stay, less adverse effects, better quality of life, and superior visualization [15]. The concerns with performing a laparoscopic surgery for ovarian masses is risk of rupture and spillage of the contents of the cyst due to limited workspace and need for a secondary surgery if ovarian malignancy is diagnosed. In a study in which 1128 adnexal masses were resected and 13 patients (1.5%) were found to have unexpected ovarian malignancies, the presence of an early-stage unexpected ovarian malignancy did not alter patient prognosis [16]. Due to cyst rupture during surgery, nine (69.2%) of these patients were upgraded to tumor stage IC [16].
In young patients where fertility is a concern, careful weighing of the risks and benefits of surgical management of ovarian cysts is warranted. Evidence suggests that removal of the ovarian cyst reduces ovarian reserve and adversely affects fertility [10]. Studies have shown decrease in anti-mullerian hormone after surgical excision of both endometriotic and non-endometriotic ovarian cysts [8,9,11]. Conservative management for small ovarian cysts that are asymptomatic is reasonable. The surgical technique has been shown to play an important role in preserving ovarian function during surgical management of ovarian masses.
The surgical technique that we described in our patients used microsurgical principles and minimal trauma to the ovarian cortex with every effort to minimize bleeding from the ovarian cortex. The latter is extremely important to avoid using methods to control bleeding such as monopolar cautery, bipolar cautery, defocused CO2 laser or argon beam coagulation because it can cause damage to ovarian cortex and compromise ovarian reserve.
The follow up of our patients up to 2-4 years did not show any evidence of recurrence. Two of them were able to achieve pregnancy while one of them was not trying to conceive to date.
Alternative surgical techniques other than excision have been described for endometriomas only, such techniques include cyst aspiration and sclerotherapy or vaporization of the cyst wall [10]. Some studies revealed lower recurrence rates for sclerotherapy when compared to aspiration [17]. When comparing excision with laser vaporization, studies have shown similar pregnancy rates with less recurrence after excision [18]. When plasma vaporization was used, another study revealed less incidence of decreased of ovarian reserve [19]. However there is not enough data to recommend one surgical technique versus another. None of these alternative techniques are recommended when serous cystadenoma is suspected because complete excision is mandatory to minimize recurrence and to ensure accurate pathological assessment to rule out malignancy.
In conclusion, laparoscopic fertility sparing ovarian cystectomy is safe and effective technique in patients presenting with large benign ovarian serous cystadenomas. Careful pre-operative evaluation of ovarian masses is imperative for fertility sparing approach to management. In order to preserve maximum ovarian function the surgeon should utilize microsurgical techniques, carefully preserving as much of the ovarian parenchyma while stripping the cyst wall achieving hemostasis with minimal use of coagulation.
References
-
Millar DM, Blake JM, Stringer DA, Hara H, Babiak C (1993) Prepubertal ovarian cyst formation: 5 years' experience. Obstet Gynecol 81: 434-438.
-
D�rum A, Blom GP, Ekerhovd E, Granberg S (2005) Prevalence and histologic diagnosis of adnexal cysts in postmenopausal women: an autopsy study. Am J Obstet Gynecol 192: 48-54.
-
Velebil P, Wingo PA, Xia Z, Wilcox LS, Peterson HB (1995) Rate of hospitalization for gynecologic disorders among reproductive-age women in the United States. Obstet Gynecol 86: 764-769.
-
Koonings PP, Campbell K, Mishell DR Jr, Grimes DA (1989) Relative frequency of primary ovarian neoplasms: a 10-year review. Obstet Gynecol 74: 921-926.
-
Jacobs I, Oram D, Fairbanks J, Turner J, Frost C, et al. (1990) A risk of malignancy index incorporating CA 125, ultrasound and menopausal status for the accurate preoperative diagnosis of ovarian cancer. Br J Obstet Gynaecol 97: 922-929
-
Djukic M, Stankovic Z, Vasiljevic M, Savic D, Lukac B, et al. (2014) Laparoscopic management of ovarian benign masses. Clin Exp Obstet Gynecol 41: 296-299.
-
Agarwal P, Agarwal P, Bagdi R, Balagopal S, Ramasundaram M, et al. (2014) Ovarian preservation in children for adenexal pathology, current trends in laparoscopic management and our experience. J Indian Assoc Pediatr Surg 19: 65-69.
-
Chen Y, Pei H, Chang Y, Chen M, Wang H, et al. (2014) The impact of endometrioma and laparoscopic cystectomy on ovarian reserve and the exploration of related factors assessed by serum anti-Mullerian hormone: a prospective cohort study. J Ovarian Res 7: 108.
-
Jang WK, Lim SY, Park JC, Lee KR, Lee A, et al. (2014) Surgical impact on serum anti-M�llerian hormone in women with benign ovarian cyst: A prospective study. Obstet Gynecol Sci 57: 121-127.
-
Legendre G1, Catala L2, Morini�re C2, Lacoeuille C2, Boussion F2, et al. (2014) Relationship between ovarian cysts and infertility: what surgery and when? Fertil Steril 101: 608-614.
-
Amooee S, Gharib M, Ravanfar P (2015) Comparison of anti-mullerian hormone level in non-endometriotic benign ovarian cyst before and after laparoscopic cystectomy. Iran J Reprod Med 13: 149-154.
-
Kaijser J, Bourne T, Valentin L, Sayasneh A, Van Holsbeke C, et al. (2013) Improving strategies for diagnosing ovarian cancer: a summary of the International Ovarian Tumor Analysis (IOTA) studies. Ultrasound Obstet Gynecol 41: 9-20.
-
Moss EL, Hollingworth J, Reynolds TM (2005) The role of CA125 in clinical practice. J Clin Pathol 58: 308-312.
-
Medeiros LR, Stein AT, Fachel J, Garry R, Furness S (2008) Laparoscopy versus laparotomy for benign ovarian tumor: a systematic review and meta-analysis. Int J Gynecol Cancer 18: 387-399.
-
Grammatikakis I, Trompoukis P, Zervoudis S, Mavrelos C, Economides P, et al. (2015) Laparoscopic treatment of 1522 adnexal masses: an 8-year experience. Diagn Ther Endosc 2015: 979162.
-
Matsushita H, Watanabe K, Yokoi T, Wakatsuki A (2014) Unexpected ovarian malignancy following laparoscopic excision of adnexal masses. Hum Reprod 29: 1912-1917.
-
Marana R, Caruana P, Muzii L, Catalano GF, Mancuso S (1996) Operative laparoscopy for ovarian cysts. Excision vs. aspiration. J Reprod Med 41: 435-438.
-
Carmona F, Martinez-Zamora MA, Rabanal A, Martinez-Roman S, Balasch J (2011) Ovarian cystectomy versus laser vaporization in the treatment of ovarian endometriomas: a randomized clinical trial with a five-year follow-up. Fertil Steril 96: 251-254.
-
Roman H, Auber M, Mokdad C, Martin C, Diguet A, et al. (2011) Ovarian endometrioma ablation using plasma energy versus cystectomy: a step toward better preservation of the ovarian parenchyma in women wishing to conceive. Fertil Steril 96: 1396-1400.