Obstetrics and Gynaecology Cases - Reviews
Case Report on a 10cm Pelvic Mass: Unruptured Chronic Ectopic versus Neoplasm
Christine Rojas*, Kerry Ann Hudson and Kevin Byrd
Naval Medical Center Portsmouth, USA
*Corresponding author: Christine Rojas, CAPT, USAF, MC, Naval Medical Center Portsmouth, 620 John Paul Jones Circle, Portsmouth, Virginia 23708, USA, Tel: (757) 953-1817, E-mail: christine.rojas2.mil@mail.mil
Obstet Gynecol Cases Rev, OGCR-2-033, (Volume 2, Issue 2), Case Report; ISSN: 2377-9004
Received: March 13, 2015 | Accepted: April 12, 2015 | Published: April 14, 2015
Citation: Rojas C, Hudson KA, Byrd K (2015) Case Report on a 10cm Pelvic Mass: Unruptured Chronic Ectopic versus Neoplasm. Obstet Gynecol Cases Rev 2:033. 10.23937/2377-9004/1410033
Copyright: © 2015 Rojas C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Ectopic pregnancy is the leading cause of maternal death in the first trimester. There is no correlation between serum β-hCG levels, mass size and tubal rupture.
Case: A 28-year-old G3P1 presented after elective surgical termination of a 5-week gestation with right pelvic pain and β-hCG of 80mIU. Imaging revealed a 10cm adnexal mass and serum cancer antigen 125 was 44IU/mL. Exploratory laparotomy and right salpingo-oopherectomy were performed revealing no hemo peritoneum, extensive adhesive disease and a 10 centimeter hematosalpinx. Pathologic diagnosis was consistent with products of conception.
Conclusion: Ectopic pregnancy should be considered in the differential diagnosis of a fertile female presenting with a large adnexal mass, irrespective of elevated tumor markers.
Introduction
Ectopic pregnancy is the leading cause of maternal death in the first trimester. Approximately 18% of ectopic pregnancies present to the emergency department with vaginal bleeding, abdominal pain or both [1]. The diagnosis of an ectopic pregnancy is based on the correlation of clinical signs, physical symptoms, serum β-hCG and ultrasonography. Despite the high sensitivity of ultrasonography in the detection of ectopic pregnancies, the presence of a large adnexal mass may pose challenges in determining whether the mass is an ectopic pregnancy versus neoplasm. A chronic ectopic may present as a large, unruptured mass that consists of multiple small hemorrhages into the peritoneal cavity with the formation of a large hematosalpinx [2]. A chronic ectopic pregnancy may have less acute symptoms. We present an unusual chronic ectopic pregnancy presenting as a 10cm unruptured adnexal mass with a low serum β-hCG level.
Case
A 28-year-old, gravida 3 para 1, presented to an outside facility complaining of new onset of right pelvic cramping and a positive urine pregnancy test. Thirty days prior, she had undergone an uncomplicated elective surgical termination of a 5-week gestation. Her obstetrical history was notable for one uncomplicated vaginal delivery, one spontaneous abortion and the recent elective termination. Her last menstrual cycle had been two months prior to presenting to the gynecologist. She had no history of irregular menstrual cycles, pelvic inflammatory disease or endometriosis.
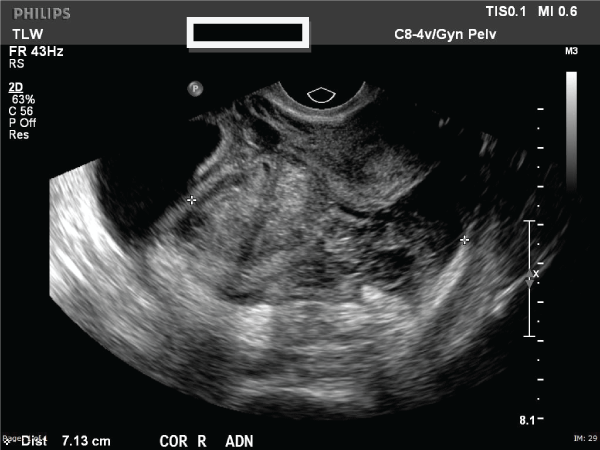
At presentation, her vital signs were unremarkable and she was alert and in no acute distress. On physical examination, her abdomen was soft, non-distended with mild tenderness in the right lower quadrant. Her laboratory evaluation was remarkable for a serum β-hCG of 80mIU, hemoglobin of 9.4g/L and hematocrit of 28.9%. Ultrasonography revealed a 10cm adnexal mass of unknown etiology and small free fluid collection in the lower pelvis (Figure 1). The mass was noted to be heterogenous, multilobulated and multicystic in nature. Computed tomography revealed no evidence of metastatic disease. Hence, a serum cancer antigen 125 level was measured and found to be 44IU/mL. The patient was transferred to our institution for concerns of neoplastic etiology of this adnexal mass. Upon arrival, she continued to be hemodynamically stable and was admitted to the Gynecology ward and consented for diagnostic laparoscopy, possible right salpingo-oopherectomy, removal of adnexal mass, possible laparotomy and other indicated procedures with both Gynecologic Oncology and Pathology available for expected intraoperative consultation. In the operating room, diagnostic laparoscopy revealed extensive adhesions of bowel loops to the anterior and lateral abdominal wall, obscuring the pelvis. Based on the extensive adhesive disease, the decision was made to proceed with exploratory laparotomy via a midline vertical incision. After abdominal adhesioloysis was performed, a 10x6cm unruptured right hematosalpinx was exposed and a right salpingo-oopherectomy was performed in order to remove the mass in its entirety (Figure 2). The specimen was sent for frozen section analysis and was noted to be consistent with products of conception, thus confirming the diagnosis of ectopic pregnancy. Her postoperative course was unremarkable. Eight weeks postoperatively, the patient�s β-hCG was negative and she had a normal pelvic examination.
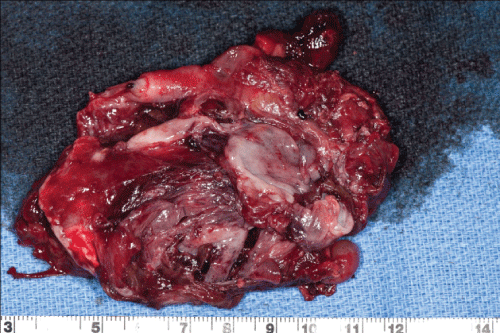
.
Figure 2: Right salpingo-oopherectomy specimen sent for frozen section analysis and confirmed to be an ectopic pregnancy
View Figure 2
Comment
This case presents an interesting diagnostic dilemma with a large adnexal mass in the setting of a low serum β-hCG and elevated CA-125. Furthermore, an accurate diagnosis can be challenging since it relies on the combination of ultrasonography and serial β-hCG [3]. Given the recent elective pregnancy termination, many would be tempted to eliminate ectopic pregnancy from the differential diagnosis. It is uncertain if this ectopic pregnancy was the initial pregnancy that was treated with elective termination unsuccessfully or if it was a subsequent pregnancy. Additionally, while uncommon, the possibility of an initial heterotopic pregnancy cannot be excluded. In this case, the patient�s records from the outside provider who performed the surgical termination were not available. Subsequently, this led to a strong suspicion of ectopic pregnancy because available documentation of an initial intrauterine pregnancy was not present.
The diagnosis in this case was further complicated by lack of radiologic features common to ectopic pregnancies diagnosed on ultrasound such as peripheral blood flow or the presence of a gestational sac, yolk sac, or fetal pole. Based on a systematic review of identification of women having ectopic pregnancies, transvaginal sonography was the single best diagnostic modality for detecting ectopic pregnancy[4]. Of the 14 studies, the authors noted the sensitivity of transvaginal sonography to detect ectopic pregnancy was 0.88 (95% CI, 0.52-0.98). Furthermore, the absence of adnexal findings had a summary likelihood ratio of 0.12 (9%% CI, 0.03-0.55) [4]. Our patient did not initially present with an acute abdomen or peritoneal signs, again making it difficult to evaluate for the acuity of the patient�s status. In addition, there were no clear ultrasound findings to suggest an ectopic pregnancy. The prompt identification and diagnosis of women who may have an ectopic pregnancy is critical for reducing maternal morbidity and mortality [3].
There was a similar case previously reported. Nacharaju et al. published a case of a 22-year-old woman with a 2 month history of irregular spotting and normal abdominal examination that consequently had an 8x6cm hematosalpinx with pathology confirming ectopic pregnancy [2]. A hematosalpinx is defined as bleeding into the fallopian tubes. It is rare for a chronic ectopic pregnancy to present as a hematosalpinx. Similarly, our patient had a benign abdomen with a large unruptured chronic ectopic pregnancy. Upon review of the literature, there are few case reports regarding chronic ectopic pregnancies presenting as a large unruptured hematosalpinx [2]. Daniilidis et al. presented a unique case of a ruptured ectopic pregnancy describing a case of a 36-year-old woman with β-hCG measurement of 13nIU/mL [3]. A negative pregnancy test via urine or low β-hCG in serum is 3.1% and 2.6% respectively in ectopic pregnancies [3]. This emphasizes the importance that the β-hCG value does not correlate to either the size of the ectopic adnexal mass or whether the ectopic pregnancy is ruptured or not. Daniilidis et al. reported a hypothesis that may contribute to ectopic pregnancies in the setting of a low β-hCG. One theory may be related to the reduction or cessation of production of the degenerate trophobloastic tissue or the existence of low mass chorionic villi which produce this hormone and their increased clearance from the circulation[3].
The diagnosis of ectopic pregnancy is challenging especially when the β-hCG is low and the ultrasound is not indicative of an ectopic pregnancy. Additionally, the elevated serum cancer antigen 125 noted in our case is not surprising since pregnancy leads to falsely elevated tumor maker values. Our case emphasizes the importance of considering an ectopic pregnancy in the differential diagnosis of a fertile female presenting with a large adnexal mass. As described by previous reports, the symptoms and signs of a chronic ectopic pregnancy are not classical[2]. This presents a challenge for physicians attempting to rapidly identify and accurately diagnose this condition. Additionally, the surgical management is further challenging due to the chronic inflammation resulting in significant adhesions. Timely diagnosis using the combination of laboratory evaluation and imaging along with prompt treatment is essential for achieving excellent maternal outcomes.
Copyright statement
I am a military service member and an employee of the U.S. Government. This work was prepared as part of my official duties. Title 17 U.S.C. 105 provides that 'Copyright protection under this title is not available for any work of the United States Government.' Title 17 U.S.C. 101 defines a United States Government work as a work prepared by a military service member or employee of the United States Government as part of that person's official duties.
Disclaimer statement
The views expressed in this article are those of the author(s) and do not necessarily reflect the official policy or position of the Department of the Navy, Department of Defense or the United States Government.
References
-
American College of Obstetricians and Gynecologists (2008) ACOG Practice Bulletin No. 94: Medical management of ectopic pregnancy. Obstet Gynecol 111: 1479-1485.
-
Nacharaju M, Vellanki VS, Gillellamudi SB, KothaVK, Alluri A (2014) A rare case of chronic ectopic pregnancy presenting as large hematosalpinx. Clin Med Insights Reprod Health 8: 1-4.
-
Daniilidis A, Pantelis A, Makris V, Balaouras D, Vrachnis N (2014) A unique case of ruptured ectopic pregnancy in a patient with negative pregnancy test- a case report and brief review of the literature. Hippokratia 3: 282-284.
-
Crochet JR, Bastian LA, Chireau MV (2013) Does this woman have an ectopic pregnancy?: the rational clinical examination systematic review. JAMA 309: 1722-1729.