Obstetrics and Gynaecology Cases - Reviews
Hybrid Arc Stereotactic Ablative Body Radiation Therapy for Pelvic Relapse of Gynecologic Malignancies
Charles A Kunos*, Howard Shaffer and Jeffrey M Fabien
Department of Radiation Oncology, Summa Cancer Institute, USA
*Corresponding author: Charles A Kunos, MD, PhD, Department of Radiation Oncology, Summa Cancer Institute, 161 North Forge Street, Akron, Ohio, USA, Tel: 330-375-3557, Fax: 330-375-3072, E-mail: kunosc@summahealth.org
Obstet Gynecol Cases Rev, OGCR-2-030, (Volume 2, Issue 2), Case Report; ISSN: 2377-9004
Received: March 12, 2015 | Accepted: March 28, 2015 | Published: March 30, 2015
Citation: Kunos CA, Shaffer H, Fabien JM (2015) Hybrid Arc Stereotactic Ablative Body Radiation Therapy for Pelvic Relapse of Gynecologic Malignancies. Obstet Gynecol Cases Rev 2:030. 10.23937/2377-9004/1410030
Copyright: © 2015 Kunos CA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Relapsed gynecologic cancers aredifficult to control in the pelvis, especially when surgery, chemotherapy and radiation treatments have already been administered. For this clinical scenario, stereotactic body radiation therapy has emerged as a meaningful treatment strategy. The new Vero stereotactic body radiation therapy system uses coplanar and noncoplanar radiation treatment beams with submillimeter precision to treat cancer targets. This study describestheinitial clinical experience with Vero hybrid arc stereotactic ablative body radiation therapy to treat relapsed gynecologic cancers detected in the pelvis.
Keywords
Vero, Radiosurgery, Stereotactic body radiation, Hybrid arc, Cervical cancer, Endometrial cancer
Introduction
Bulky pelvic relapses of gynecologic cancers mightproducefoul-smelling vaginal secretions and bleeding, pelvic pain, dysuria, or bowel obstruction [1]. Clinical management of these symptoms remains a challenge without control of the pelvic disease, especially when consideringits proximity to the bowel and the bladder. Moreover, previoussurgical and chemotherapy assertivenessand any prior pelvic radiation dose confound management of bulky pelvic relapses after primary cancer intervention [1].
One method of controlling relapsed gynecologic cancer in the pelvis is a potentially morbid surgery, the so-named pelvic exenteration [2,3]. For patients that would otherwise require exenteration, stereotactic ablative body radiation therapy (SBRT) has emerged as a non-invasive precise radiation treatment. In a phase II clinical trial, robotic SBRT demonstrated a 96 percent abdominopelvic disease target control ratewithout undo normal organ injury(4).Robotic SBRT involved image-guided �pencil beam-sized� radiation beams delivering a hypofractionated radiation dose (8 Gy X 3 consecutive daily fractions) [4]. Modern SBRT delivery systems mount a clinical radiation accelerator either to an industrial robotic arm [5], orto a helical slice-by-slice gantry [6], or within a conventional machine but have it driven by image-guided intensity modulated radiation therapy or dynamic arc delivery software [7]. Recently, a first-in-class SBRT delivery system has come to market, the Vero SBRT system [8-10].
The Vero SBRT system uses agimbaled (�4cm) pan-and-tilt radiation accelerator, whose sixty110-millimeter tall tungsten alloy leaves fashion a radiation beam for a very narrow radiation field penumbra. Dual-diagnostic Exactrac kV x-ray units and an infrared camera unitallow for�between-beam� feedback of cancer target abdominopelvic motion. A robotic pivoting O-ring (�60o) and rotational gantry (�185o) permit coplanar and non-coplanar unique treatment degrees of freedom for static and rotational arc radiation beams. In spite of all of these mechanical manipulations, Vero SBRT has submillimeter isocenter accuracy (0.4mm) [11]. No prior studies describe Vero hybrid arc SBRT to treat relapsed gynecologic cancers in the pelvis. Here, we report the initial case series experience.
Materials and Methods
Stereotactic ablative body radiation therapy
Between November 2014 and January 2015, three consecutive patients underwent hybrid arc SBRT using the Vero SBRT platform (Brainlab, Inc., Munich, Germany; Mitsubishi Heavy Industries Ltd., Tokyo, Japan) for treatment of gynecologic cancer relapses occurring in the pelvis not amenable to surgical or conventional radiation intervention. All patients underwent therapy at Summa Health System Akron City Hospital (Akron, Ohio, USA). With permission from the Summa Health System institutional review board, we conducted a retrospective case series analysis of Vero hybrid arc stereotactic body radiation therapy applied to the pelvis.
After consultation discussing surgical and non-surgical palliative treatment strategies, all three patients elected and consented to Vero stereotactic body radiation therapy. Patients underwent one to three gold-coated metallic fiducial marker placement within or around relapsed pelvic cancer targets [1]. Patients then had supine computed tomography (CT) scans with two-pin localizing, pelvic immobilization. Images were acquired as a non-contrasted contiguous helical axial CT scan with three-millimeter slice thickness (voltage 120 kVp, 350 mAs) and were transferred to the iPlan treatment planning system (Brainlab, Inc.). 2-[18F] fluoro-2-deoxy-D-glucose (18F-FDG) positron emission tomography (PET) images if any were obtained per institutional routine and were transferred into the planning system for enhanced tumor target contouring similar to previous experience [12]. The treating radiation oncologist contoured the relapsed pelvic cancer targets and occult at-risk tissue, labeled as the clinical target volume (CTV). If acquired, a thresholded 40 percent maximum standard uptake value contour on the 18F-FDG PET images created an PET clinical target volume (CTVpet) [12]. If a CTV and a CTVpet were contoured, then both volumes were combined into a single composite volume (CTV+CTVpet). The CTV or CTV+CTVpet volumes were expanded uniformly by five millimeters to generate a planning tumor volume (PTV). Normal tissue small bowel, rectum, bladder, bilateral kidneys, bilateral proximal femurs, and sacral foraminae (as surrogates for nerve root paths) were contoured most often for radiation dosimetry planning. Vero hybrid arc stereotactic body radiation therapy (Figure 1) was prescribed as 8 Gy per fraction for three fractions [4].
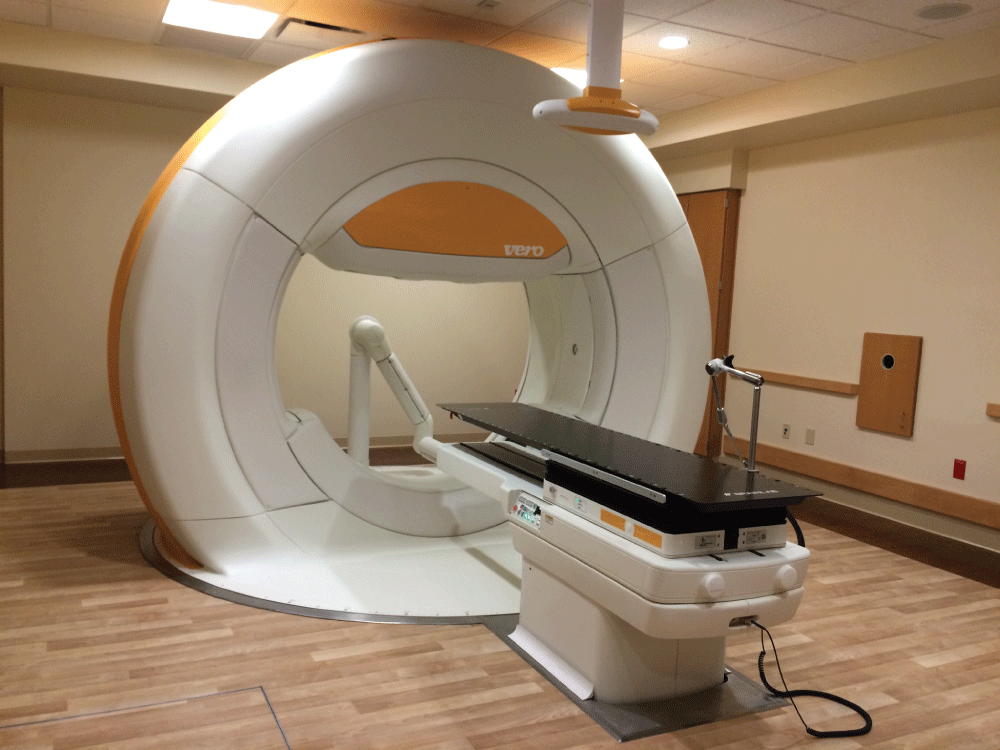
Figure 1: The Vero SBRT system
View Figure 1
Prior to radiation delivery, the treating radiation therapists verified gantry rotation and O-ring pivot position clearance of the patients. During Vero hybrid arc stereotactic body radiation therapy delivery, the treating radiation oncologist verified positional accuracy of soft tissue fiducial markers (i.e., the relapsed pelvic cancer target) using cross-plane Exactrac kV x-ray prior to any beam arc or static beam.
Toxicity assessments
Toxicity was assessed prior to therapy on the first day of treatment, the last day of treatment, and four weeks after treatment. Toxicity was graded following National Cancer Institute common terminology criteria for adverse events (CTCAE) version 4. For this study, toxicity data was compiled retrospectively at chart review.
Results
Case reports
Case 1: A 67-year-old gravida 0, para 0 woman diagnosed with FIGO stage IB, grade 1endometrioid adenocarcinoma of the uterus underwent definitive four-field pelvic radiation to a total dose of 50.4 Gy in 28 fractions in June 2009. A single brachytherapy application of 6.3 Gy was delivered in July 2009. No surgery was done. She had no clinical evidence of disease for 5 years, but had lingering back pain requiring anti-inflammatory and opioid pain management.
In November 2014, she developed a 5 cm non-operable central vaginal apex mass intimately associated with the rectum and fixed to the pelvic floor.Interstitial brachytherapy was not technically feasible given the close proximity of her relapsed mass and rectum. Surgical resection was not advised given adherence of the relapsed mass to the pelvic floor and given the associated surgical morbidity risk. Given her desire for treatment and a recommendation for stereotactic body radiation therapy from a gynecologic oncology tumor board, she elected and consented to SBRT treatment in late November 2014. After written informed consent, she had one gold-coated fiducial marker placed by the treating radiation oncologist within the relapsed vaginal apex mass under 2% topical lidocaine anesthesia. Non-contrasted computed tomography simulation was done seven days afterward. The patient was unable to tolerate an 18-FDG PET scan in a protracted supine position.
A PTV of 257cm3 received 24 Gy in three fractions of 8 Gy prescribed to the 100% isodose line with a conformality index of 1.04 to achieve 95% target coverage. Twonon-coplanar hybrid dynamic arcseach withsevenintegrated 6MV intensity modulated radiation therapy static photon beams were used. Fiducial marker tracking was done each before the arc and before the static field group. During her fractionated SBRT course, she developed no significant skin, urinary, or gastrointestinal toxicities.At four-week follow-up, she had no pelvic bleeding, pelvic pain, or other symptomatic complaints.
She remains alivethree months after Vero hybrid arc stereotactic body radiation therapy without symptoms or clinical pelvic disease progression.
Case 2: A 66-year old gravida 2, para 2 woman had a stage IB, grade 2endometrioid adenocarcinoma of the uterus diagnosed inSeptember 2012. She underwent laparoscopic-assisted total hysterectomy and bilateral salpingo-oophorectomy with lymph node sampling in October 2012. Intravaginal brachytherapy was administered to the proximal four centimeters of the vagina for a dose of 21 Gy in three weekly fractions. She completed therapy in December 2012.
In June 2014, she had recurrent disease detected in the left (5 centimeters) and right (2 centimeters) vaginal apices on pelvic examination and CT imaging. Rather than pelvic exenteration, she elected palliative four-field pelvic radiation and completed a course of 45 Gy in 25 fractions in July 2014. Posttherapy surveillance pelvic examination and CT imaging confirmed a partial response to therapy in December 2014.
At this time, a treatment recommendation for SBRT was made and agreedat a gynecologic oncology tumor board. Palliative treatment options were presented to the patient in December 2014. She agreed to the recommended SBRT treatment and signed informed consent. She had single fiducial markers placed by the treating radiation oncologist into eachof the two vaginal masses under 2% topical lidocaine anesthesias in December 2014. Non-contrasted computed tomography simulation was done two days after fiducial marker placement.
A PTV of 255cm3 received 24 Gy in three fractions of 8 Gy prescribed to the 100% isodose line with a conformality index of 1.06. Ninety percent PTV target coverage was achieved. Onehybrid dynamic arc with seven integrated 6MV intensity modulated radiation therapy static photon beams were utilized in the radiation plan. Fiducial marking tracking was done before the arc and before the static field group.Overher SBRT course, she complained of no skin, urinary, or gastrointestinal adverse events. At her four-week follow-up, she reported grade 2 fatigue and a urinary tract infection, both of which did not limit her activities.
She remains alivethree months after Vero hybrid arc stereotactic body radiation therapy. Her cancer therapy treatment plan with her gynecologic oncologist includes consideration of post-SBRT systemic chemotherapy.
Case 3: A 34-year old gravida 1, para 1 woman had a stage IB1, grade 2 adenocarcinoma of the uterine cervix first diagnosed in June 2012. She underwent robotic-assisted total hysterectomy and bilateral salpingo-oophorectomy with lymph node sampling in August 2012. Specimen histopathology identified a two-centimeter adenocarcinoma with deep stromal invasion and lymphovascular invasion. Surgical margins were negative. Thirty-four pelvic and low para-aortic lymph nodes were negative for malignancy. She underwent adjuvant intensity modulated radiation therapy to the pelvis to a total dose of 46.8 Gy in 27 fractions. No brachytherapy was administered. She completed radiation therapy in January 2013.
In February 2014, she had recurrent disease detected in the right vaginal apex on pelvic examination. Rather than undergo pelvic exenteration, she elected to receive multiple cycles of bevacizumab, cisplatin, and paclitaxel chemotherapy. Post-chemotherapy surveillance pelvic examination and imaging confirmed a near complete response in July 2014. In December 2014, surveillance 18-FDG PET scan detected a four-centimeter right pelvic sidewall mass encasing the right ureter (SUV maximum 14). A treatment recommendation for stereotactic body radiation therapy was made the same month at a multidisciplinary gynecologic oncology tumor board. Palliative treatment options were presented to the patient in late December 2014. She agreed to therapy and signed informed consent for SBRT. An interventional radiologist placed three fiducial markers within the right pelvic sidewall mass in late December 2014. Non-contrasted computed tomography simulation was done two days after fiducial marker placement. Her already acquired surveillance 18-FDG PET scan was overlaid on simulation images for SBRT dosimetry planning.
A tumor volume of 84cm3 received 24 Gy in three fractions of 8 Gy prescribed to the 100% isodose line with a conformality index of 1.25. 95% target coverage was reached. One hybrid dynamic arc and seven integrated 6MV intensity modulated radiation therapy static photon beams were applied. Before the arc and before the static field groups, fiducial marker positions were checked.By her second fraction of SBRT, she noted 4/10 pain intensity in the deep right pelvis. Dexamethasone and oxycodone were prescribed, with relief of symptoms noted afterward.
At her four-week follow-up visit, she reported no fatigue or pelvic pain. Surveillance 18-FDG PET scan done at that timeidentified improved signal in the pelvic cancer target, butalso new disease progression in the liver. She remains alive and her cancer therapy treatment plan with her gynecologic oncologist includes consideration of post-SBRT systemic chemotherapy.
Discussion
For gynecologic cancers initially managed by surgery, chemotherapy, or pelvic radiation, interventions for pelvic relapses pose increase risk of long-term morbidity, such as debilitating lymphedema, diverting colostomy and urinary conduits, and poor body image and sexual health [13-15]. While a small volume isolated central pelvic relapse may be approached surgically, often a pelvic exenteration must be done to remove disease with adequate surgical margin. Patients with co-morbid disease may be unwilling or may be unable to undergo second surgeries for relapsed gynecologic cancers involving the pelvis. Stereotactic ablative body radiation therapy such as that provided by the Vero SBRT system offers treatment with high radiation dose precision and limited therapy-related toxicities.
A phase II clinical trial of robotic-armSBRT established the safety and efficacy of this approach among patients with relapsed gynecologic cancers [4]. To our knowledge, this case series reports the first experiences of hypofractionated (8 Gy X three fractions) Vero hybrid arc stereotactic body radiation therapy in patients with relapsed gynecologic cancers.
In our retrospective case series, delivered radiation was well-tolerated. Corticosteroid and narcotic analgesia alleviated on-treatment pelvic pain in one patient. This symptomatic pain resolved by the four-week follow-up visit. No radiation cystitis or enteritis was encountered during the limited posttherapy observation period. Previously determined SBRT planning parameters were rigorously followed [16,17], and may account for the low incidence of toxicity seen in these three patients. Possible late toxicities such as fistula formation or chronic enteritis have not been observed, but follow-up is too premature to comment definitely on the incidence of late Vero SBRT treatment toxicities.
While the phase II clinical trial prescription dose has been carried forward to the Vero SBRT system, Vero hybrid arc stereotactic body radiation therapy results in at least one outstanding treatment difference. Currently, the more widely available robotic-arm platform uses a fixed or iris-collimated linear accelerator that may target only a fraction of the entire intended tumor volume at any single treatment node. This raises the possibility of low marginal radiation dose and geographical miss, as seen early on with robotic-arm stereotactic radiation therapy in the pelvis [1,18]. Later experience demonstrated improved radiosurgical target delineation with18-FDG PET scan data applied during stereotactic body radiation therapy planning [4,12]. While 18-FDG PET scan data has been integrated to improve target delineation, Vero hybrid arc stereotactic body radiation therapy treats the entire PTVwhen the radiation beam is on. We speculate that Vero hybrid arc stereotactic body radiation therapy, refined by 18-FDG PET scan data, lowers the chance of peripheral cancer cells receiving insufficient radiation prescription dose. Further follow-up of patients with relapsed gynecologic cancers treated by Vero SBRT must be done to validate such a claim.
Overall, these cases indicated that a Vero hybrid arc stereotactic body radiation therapy approach safely delivered radiation dose to abdominopelvic sites of relapsed gynecologic cancers. The therapy may be administered with minimal toxicity even in a group of pretreated patients. The case series would be strengthened by an appraisal of a larger patient cohort, by longer-term follow-up for assessment of treatment-related sequelae and durability of radiosurgical target response, and by reporting of longer-term cancer-related survival outcome.
Conclusion
Vero hybrid arc stereotactic body radiation therapy was safe to deliver, well-tolerated, and provided clinical benefit in the relief of relapsed gynecologic cancer-related symptoms. A prospective clinical trial of Vero hybrid arc stereotactic body radiation therapy in patients with relapsed gynecologic cancers in the abdomen and pelvis would be of clinical interest.
Ethics Statement
This case review study wasperformed with permission from the Summa Health System institutional review board.
References
-
Kunos C, Chen W, DeBernardo R, Waggoner S, Brindle J, et al. (2009) Stereotactic body radiosurgery for pelvic relapse of gynecologic malignancies. Technol Cancer Res Treat 8: 393-400.
-
Rutledge FN, Smith JP, Wharton JT, O'Quinn AG (1977) Pelvic exenteration: analysis of 296 patients. Am J Obstet Gynecol 129: 881-892.
-
Finlayson CA, Eisenberg BL (1996) Palliative pelvic exenteration: patient selection and results. Oncology (Williston Park) 10: 479-484.
-
Kunos CA, Brindle J, Waggoner S, Zanotti K, Resnick K, et al. (2012) Phase II Clinical Trial of Robotic Stereotactic Body Radiosurgery for Metastatic Gynecologic Malignancies. Front Oncol 2: 181.
-
Adler JR Jr, Chang SD, Murphy MJ, Doty J, Geis P, et al. (1997) The Cyberknife: a frameless robotic system for radiosurgery. Stereotact Funct Neurosurg 69: 124-128.
-
Mackie TR, Holmes T, Swerdloff S, Reckwerdt P, Deasy JO, et al. (1993) Tomotherapy: a new concept for the delivery of dynamic conformal radiotherapy. Med Phys 20: 1709-1719.
-
Benedict SH, Cardinale RM, Wu Q, Zwicker RD, Broaddus WC, et al. (2001) Intensity-modulated stereotactic radiosurgery using dynamic micro-multileaf collimation. Int J Radiat Oncol Biol Phys 50: 751-758.
-
Depuydt T, Poels K, Verellen D, Engels B, Collen C, et al. (2014) Treating patients with real-time tumor tracking using the Vero gimbaled linac system: implementation and first review. Radiother Oncol 112: 343-351.
-
Poels K1, Depuydt T, Verellen D, Engels B, Collen C, et al. (2013) A complementary dual-modality verification for tumor tracking on a gimbaled linac system. Radiother Oncol 109: 469-474.
-
Depuydt T, Poels K, Verellen D, Engels B, Collen C, et al. (2013) Initial assessment of tumor tracking with a gimbaled linac system in clinical circumstances: a patient simulation study. Radiother Oncol 106: 236-240.
-
Depuydt T, Penne R, Verellen D, Hrbacek J, Lang S, et al. (2012) Computer-aided analysis of star shot films for high-accuracy radiation therapy treatment units. Phys Med Biol 57: 2997-3011.
-
Kunos C, DeBernardo R, Fabien J, Dobbins D, Zhang Y, et al. (2011) 18DG-PET/CT definition of clinical target volume for robotic stereotactic body radiosurgery treatment of metastatic gynecologic malignancies. J Nucl Med Radiat Ther S4: 001.
-
Chase DM, Huang HQ, Wenzel L, Cella D, McQuellon R, et al. (2012) Quality of life and survival in advanced cervical cancer: a Gynecologic Oncology Group study. Gynecol Oncol 125: 315-319.
-
Monk BJ, Huang HQ, Cella D, Long HJ 3rd; Gynecologic Oncology Group Study (2005) Quality of life outcomes from a randomized phase III trial of cisplatin with or without topotecan in advanced carcinoma of the cervix: a Gynecologic Oncology Group Study. J Clin Oncol 23: 4617-4625.
-
Friedman LC, Abdallah R, Schluchter M, Panneerselvam A, Kunos CA (2011) Adherence to vaginal dilation following high dose rate brachytherapy for endometrial cancer. Int J Radiat Oncol Biol Phys 80: 751-757.
-
Kunos CA, Debernardo R, Radivoyevitch T, Fabien J, Dobbins DC, et al. (2012) Hematological toxicity after robotic stereotactic body radiosurgery for treatment of metastatic gynecologic malignancies. Int J Radiat Oncol Biol Phys 84: e35-41.
-
Mislmani M, Frasure H, Suppiah S, Fabien J, Lo SS, et al. (2014) Acute gastrointestinal toxicity after robotic stereotactic ablative radiotherapy for treatment of metastatic gynecological malignancies. Future Oncol 10: 241-248.
-
Kunos C, von Gruenigen V, Waggoner S, Brindle J, Zhang Y, et al. (2008) Cyberknife radiosurgery for squamous cell carcinoma of vulva after prior pelvic radiation therapy. Technol Cancer Res Treat 7: 375-380.





