Obstetrics and Gynaecology Cases - Reviews
Aortobifemoral Reconstruction during Pregnancy
Müller VA, Kasper AS and Hinterseher I*
Department of General, Visceral, Vascular and Thoracic Surgery, Charité Universitätsmedizin Berlin, Campus Mitte, Germany
*Corresponding author: Irene Hinterseher, M.D, Department of General, Visceral, Vascular and Thoracic Surgery, Charité Universitätsmedizin Berlin, Campus Mitte, Charitéplatz 1, 10177 Berlin, Germany, E-Mail: irene.hinterseher@charite.de
Obstet Gynecol Cases Rev, OGCR-2-028, (Volume 2, Issue 2), Case Report; ISSN: 2377-9004
Received: February 19, 2015 | Accepted: March 25, 2015 | Published: March 28, 2015
Citation: Müller VA, Kasper AS, Hinterseher I (2015) Aortobifemoral Reconstruction during Pregnancy. Obstet Gynecol Cases Rev 2:028. 10.23937/2377-9004/1410028
Copyright: © 2015 Müller VA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
We report a case of aortobifemoral bypass because of severe peripheral artery disease in a 40-year-old woman at 13 weeks of pregnancy. The patient presented herself to the emergency room with necrosis on her toes and a reduction of her maximal walking distance. She was obese and a heavy smoker although she has been pregnant at that time. We found a complete obstruction of the iliac artery on the left side and a high-grade stenosis of the common iliac artery on the right side. The indication for aortobifemoral bypass has been chosen after interdisciplinary discussion. The operation went well. The necrosis diminished and she gave birth to a healthy child.
Keywords
Aortobifemoral bypass, Peripheral artery occlusive disease, Pregnancy
Introduction
Peripheral artery occlusive disease (PAOD) and mandatory revascularization procedures are very rare during pregnancy and need to undergo a precise risk evaluation.
There are several reports about percutaneous transluminal coronary angioplasty (PTCA) and coronary stent procedures in pregnant women [1,2].
Until now, there are no reports about severe PAOD and aortobifemoral revascularization during pregnancy.
Case Report
A forty-year-old woman presented to the emergency unit with necrosis of her third and forth toes on the right side. She was in the twelfth week of gestation (gravida 4, para 2). Her maximal walking distance was fifty meters straight. The woman was a heavy smoker with forty cigarettes per day and she was obese (102kg, 159cm, BMI 40). In her last pregnancies she suffered from insulin dependent diabetes.
Duplex ultrasound showed monophasic flow profile in both common femoral arteries. Following magnetic resonance tomography which showed a complete obstruction of the iliac artery on the left side and a high-grade stenosis of the common iliac artery on the right side (Figure 1).
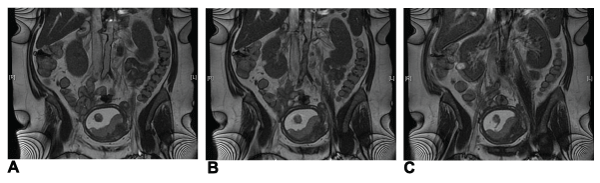
Figure 1: Magnetic resonance tomography prior to operation. The uterus and fetus is shown in the lower part of the abdomen. Pictures A to C are serial. A:
shows the beginning of the occlusion of the left common iliac artery. B: shows a high-grade stenosis of the right common iliac artery and again the occlusion of
the left one, additionally severe calcifications of the infrarenal aorta. C: shows that the right external iliac artery is open and that the left one is still occluded.
View Figure 1
Because of the end-stage peripheral artery occlusive disease there was an absolutely indication for treatment and because of the early stage of the pregnancy it was not possible to wait until delivery.
After thoroughly interdisciplinary discussion together with surgeons, gynecologists, angiologists, and radiologists we decided to do an aortobifemoral bypass. The operation had been done in the thirteenth gestation week without any problems. We performed a median laparotomy. The infrarenal aorta was at first only clamped tangentially to ensure some blood flow to the uterus. This turned out to be very difficult because of the very small calibre and some serious calcification of the aorta. We performed an end-to-side-anastomosis with the prosthesis (12 x 6 mm polyesterprosthesis, Dacron, Vascutek, a Terumo Company, Scotland UK) and the aorta. As the suture was not completely leak-proof at first, it needed to be a complete clamping of the aorta for a short period of time (six minutes). We did not need any blood transfusion. The time of operation was 280 minutes. During the operation a gynecologist monitored the fetus via ultrasound before and after clamping of the aorta and at the end of the operation. The fetus appeared to be vital and stable at all times.
The patient spent altogether six days on an intensive care unit and could be discharged from the hospital after the eleventh day.
The postoperative magnetic resonance tomography using optimized time of flight sequences without any contrast agent showed a good flow of the aorta, the prosthesis and the arteries of both legs (Figure 2). Six month later a caesarean section was performed (request of the patient) and a healthy girl had been born (3415g, 49cm, APGAR 9/10/10).
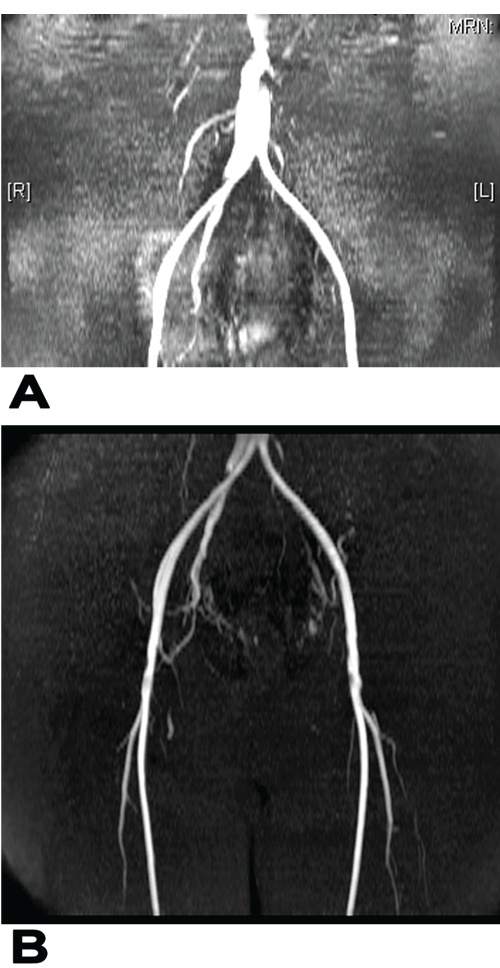
Figure 2: The postoperative magnetic resonance tomography with optimized
time of flight sequences without any contrast agent showed a good flow of the
aorta, the upper anastomosis (A), the prosthesis and lower anastomoses and
the arteries of both legs (B). The image also shows the multiple collaterals
to the uterus.
View Figure 2
One year after the operation the patient presented herself to the outpatient clinic. The necrosis of the toes had healed completely and the patient was without any complaints.
Three years after the operation the patient needed to be treated for an incisional hernia in the median laparotomy. She received a fifteen times fifteen ultrapro open mesh repair using a sublay technique [3].
Discussion
Vascular intervention during pregnancy is rare. This is the first case report about a pregnant woman receiving aortobifemoral reconstruction during pregnancy.
With the increasing age and fertility of women the incidence of atherosclerosis in pregnancy will increase. By now, there are several reports about coronary artery disease or myocardial infarction in pregnancy. Cardiovascular diseases seem to complicate approximately 0.4% to 4% of all pregnancies [4].
Cardiac catheterizations also carry risks, but were reported to be performed rather safely in pregnancy [5]. Appropriate abdominal shielding, use of a brachial or radial approach, and lower fluoroscopy times are important to minimize fetal exposure to radiation [6]. It is common sense that nuclear imaging should be especially avoided during organogenesis (10 to 50 days) due to the risk of teratogenesis. In the second and third trimesters, nuclear imaging still poses a risk of intrauterine growth retardation and central nervous system abnormalities [7].
Today in high risk patients endovascular treatment of atherosclerosis is preferred but in this case of course it was not possible to shield the abdomen. This was one of the points why the decision which operation we should perform was so difficult. We had several ideas in mind: 1) The endovascular approach was not feasible because of the early stage of pregnancy and necessary high dosage of radiation and contrast medium and additionally because of the configuration of the stenosis. It did not look like that the left common iliac artery could be treated by endovascular therapy. Besides that, following the TASC (Trans Atlantic Inter-Society Consensus TASC II) Criteria we were dealing with a Type D lesion which has better long-term results with open revascularization [8]. What also needs to bear in mind is that with a stent the patient would have needed an antiplatelet medication. Salicylates are able to cross the placenta and enter fetal circulation. High doses of acetylsalicylic acid are known to cause fetal complications including mortality, intrauterine growth retardation, bleeding abnormalities, neonatal acidosis and premature closure of the ductus arteriosus [9]. There is not much known about the safety of other antiplatelet agents such as clopidogrel. The anticoagulant of choice during pregnancy is heparin, because it does not cross the placenta. 2) A hybrid procedure with stenting the short stenosis on the right side in combination with a femoro-femoral crossover bypass from right to left was discussed as well. This would have been less invasive but not really suitable for a forty year old woman with an expected length of stay more than ten years. Also X-Ray and contrast agent would be needed. 3) Another idea was to perform an axillo-bifemoral bypass subcutaneously. We abandoned this idea because of the expected growing of the abdomen. Additionally with this procedure the patient needs to be therapeutically anticoagulated. 4) The aortobifemoral bypass is the standard procedure for this type of lesion. The aortobifemoral repair is the therapy with the best longterm results. We did not think that clamping of the aorta causes the fetus any harm because of the aorta being very stenotic at all and the internal iliac arteries and the uterine arteries were nourished mainly by multiple collaterals (Figure 2). Abdominal surgery during pregnancy has been reported to be safe. About two percent of women require surgery because of a non-obstetric reason during pregnancy [10]. The most common non-obstetric operation during pregnancy is an appendectomy (44%), followed by a cholecystectomy (22.3%). Laparoscopy is safe even during pregnancy, with the known advantages of minimally invasive surgery, but it carries a higher miscarriage rate than laparotomy, with a comparable preterm birth rate [11]. That is why we chose this kind of procedure although we knew that incisional hernias have a higher risk to develop in patients undergoing aortic surgery [12,13].
Conclusion
This report shows that major aortic surgery is feasible during pregnancy and should be performed if mandatory.
References
-
Dwyer BK, Taylor L, Fuller A, Brummel C, Lyell DJ (2005) Percutaneous transluminal coronary angioplasty and stent placement in pregnancy. Obstet Gynecol 106: 1162-1164.
-
Sharma GL, Loubeyre C, Morice MC (2002) Safety and feasibility of the radial approach for primary angioplasty in acute myocardial infarction during pregnancy. J Invasive Cardiol 14: 359-362.
-
Berger D, Lux A (2013) Operative therapy of secondary ventral hernia: technical principles. Chirurg 84: 1001-1012.
-
Burlew BS (1990) Managing the pregnant patient with heart disease. Clin Cardiol 13: 757-762.
-
Collins JS, Bossone E, Eagle KA, Mehta RH (2002) Asymptomatic coronary artery disease in a pregnant patient. A case report and review of literature. Herz 27: 548-554.
-
Rezig K, Diar N, Walcker JL (2000) Myocardial infarction, pregnancy and anesthesia. Ann Fr Anesth Reanim 19: 544-548.
-
Scharw�chter C, R�ser A, Schwartz CA, Haage P (2014) Pr�natale Strahlenexposition: Dosisermittlung. Fortschr R�ntgenstr.
-
Norgren L, Hiatt WR, Dormandy JA, Nehler MR, Harris KA, et al. (2007) Inter-Society consensus for the management of peripheral arterial disease (TASC II). J Vasc Surg 45: S5-S67.
-
Rutherford JD (1998) Coronary artery disease in the childbearing age. In: Elkham U, Gleicher N Cardiac problems in pregnancy: diagnosis and management of maternal and fetal heart disease. (3rd edn) NewYork: Wiley-Liss Inc: 121-130.
-
Cheek TG, Baird E (2009) Anesthesia for nonobstetric surgery: maternal and fetal considerations. Clin Obstet Gynecol 52: 535-545.
-
Juhasz-B�ss I, Solomayer E, Strik M, Rasp� C (2014) Abdominal surgery in pregnancy--an interdisciplinary challenge. Dtsch Arztebl Int 111: 465-472.
-
Augestad KM, Wilsgaard T, Solberg S (2002) Incisional hernia after surgery for abdominal aortic aneurysm. Tidsskr Nor Laegeforen 122: 22-24.
-
Takagi H, Sugimoto M, Kato T, Matsuno Y, Umemoto T (2007) Postoperative incision hernia in patients with abdominal aortic aneurysm and aortoiliac occlusive disease: a systematic review. Eur J Vasc Endovasc Surg 33: 177-181.





