Obstetrics and Gynaecology Cases - Reviews
Endoscopic Conservative Treatment for an Ureterovaginal Fistula Caused by Foreign Body
DeLeon E1, Lankford D2, Allman D2, Phillibert D1, Paolucci M1, Gore S1 and Clare C1*
1Department of Obstetrics and Gynecology, New York Medical College, USA
2Department of Urology, New York Medical College, USA
*Corresponding author: Camille A. Clare, MD, MPH, Department of Obstetrics and Gynecology, Metropolitan Hospital, 1901 First Avenue, Room 4B5, New York, New York 10029, USA, Tel: 212-423-6796, Fax: 212-423-8121, E-mail: Camille_clare@nymc.edu
Obstet Gynecol Cases Rev, OGCR-2-020, (Volume 2, Issue 1), Case Report; ISSN: 2377-9004
Received: December 13, 2014 | Accepted: January 17, 2015 | Published: January 20, 2015
Citation: DeLeon E, Lankford D, Allman D, Phillibert D, Paolucci M et al., (2015) Endoscopic Conservative Treatment for an Ureterovaginal Fistula Caused by Foreign Body. Gynecol Cases Rev 2:020. 10.23937/2377-9004/1410020
Copyright: © 2015 DeLeon E, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Foreign body placement in the vagina is a rare cause of ureterovaginal fistula. A fistula is often due to an unrecognized injury to the ureter, most commonly after gynecologic pelvic surgery, such as during hysterectomy for benign indications. This manuscript will discuss a case of a 34-year-old African American female who presents with a history of sexual assault and a one month history of urinary incontinence. Physical examination revealed clear liquid in the vaginal vault and a malodorous foreign body embedded in the vaginal mucosa. Cystoscopy ultimately confirmed a left ureterovaginal fistula. A CT cystogram was performed after removal of the foreign body, which demonstrated the size and location of the fistula. A cystoscopy, retrograde pyelography and fistulography were all performed. The patient�s kidney function was determined to be adequate with estimated creatinine clearance and the appearance of symmetric uptake of contrast on CT scan. The patient�s symptoms resolved after conservative treatment with JJ catheter stent placement for six weeks. Therefore, conservative endoscopy treatment should be considered for small fistulae. Trauma from sexual assault may be physical and emotional, and therefore, a multidisciplinary approach to treatment is paramount.
Keywords
Ureterovaginal fistula, Foreign body, Endoscopic treatment
Introduction
Urogenital fistulae are abnormal connections between the urogenital system and adjacent structures and organs. These fistulae are often caused by anunrecognized injury to the ureter. The ureter can be injured during any gynecologic pelvic surgery, most commonly during hysterectomies for benign reasons [1,2]. The ureter is at greatest risk of injury in the distal three centimeters, as it courses through a tunnel in the cardinal ligament over the anterior vaginal fornix to enter the bladder near the cervix. Injury also occurs during ligation of the uterine vessels and the uterosacral and cardinal ligaments [3]. The natural course of the left ureter in the pelvis is more midline to the cervix than the right ureter, which places it at greater risk of injury [1]. The types of injury leading to ureterovaginal fistulae include: partial and complete ureteral transection, thermal injury from electrocautery, ischemic injury caused by suture ligation, crush injury from clamp trauma or damage to the delicate periureteral blood supply. In rare instances, erosion due to the presence of a retained foreign body, such as a pessary, can be a cause of a ureteral injury [2].
Case
A 34-year-old African American female P2012 presented to the ED complaining of urinary incontinence x 1 month. Symptoms progressed from a dribble to the passage of copious amounts of urine and an inability to control urinary flow. The patient stated a history of sexual assault during which a foreign object was placed in the vagina and was not removed. At the time of presentation, she was afebrile, BP 127/81, HR 98 bpm, O2 saturation 98% on room air. Vaginal exam revealed normal external female genitalia, 100 cc of pooled clear liquid in the vaginal vault, and a frank malodorous, unrecognizable object adherent to the cervix which was embedded in necrotic vaginal mucosa. Pelvic CT scan revealed a thin curvilinear shaped foreign body within the vaginacontaining internal fluid and air and an increased soft tissue thickening between the urinary bladder and anterior vaginal wall.
The patient was taken to the OR for an exam under anesthesia. A 4-5 cm bottle cap was removed from the vagina. A 3 cm mucosal erosion with active leaking of urine between the bladder anteriorly and the cervix posteriorly was noted. Cystoscopy revealed a visually normal right ureteral orifice. Irritation obscured the left ureteral orifice, preventing its direct visualization. A Foley catheter was placed. Repeat CT scan showed a subtle irregularity involving the posterior wall of the bladder but no evidence of fistula. A CT urography scandemonstrated a fistula based on the finding of contrast within the vagina, but its exact location was indeterminate. The patient received a CT cystogram after removal of the foreign body, which demonstrated the size and location of the fistula.The patient was discharged home with the Foley catheter in place and follow-up in the urology clinic. After six weeks of conservative management, urine continued to leak into the vaginal vault. The patient was taken to the OR for a repeat cystoscopy. A left ureterovaginal fistula was identified, and a JJ catheter stent was placed.During the second procedure, a cystoscopy, retrograde pyelography and fistulography were all performed. The patient�s kidney function was determined to be adequate with estimated creatinine clearance and the appearance of symmetric uptake of contrast on CT scan.Six weeks later, her symptoms had resolved completely (Figure 1,2).
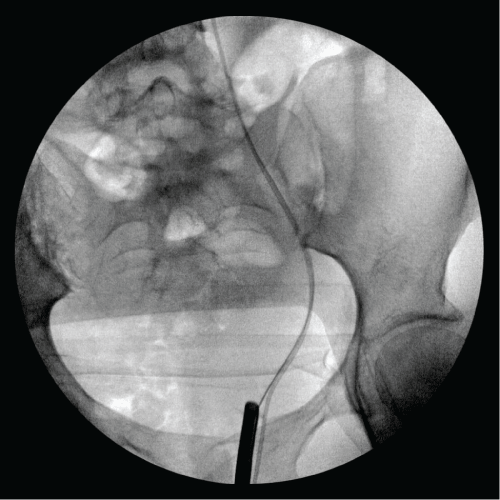
Figure 1: Fluoroscopic image showing a wire within the bladder through
the left ureteral orifice. The open ended catheter remains in fistula tract
which helped when placing the wire. A cystoscope is seen within the
bladder through the urethra.
View Figure 1
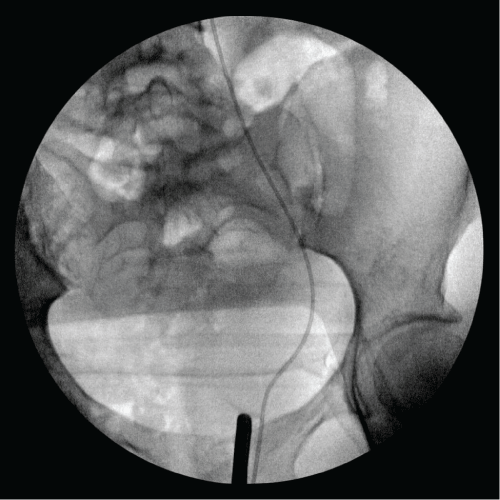
Figure 2: Fluoroscopic image showing open ended catheter within the
vagina, through the fistula, and in the urinary system. A cystoscope is seen
within the vagina.
View Figure 2
Discussion
Etiology/Prevalence
The exact incidence of urogenital fistulae is unknown as many women never seek treatment, but the World Health Organization estimates that there are 130,000 new cases worldwide per year [2,3]. The prevalence and etiology of urogenital fistulae varies geographically. Urogenital fistulae are more common in developing countriesas a result of obstructed labor [1,2].
In developed countries, urogenital fistulae are most often iatrogenic at the time of gynecologic surgery [1,3]. Fistulaemost commonly occur during hysterectomies for benign indications [2]. Trauma related to vaginal foreign body placement is another rare cause of urogenital fistula formation. The incidence of a foreign body causing a urogenital fistula is unknown, but there are a number of reports describing such cases. The foreign body in most reported cases is a ring pessary [2,4].
The location of the connecting tract determines what type of fistula is present. Vesicovaginal fistulae, tracts between the bladder and the vagina, are the most common type, occurring three times more frequently than ureterovaginal fistulae, connections between the ureter and the vagina [2,3]. Ureterovesicovaginal fistulae, connecting tracts between the ureter, bladder, and vagina, are infrequently encountered in clinical practice. In our case, an ureterovaginal fistula was identified only after the foreign body was removed and the damaged tissue was no longer subjected to the pressure applied by the object.
TreatmentOnce an ureterovaginal fistula is identified, ureteral stents should be placed and remain for 6 to 8 weeks [2,3]. Up to 80% of small fistulas (diameter of 1 cm or less) will close spontaneously with stenting alone [2]. If a fistula does not close after stenting, it must be repaired surgically. Fistulae within the distal third of the ureter are repaired by ureteral reimplantation into the bladder, known as an ureteroneocystostomy [2,3]. Fistulae in the middle and upper thirds of the ureter are repaired by ureteroureterostomy in which the involved area is resected, and the two ends of the ureter are reanastamosed [2,3]. Success of a fistula repair is most commonly defined as cessation of urine leakage upon discharge from the hospital. Long-term success rates after fistula repair are unknown as many patients are lost to follow up [3].
Psychological support must also be provided, especially in cases that involve rape and other forms of assault, such as with our patient. Our patient was open to and received psychiatric counseling while she was in the hospital initially. She continued to follow up with psychiatry as an outpatient.
References
-
Hoffman B, Schorge J, Schaffer J, Halvorson L, Bradshaw K, et al. (2008) Williams Gynecology. New York: McGraw-Hill Medical, Print.
-
Garely AD, Mann Jr WJ (2013) Urogenital tract fistulas in women. In: UpToDate, Post TW (Ed), UpToDate, Waltham, MA. (Accessed on November 25, 2013.)
-
Wong MJ, Wong K, Rezvan A, Tate A, Bhatia NN, et al. (2012) Urogenital fistula. Female Pelvic Med Reconstr Surg 18: 71-78.
-
Massinde A, Kihunrwa A (2013) Large vesico-vaginal fistula caused by a foreign body. Ann Med Health Sci Res 3: 456-457.





