Obstetrics and Gynaecology Cases - Reviews
Successful Outcome of an Uneventful Caesarean Scar Pregnancy with Intra-Ligamentary Development
Akladios Cherif Y1*, and Langer Bruno
Department of Gynaecology & Obstetrics, Strasbourg University Center, France
*Corresponding author: Cherif Y. Akladios, MD, PhD, Department of Gynaecology & Obstetrics, Strasbourg University Center, 1 Avenue Molière, 67098 Strasbourg cedex, France, Tel: +33 388127455; E-mail: cherif.youssef2@wanadoo.fr
Obstet Gynecol Cases Rev, OGCR-1-007, (Volume 1, Issue 2), Case Report; ISSN: 2377-9004
Received: October 22, 2014 | Accepted: November 12, 2014 | Published: November 15, 2014
Citation: Akladios CY, Bruno L (2014) Successful Outcome of an Uneventful Caesarean Scar Pregnancy with Intra-Ligamentary Development. Gynecol Cases Rev 1:007. 10.23937/2377-9004/1410007
Copyright: © 2014 Akladios CY, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Keywords
Cesarean scar pregnancy, Live-born, Cesarean delivery
Introduction
We report a case of an uneventful, cesarean scar pregnancy with intra-ligamentary development, diagnosed during a planned caesarean delivery at 38 weeks. A healthy boy weighting 3600 g was delivered. The diagnosis was never suspected during antenatal care.
Case Report
A 33-year-old woman, gravida 5, para 2, was scheduled for a caesarean delivery at 38 weeks, because of both the foetus�s breech presentation and her history of 2 caesarean deliveries. A subsequent dilatation and curettage for incomplete abortion completed her obstetric history. Early pregnancy was uneventful. Ultrasound at 6 and 8 weeks showed a viable and apparently normally situated embryo. During the second and third trimester, fetal growth and Doppler waveforms were within normal limits (Figure 1), and the placenta appeared to be anterior not praevia. A caesarean section was scheduled at 38+3 weeks of gestation. It began with a parietal incision, according to the Misgav-Ladach technique. The observation of large vessels crossing the uterine wall suggested placenta accreta. After an incision in the presumed uterus, we removed a baby boy weighing 3600g, in good general condition with Apgar score 10 at 1 minute.
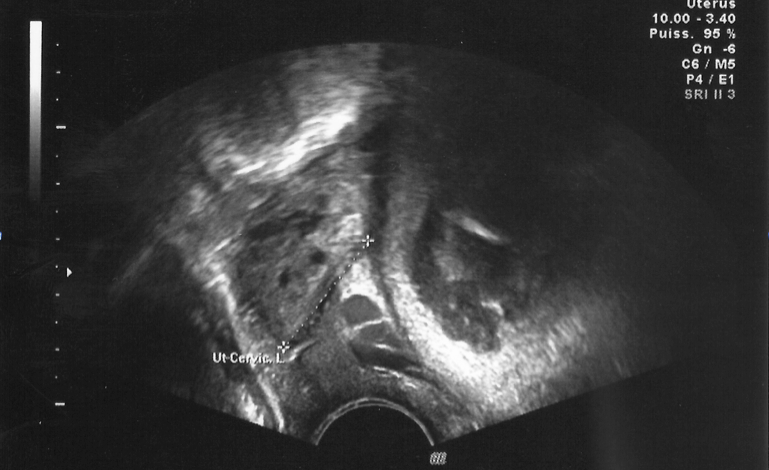 Figure 1: A trans-vaginal ultrasonography showing a normally situated, intrauterine
pregnancy with anterior placenta.
View Figure 1
Figure 1: A trans-vaginal ultrasonography showing a normally situated, intrauterine
pregnancy with anterior placenta.
View Figure 1
Exploration of the abdominal cavity showed that the gestational sac was actually located over the antero-lateral aspect of the uterus at the level of the lower segment creating thus a complete dehesence of the anterior uterine wall, probably at the level of the caesarean scar. It occupies further the left broad ligament. A small, empty uterus was identified to the right of this sac�s posterolateral pole but did not communicate with it (Figure 2). Dissection of the bladder made it possible to locate the cervix, which was connected to the body of the uterus only by theposterior wall. The diagnosis of caesarean scar pregnancy (CSP) and intra-ligamentary development of the sac was finally retained. We decided to perform a subtotal hysterectomy. There was no need for blood transfusion. The patient was discharged from the hospital at day 8.
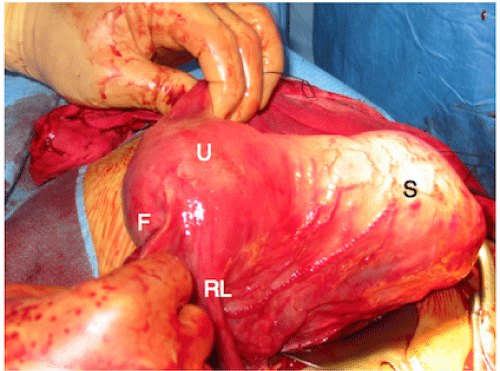 Figure 2: A side view showing the uterine body (U), the interstitial segment of
the fallopian tube (F), and the right round ligament. Anteriorly and to the left
is the empty gestational sac (GS), covered by the peritoneum: photo taken
after foetus and placenta extraction. The uterus is displaced 90 degrees by
the gestational sac.
View Figure 2
Figure 2: A side view showing the uterine body (U), the interstitial segment of
the fallopian tube (F), and the right round ligament. Anteriorly and to the left
is the empty gestational sac (GS), covered by the peritoneum: photo taken
after foetus and placenta extraction. The uterus is displaced 90 degrees by
the gestational sac.
View Figure 2
Discussion
Caesarean scar pregnancy is a rare obstetric complication, but its incidence is rising rapidly as a consequence of the inexorable rise in caesarean deliveries combined with the widespread use of transvaginal ultrasound scans, which allow earlier detection of this type of pregnancy [1]. The fundamental pathophysiology of CPS is believed to be the blastocyst�s invasion of the myometrium through a microtubular tract between the caesarean scar and the endometrial cavity [1]. The blastocyst, completely surrounded by myometrium and fibrous tissue of the scar, is totally separated from the endometrial cavity. The vascularization and the consequent developmental potential of a CPS seem to be proportional to the depth of invasion. Hence deeply implanted pregnancies are known to be more vascularized and thus able to maintain viability of the embryo [2]. In our case, the gestational sac did not communicate with the uterine cavity. One can think that it began as a deeply implanted sac that then developed in the loose areolar tissue of the left broad ligament.
It is currently agreed that early diagnosis of CSP enables prompt treatment and thus avoids bleeding and uterine rupture [3]. The diagnosis, however, is difficult and requires a high degree of clinical suspicion. In fact, there are no specific symptoms for CSP: bleeding is the most common symptom, but is encountered in less than 50% of cases. Although the ultrasonographic criteria of CSP are well established [2,3], images appear to be misinterpreted in up to 71% of cases with delayed diagnosis [4]. Moreover, it must be distinguished from low implantation, inevitable abortion and cervical pregnancy. Little information is available about the natural history and course of this pathology, because the pregnancy is terminated in almost all published cases as soon as the diagnosis is made. Despite the numerous therapeutic modalities thus far reported [5], no consensus defining optimal management has been established. Expectant management, however, is known to be unsuccessful and at a high risk of severe haemorrhage and uterine rupture [2]. Until now, among few published cases managed expectantly, two had given a live born infant by caesarean delivery at 35 [6] and 36 [7] weeks of gestation. The indication for the caesarean in both cases was abdominal pain and bleeding after 28 and 30 weeks of follow up respectively. Our case is different from these two cases in that it was not diagnosed as a caesarean scar pregnancy until delivery. Also the absence of bleeding which could be related to the absence of communication in-between the gestational sac and the uterine cavity. In another case diagnosed at 16 weeks, a laparotomy and hysterectomy were required at 20 weeks because of a ruptured uterus [8]. In our case the development of the pregnancy in the broad ligament could have protected the patient from such issue. The development of this pregnancy is very much close to that of extra-uterine intra-ligamentary pregrancy than already described cesarean scar pregnancies. It�s to our best knowledge the first reported uneventful CSP that reaches term and leads to delivery of a normal healthy newborn. It could raise the question of a potential role of expectant management in selected cases of CSP. It should however be empathised that our case is a high risk situation resulting from different procedures done to the patient which should be remind every time it�s a question of commoditization of caesarean section. Furthermore, although clinical course was uneventful, expectant management in similar cases should be considered with caution.
References
-
Jurkovic D, Hillaby K, Woelfer B, Lawrence A, Salim R, et al. (2003) First-trimester diagnosis and management of pregnancies implanted into the lower uterine segment Cesarean section scar. Ultrasound Obstet Gynecol 21: 220-227.
-
Ash A, Smith A, Maxwell D (2007) Caesarean scar pregnancy. BJOG 114: 253-263.
-
Vial Y, Petignat P, Hohlfeld P (2000) Pregnancy in a cesarean scar. Ultrasound Obstet Gynecol 16: 592-593.
-
Wang YL, Su TH, Chen HS (2006) Operative laparoscopy for unruptured ectopic pregnancy in a caesarean scar. BJOG 113: 1035-1038.
-
Michener C, Dickinson JE (2009) Caesarean scar ectopic pregnancy: a single centre case series. Aust N Z J Obstet Gynaecol 49: 451-455.
-
Herman A, Weinraub Z, Avrech O, Maymon R, Ron-El R, et al. (1995) Follow up and outcome of isthmic pregnancy located in a previous caesarean section scar. Br J Obstet Gynaecol 102: 839-841.
-
El-Matary A, Akinlade R, Jolaoso A (2007) Caesarean scar pregnancy with expectant management to full term. J Obstet Gynaecol 6: 624-625.
-
Smith A, Ash A, Maxwell D (2007) Sonographic diagnosis of cesarean scar pregnancy at 16 weeks. J Clin Ultrasound 35: 212-215.





