Obstetrics and Gynaecology Cases - Reviews
Laparoscopic Single Mesh Sacrohysteropexy Plus bladder Patch for Pelvic Organ Prolapse
Mai Myoga1, Kazuaki Yoshimura1*, Kazuaki Nishimura1, Kaori Hoshino1 and Toru Hachisuga2
1Department of Obstetrics and Gynecology, Wakamatsu Hospital of University of Occupational and Environmental Health, Japan
2Department of Obstetrics and Gynecology, University of Occupational and Environmental Health, Japan
*Corresponding author:
Kazuaki Yoshimura, Department of Obstetrics and Gynecology, Wakamatsu Hospital of University of Occupational and Environmental Health, 1-17-1 Hamamachi, Wakamatsu-ku, Kitakyushu, 808-0024, Japan, Tel: +81-93-761-0090, Fax: +81-93-588-3904, E-mail: yoppy@med.uoeh-u.ac.jp
Obstet Gynecol Cases Rev, OGCR-4-101, (Volume 4, Issue 1), Case Report; ISSN: 2377-9004
Received: August 26, 2016 | Accepted: January 26, 2017 | Published: January 28, 2017
Citation: Myoga M, Yoshimura K, Nishimura K, Hoshino K, Hachisuga T (2017) Laparoscopic Single Mesh Sacrohysteropexy Plus bladder Patch for Pelvic Organ Prolapse. Obstet Gynecol Cases Rev 4:101. 10.23937/2377-9004/1410101
Copyright: © 2017 Myoga M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Here we introduce a laparoscopic sacrohysteropexy plus bladder patch procedure as a useful operative procedure for POP patients who desire uterine preservation. A 62-year-old woman, gravida 2 para 2 with pelvic organ prolapse quantification (POP-Q) stage III of uterine prolapse and stage II of cystocele, came to our hospital and desired a POP operation with uterine preservation. She underwent laparoscopic single mesh sacrohysteropexy. A 4-port diamond-shaped approach was used. A 3cm-wide polypropylene mesh was fixed to the anterior longitudinal ligament on the sacral promontory, Levator ani, andthe posterior uterine cervix. The bladder was dissected and a triangular shaped mesh (4 × 5 cm) was placed from the most distal portion of the vagina to the uterine cervix. The operation time was 150 min. Blood loss was 10 ml. One year after the operation, there were no complications, no symptoms, and a good anatomical outcome was confirmed.
Keywords
Laparoscopic sacrohysteropexy, Pelvic organ prolapse, Bladder patch
Introduction
The transvaginal mesh procedure was developed in France [1]. This popular procedure is also wide spread in Japan. However, since the Food and Drug administration (FDA) alert for the transvaginal mesh surgery in 2011 (http://www.fda.gov/MedicalDevices/Safety/AlertsandNotices/ucm262435.htm), urogynecologists have been anticipating a newer operative procedure. Recently, laparoscopic sacrocolpopexy (LSC), which is simultaneously performed with supracervical hysterectomy, has been one of the most popular surgical procedures for uterine prolapse using laparoscopy. Historically, LSC has excellent outcomes, however, it requires the learning of difficult techniques--and the operation times are typically longer. In addition, patients may feel a sense of loss of their uterine corpus, and there still remains a risk of uterine cervical cancer due to the remaining uterine cervix. For such cases, Laparoscopic sacrohysteropexy (LSH) is an effective procedure with uterine preservation, and will typically achieve good outcomes with non-absorbable mesh. Although a double mesh LSH method was previously reported as a POP operation method with uterine preservation, it requires complicated procedures and longer operation times. Here we introduce a novel surgical technique a single mesh LSH plus bladder patch procedure.
Case Report
A 62-year-old woman, gravida 2 para 2 with pelvic organ prolapse quantification (POP-Q) stage III of uterine prolapse and stage II of cystocele, came to our hospital and desired a POP operation with uterine preservation. She underwent laparoscopic sacrohysteropexy (LSH).The patient was placed in the lithotomy position under general anesthesia. A 4-portdiamond-shaped approach was used (Kii Ballon Blunt Tip System®, 12 × 100 mm, Applied Medical, USA and E-Z trocar smart insertion®, Hakko, Japan). The sigmoid colon was pulled up to the left side to ensure clear view of the sacral promontory. The peritoneum over the sacral promontory was opened about 3 cm. The anterior-longitudinal ligament on the sacral promontory and right ureter were identified. A tunnel was made under the peritoneum, from the sacral promontory to the Douglas pouch. The para-rectal space was dissected to the Lavator ani muscle. The vesico-uterine peritoneum was incised, and the bladder was dissected distally. Two pieces of mesh (Polyform® Synthetic Mesh, Boston Scientific Corporation, USA) were cut on the clean field. The first one (4 × 5 cm, rounded isosceles triangle shape) for anterior vaginal support and the second one (3 × 12 cm) for suspension of the uterus were used (Figure 1).The vertex of an isosceles triangle shaped mesh was fixed to the most distal point of the anterior vagina with non-absorbable surgical suture (ETHIBOND EXCEL®, #0-SH, ETHICON, Somerville, NJ, USA) and was adjusted to fit the front of the vagina. The other side of the mesh was sutured to the cervix with the same string. The remaining portion of the mesh was fixed to the vaginal wall with 6 to 8 absorbable tacks (AbsorobaTack®, COVIDIEN, Mansfield, MA, USA) (Figure 2). The posterior mesh was fixed firmly to the Lavator ani muscle and the posterior cervix by using the same non-absorbablesutures. The mesh was passed through the tunnel under the peritoneum and fixed to the anterior longitudinal ligament on the sacral promontory with 2 sutures of the non-absorbable string. The peritoneum was closed with glyconate monofilament absorbable suture (Monosyn®, #0-CT1, B.BRAUN, Barcelona, Spain). Figure 3 shows a schema of the sagittal section of the pelvis after LSH. The operation time was 150 min. Blood loss was 10ml. One year after the operation, there were neither complications nor symptoms, and a good anatomical outcome was confirmed.

.
Figure 1: A posterior mesh and a bladder patch (an isosceles triangle shaped mesh).
View Figure 1
.
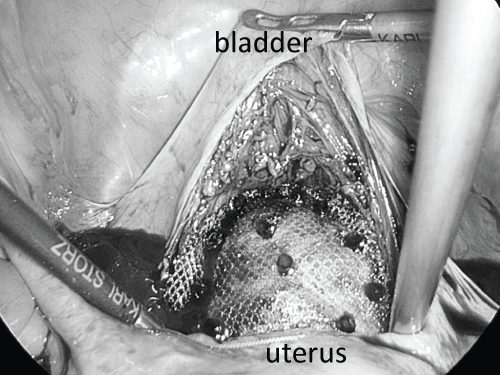
Figure 2: A bladder patch was placed between bladder and the anterior vaginal wall.
View Figure 2
Discussion
There are various vaginal and abdominal of POP surgery approaches. In 1880, the Manchester operation was first reported as a surgical method for pelvic organ prolapse. After that, many non-mesh POP procedures have been developed and reported. In 2004, transvaginal mesh surgery was first reported from the French TVM (tension-free vaginal mesh) group [1]. Transvaginal mesh surgery is an innovative and popular procedure for all types of POP; its popularity spread worldwide in a very short time. However, the FDA reported alerted severe complications regarding transvaginal mesh usage (2011).
.
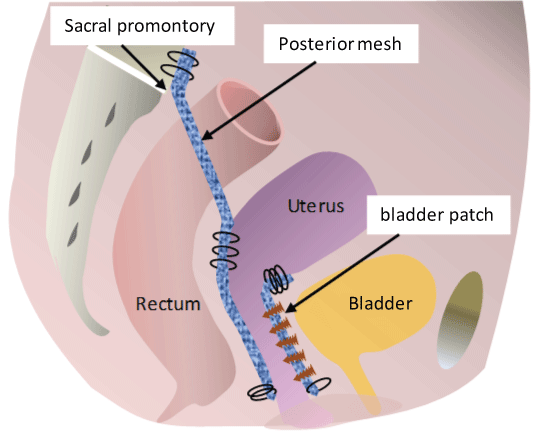
Figure 3: Sagittal section of the pelvis after LSH.
A posterior polypropylene mesh was fixed to the anterior longitudinal ligament on the sacral promontory, the posterior uterine cervix and Levator ani muscle. A bladder patch was placed from the most distal portion of the vagina to the uterine cervix.
View Figure 3
Laparoscopic sacrohysteropexy (LSH) is a less invasive procedure and a new technique of POP surgery which can achieve patients' desires of uterine preservation. Various methods of LSH have been reported, and a standard LSH procedure has yet to be established. In 2001, Lerson, et al. reported 13 cases of abdominal LSH with synthetic mesh, which could preserve the uterus. They used a 'Y' shaped mesh and accomplished the lifting of patients' uterus by fixing it on to the anterior longitudinal ligament, the anterior cervix, and the posterior cervix [2]. Price, et al. reported an LSH procedure using only the anterior Y shaped mesh [3]. Lewis, et al. reported an LSH procedure using only the posterior mesh [4].
There are few reports about regarding long-term outcomes of LSH because of it's a relatively short history. In 2011, Costantini, et al. reported about the five-year outcomes of uterus sparing surgery by using both anterior and posterior mesh (47 abdominal sacrohysteropexy and 8 laparoscopic sacrohysteropexy) for symptomatic POP. There was no recurrent uterine prolapse reported, however, there was stage II cystocele (7.7%) and stage II rectocele (5.7%) [5].
Therefore based on those findings, we attempted a new method to rectify this. We used a single posterior mesh along with a smaller triangular mesh for cystocele (bladder patch), and inserted the meshes through the perineal body. This procedure will save significant timeand blood loss because there is no need for the opening of the broad ligament around the uterine artery. So far, seven patients underwent LSH in our hospital. The median operating time was 160 min (120-230), and the median blood loss was 31 ml (10-100).
All cases have good anatomical and functional outcomes (The postoperative periods were 3-12 months).In addition, for patients who desire to not to lose their fertility, LSH is a suitable procedure because it preserves the uterus. There are a few reports about pregnancy after sacrohysteropexy. Balsak, et al. reported that a patient who underwent abdominal sacrohysteropexy became pregnant and delivered vaginally [6]. Lewis, et al. reported of a cesarean section after an LSH procedure. However, the patient required a second surgery due to recurrence, one year after the initial surgery [4]. We have not undergone LSH yet for POP patients who hope their fertility desired to preserve their fertility preservation.
There are some limitations in this study. There are few reports of LSH and the long-term outcomes are still unknown. In 2014, a multicenter randomized controlled trial comparing LSH with vaginal sacrospinous hysteropexy began in Belgium and Holland [7]. This trial should help uncover more data regarding the efficacy of LSH.
In conclusion, in this paper we introduced a novel technique using a single mesh LSH with a patch. We believe that our suggested technique is a better option for POP patients who wish to preserve their uterus.
References
-
Debodinance P, Berrocal J, Clave H, Cosson M, Garbin O, et al. (2004) Changing attitudes on the surgical treatment of urogenital prolapse: birth of the tension-free vaginal mesh. J Gynecol Obstet Biol Reprod (Paris) 33: 577-588.
-
Leron E, Stanton SL (2001) Sacrohysteropexy with synthetic mesh for the management of uterovaginal prolapse. BJOG 108: 629-633.
-
Price N, Slack A, Jackson SR (2010) Laparoscopic hysteropexy: the initial results of a uterine suspension procedure for uterovaginal prolapse. BJOG 117: 62-68.
-
Lewis CM, Culligan P (2012) Sacrohysteropexy followed by successful pregnancy and eventual reoperation for prolapse. Int Urogynecol J 23: 957-959.
-
Costantini E, Lazzeri M, Zucchi A, Bini V, Mearini L, et al. (2011) Five-year outcome of uterus sparing surgery for pelvic organ prolapse repair: a single-center experience. Int Urogynecol J 22: 287-292.
-
Balsak D, Eser A, Erol O, Deniz Altintas D, Aksin S (2015) Pregnancy and Vaginal Delivery after Sacrohysteropexy. Case Rep Obstet Gynecol 2015: 305107.
-
van IMN, Coolen AL, Detollenaere RJ, den Boon J, Bongers M, et al. (2014) Hysteropexy in the treatment of uterine prolapse stage 2 or higher: a multicenter randomized controlled non-inferiority trial comparing laparoscopic sacrohysteropexy with vaginal sacrospinous hysteropexy (LAVA-trial, study protocol). BMC Womens Health 14: 112.





