Obstetrics and Gynaecology Cases - Reviews
Giant Vulvar Leiomyoma: Successful Management in a Poor Setting of a Common Neoplasm in an Uncommon Site
Bang Guy Aristide1*, Savom Eric Patrick1, Metogo Ntsama Junie Annick2, Missi Amanda Marlène1, and Essomba Arthur1,3
1General Surgery Unit, Yaoundé University Teaching Hospital, Cameroon
2Department of Obstetrics and Gynecology, Gyneco-Obstetric and Pediatric Hospital of Yaoundé, Cameroon
3Department of Surgery and Specialties, Faculty of Medicine and Biomedical Sciences, University of Yaoundé, Cameroon
*Corresponding author: Bang Guy Aristide, General surgery unit, Yaoundé' University Teaching Hospital, Cameroon, E-mail: guyaristidebang@yahoo.fr
Obstet Gynecol Cases Rev, OGCR-3-100, (Volume 3, Issue 6), Case Report; ISSN: 2377-9004
Received: May 29, 2016 | Accepted: November 25, 2016 | Published: December 01, 2016
Citation: Bang GA, Savom EP, Metogo Ntsama JA, Missi AM, Essomba A (2016) Giant Vulvar Leiomyoma: Successful Management in a Poor Setting of a Common Neoplasm in an Uncommon Site. Obstet Gynecol Cases Rev 3:100. 10.23937/2377-9004/1410100
Copyright: © 2016 Aristide BG, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
In clinical practice, leiomyoma of the vulva are infrequent and rarely encountered. We report the case of a 36-year-old Cameroonian with a 10-year history of a left labia majora swelling. After evaluating history and clinical examination, a decision of excision of this tumor was taken. Intraoperatively, the mass was well circumscribed with a weight of 480 g. The cosmetic result was good. Histopathology confirmed the diagnosis of vulvar leiomyoma.
Keywords
Vulvar tumor, Leiomyoma, Meticulous examination, Africa
Introduction
Vulvar tumors are infrequent; amongst them, malignant lesions are extremely rare, squamous cell carcinoma being the commonest [1]. Benign neoplastic lesions encountered in vulvar are: melanocytic nevi, hemangiomas, seborrheic keratosis, hidradenomas, neurofibromas, leiomyomas, vulvar cyst, angiomyxoma and fibroadenoma [2-4].
Leiomyoma or fibroid though very commonly seen in the uterus is a rare entity in vulva with an incidence of 4.2% [5]. In Africa, poor access to health care facilities and limited financial resources of patients in one hand and taboos surrounding sex on the other hand lead to delayed diagnosis with atypical clinical presentation. We present the case of a 36-year-old Cameroonian female with a 10-year history of progressively growing vulval mass with a histological report of leiomyoma after surgery.
Case Presentation
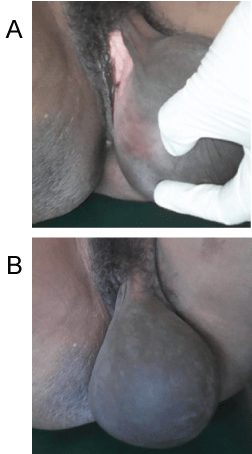
A 36-year-old Gravida 8 Para 8 Cameroonian female was received during a free mass health campaign organized by our department in a remote and isolated region of the country, with a complain of vulvar swelling. This was noticed initially as a small non-traumatic vulvar mass 10-year ago which gradually increased to present size. There was no history of fever, vulvar pains, dyspareunia or vaginal discharges. Four uncomplicated per-vaginal deliveries were carried out with this mass. Limited financial resources prevented the patient from seeking medical assistance. Previous medical and familial history was not contributive to the present illness. On examination, her general condition was fair and vital signs were stable. Vulvar examination showed a 12 × 7 cm tumor located in the left labia majora (Figure 1A). The tumor was well circumscribed, firm consistency, painless, and not adherent to skin or other structures. Overlying skin was unremarkable (Figure 1B). No associated inguinal lymphadenopathy was noticed and the rest of gynecological, abdominal and thoracic examination was unremarkable.
.
Figure 1: Preoperative view of the vulvar mass. A) Left labia majora giant mass; B) Normal overlying skin.
View Figure 1
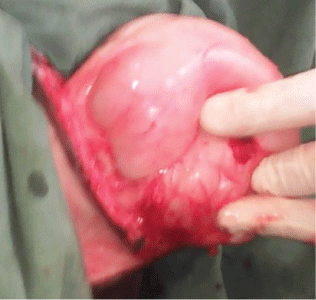
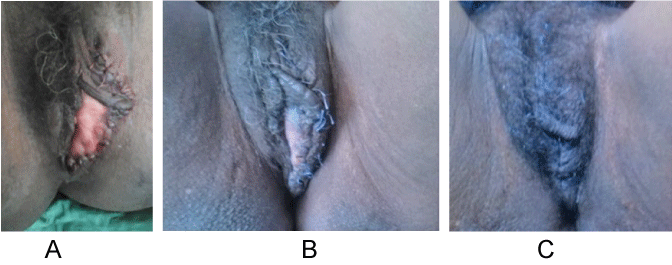
We proposed the patient to come for free of charge management in our unit in the capital city but she declined not wanting to leave her children. Radiologic Imagery was consequently not possible. Keeping all clinical features in mind, all of them in favor of a benign tumor, a decision for surgical excision of the swelling was taken. Under spinal anesthesia, an incision was made at the mucocutaneous junction. The tumor was enucleated (Figure 2) without any major bleeding nor rupture. The overlying excess skin was excised and the wound closed; but we noticed an eversion of the vaginal mucosa (Figure 3A). The patient was discharge at postoperative day one without any complications. The follow-up examination at two weeks (Figure 3B) and 3 months (Figure 3C) showed a good cosmetic result.
.
Figure 3: Cosmetic result. A) At the end of surgery; B) 2 weeks after surgery; C) 3 months after surgery.
View Figure 3
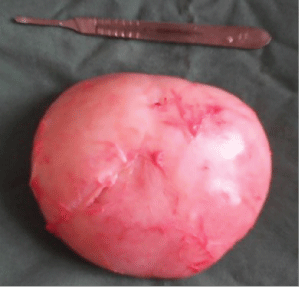
Grossly, the specimen consisted of a single nodular reddish tissue, weighing 480 g and measuring 12 × 8 × 6 cm (Figure 4). Microscopy revealed benign tumor composed of sheets and fascicles of oval to spindle shaped cells with abundant dense cytoplasm, focal lymphocytic infiltrate and areas of hyalinization without areas of necrosis nor abnormal mitosis. Final diagnosis of leiomyoma was ascertained.
Discussion
This case present a common neoplasm (leiomyoma) occurring in an uncommon site (labia majora) with a particular clinical presentation (giant mass of 480 g) and emphasized the importance of detailed history and meticulous examination in the diagnosis in a poor setting.
In developing countries as our own, there is a poor access to health care facilities for most people and when they exist, the hospital fees are too expensive for them. On the other hand, there is a lack of imaging devices; Nar, et al. [6] think that less than 20% of the populations in developing countries have access to imaging devices. This situation is more pronounced in remote and isolated regions as the one in which lives our patient. Thus justifies the uncommon presentation of diseases because of their long-term evolution at the moment of diagnosis. Our patient had a 10-year history of her vulvar mass and had delivered 4 times with it. The mass were large, with a weight of 480 g. Giant vulvar masses are rare in the literature. Karaman, et al. [7] reported in 2015 a giant vulvar epidermoid cyst in an adolescent girl measuring 11 × 8 × 10 cm and Yang, et al. a 12 cm-diameter cyst in a 37-year-old woman in 2012 [8]. A well conducted medical history and a carefully examination allow generally differentiation between benign and malignant tumors. All the clinical features of the swelling and its long-term evolution without alteration of general state were in favor of a benign mass. We could then perform surgery despite the absence of preoperative imaging. This approach had already been described in India [9]. We think that this isn't malpractice but medical practice adapted to the (poor setting) environment.
Smooth muscle tumors of the vulva are rare with an incidence of 4.2% [5] and they include a variety of histologic types. Another unusual site include: ovaries, bladder, urethra, sinonasal cavities, orbits and kidney [9]. The most common preoperative differential diagnosis is Bartholin's gland cyst [9-11]. Some authors have described leiomyoma of the vulvar associated with other leiomyoma in the same patient [12,13].
Surgical excision is the treatment of choice in all smooth muscle tumors of the vulva, but there is a great challenge to obtain a good cosmetic result particularly in giant tumors. Our case shows that even if the immediate cosmetic result is not fully satisfactory, no further surgical procedures are required. Without any intervention, small eversions of the mucosa can be corrected by wound healing with remodeling. After the surgery, a long-term follow-up is advised since some recurrence after 10 years have been reported [11].
Conclusion
Vulvar tumors are infrequent and vulvar leiomyoma is a rare type. Even if ultrasonography and magnetic resonance imaging might be of help in establishing the diagnosis, in developing countries as our own, emphasis should be placed on detailed history and meticulous clinical examination. A long-term follow-up is advised.
Competing Interests
The authors declare no competing interests.
Authors' Contribution
All persons designated as authors above, qualify for authorship, they took active part in the management of these patients and write up of this manuscript. All authors have read and agreed to the final manuscript.
References
-
De Hullu JA, Avoort IA, Oonk MH, Zee AG (2006) Management of vulvar cancers. EJSO 32: 825-831.
-
Hood AF, Lumadue J (1992) Benign vulvar tumors. Dermatol Clin 10: 371-385.
-
Leon DC, Montiel DP, Vazquez H, Hernandez C, Cetina L, et al. (2009) Vulvar fibroadenoma: a common neoplasm in an uncommon site. World J Surg Oncol 7: 70.
-
Zizi-Sermpetzoglou A, Myoteri D, Koulia K, Kontostolis V, Moschouris H, et al. (2015) Aggressive angiomyxoma of the vulva: a bizarre perineal lesion. Case Rep Oncol Med 2015: 292304.
-
Stout AP (1983) Solitary cutaneous and subcutaneous leiomyoma. Am J Surg Pathol 7: 463-475.
-
Nar AS, Bawa A, Mishra A, Mittal A (2014) Role of diagnostic laparoscopy in chronic abdominal conditions with uncertain diagnosis. Niger J Surg 20: 75-78.
-
Karaman E, Cim N, Akdemir Z, Elci E, Akdeniz H (2015) Giant vulvar epidermoid cyst in an adolescent girl. Case Rep Obstet Gynecol 2015: 942190.
-
Yang WC, Huang WC, Yang JM, Lee FK (2012) Successful management of a giant primary epidermoid cyst arising in the labia majors. Taiwan J Obstet Gynecol 51: 112-114.
-
Pandey D, Shetty J, Saxena A, Srilatha PS (2014) Leiomyoma in vulva: a diagnostic dilemma. Case Rep Obstet Gynecol 2014: 386432.
-
Francis SA, Wilcox FL, Sissons M (2012) Bartholin's gland leiomyoma: a diagnostic and management dilemma. J Obstet Gynaecol Res 38: 941-943.
-
Nielsen GP, Rosenberg AE, Koerner FC, Young RH, Scully RE (1996) Smooth muscle tumors of the vulva: a clinic-pathological study of 25 cases and review of the literature. Am J Surg Pathol 20: 779-793.
-
Wahlen T, Astedt B (1965) Familial occurrence of coexisting leiomyoma of vulva and esophagus. Acta Obstet Gynecol Scand 44: 197-203.
-
Faber K, Jones MA, Spratt D, Tarraza JHM (1991) Vulvar leiomyomatosis in a patient with esophagogastricleiomyomatosis: review of the syndrome. Gynecol Oncol 41: 92-94.